National Demand Optimisation Group (NDOG): demand optimisation in laboratory medicine - phase IV report
The National Demand Optimisation Group (NDOG) is a Scottish Government commissioned group. Its main objective is to reduce unwarranted variation in laboratory diagnostic testing, contributing to improved patient outcomes The group has recently completed its fourth phase of work.
Annex D: RE-DO Proposal Paper (August 2020)
REDO Laboratory Testing (Re-Engineered Demand Optimisation)
A Post COVID-19 Approach to Appropriate Laboratory Test Use.
Background
It has been widely accepted and demonstrated that there is considerable variation in the use of diagnostic tests across the NHS. While some of this variation may be attributed to clinical and demographic differences, the degree of variation suggests an element of over/under-requesting, or unnecessary repeat testing. In addition, the lack of availability or awareness of certain tests within some NHS Boards will also limit their optimal use and thus further amplify any variation in such use. Demand Optimisation is defined as the process by which diagnostic test use is optimised to maximise clinical utility, which in turn optimises clinical care and drives more efficient use of associated scarce NHS resources.
Demand Optimisation has become a focus programme within the Scottish Government's Healthcare Science National Delivery Plan (NDP). In 2015, the Scottish Government requested that a National Demand Optimisation Group (NDOG) be established to review the third deliverable of the NDP. This group has subsequently delivered through three phases and is about to commence Phase Four. The programme has identified areas of good practice across the disciplines, coordinated collection of laboratory test use data, compiled an Atlas of Variation, developed online Atlas tools and interactive elements and had just begun formulating flash reports on appropriate test use for GP pilot work. The onset of the COVID-19 pandemic understandably paused the programme's work in March 2020.
COVID-19
The impact of the COVID-19 pandemic on the delivery of healthcare has been dramatic. Non-essential work was set aside with resources focused on preparing for and dealing with the impact of the virus. Lockdown and social distancing also had a major effect on the types of services offered and the capacity for such work. Significant changes in how laboratory tests are used, both during the lockdown phase and the recovery period, would seem to be continuing, with the new ways of working and the reduced capacity for patient facing interaction, including phlebotomy, being major factors affecting laboratory test use. The need for appropriate, targeted use of diagnostic tests will likely be even more important in the changed, scarred and finance limited NHS of the future, especially during any attempted "catch up" or recovery phase.
Changed ways of working within the NHS, along with the limitations of delivery in a socially distanced setting, will clearly have major effects on how test use activity can be recorded, assessed and compared. The Demand Optimisation programme has an even more important role than before to ensure that such limited capacity and resource can be best used to ensure optimal use of laboratory tests and ultimately patient care.
Impact of the COVID-19 Pandemic on Laboratory Testing
During Lockdown and with the refocus of NHS care towards dealing with the pandemic, many services within both primary and secondary care were significantly reduced or paused. In addition, patient numbers presenting to NHS facilities also reduced significantly. This had a dramatic effect on phlebotomy and subsequent laboratory test use. An example of this is seen in the graph below from NHS Grampian, which demonstrated reductions in early lockdown of around 70%. This has slowly begun to rise again as lockdown has eased and some services have returned, however levels remain around 30% less than before.
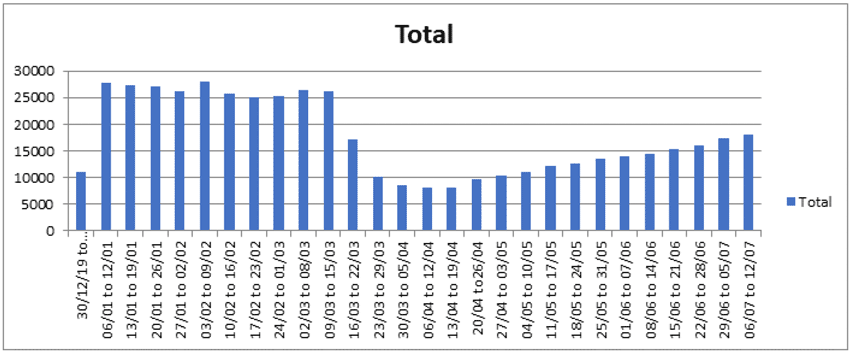
In addition, out-patient activity has significantly reduced and is very slowly returning:
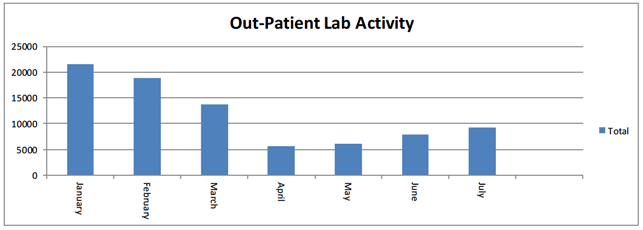
Impact on Secondary Care
Huge backlogs in elective activity have inevitably built up – this will include expansion of waiting lists for out-patient referral, investigations, surgery, other procedures, and treatment. Social distancing has reduced capacity in all these areas, with many services still on pause. Out-patient follow up and new referrals continue to see a significant expansion in remote ways of working, such as Near-Me, Microsoft teams and telephone consultation use. Blood samples usually taken in a secondary care clinic setting are now more appropriately being targeted towards a community solution – however there are limitations with that - see below. In addition, while there have been significant reductions in pathology workload, the likely backlog that has been created clinically will inevitably impact cellular pathology departments in the near future as activity resumes and "catch up" is attempted. Complexity of specimens is also likely to increase as a result of more advanced presentations.
Impact on Primary Care
Similar backlogs have also developed in Primary Care; however capacity is also limited due to continued staff absence and social distancing restrictions leading to reduced throughput of things like blood testing within practices. While overall testing remains well below pre-COVID-19 levels, "new" capacity levels for phlebotomy would appear to have been exhausted. Expansion of community-based phlebotomy focused around General Practice would seem unlikely given these limitations, which would severely impact the overall effectiveness of remote secondary care clinics, given their now increased dependency on remote phlebotomy delivered in the community. Some Boards are now actively looking to develop new community-based phlebotomy centres which could deliver such services without placing additional demand on GP practices.
Impact on the Demand Optimisation Programme
Clearly the need for appropriate lab testing remains and is arguably much more important given the capacity limitations and clinical backlogs that have developed. It is also evident that new ways of working, including shifting focus on location and delivery will make both time and peer-based comparisons of test use difficult. The Atlas of Variation approach modelled previously within the programme will need a complete re-focus to fit this changing landscape. The challenge therefore for the programme going forward will be to re-engineer itself post COVID-19 and develop appropriate monitoring metrics and associated interventions to help ensure laboratory test use is optimised.
A Re-Engineered Demand Optimisation Programme
Healthcare provision is re-engineering itself to fit the new "normal". The Demand Optimisation programme also needs to re-engineer itself to focus on issues facing the Scottish NHS as it emerges from lockdown. A backlog in appropriate investigations is likely to have developed, however clinical capacity to deal with such a backlog will be limited. The need to identify laboratory testing trends and provide appropriate testing guidance as services return will be important, however this will be a new normal comprising some of what happened before, some new ways of working and a "catch-up" element.
New Demand Optimisation Programme objectives:
1) Source data and observations from all boards/networks on the changes in healthcare infrastructure and provision as a result of the COVID-19 pandemic.
2) Collect discipline specific laboratory activity data for the main sources – Primary care, Secondary care and out-patients.
3) Estimate the "gap" in testing for different areas/disciplines – this is likely to relate to healthcare provision that was missed, delayed or postponed.
4) Histopathology – expected that workload will increase as catch up is attempted – needs monitoring and prioritized given the fixed capacity of services. Specimen type, volume of work and complexity needs tracking to assist prioritisation decisions.
5) Development of educational guidance as a matter of urgency, mainly via the networks, to roll out across healthcare settings – this needs to focus on avoiding samples as well as tests – the limitations are largely with patient interaction/phlebotomy, not with laboratory capacity (for blood sciences).
6) Atlas of Variation – needs a re-think – both to acknowledge and track the new post COVID-19 metrics, but also to allow peer comparison across boards, regions, clusters and nations. Such comparisons are likely to be single use rather than looking chronologically at what came before COVID-19. A Post-COVID-19 dashboard needs developing.
7) Focus on key areas such as cancer and diabetes where reduced testing during the pandemic is likely to have had a negative effect on individuals. Identification of specific requesting patterns that have failed to catch up.
A new era for Demand Optimisation
The COVID-19 pandemic has had a dramatic impact on the delivery of healthcare across the UK and will continue to do so as new ways of working are embedded long term. Clearly there has been a significant gap in provision as a result of delayed investigations and treatment, however the ability of the already stretched system to "catch up" will be limited – especially if social distancing limitations on clinical interface capacity remain.
Laboratory testing remains an especially important part of healthcare delivery and given limitations of the overall NHS system combined with the likely increased demand, it is vital that capacity and resource use are optimised. Demand optimisation of such processes affecting the whole "vein to brain" pathway is even more important than it was before but needs to be re-engineered to interface with the new challenges now being presented. This should now be seen as a priority for Laboratory Medicine and the wider NHS.
Contact
Email: Caroline.Ballantyne@gov.scot