Adult social care: independent review
The Independent Review of Adult Social Care in Scotland was led by Derek Feeley, a former Scottish Government Director General for Health and Social Care and Chief Executive of NHS Scotland. Mr Feeley was supported by an Advisory Panel comprising Scottish and International experts.
Chapter 7 A new approach to improving outcomes – closing the implementation gap, a new system for managing quality
"Self-directed support is absolutely the right policy but there has been a failure of implementation.”
"Elements of an ideal model of social care would include suitable housing, investment in training, technology enabled care, capacity building in communities, funding for community rehabilitation, and a shift away from crisis intervention to a much earlier more enabling, person centred, model of care.”
What is high quality social care support and where do we find it?
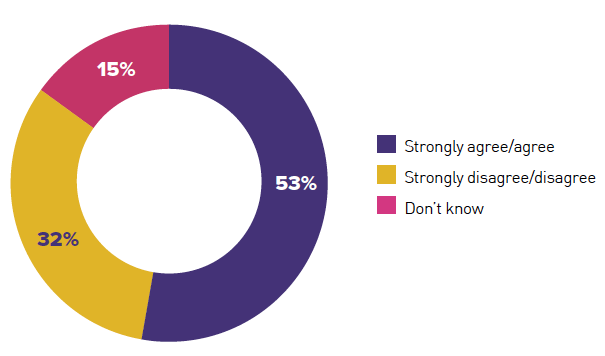
The quote about self-directed support from one of the participants became a recurring theme in our engagement process. People recognised the ground-breaking legislation to introduce initiatives like self-directed support but were frustrated by both the pace and the variability of implementation. The recent report by Self-Directed Support Scotland (SDSS) and the ALLIANCE[29] provides evidence to back up the assertion. As the charts below show, only 53% of people felt prepared for their needs assessment and only 42% felt that they had all self-directed support options discussed with them:
"I felt prepared for my needs assessment"
(My Support My Choice (Health and Social Care Alliance Scotland
and Self-Directed Support Scotland, Chart 11)
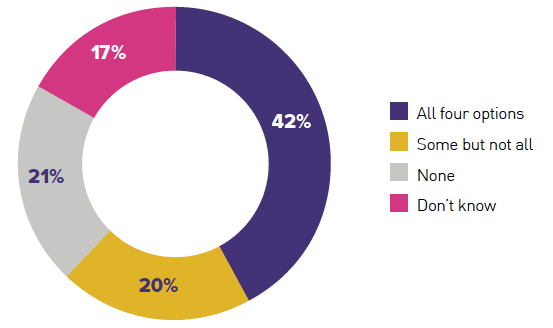
"Discussing SDS Support with Professionals"
My Support My Choice (Health and Social Care Alliance Scotland, Chart 12)
We heard similar perspectives shared with us on the impact of the Carers Act. Furthermore, the Audit Scotland Report on progress with implementation of health and social care integration[30] explores a consistent set of themes, describing progress in some areas but a good deal of variability.
The underlying reason for these challenges lies in the fact that we have no systematic approach to implementation and improvement in social care support. One widely used system of improvement is built on five components, all of which we'll cover in the report (adapted from Langley et al, The Improvement Guide, 2009):
- Establishing constancy of purpose;
- Gathering intelligence for improvement (establishing whether and how people's right and needs are being met);
- Taking a systems approach (seeing the interdependencies between the various parties);
- Planning for improvement (commissioning and investing in the right activities); and
- Learning from a portfolio of improvement programmes (a way to share learning across the country).
In chapter 2 of the report, we described what we believe to be the purpose of social care support in Scotland. Simply stating the purpose is not enough, however, to secure constancy in pursuit of the purpose. That needs an environment and culture that enable everyone in the system to contribute every day to the achievement of the purpose. We explored with people what might be the key elements of that supportive culture. Amongst the issues that were identified were: a focus on long term outcomes, an environment of co-operation and trust, valuing lived experience, replacing judgement with learning, and backing that up with a proper stewardship of our resources.
In the remainder of this chapter, we will set out recommendations for a system of improvement. We will propose how to close the implementation gap in a way that is rights based, systematic, planned, prioritised and continuous. But before we get to how we are going to improve, it is useful to spend some time on the question of what. Our remit specifies that we are to "recommend improvements to adult social care support in Scotland, primarily in terms of the outcomes achieved by and with people who use services . . ." In short, we are invited to improve quality. Don Berwick, former Administrator of the Centres for Medicare and Medicaid in the Obama Administration, describes quality as the degree to which the results of the work you do match the needs you intend to meet. What people have been describing to us as they talk about SDS etc., is a quality gap. This is how we go about closing the quality gap.
First, we need a workable definition of quality in social care support. A statement of its essential dimensions. There is already a lot to build from here. Principally (but not exclusively), we currently describe high quality social care support through 5 Health and Social Care Standards, 146 Standard Statements, 9 Health and Wellbeing Outcomes, and 23 Integration Indicators. Through a process of well-intentioned accretion, we have a situation now where we could not find a single shared definition of social care support. On the basis of our feedback from people receiving support and those providing it, we have created the following distillation of high quality social care which we recommend is deployed across the system to help understand people's experience of social care supports, alongside measures of the kind recommended in Chapter 6, whether the person is receiving support to live at home or is in a care home:
6 Quality Dimensions
- Accessible – I get the support I have a right to receive when and how I need it.
- Personalised – I am able to direct my support and I am a full partner in its planning.
- Integrated – if I need care, it is joined up. I get the help I need to navigate.
- Preventative – my needs are understood and addressed at lower levels, they are anticipated and I have a plan for the future.
- Respectful – I can live with dignity and my voice is heard.
- Safe – I feel safe in my environment and free from harm.
Creating the conditions for improvement – infrastructure and culture
There is an old Palestinian saying which goes something like "you can't fatten a cow by weighing it". It has shades of the recommendations made by W Edwards Deming[31]. As Deming points out, inspection is too late. The quality, good or bad, is already in the product or service. You cannot inspect quality into a product; instead you have to reduce the need for inspection on a mass basis by building quality into the product in the first place.
It is important to note Deming's use of the term "inspection on a mass basis." He doesn't call for the elimination of inspection altogether, but rather for its reduction to the optimal level. Some inspection is always necessary, and is an important tool for gathering intelligence about what and how you are doing, as well as what needs to be prioritised for improvement. We also recognise and value the regulation role at individual practitioner and service levels. But wholesale reliance on inspection is seldom appropriate, and is costly in both time and money. And most important, inspection cannot always catch problems that are inherent in the system itself.
And yet, that is pretty much all we have in social care support a total reliance on external verification as a vehicle for improvement. It won't work. It distorts our sense of who is the 'customer' away from the person in need of care and support towards the inspector and it inhibits the sharing of learning and innovation.
Our social care support system is crying out for the kind of step change that the Scottish Government made with the National Health Service back in 2007 when they introduced the Scottish Patient Safety Programme as a means to secure large scale national improvement in outcomes for patients. The programme has become a world leader, replicated across the world, and achieved a significant breakthrough in the quality and safety of the NHS in Scotland.
We recommend that creating a similar approach to national improvement in social care should be a key responsibility of the National Care Service. The National Care Service should utilize the intelligence generated from the Care Inspectorate's work to identify a number of areas where national performance is currently falling short of our expectations. It should set aims for the improvement required then commission the Care Inspectorate and Healthcare Improvement Scotland to design and develop a collaborative improvement effort to generate the level of performance required. Those two organisations should engage with providers, people with lived experience and unpaid carers to agree a set of changes and build the necessary local improvement capacity and capability.
We recommend that just as Healthcare Improvement Scotland sits within NHS Scotland, so too should the Care Inspectorate be part of the National Care Service. We further recommend that it should work in partnership with Healthcare Improvement Scotland and the two organisations should create complementary functionality rather than compete or duplicate. In social care national improvement programmes, the Care Inspectorate can bring subject matter expertise and the quality improvement input can be provided by Healthcare Improvement Scotland.
Their role in the development of quality improvement activities will require a rebalancing of the Care Inspectorate's role, building on the current strategy, energy and direction of travel. It will be a key contributor to the quality planning that will be carried out in the National Care Service. Elsewhere in this report, we propose an important new role for the Care Inspectorate in relation to market oversight. In order to create space for these new functions, we recommend that the Care Inspectorate shifts some of its quality assurance activities to the Integration Joint Boards and to providers, involving people using services and carers in improvement and quality assurance work. The Care Inspectorate and Healthcare Improvement Scotland should be held jointly accountable for the planning and delivery of improvement programmes.
Building capacity and capability
These new approaches and quality improvement methods will require a significant building of improvement capability at the point of social care support. Staff in care homes, for example, will need basic improvement knowledge. In addition, we will have to create some kind of quality improvement infrastructure for this work.
In order to manage the impact of the Covid-19 pandemic, the Chief Nursing Officer for Scotland and her team have led work to develop what they call a 'safety huddle tool' in care homes. This has generated daily intelligence on the current situation in all care homes across Scotland and has potential as an important building block for the kind of quality improvement infrastructure we might require.
In the United States, The Agency for Healthcare Research and Quality (AHRQ) is partnering with the University of New Mexico's ECHO Institute and the Institute for Healthcare Improvement (IHI) to establish a National Nursing Home Action Network. The network aims to provide training and mentorship to 15,000 nursing homes across the country via over 100 geographic hubs to increase the implementation of evidence-based infection prevention and safety practices to protect residents and staff. A similar model could be used to build on the success of the 'daily huddle'.
Robert Faulds
I had addiction issues and was on methadone for 18 years and I was a heroin addict for a couple of decades. It stole a good part of my life. Now I volunteer at the treatment centre, which helped me get clean and I also work a 12 step programme with a sponsor which has changed my way of thinking.
Having to go to the chemist for methadone, is brutal. Going through the door at the chemist made me feel like less of a person, a second class citizen. I had a terrible self-hatred, there was no exit strategy. I thought I would die in addiction and although I would have accepted that, I couldn't accept it for my daughter, she never chose this situation.
We're dying out there, my pals are dying out there and we are trying to get treatment but it's hard to get treatment. I just needed some guidance, and the structure that Rainbow House, a recovery service in Glasgow, gave me.
I needed time to breathe and process the things that had gone on in my life. My life transformed in seven months. If I wasn't for that service, I would likely be dead.
I now volunteer at Rainbow House and I plan to work in addictions, in the future. I've got a beautiful daughter and a lovely family and I believe my life is going to be good. A big part of recovery is hope. Most people don't know what recovery is, we need to make it visible, we need to give it direction.
"We’re dying out there, my pals are dying out there and we are trying to get treatment but it’s hard to get treatment.”
Recommendations
We make the following recommendations:
27. A National Improvement Programme for social care, along the lines of the NHS Patient Safety Programme, should be introduced by the National Care Service, and should address the three following key areas:
- The experience and implementation of self-directed support must be improved, placing people using services' needs, rights and preferences at the heart of the decision making process.
- The safety and quality of care provided in care homes must be improved to guarantee consistent, appropriate standards of care.
- Commissioning and procurement processes must be improved in order to provide a vehicle for raising the quality of social care support and for enhancing the conditions and experience of the social care workforce.
Contact
Email: Donna.Bell@gov.scot