Realistic Medicine - Doing the right thing: Chief Medical Officer annual report 2022 to 2023
Chief Medical Officer's (CMO) third annual report, and the seventh on Realistic Medicine. It reflects on the challenges our system is facing and asks professionals to practise Realistic Medicine, in order to deliver value based health and care and a more sustainable system.
Chapter 4: Climate and Health: Planet and People in Partnership
The climate emergency
– the single biggest health threat facing humanity
The climate emergency is no longer a potential and distant threat. Instead it is an immediate population health crisis, unfolding in multiple ways and affecting everyone globally. It requires action now to prevent its worst impacts. The earth has warmed by about 1.1oC since the beginning of the industrial revolution, with most of this warming happening in the last 50 years. The last decade was the warmest ever recorded. A child born today is entering a world with a different climate to the one I was born into. In March 2023, the Intergovernmental Panel on Climate Change highlighted the burning of fossil fuels, and unequal and unsustainable energy and land use as the main drivers of global warming to date, and that the pace and scale of action needs to accelerate to keep global temperatures below 1.5oC. Every increment of warming results in rapidly escalating hazards, with more intense heatwaves, heavier rainfall, food and water insecurity, and other extremes that put human health and ecosystems at risk. Climate change has a multiplier effect, and covers not just extremes of weather, but also the impact of pollution and biodiversity loss on the natural environment. The consequences of these changes demonstrate how closely linked human health is to that of our planet and its natural systems.
Globally, the impacts of adverse climate events reduce access to the resources on which we all depend, including food, water, health, education, and transport. During this last year newsfeeds reported on wildfires in Europe that destroyed nearly 660,000 hectares of land; floods in Pakistan that put one third of the country under water; heatwaves that saw new temperature highs of 49o C in Delhi, 50.7o C on the northwest coast of Australia and 47o C in Portugal; storms that killed hundreds and cut off thousands of people from essential food and care in Madagascar, Malawi and Mozambique; and droughts that have put up to 20 million people living in the Horn of Africa at risk of starvation.
Closer to home, temperatures in the UK exceeded 40o C for the first time during heatwaves in 2022. England recorded 2803 excess deaths in those over 65 years of age during these heat-periods between June and August 2022. In Scotland the shifts in rain patterns and the late winters, early springs and hot summers may have seemed positive to some, but they are the warning signs of nature being out of balance. In the past year, the lack of rain during growing season destroyed significant agriculture and heightened risks of fires. Storms and their resultant floods broke transport links, destroyed family homes and property, and increased the risk of damp in housing. The climate emergency is very much here and affecting us now.
We are at a unique moment in history, a turning point where the future is in our hands. We have a vital role to play, as we continue to work tirelessly to support the people we care for, and as the people who make our health and care services anchor institutions within our communities, embodying and protecting the core values of our society.
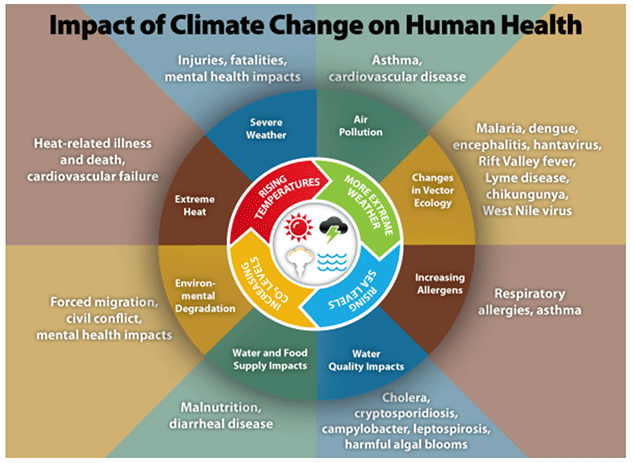
The climate emergency affects human health and wellbeing both directly and indirectly.
Direct effects of the climate emergency on human health are seen through changing weather patterns. Heat stress, floods, cyclones, wildfires, and storms can all impact directly on our health. Prominent most recently has been the effect of heatwaves across the globe. Heat-related deaths in Scotland could rise from 85 in the year 2000, to 285 a year by 2050, with particularly those at the extremes of age being most vulnerable. Heatwaves affect maternal health with increasing risks of lower birth weights and preterm births. Flooding and economic disruption are also associated with mental health impacts due to unforeseen costs, business disruption, and temporary housing in Scotland.
Indirectly, the climate emergency is changing the nature and patterns of diseases we experience. Vector-borne diseases are increasing globally, mosquitoes have longer breeding seasons and are occupying more widespread geographies. In the UK the prevalence of Lyme disease and West Nile virus is increasing. The incidence of Lyme disease in Scotland increased by 50% from 200 in 2015, to 308 in 2019. Bacteria, parasites, harmful algae, and viruses are becoming more prevalent, harder to control, and more resistant, affecting food security and causing food-borne illnesses.
Air pollution is created from fine particulate matter emitted from various sources including fossil fuels, vehicle exhausts, tyres, brakes, burning of wood and coal, industrial processes, chemical reactions, and agricultural processes. These particles are small enough to penetrate the lungs and make their way into the bloodstream and then to other organs of the body. The World Health Organisation (WHO) Global Air Quality Guidelines indicate that 90% of people live in areas where ambient air pollution is at harmful levels. Coastal flooding, riverbank overflow, and landslides are increasingly common, and difficult to manage. Flash floods and increased run off from the floods has led to water contamination, and interruption of water supplies, with cholera risks increasing year on year.
Glasgow to Inverness 175 miles
4 miles Glasgow to... another bit of Glasgow
Equivalent tailpipe greenhouse gas emissions from a Ventolin Evohaler (containing 100 2-puff doses) and a Ventolin Accuhaler (60 1-puff doses). Assumes car achieves 100gCO2/km.
Inhaling cleaner air
The climate emergency has been described as the greatest threat to global health. The National Health Service accounts for 5.4% of UK carbon emissions. In general practice the majority of emissions are from prescribing, 25% of which are from metered dose inhalers (MDIs).
MDIs contain hydrofluorocarbons. The environmental impact of one MDI is equivalent to driving 175 miles by car, for example driving from Glasgow to Inverness. A dry powder inhaler (DPI) is closer to a 4-mile drive. Disposal of inhalers in landfill is harmful to the environment in both material waste and greenhouse gas emissions.
Garscadden Burn Medical Practice initiated the change in peoples' treatment, where appropriate, from MDI to a DPI. All six practices within Cluster A of North West Glasgow Health and Social Care Partnership agreed to deliver a Quality Improvement Programme – Greener Respiratory Health;
The aim was to:
- reduce use of MDI where appropriate, raise awareness of environmental impact, and encourage greener disposal of inhalers;
- develop an audit tool to monitor and quantify the Quality Improvement approach;
- gather data on overall patient management, quantify appropriate inhaler changes and the resultant reduction in greenhouse gas emissions; and,
- avoid increasing the Practice Nurse workload by making the audit tool easy to use, and completed as part of asthma/COPD reviews.
What have the outcomes been/What difference has this made?
- from January – mid-April 2023, 128 patient reviews were completed. In this group 643 MDI's had been prescribed in the previous 12 months;
- most people were not aware of the environmental impact of MDI inhalers;
- 104 people were suitable for and wanted to switch to a DPI;
- by swapping 104 people to a DPI the need for MDI prescriptions were reduced;
- this saved 12,217kg of CO2, the equivalent of driving 112,525 miles or travelling 4.5 times around our planet; and,
- this approach continues to deliver the co-benefits of reducing the carbon footprint of care and reduce air pollution, while supporting shared decision making.
The climate emergency is also a socioeconomic emergency
Health and equity are inextricably linked. Those who are already most vulnerable in society are least able to protect themselves against the impacts of adverse events. The drivers of the climate emergency also reflect a global and local inequality. The majority of the greenhouse gas emissions are, and have been historically, linked to high income countries and the energy systems used to power economic systems. As we have explored in the previous chapter, increasing social inequalities contribute to widening health inequalities. Those living in areas of deprivation and in rural areas are most vulnerable to extreme weather events such as storms and extreme cold, especially where housing lacks insulation and heating is expensive . Air pollution levels are higher in almost all deprived areas in Scotland. The Third UK Climate Change Risk Assessment found that flood disadvantage is greater in coastal areas, declining urban cities and dispersed rural communities.
The climate emergency adversely impacts GDP and local economic development in several ways including:
1. destruction of livelihoods;
2. damage to infrastructure by extreme weather events; and,
3. increasing costs linked to core resources such as food and water.
The IMF in 2020 predicted that direct damages linked to climate disasters such as wildfires and flooding between 2010-2020 cost US$ 1.3 trillion (on average 0.2% of global GDP annually). Increases in energy and food prices affect the lowest-income households most across the globe. Fuel poverty, whereby households spend greater than 10% of their income on energy, is highest in rural and remote regions of Scotland. Food security and food safety have been threatened. The increase in cost for poorer families is a much larger proportion of the household budget than for wealthier households who can often absorb more of the shock. The figure below from the World Health Organisation shows some of the mechanisms through which climate change can influence health outcomes.
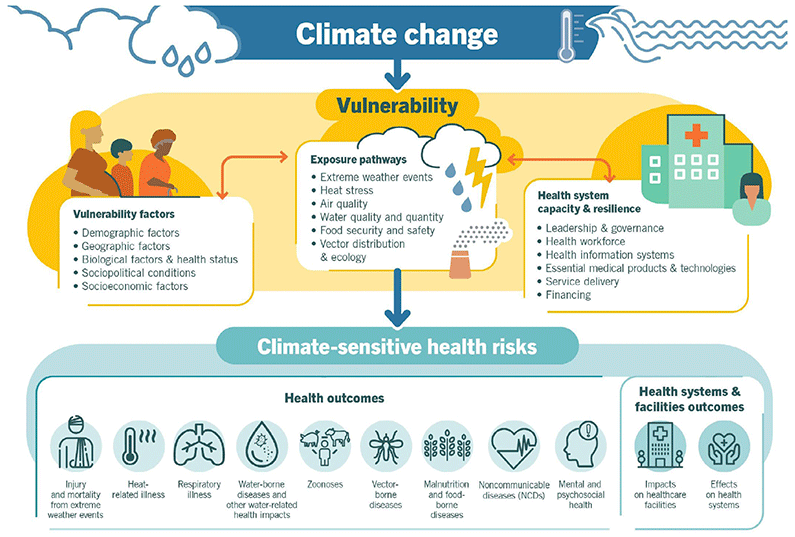
Reducing our impact on the environment and adapting to change
I've mentioned this in previous reports, however it remains a sobering fact. If healthcare were a country it would be the fifth largest emitter on the planet. The global health care climate footprint is equivalent to the greenhouse gas emissions from 514 coal-fired power plants.
Recognising this, Scotland was the first national health service in the UK to commit to becoming a 'net zero' organisation. Our NHS Scotland Climate Emergency and Sustainability Strategy 2022-26 was published in August 2022. It sets out five main areas where change can happen:
- sustainable buildings and lands;
- sustainable travel;
- sustainable goods and services;
- sustainable care; and
- sustainable communities.
Clinicians and staff must be at the heart of work to achieve a culture of stewardship within NHS Scotland, where resources are safeguarded and responsibly used to provide environmentally sustainable healthcare. Improving patient care is fundamental and all steps taken are with the dual focus of improving outcomes for patients and reducing environmental impact. The aim of this strategy is to complement action taking place at an individual level, but also to help provide the support to staff to take action to reduce their impact.
We have already seen the impact clinicians can have in this space. Desflurane was responsible for most of the emissions from NHS Scotland's use of volatile medical gases. Green Anaesthesia Scotland, a grassroots group of anaesthetists, started to decrease the use of this drug in 2017, substituting it with another agent, Sevoflurane, which is just as safe and effective, reduces carbon emissions by more than 80%, and costs four times less. This work continued with the establishment of the National Green Theatre Programme and, after consultation with the wider anaesthetic community, it was agreed that Desflurane will no longer be available on the National Procurement contract. This has saved emissions equivalent to powering 1,700 homes every year.
To fully tackle the climate emergency, effective collaborative working across the healthcare system will be vital. There is great power in combining the aims of Estates Management teams and Procurement teams to unify the action of proactive and positive change. For example, it is estimated across Scotland that approximately only 30% of waste found in orange clinical waste bags is clinical waste; the remaining 70% is either similar to residual (domestic) waste, or is valuable recycling material. The mis-segregation of waste has a significant cost burden in terms of both financial and environmental cost. To promote greater understanding of the risk posed and working to support and encourage clinicians to make informed decisions, NHS Scotland has launched a waste management training package to help staff segregate and manage the valuable resources in waste better. This work came through a Short Life Working Group of Waste Management Officers and led by NHS Assure. It is the first national training package for waste management in place for NHS Scotland, and is a great example of one of the many ways that clinicians are being supported to take more sustainable action.
Of course whilst we should and will take action to combat the emissions of the NHS, it is also vital that we ensure that we are able to adapt to changes. Fortunately, many of our actions to reduce emissions, promote biodiversity and reduce pollution also make the NHS more resilient. For example, developing and managing greenspace and other green infrastructure such as green roofs and rain gardens to mitigate flood and overheating risks, will also promote biodiversity and make the NHS estate more appealing for staff and the people we care for.
Making use of green and blue spaces
Nearly 2.8 million people in the UK live more than 10 minutes' walk from a garden, public park or playing field. A Health Impact Assessment by the Lancet Planetary Health in more than 1,000 European cities in 31 countries, concluded that 43,000 premature deaths in Europe could be prevented every year if urban green spaces were increased.
Green and blue prescriptions (blue prescriptions refer to nature activities related to water) are 'doses' of nature tailored to people's wellbeing needs.
In Edinburgh, five GP practices worked with the Royal Society for the Protection of Birds to deliver Nature Prescriptions. This included a leaflet and a monthly calendar of nature activities and ideas. Nature was prescribed for 32 different health conditions across all age groups. Prescribers were predominantly GPs, but included Practice Nurses, Health Care Assistants, a Community Psychiatric Nurse and a Link Worker. 74% of people reported that the Nature Prescription had benefitted them, with 70% stating they continued to connect with nature daily, or multiple times a week. People and prescribers also reported increased awareness of nature.
In terms of action to adapt, in June 2019, NHS Chief Executives committed to each Health Board undertaking a Climate Change Risk Assessment covering all operational areas and producing a Climate Change Adaptation Plan to ensure climate-resilient health systems under changing climate conditions. To date, 17 Health Boards have completed a Climate Change Risk Assessment. Building on this, these Boards are developing Adaptation Plans. Due to the important role the NHS plays in local communities, this work will contribute to public sector-wide local and regional adaptation planning activity.
The triple win – co-benefits of action
When I think about the role of health and social care leaders in tackling the climate emergency, I think of three things:
1. the impact of the climate emergency on health itself. This relates to the direct impact of weather extremes and the indirect impact of changing patterns of disease. These factors give us cause to rethink how we deliver sustainable healthcare;
2. the resilience of our health and social care systems. The global examples illustrated above demonstrate the incredible challenges these events present to the provision of healthcare. We must work together to ensure our health and care services are equipped to cope with ever increasing environmental challenges; and
3. the impact that the delivery of health and social care has on the climate emergency. For me this relates to leaders and health and care professionals recognising the need for more sustainable care and collaborating to develop greener pathways of care that will deliver better value, more sustainable care which help to eliminate waste – both wasted resources and the time wasted in providing low value, or futile care.
Practising Realistic Medicine can help us tackle the climate emergency on all three fronts. By practising Realistic Medicine we can deliver better value for the individuals we care for, improve the resilience of our health and care system by reducing waste and potential harm, and redirect resource that is currently wasted to higher value, greener, more sustainable care. A challenge to us all is to identify those areas of work that we all contribute to, but which don't add any meaningful difference to the people we care for. After all, inappropriate care is wasteful care. We can reduce the carbon footprint of our healthcare through promoting good health, detecting treatable and preventable illness early, utilising convenient access to virtual patient services when this is appropriate, reducing prescriptions that are redundant and working together to prescribe the right drugs for the right diagnosis.
Re-using and recycling walking aids in NHS Forth Valley
Over 8,000 walking aids were being issued to people by NHS Forth Valley annually with no clear pathway of returning the items when they were no longer required. Many items were being discarded in clinical areas causing infection control problems, or ending up in landfill. The purchasing of new walking aids meant that the budget was grossly overspent.
In 2021, a returns pathway was created to encourage Forth Valley residents to return walking aids to their local recycling centre. Walking aids are collected, inspected and if fit for re-use, cleaned and returned to NHS Forth Valley. Walking aids not fit for re-use are recycled.
5,153 walking aids have been returned to NHS Forth Valley fit for re-use, with an additional 3,337 items recycled since the pathway was introduced, contributing to carbon savings of approximately 29,375 KgCO2e. Approximately 50% of walking aid orders are now fulfilled using re-used aids, generating a significant cost saving too.
There is an extraordinary triple win for us all through a positive response to the climate emergency the co-benefits of action will improve our own health and the health of our communities and the population in Scotland, it will improve our experience of working in and with the NHS, and NHS Scotland's ability to deliver sustainably now and in the future.
Triple wins:
Taking climate action
- improves health outcomes for patients, our population and the planet
- creates a safer, sustainable place to work
- reduces cost of care immediately and in the future
Climate action is not only action to keep our planet safe, it is action for health and wellbeing
Investing in climate friendly and climate resilient energy, food and infrastructure has multiple benefits for health now and in the future. Increasing availability of public transport and infrastructure that enables active travel will both reduce carbon emissions and improve air quality, bringing multiple health benefits. For example, cleaner air reduces the risk of respiratory and other illnesses, walking and cycling promote physical and mental health, and access to green spaces reduces social isolation and enhances community cohesion. Indeed the annual health and economic benefits of active commuting to work in Scotland has been estimated to be EUR 700.2 million, and EUR 79.8 million for cycling to work.
Sustaining momentum
Work with the Sustrans' NHS Workplace Engagement Programme is underway in NHS Dumfries & Galloway, NHS Grampian, NHS Highlands and NHS Shetland. A Workplace Engagement Programme Officer has also been employed in NHS Ayrshire & Arran via Sustrans since November 2022. The overall aim of the programme of increasing active travel should contribute to cleaner air in our local communities, increase physical activity levels of staff, and reduce travel costs for staff-and it's already having a positive impact for many individuals:
Helen Hendry, Obstetrics, Raigmore Hospital
Helen always drove the 2.5 miles to work but in 2019, worried by her family history of Type 2 diabetes and her high BMI, she bought an ebike through the staff cycle to work scheme. She now gets daily exercise from her commute, with the ebike helping with the hills and making the trip really comfortable.
After just a month she sold her car. Running just one household car made immediate savings of £300 per month.
Helen says: "I really love my commute and my ebike. I have a good route and park right outside my office – no stress! The exercise and fresh air really helps me clear my head after a day at work before I go home to my family. On the odd occasion when I need to use the car instead, I really miss my cycle!
The staff cycle to work scheme saved me money on the bike and accessories like a helmet and a good lock, and let me spread payments which was really helpful. An Active Travel Project Bike Doctor session gave me free help and advice with my brakes.
Since I've switched from driving to my ebike, I've lost 3 stone.
I really enjoy it and feel great. The financial savings are also really welcome!"
The human food system is responsible for more than one third of global greenhouse gas emissions, and the primary cause of biodiversity loss. Yet, globally 25-30% of food produced is lost or wasted on an annual basis. Transitioning to less carbon intensive diets with less meat and more plant-based foods, and only producing what we need would bring co-benefits of reducing carbon emissions, protecting biodiversity, and consuming healthier diets.
Reducing waste not only reduces procurement costs but also the energy used to produce stuff that ultimately does not get used. An estimated 10% of prescribed medication is thrown into toilets or drains. The presence of pharmaceuticals in the environment, particularly antimicrobials, has also been associated with the exacerbation of antimicrobial resistance in bacteria, fungi and other microorganisms. Whilst there is limited understanding on the contribution of environmental antimicrobial resistance on population health, this is nevertheless an area of serious concern, since antimicrobial resistance is a major global health problem which accounted for 4.95 million deaths in 2019.
Wastewater systems were never designed to remove small, complex chemical molecules. Inevitably many medicines pass through the treatment plants and end up in surface waters and rivers in the effluent or in the sludge which is then spread on crops and can enter the food chain. NHS Highland is leading a Medical Research Council project to develop an eco-directed framework for prescribing decisions, essentially aiming to include environmental data about risk and hazard into a model which could help formulary choices or health technology assessments in the future. When we choose to consider environmental sustainability in selecting, prescribing, using, and disposing of medicines the application of Realistic Medicine again comes to the fore:
- promoting a person-centred approach to preventing population ill health;
- using shared decision making to discuss the risks and benefits of medicines;
- optimising pharmaceutical use and prescription;
- reduction of pharmaceutical wastes and inappropriate polypharmacy;
- enhancing the use of social prescribing; and,
- reducing variations in clinical practice.
Words into Action
Our physical and mental health is dependent on flourishing natural and social systems and the wise stewardship of these, but the continuous warming of the planet is placing health, wellbeing and health systems in danger. As health and care professionals we must not lose sight of our role in delivering a sustainable health and care system, and we must recognise and fully understand the links between practising sustainably, planetary health and human health.
Taking proactive action to mitigate against the climate emergency, and to adapting to its effects will improve our environment, and reduce biodiversity loss. What we, as a community of health and social care providers, now know is that taking action to become more climate resilient will simultaneously change the health of Scotland for the better.
All the adaptation and mitigation measures needed to reduce the suffering that the climate emergency will bring, are actions, which will also reduce disease, improve wellbeing, create better living conditions, and foster relationships with nature. This is the integrated nature of the four threats to population health that we face. Many of us will have strong personal reasons for wanting to take proactive steps for our loved ones, as well as future generations. I have found that aligning personal values to areas within my professional role and influence to be deeply fulfilling.
We can act individually by making wise choices. This year the United Nations campaign for Individual Action was launched setting out 10 steps each person can take to tackle the climate emergency. From a healthcare perspective, this can be made more specific by thinking of the areas of clinical practice that link to environmentally sustainable healthcare. The 10 things healthcare workers can do to combat climate change from Dr Sarah Barlett and Dr Marion Slater from the Royal College of Physicians of Edinburgh gives an outline of this.
10 things health workers can do to reduce our professional impact on the environment
1. Practise good preventative medicine
2. De-prescribe unnecessary medication and consider what you do prescribe
3. Reduce the number of investigations you request
4. Use telephone consultations and low carbon meetings when possible
5. Reduce unnecessary use of disposable PPE
6. Switch things off and close doors
7. Walk or cycle to work (or use public transport)
8. Bring your own (local plant based) food and drink in reusable containers
9. Learn about the problem, audit your practice, and share the stories
10. Join discussions in your trust about the big things (procurement, energy, recycling etc)
We can act collectively
In our role as healthcare professionals we can help make the connections between the changing climate and our health and wellbeing, and importantly relate these to the people we care for. Frequent surveys continue to place health and care workers as the most trusted professional community. Our voices and our values matter and have influence. We work within anchor institutions that provide stability and connection across the whole of Scotland. Our NHS as an institution is dependable and a trusted source of "societal value". The NHS workforce has the power to model actions – assessing risk, demonstrating climate resilience, and planning for all our futures. As global citizens our NHS in Scotland has something exceptional to offer to global conversations on how to reimagine healthcare differently.
Taking action for the climate emergency is not about doing more work, filling in more forms or ticking more boxes. Taking action is intrinsically about enacting our values: valuing people, our planet and our health. We can nurture the conditions that allow people to live healthy lives and flourish. Our commitment is to a health and care system that is open to everyone, a place that cares about how each person is now and how they will be in the future.
We are acting as a country
Low-carbon policies across industry, agriculture and transport in the nine largest greenhouse-gas-emitting counties would avoid an estimated 10 million premature deaths every year.
Scotland's aim of leading the world in this area is ambitious and necessary. We have a national co-ordinated response, with every sector taking action to reduce the negative impacts of the climate emergency. The actions we take as a country within a global community to stop the earth's temperature rising are actions which will reduce disease, improve fitness, support mental health and wellbeing, create spaces and places that are more conducive to nature and good to be in, reduce living costs and increase our solidarity.
Conclusion
It is no longer acceptable to simply talk of the action required to mitigate the harmful impacts of the climate emergency. The impacts are already being felt around the world and more urgent action is necessary. The earlier and more collectively we act, the bigger and quicker the gains will be. By addressing the wide range of health impacts of the climate emergency, by strengthening our services and systems so that they are sustainable and climate resilient, and by promoting the health co-benefits of all the work that is done nationally and locally to mitigate climate change, we bring about our triple wins. And we must recognise also that these gains extend far beyond the beneficial impact that we can have on the climate. By taking action, we also bring benefit and mitigate risks associated with our other population health challenges too. This is the right thing to do and we must now ensure that these known actions are fully achieved across the country.
Contact
Email: realisticmedicine@gov.scot