Adult social care: independent review
The Independent Review of Adult Social Care in Scotland was led by Derek Feeley, a former Scottish Government Director General for Health and Social Care and Chief Executive of NHS Scotland. Mr Feeley was supported by an Advisory Panel comprising Scottish and International experts.
Chapter 1 What we heard
"... it should feel nurturing and supportive, rather than a battlefield.”
This review is about people's experiences of social care support, whether you use social care services and supports, care for someone who uses them, or work in them. It has been our priority to hear from as many people as possible, to listen to your experiences and to learn from your ideas. To make that happen, we have carried out an engagement programme focused on three kinds of activity:
Open enquiry – From September to November 2020, individuals and organisations could submit views, papers and evidence to the review.
Stakeholder engagement events – From September to November 2020, stakeholder engagement events were held with the support of the Health and Social Care Alliance Scotland (The ALLIANCE[1]). Each event had a particular focus such as learning disabilities, physical disabilities, mental health and dementia, addictions and the experience of carers.
Meetings with key stakeholder groups and organisations – From September 2020 to January 2021, the Chair of the review, members of the advisory panel and members of the review Secretariat attended meetings to hear from key stakeholder groups and organisations, and from people who work in social care support services.
The quotes you will find at the start of each chapter in this report are from individuals and organisations who participated in our programme of engagement, and who have lived experience of either using social care supports, or working in social care services.
Our programme of engagement, most of which took place online, resulted in:
- 228 Written submissions
- 13 Engagement events
- 128 Meetings with stakeholders
In total, we met over a thousand people in just a few months, and we are grateful to you all for your time, insights and wisdom.
This review was commissioned by Scottish Ministers in response to the experience so far of Covid-19, and we of course heard about people's experience of care during the pandemic.
We heard some positive experiences of the sector's response to Covid-19, including how quickly providers adapted to new and very difficult circumstances and a heightened public awareness, in time, of the vital work of the sector. Some people who work in social care support mentioned to us that during the pandemic they have been able to make decisions more quickly, to good effect. Inevitably, we heard of many negative experiences too: people who had been affected by the impact of the pandemic on care home residents and staff, people whose community-based supports had been reduced or entirely stopped, pressures on carers and providers and the impact on people's physical and mental wellbeing.
However, this is not "just" a review of social care during Covid-19 and all that we have learned from it. It takes into account all the different types of support and care that are provided in a range of settings, including residential settings such as care homes and in people's own homes, and it covers care and support for a broad range of people with long-term conditions, older people, people with physical disabilities, people with learning disabilities, people with mental health problems, people with addictions, and people with experience of the criminal justice system. This review covers all of these life circumstances, and takes account of people's experiences over many years.
Because our remit is so broad, it was vitally important that we listened to people's experience of the full spectrum of adult social care services and supports. We have summarised the key themes we heard below. You can read a full report on the engagement events here: Independent Review of Adult Social Care – Engagement report.
"Service design and delivery can only improve if people with lived experience are involved in the process. It is impossible to address inequality if the people who experience it are not in the room.”
Key Themes
Access, eligibility and assessment
People told us about the transformative impact that "good" social care services and supports can have – and in many cases have had – on their lives and the lives of people they love. We heard about the dedication and responsiveness of people in the workforce; about self-directed support enabling people to "live a real life"; about integrated health and social care support services that work together well, jointly focusing on the wellbeing of the person using care; and about carers being supported to carry on caring for loved ones.
But we also heard a lot of frustration about the existing structure and design of social care. People feel that the term itself – social care – is too often used negatively, to mean services that are for people only when in crisis, that just prevent or delay a deteriorating situation, or are a buffer to absorb pressure that would otherwise fall upon the NHS. People told us that social care support should instead be understood as an asset that provides constructive, optimistic support to help people achieve their goals and desired outcomes: to live their best lives and maximise their wellbeing, as equal citizens.
We heard that our current system too often does not feel like a system at all: it feels like a guddle, and that causes people worry and anxiety. For people with care and support needs and their families the challenges of accessing support, only to find they are unavailable or unaffordable, or those seeking support are ineligible, causes unnecessary suffering and hardship. This is not a humane response to people living with disability or ill health, or who are simply getting older and are no longer able to live their lives without some support. For family members it means having to take on heavy responsibilities for caring. Some try to juggle this alongside work, but many give up, putting themselves into a precarious financial position. For staff it can lead to burnout, with the constant stress of having to respond to crises, and the feeling that whatever you do it is not enough.
People described the process of accessing social care as 'notoriously difficult', 'over-complicated' and 'bureaucratic'. When experiences had been negative, people told us that they had to 'fight for' and 'justify' their right for support. We heard that accessing social care is sometimes too difficult right from the start, with an inadequate referral process and not enough information available about supports, including peer support.
Eligibility criteria were described as one of the main barriers to accessing social care.
People also told us that the threshold for accessing support is too high, and too often meaningful support is only available when people are acutely unwell or in crisis[2][3] . We heard about the negative impact this has on the mental and physical wellbeing of people using social care support, their carers and the workforce.
We heard that the assessment process is too often based on a medical model focused on deficits – the things people cannot do – with little or no account taken of holistic and social needs; that it is too complex and takes too long; and once it is completed it takes too long before support is available. Some people with complex needs, including neurological conditions and sensory impairments, told us that their experience of assessment was that not all social workers had enough training in their functional difficulties.
In order to improve, people told us that social care needs to focus on holistic wellbeing and personal outcomes, rather than outputs and money. It should be flexible so that it can adapt to changing needs and wishes. It should take account of wider supports in a person's life, such as the support of carers and local services offered by community organisations to enable people to fulfil their potential, goals and outcomes, without reducing appropriate formal supports and shifting a burden of care onto families and informal networks. Assessment should be simplified and based upon collaborative engagement with the person's needs, rights and preferences at the centre.
Structure and design of services
We heard that recent changes across health and social care have produced improvements, especially in some parts of the country, but there is much more to be done. People told us that Integration Joint Boards have had benefits in terms of health and social care support services working together better locally, but in many instances people need to be much more directly involved in planning their own care, and in decisions about local priorities.
We heard that national and local services need to work together better, that transitions between children's and adult's services must improve, and so should joint working with other services such as transport, housing, education and employment.
People told us how frustrating they found it to be asked to repeat the same information to several different professionals when better data sharing arrangements would remove the need.
We were told consistently that Scotland needs to shift its attitude towards technology and data sharing to improve people's experience of social care. Technological solutions should of course never be "forced" on people as a substitute for other kinds of care, but experience during the pandemic has highlighted that, for some people, technology can really help people to live independently in their own communities and to feel less lonely.
Technology is not a replacement for support provided by another person but it can play a much bigger role in improving the lives of people who use social care services and supports. It can also help with people's ownership of their care and support, particularly when people "own" their own data or information that is about them and share it with the people who support them.
Planning, commissioning and procurement
Many people told us that Scotland has 'good strategies but poor implementation'. This 'implementation gap' was often referred to in terms of the differences between what is set out in legislation and guidance and what actually happens on the ground. We were also told about places and local teams that are good at follow-through from intention to service delivery, but with a sense that where that was people's experience it was partly because they were 'lucky'. More generally, people described current planning, commissioning and procurement processes as 'discredited', with poor outcomes for people who use services and for the workforce. Some people felt that Integration Joint Boards had made some improvements on this but a significant number of people we spoke to had serious concerns. Currently, Integration Joint Boards do not have responsibility for procurement or contracts.
We heard that the market approach to commissioning and procurement produces 'competition, not collaboration', which, in turn, leads to too much focus on costs rather than high quality, person-centred care and support. We were repeatedly told that this focus on costs causes poor terms and conditions, including pay, for the workforce.
People spoke to us about 'short-termism' resulting in providers spending significant time and resources applying and reapplying for contracts. This results in uncertainty for providers and the workforce, which makes it difficult to attract and retain staff. Providers cannot afford to have staff 'waiting in the wings for contracts to come along'. We also heard that commissioning using generic frameworks based on hourly rates does not work well for people with fluctuating needs for support, particularly where those relate to mental health.
Just as with individual care planning, people told us that local communities and third sector organisations should be more involved in collaborative approaches to planning, commissioning and procuring social care support services. Where people felt that they had had a good experience of using self-directed support they often also described good collaboration between organisations, communities and individuals in the design and delivery of care and support.
And we heard repeatedly that simpler and more accessible arrangements to challenge decisions – without recourse to the Courts – need to be established.
We refer to commissioning and procurement practices throughout this report, and Chapter 9 is dedicated to the subject. These are fairly technical terms and it may be helpful to explain what we are referring to at the start. Commissioning is the process by which public bodies strategically plan ahead for the services they will provide, either directly or by procurement, to meet their populations' needs, using the budgets at their disposal. Procurement is the process of contracting for (purchasing) specific services on the basis of that commissioning activity. It is important to note that not all commissioning activity results in procurement and that commissioning decisions and priorities should form the basis of any procurement process – never the other way around.
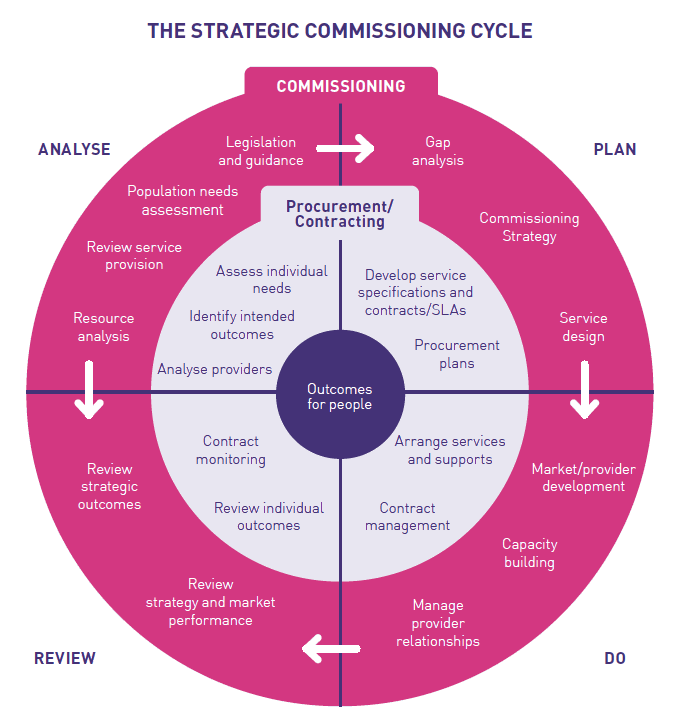
Most models of commissioning emphasise its cyclical nature, with strategic commissioning providing the context for procurement and contracting. The cycle is sequential and each part is of equal importance. A key principle of the commissioning process is that it should be equitable and transparent, and therefore open to influence from all stakeholders via an on-going dialogue with people who use services, unpaid carers and providers. Outcomes for people are at the centre of the model, which is commonly illustrated in the diagram shown here (originally developed by the Institute of Public Care at Oxford BrookesUniversity).
This diagram of course does not take account of our proposals for ethical and collaborative commissioning. It could usefully be updated to reflect those as work progresses.
Workforce
Despite challenging circumstances, we heard repeatedly that the social care workforce are 'motivated', 'resilient', 'adaptable' and 'proud of their work'. However, a range of serious concerns were raised.
People told us they are worried about 'casualisation' of the largely female social care support workforce, which is both undervalued and underpaid as a result, despite their essential work to improve people's lives and wellbeing, and support their independence, every day.
We frequently heard that people 'could earn more working in a supermarket', and people also spoke to us about a lack of support and training opportunities with sometimes serious consequences for people who use services. This need to improve the skillset of the workforce was reported to us in various ways. People with complex needs or sensory impairments told us they could not get appropriate support. We heard about assessments being inadequate because assessors do not have sufficient training to understand people's circumstances. People told us that sometimes the full range of options available under self-directed support are not adequately explained. And employers told us that the lack of training and career development opportunities makes it difficult to attract and retain staff, which makes it difficult to establish rapport and trust between people who use social care support and their carers. At the same time, it was brought home to us many times that social care support is highly skilled and that many people in the workforce are very experienced. The fact that people who work in social care are undervalued and underpaid in no way correlates either with their skillset or importance to society.
Some people had specific ideas for how to improve the experience of the workforce, such as a national campaign to promote the value of social care support and help make it a more attractive career choice; a minimum wage for social care workers, with some suggesting £15 per hour; implementation of the Fair Work principles to improve workers' working conditions; peer support and supervision; and a more consistent approach to providing high quality training for staff.
Unpaid Carers
Unpaid carers were very clear with us that they want to care, and care well. But like the workforce, they told us that they are simultaneously undervalued by society and given 'all the responsibility without the support, resources or recognition'. We heard that carers are often unaware of their rights and the support available to them. Accessing support, whether for respite services or advice, was often described as 'complex', 'time consuming' and 'frustrating'.
Carers told us that respite is not always recognised as essential support. Without respite, some carers are 'on the job' 24 hours a day, which is unsustainable, unfair and limits their own life opportunities. Sometimes, we were told, inappropriate respite is offered, such as taking cared-for people into unsuitable care homes.
We also heard many carers reflect on the gender issue that also applies to the paid workforce. Many unpaid carers are women, and they told us they are often overlooked and disregarded.
Registration, regulation and inspection
We heard mixed views on current arrangements for regulation and inspection of social care support services. Some good examples were described to us of meaningful dialogue and engagement with the Care Inspectorate, illustrated with observations like inspections being based on dialogue and improvement. On the other hand, we heard that too much attention is paid to procedural and process issues and not enough to individuals' experience of care and how social care connects people with their communities.
People told us that there is a clear accountability gap between national and local levels, and that there is not meaningful joint inspection of health and social care support services. We also heard that there is significant duplication in the information requested from services by the Care Inspectorate and local commissioners, which wastes time that could be better used to improve quality. Many people emphasised the need for much more support for locally driven improvement work to raise standards of care. Where members of the workforce had taken part in local improvement work, they expressed pride and satisfaction in the progress made, and they wanted to do more of it.
On registration, regulation and support for the workforce, we heard that the Scottish Social Services Council is not equipped or resourced to support effective training and development of staff. We listened to general observations that the workforce too often feel policed rather than supported as a consequence of current registration arrangements. We also heard particular concerns about the absence of support for, and regulation of, personal assistants, and failure to extend training opportunities for the paid workforce to unpaid carers.
Equality
Equality – and inequality – were raised with us again and again.
Some people who use social care services and supports told us that they are expected to pay to access their human rights: to carry out normal day-to-day activities such as washing and getting dressed, and going to work.
We heard about gender unfairness, as before; that the needs, rights and preferences of people from minority ethnic communities are often overlooked; that communication support for people with sensory impairments and learning disabilities is often inadequate; and that the stigma sometimes attached to accessing supports for mental health problems, addictions and criminal justice issues should be addressed.
We also heard that advocacy arrangements need to be improved, so that people with incapacity and others who are accessing supports and services have their needs, rights and preferences properly represented.
National Care Service
Many people asked what would be meant by a National Care Service, which the First Minister mentioned when she announced this review in the Programme for Government.[4] In response we asked the people we were talking to what they thought such an idea should and should not mean.
There was a wide variety of views about what a National Care Service should represent. Points mentioned frequently included: social care services should not be run for profit as a matter of principle – different rules should not apply to social care support compared with the NHS; charges, if any, should be fairer and the same in different Local Authority areas; assessments and care packages should be portable between Local Authority areas; and the workforce should be better supported with effective planning, training and support arrangements consistently managed at national level. We asked what would worry people about a National Care Service, and the most frequently mentioned concern was that it would bring loss of local knowledge and expertise. Many people said they thought a better mix of national and local responsibilities and activities was needed.
Having listened carefully to the experiences, views and ideas so generously shared with us, we have set out our proposals for reforming adult social care in Scotland in the remainder of this report.
Susan McKinstery
I think the public don't realise, that when you depend on care services for your most fundamental rights and needs, that can put you in a very precarious position. The fact that services can be taken away by someone who often doesn't know you or understand the complexity of your situation is such a violation.
You are made to feel guilty for asking for help and you have it driven home to you that resources are limited and there are people with greater needs than yours. The result of this is that you are given the sense that by accepting support, you are taking resources away from someone more deserving. Nobody should be made to feel like that. We need a system based on rights and aspirations of individuals and one which is adequately funded and structured in a way which allows these to be upheld. Those who need support to live fully and to navigate the real-world barriers they face should be able to ask for that support without guilt or the endless need to justify themselves. Care itself shouldn't be yet another barrier.
Ultimately, I believe we need more people with lived experience of social care in positions of power and influence. Those of us who have experience of the system from this perspective know the importance of not only involving people in decisions which affect their lives but, importantly, believing them as experts in their own needs. As the saying goes, nothing about us without us.
"Those who need support to live fully and to navigate the real-world barriers they face should be able to ask for that support without guilt or the endless need to justify themselves.”
Contact
Email: Donna.Bell@gov.scot