Out-of-Hospital Cardiac Arrest: A Strategy for Scotland
The Out-of-Hospital Cardiac Arrest(OHCA) strategy, which has been developed in collaboration with a range of stakeholders, is a 5 year plan with the aim of ensuring that by 2020 Scotland becomes an international leader in OHCA outcomes. The headline aim is to save an additional 1,000 lives by 2020.
BACKGROUND
Shape of the Problem
Out-of-hospital cardiac arrest: A healthcare challenge
Out-of-hospital cardiac arrest remains a significant healthcare challenge in Scotland. In 2011/12 the Scottish Ambulance Service responded to approximately 8,900 adult OHCA calls, 3,058 of these resulted in resuscitation attempts.[1] Although almost a third of these patients had a favourable 'shockable' heart rhythm, overall only 16.1% had return of a pulse (i.e. return of spontaneous circulation, or ROSC) before arriving in the Emergency Department. Having reached hospital, not all survive to leave hospital alive.
Because of the greater distances involved, responding quickly to an OHCA in remote and rural locations is particularly challenging for emergency services. We also know that for a number of reasons, outcomes from OHCA are not as good in more deprived communities.
It should be noted that data on survival to discharge after OHCA has not been routinely collected on a national basis in Scotland. However, extrapolating from the number of patients who had ROSC it is likely that only around 1 in 20 patients survives to discharge in Scotland following OHCA.
International comparisons of OHCA survival
This picture of poor survival after OHCA is not universal in developed countries. There is significant differences in survival after OHCA between centres across the USA and between different European cities.[2,3,4,5]
Figure 1: Difference in survival to discharge for OHCA (all rhythms) treated by emergency medical services in USA and EU.
| USA |
EU |
|
|---|---|---|
| Best |
16.3% |
22.0% |
| Worst |
3.0% |
3.6% |
| Fold Difference |
5 times |
6 times |
Seattle & King County in the state of Washington, USA - currently among the best for regional OHCA survival - reported an overall (all-rhythms) survival to discharge rate of 22% in 2013.[6] Across Europe, the average go-home survival rate is almost twice that of Scotland at around 9%.[5] Currently the single centre with the best OHCA outcomes is Stavanger, quoting 25% overall survival.[2] The whole-country registries reported in the literature illustrate this pattern with significant inter-regional variation in outcomes, e.g. the All-Japan Registry reporting a range of neurologically intact survival from 1.9% to 3.1% after OHCA (2005-07).[7] In contrast the Swedish national registry illustrates the potential of whole system optimisation to improve outcomes across a nation reporting an increase in OHCA survival from 4.8% in 1992 to 10.7% in 2011.[8]
There is much to learn about improving OHCA outcomes from the experience of international centres of excellence. Box 3 summarises the key lessons.
| Box 3 Learning from International Experience There is much we can learn from other areas to help us address the challenges. Centres of excellence and international leaders in OHCA are to be found in North America (e.g. Seattle, Arizona, Maryland, British Columbia), in Scandinavia (e.g. Copenhagen, Stavanger) and in Australia (e.g. Melbourne). Although each system has its own nuances, there are a number of themes that are consistent across them all.
Benchmarking, networking and learning from centres of excellence will enable Scotland to build upon what we already have in place and help us to work towards our national ambition of being recognised as an international leader for our approach to out-of-hospital cardiac arrest. |
System of care
Regional differences in survival after OHCA do not reflect a range of medical approaches - resuscitation guidelines are the same in all of these locations. Similarly, higher rates of survival in some centres cannot be fully explained by differences in patient demographics or health infrastructure. These observations strongly suggest that OHCA, in many cases, is a treatable condition, and that outcomes are dependent on the effectiveness of the overall system of care.
Quality of life for survivors of OHCA
The majority of survivors after OHCA are discharged from hospital to live independent lives. A recent audit of 107 consecutive survivors after OHCA admitted to the intensive care unit at Edinburgh Royal Infirmary showed that only 1 patient out of 53 survivors was discharged with severe neurological disability.[9] This finding is consistent with other centres e.g. a large multi-centre European study of ICU management of OHCA (939 patients) found that 91% of survivors were discharged neurologically intact, to independent living, similarly the Ontario Pre-hospital Advanced Life Support study found that of 305 survivors, 96% were living independently at 12 months.[10] The consensus of recent work in this area is that cognitive impairment (e.g. memory problems) is common in cardiac arrest survivors, but has little effect on activities of daily living or quality of life.[11-13]
The importance of a quick reaction
Rapidly initiated CPR and defibrillation are of paramount importance. Bystander CPR can increase a patient's chances of survival by 2-3 times,[14,15]however time is everything. Untreated, the survival chances of a patient in VF decrease by an estimated 10% per minute. Bystander CPR buys time, halving the rate of this decrease. Survival probability is higher if shocks are delivered earlier, and higher still if bystander CPR is performed. See Figure 2 below.
Defibrillation and CPR
Defibrillation works in synergy with CPR, and is most effective the earlier it is performed. Delivering a defibrillatory electrical shock to the heart within 3-5 minutes of collapse can produce survival rates as high as 75%.
Defibrillation is the only successful treatment available for the commonest heart rhythm disturbance causing OHCA - ventricular fibrillation (VF). Defibrillation consists of delivering a therapeutic dose of electrical energy to the heart using a device called a defibrillator. The earlier defibrillation is performed, the more likely it is to be successful in restarting the heart. The rapid reduction in the likelihood of survival can be slowed if CPR is performed to 'buy-time' until defibrillation can be performed.
In order to achieve early CPR and defibrillation, Scottish Ambulance Service responders must arrive at the scene as quickly as possible. In areas where geographical constraints make this a challenging goal, these actions could be carried out by trained first responders (e.g. CFR or Fire Service) or willing bystanders, coached by Ambulance control call-takers. It is crucial to understand that improving the in-hospital care of patients after OHCA is almost irrelevant to improving overall survival figures unless we first optimise what occurs pre-hospital, during the first few minutes after OHCA. A patient who is successfully resuscitated before arriving at the Emergency Department is 35 times more likely to survive to hospital discharge than a patient who arrives without a pulse.[16]
Post Resuscitation Care
After the initial resuscitation phase, a complex series of interventions is required to ensure the best chance of a patient's long-term survival. Key elements may include rapid stabilisation in the Emergency Department, Percutaneous Coronary Intervention (PCI) by Cardiology and ventilatory support with temperature management by Intensive Care. This combination of interventions is not available in all hospitals resulting in the need for secondary transfer to specialist centres - this suggests a rationale for regionalisation of post-arrest management similar to that for major trauma, stroke and myocardial infarction.
Figure 2: The effect of bystander CPR and call-to-shock interval on the likelihood of survival to hospital discharge.
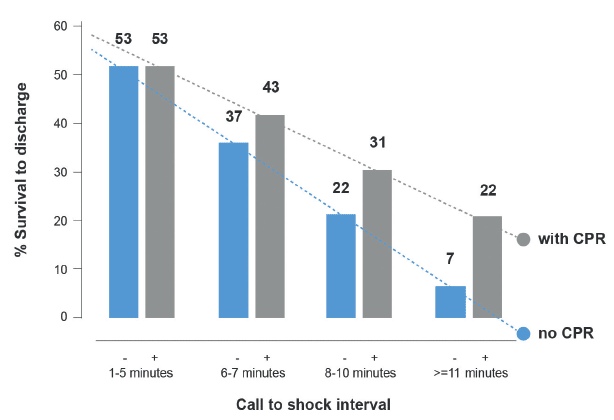
Figure 3: Impact of the Danish 'Survival' Programme. Bystander witnessed arrest, Bystander CPR, Shockable heart rhythm as first recorded rhythm and Survival on arrival at the hospital, Denmark 2001-2010.[17]
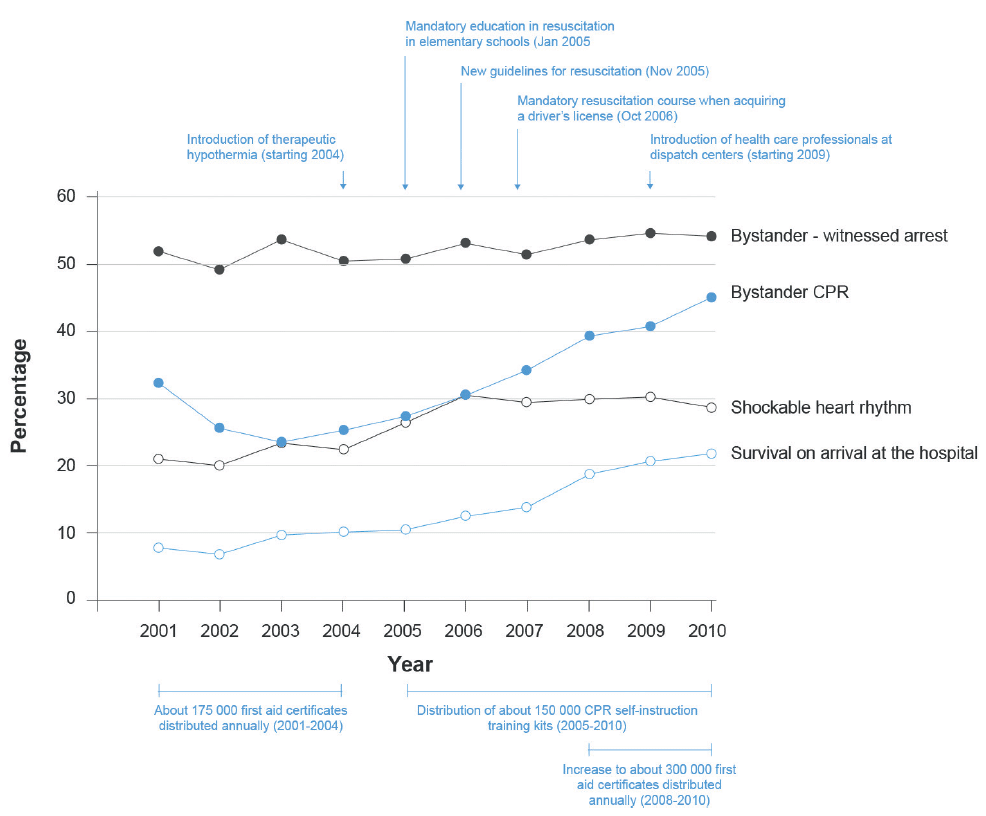
This figure from published work in Denmark illustrates the increase in survival after OHCA in parallel with a rise in the incidence of bystander CPR. The increase in CPR was achieved after a range of measures including mandatory resuscitation training in schools and legislation to make CPR training part of acquiring a driver's licence.
Optimising the Chain of Survival
Achieving our ambition of Scotland matching the OHCA outcomes achieved by the best systems in the world will require a broad range of actions and improvements to address all the elements of the 'augmented chain of survival', (see Figure 4).
Figure 4: The 'augmented chain of survival' [18]
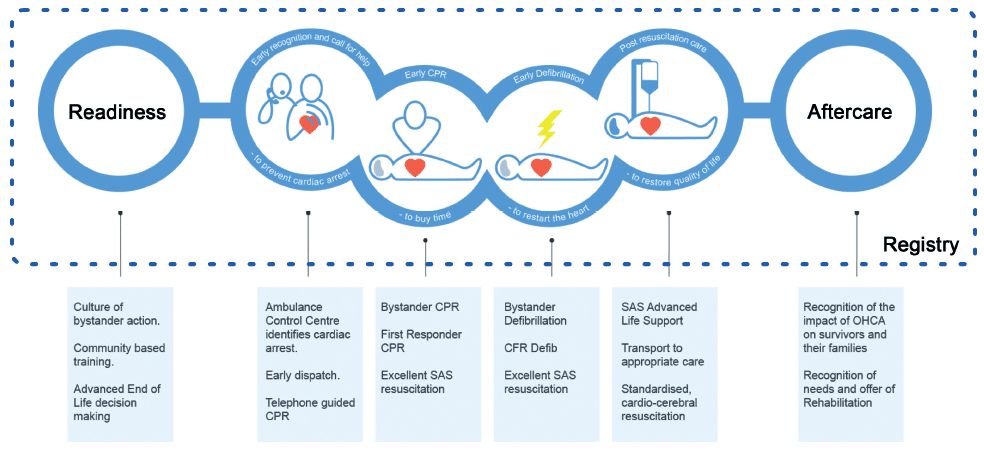
In addition to the traditional elements of the chain of survival, the 'augmented' chain includes community readiness to respond to OHCA and the rehabilitation and aftercare of patients and families involved. These additional links are not usually emphasised, but are crucial to improving outcomes after OHCA across all of the communities in Scotland.
A chain is a good metaphor for the series of events required to resuscitate someone after OHCA. It is a reminder that all of the links must be robustly joined. Individual elements have limited value if the links preceding and following are not also strong.
The diagram above highlights the whole chain occurring in a context of good data. A registry based on robust and systematic data collection provides the information needed for governance, benchmarking and to drive quality improvement.
Contact
Email: David Cline