Adult social care: independent review
The Independent Review of Adult Social Care in Scotland was led by Derek Feeley, a former Scottish Government Director General for Health and Social Care and Chief Executive of NHS Scotland. Mr Feeley was supported by an Advisory Panel comprising Scottish and International experts.
Chapter 11 Finance
"The key issue affecting the social care sector is lack of funding.”
As we said at the beginning of this report, we have deliberately not started with finance. We felt it was vitally important to conduct this review from the perspective of people's experience of adult social care support, and the role adult social has to play in Scotland's wellbeing as a whole.
Nevertheless, we must come to money in the end. The proposals we have set out here do not come without cost: but nor are they only about cost. There is clear evidence that social care support is not a drag on our resources; it creates jobs and economic growth. It enables people who access care and support, and their carers, to seek and hold down employment themselves. Accordingly, a major thrust of this section of the report is to describe the investments required to create a system of social care support that will enable everyone in Scotland to get the social care support they need to live their lives as they choose and that promotes and ensures human rights, wellbeing, independent living and equity. As we consider money, we want to reiterate the importance of replacing old thinking with new thinking. Investing in people is beneficial to society: it is an investment in ourselves and one another. As a system, we need to consider investment choices through the constructive, empowering focus of a new mindset:
Old Thinking:
Social care support is a burden on society
Managing need
Available in a crisis
Competition and markets
Transactions
A place for services (e.g. a care home)
Variable
New Thinking:
Social care support is an investment
Enabling rights and capabilities
Preventative and anticipatory
Collaboration
Relationships
A vehicle for supporting independent living
Consistent and fair
In this chapter we set out a brief analysis of current expenditure on adult social care; opportunities to spend money better; our recommendations for additional investment; the evidence to support our assertion that that expenditure is itself an investment; and finally some options for raising money to support these changes. We have by necessity used a number of proxies in this assessment to help us "size" the level of investment we think is required. These proxies are often not ideal: for instance, delayed discharge is in many ways an "old thinking" measure, but we have used them here as the best mechanism available to us to understand what needs to happen.
Current expenditure on adult social care
In 2018/19 expenditure on formal adult social care in Scotland was £3.8bn:
- Most funding came from the public sector (84%), with the balance from individuals through Local Authority service charges and self-funding of care home places by residents.
- Almost two thirds of expenditure was on services for older people.
- There was marginally more expenditure on community based services (54%) than on accommodation based services.
In addition, the economic value of the contribution made by carers is estimated to have been £36bn[45].
"Social care is not funded in a way which is sustainable or supports transformation of services.”
Total adult social care funding and expenditure of £3.8bn are illustrated in this chart:
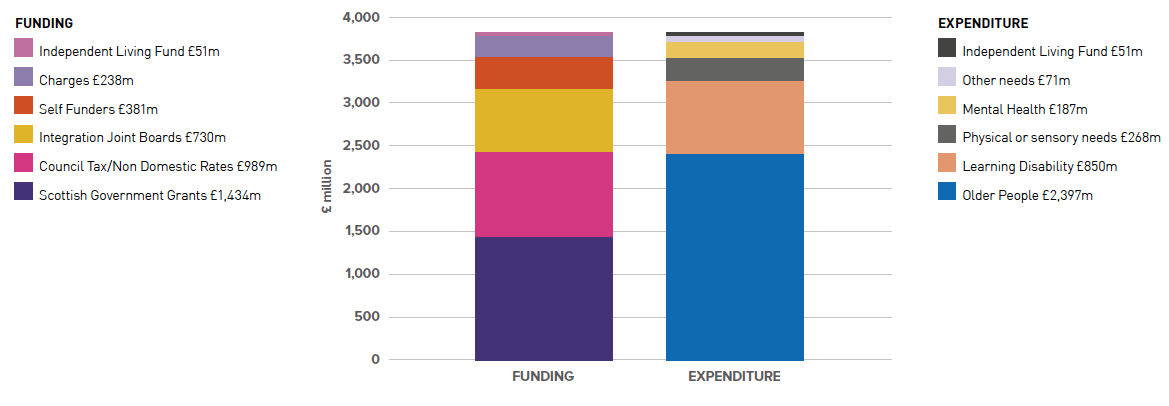
Most of the funding came from the public sector (84%) with the balance coming from individuals through Local Authority service charges and self-funding care home residents.
Related expenditure, on community based health services and unplanned hospital care, which are under the control of Integration Joint Boards, totalled £6.1bn in 2018/19.
The proposals we have set out earlier in this report relate to total health and adult social care expenditure of Integration Joint Boards.
In 2020/21 the Scottish Government became responsible for social security payments, with budgets for adult benefits totalling £3bn. There is considerable overlap between people who use social care supports and people who access benefits, but not everyone who uses one uses the other.
Opportunities to spend money better
Costs arise in our current system because social care supports are often too focused on crisis management and late intervention, and not enough on prevention and empowering people to live fulfilling lives. Costs like these are borne not only by the public sector, but also by people who use social care support[46] and their families and carers, and many are avoidable. We have not carried out an extensive analysis of these costs, but we have looked at examples that we recommend a National Care Service should consider carefully for opportunities to improve. We are not suggesting that the money spent on these areas of activity is currently wasted: we are suggesting that with more effective care planning and delivery it could in some instances be put to better use to support people more effectively:
- Delayed discharges accounted for 542,000 bed days in 2019/20, i.e., 8.9% of all beds in NHS Scotland, costing £134m[47]. We know that being delayed in hospital when someone is ready to go home is bad for their wellbeing.
- There is significant variation in the length of time people spend in hospital in the last six months of their lives. In some circumstances, hospital care is exactly right for people nearing the end of life. In other cases, more time could be spent at home, which is what many people want, if better support were available. The average length of stay in hospital in the last six months of life varies by 66% across Integration Joint Boards. In total, hospital care in the last six months of life amounted to 1.1m hospital bed days in 2019/20, i.e.,19% of all beds[48].
- Similarly, there is significant variation in models of care and hospitalisation rates for people with dementia[49], the costs of which in total are £2.6bn per year[50].
- In 2019/20, £58m was spent on out-of-area care home placements for adults with learning disabilities, for reasons other than choice, at a median cost per placement of over £87k[51].
- Waiting times for adult social care carry a significant burden for people who need support. In 2017/18 the proportion of people with substantial or critical needs waiting more than six weeks for a community care assessment was 7% and 8% respectively[52]. Recent analysis suggests that in 2018/19, older people had 20% fewer unplanned admissions to hospital in the six months after receiving homecare support than in the six months prior.
Additional investment
In this section we cover a number of areas in which we believe additional investment in adult social care is needed.
Expanding access to social care support and investing in prevention
Despite the fiscal effects of austerity in recent years, Integration Joint Boards and Local Authorities have increased expenditure on adult social care in real terms since 2009/10 by 7% in total and by 5% per capita. This is in contrast to the position in England, where expenditure fell in real terms by 1% and 6% respectively[53].
As the older population has increased and resources have been focused increasingly on those in greatest need, a smaller proportion of the adult population is in receipt of social care support than was before austerity, with the result that the needs of a number of people are probably not being met and for others they are being met in a crisis response rather than to anticipate or avoid such interventions. Some of this reduction may reflect substitution of formal services with asset based approaches[54], and some may be the result of genuine reduction in need as other supports have improved people's lives, but this is difficult to quantify. As approximate as the evidence available to us is, it nonetheless suggests to us that there is an opportunity to invest more than we do currently in preventative care that can yield benefits for individuals and the system as a whole.
To assess the extent to which there are opportunities for better investment in social care support, the Scottish Government is currently carrying out a detailed analysis exploring the determinants of social care service use across data-zones. This is important work and we are reassured that it is underway. Its results are not yet available so for the purposes of this report we have carried out a higher level assessment as follows:
- A longitudinal analysis that used 2009/10 service use data to calculate the expected number of people using social care support in 2018/19, and compared those to the actual number.
- An analysis of variation across Integration Joint Boards to calculate the expected number of people using social care support in 2018/19 based on standardised Scottish average rates (i.e. adjusted for differences in age/sex and morbidity and life circumstances), and compared those to the actual number.
We found that there were 25,505 fewer people (20%) receiving care in 2018/19 than expected based on 2009/10 levels of access. We estimate that it would cost around £288m to cover that "gap". In addition, there were 10,412 fewer people (10%) receiving care in 2018/19 than expected based on the standardised rates. We estimate that it would cost around £148m to cover that "gap". With the caveats noted above regarding the difficulty of interpreting this data, we therefore estimate that there may be approximately 36,000 people in Scotland who do not currently have access to social care support and for whom it would be beneficial, and that it would cost about £436m to meet this need. We recommend investment in social care is increased in order to expand access to social care support.
We have discussed elsewhere the importance of community connections and low-level preventive support for people, and suggested that Integration Joint Boards should commission and grant-fund community organisations.
Fair Work
Our recommendations include implementing the findings of the Fair Work Convention. Investing in Fair Work is an investment in Scottish society, which helps to drive national and local economic growth as well as, in this context, a fair reflection of the importance of the work done in social care supports. We make a clear link between the importance of remunerating the workforce fairly, commissioning social care support ethically and collaboratively, and making good use of available public resources.
We have calculated the costs we anticipate associated with increasing the Real Living Wage to £9.50 per hour, along with ensuring it is paid to all staff working in adult social care support. Increasing the Real Living Wage to £9.50 per hour for frontline adult social care staff would cost £15.5m p.a.. This estimate includes staff working in care homes, home care and housing support, day-care, adult placement services, personal assistants and sleepovers. Extending the Real Living Wage to include auxiliary staff working in adult services would cost an additional £4m p.a.. As discussed in Chapter 10 on Fair Work, we acknowledge that trade unions representing the workforce are keen to exceed the Real Living Wage and are calling for an uplift to £15 per hour. The costs associated with implementing the Real Living Wage represent the 'floor' rather than the 'ceiling'. More accurate assessments will require the job evaluation process described earlier in the report. But in broad terms, every pound beyond the Real Living Wage will increase the national social care support wage bill by about £100m per annum. Of course, there is also a debate to be had about who should bear those costs and how they should be factored into contracts and commissioning.
Removing charging for non-residential social care support
Our "new thinking" approach extends to what is fair and right for people receiving social care supports in their own homes. People should no longer be charged for non-residential social care support such as care and, support at home, and day care. It does not make sense for people to have access to health care free at the point of need but, in circumstances that are equally related to their health and wellbeing, to be charged for support. It also does not support delivery of their human rights.
In 2019/20 Local Authority income raised from non-residential user charges was £51m. We know from the experience of introducing Free Personal and Nursing Care that the removal of charges may lead to increased use of services. We therefore suggest that planning for the removal of non-residential charges should take account of the likelihood of increased use.
Free Personal and Nursing Care for self-funding care home residents
The removal of charging for non-residential care should mean that the only cost for people in receipt of social care should be the means tested accommodation costs for care home residents. However, in recent years the cost of providing Free Personal and Nursing Care has increased significantly and the payment made to providers by Local Authorities for self-funding residents has not kept pace with this. This is not an issue for Local Authority funded placements covered by the National Care Home Contract, which contains reasonable provision for the cost of Free Personal and Nursing Care.
Using the National Care Home Contract as a benchmark, the difference between the costs included for Free Personal and Nursing Care and the sums paid by Local Authorities for self-funders were £191 and £230 per week respectively in 2019/20. We recommend that the sums paid for Free Personal and Nursing Care for self-funders using care homes should be increased to the levels included in the National Care Home Contract, and that this would cost £116m p.a..
Care Home Accommodation Costs
Our recommendations mean that all people in Scotland will receive social care free at the point of need. The only costs that will remain are those for accommodation, either directly through fees for care home residents or indirectly through household costs for those receiving care in their own homes. Although in most cases these are higher for care home residents, they are in principle the same.
An individual's contribution to their care home accommodation costs is funded primarily through their own income, with the Local Authority making up the balance on the basis of a means test on the individual's assets. Below the lower limit the Local Authority meets all of the shortfall and above the upper limit the individual covers the total cost, by drawing down the value of their assets.
We considered whether it is appropriate for people to contribute to their accommodation costs in residential care, or whether this too should be free at the point of use. We concluded that it is reasonable for some charge to be made where the individual's means permit, because in other circumstances that person would be paying accommodation costs at home. The National Care Service could in future consider whether adjustments to the means testing arrangements that are used would introduce greater fairness, but we have not considered this complex question in detail during this review. It is worth noting that many of the alternative approaches suggested previously in the UK and overseas tend to be regressive in nature and we propose that any future work should exercise caution in this regard.
Re-opening the Independent Living Fund
The Independent Living Fund plays an important role in supporting its members' wellbeing and independence. The existing fund has 2,600 members and we estimate that there are a further 3,400 people who would be eligible for an award were we to re-open the fund and retain the existing threshold sum for access.
As indicated earlier in the report, we see the Independent Living Fund operating in future as part of the National Care Service. In effect, it will provide a national service of self-directed support to people with the most complex needs in the country. We recommend that the Independent Living Fund should be re-opened. To ensure that the Fund focuses on people with the most complex needs, we recommend that the threshold sum for entry to the new scheme should be reviewed and adjusted. To give some indication of the likely additional costs, if the threshold sum for new entrants was set at £600 per week, an additional investment of £32m would be required, increasing the total fund value to £85m p.a..
Unpaid Carers
In recognition of concerns we heard about the Carer's Allowance, and the impact of caring on some people's income, we recommend a review of financial support made available to unpaid carers should be taken forward. As part of its focus on improving support for unpaid carers, the National Care Service should also increase investment in a range of respite provision including options for non-residential respite, and for short breaks.
Although charges to carers are waived under the Carer's Act, some Local Authorities allocate charges to the supported person for respite. Removing such charges should be considered alongside other investment priorities.
Future funding
On top of the initial investment set out above, Scotland's ageing demography means that more money will need to be spent on adult social care over the long term. This challenge exists for the rest of the UK as well.
Based on Personal Social Services Research Unit (PSSRU) research[55] a reasonable starting point for projections is a 3.5% p.a. real increase in social care expenditure every year to 2035 in Scotland, but more specific Scottish projections will be vital in the future.
The Scottish Government's Health and Social Care Medium Term Financial Framework[56] includes an assumption of nominal growth rates for social care of 4% p.a. gross and 3% p.a.net of savings until 2023/24. Assuming 1.8% p.a. inflation, the growth rate in the Medium Term Financial Framework is currently 1.3% p.a. lower than the rate recommended by PSSRU. We recommend that future planning for investment in adult social care must factor in demographic change.
Spending on adult social care is an investment in the Scottish economy
When we add up the recommendations we have made above, the total annual additional expenditure we are suggesting is £0.66bn p.a., i.e., about 0.4% of Scottish GDP.
This is a 20% increase in real terms over 2018/19 levels and twice the total real terms increase in adult social care expenditure over whole of the previous ten years (£.3bn). Even allowing for a phased introduction, an investment on these lines will require a long-term and substantial uplift in adult social care funding.
We believe that the scale of this increase in funding is warranted on the human rights basis we have set out, and also that it represents a good investment in the Scottish economy and has a positive impact on women's employment and the gender pay gap:
- The social care sector directly employs 205,000[57] people, approximately 8% of the workforce, with 148,000 working in adult social care. In addition, a further 51,000 jobs are generated as a result of adult social care in other sectors. In 2019 women made up 83% of the workforce, and average earnings were 56% of Scottish average in 2016[58].
- The contribution of adult social care to the Scottish economy extends beyond the care sector. For every £1 spent on social care, more than £2 is generated in other sectors[59]. A recent report[60]estimates that an increase in social care expenditure of 1% of GDP would create three times as many jobs in the UK economy than it would if spent in the construction industry; and the sums recouped by the Treasury through taxes and NI would be 50% higher.
- The Women's Budget Group[61] estimates that the majority of new jobs created by investment in social care will be taken by women.
- Such investment generates social value. Through the combined influence of emotional wellbeing, health maintenance and sustaining natural support and prevention, social care has a direct, indirect and extended impact: a study of the Independent Living Fund in Northern Ireland estimates that every £1 spent generates £11 of social value[62].
- The Social Justice Commission[63] suggests that expenditure on care should be given an equivalence to investment in any other key sector, and should feature prominently in economic policy, not only in post-Covid economic and social recovery, but as a focus of investment supported through organisations like the Scottish National Investment Bank and economic development funding.
- Both for people who use social care support, and equally importantly for unpaid carers, the availability of high quality adult social care support can help people to engage in and remain in education and also to enter and remain in work.
The additional expenditure we are recommending here should not be seen in economic terms as a revenue cost but rather as an investment that encourages job creation and provides economic stimulus. It should play a key part in post-pandemic recovery plans, particularly in light of the Institute for Fiscal Studies' analysis that more women are likely to lose their jobs than men as a result of Covid-19[64].
Options for Raising Revenue
Should the Scottish Government accept our recommendations on investment, it will need to consider a range of options for generating new revenues. We have outlined broad ideas here, many of them drawn from an analysis of how other countries have gone about funding investments in their social care systems[65][66][67]. It is for the Scottish Government and Scottish Parliament, in due course, to consider what would be most appropriate. Broadly, the following options are available:
- Introduction of mandatory social insurance;
- Changes to existing devolved taxes to raise additional revenue;
- Introduction of a new local tax;
- Seeking devolved powers for a new national devolved tax in Scotland; and
- Seeking devolution of existing reserved taxes to raise additional revenue.
These options are not uniform in their deliverability. Scotland has no history of mandating insurance, people have been reluctant to insure against future social care need, and the insurance industry is not well prepared for a new market. Changes to existing devolved taxes or the introduction of new local taxes are within the competence of the Scottish Parliament, but would require careful assessment against the Scottish Government's wider tax priorities, and would have to be consistent with the Scottish Government's stated principles for taxation.
There are also a set of specific challenges when considering the options, in particular:
Equity and intergenerational fairness
Any funding mechanism should be progressive in respect of ability to pay. It should also be equitable between people of different age groups. This is particularly important with newly established funded schemes, where the demands on the fund from the elderly are likely to exceed their contributions in the short term.
Hypothecation and the visibility of any new funding mechanism
In the design of any new tax, it is important to consider the degree to which, if at all, new revenues would be hypothecated to protect funding for adult social care. Hypothecation is not commonly used in the UK. It could constrain future options and impact the extent to which funding could adapt over time to meet demand.
There is evidence of public support[68] for hypothecation to fund increased expenditure on social care but it can constrain future allocation decisions and potentially funding across the economic cycle. Consideration would need to be given to whether hypothecation would achieve greater transparency and deliver sufficient funding stability in practice.
Broadly, options could take several forms:
- Strict hypothecation, where spending is linked directly to new revenue raised and funding is used only for that purpose.
- Partial hypothecation, where new revenue raised is ring-fenced to fund increased expenditure, but existing baseline funding is not protected. This is the approach that has been recommended to fund increased investment for social care in a report to the Welsh Government[69].
- Indicated spend, where the raising of new revenues is symbolically linked to adult social care, but in practice the revenue raised is not ring-fenced.
- No form of hypothecation.
The speed of reform will have a big impact on the viability of funding options, as do options that can be delivered within the existing devolved settlement, versus options that would require new tax powers or the devolution of existing UK taxes.
In addition, the design of any new funding mechanism needs to be carefully considered to ensure it is proportionate, sustainable, embeds intergenerational fairness and is consistent with the Scottish Government's wider economic and fiscal strategies and outlook.
Addressing these important questions is a sizeable task in itself, which we recommend requires considerable further analysis and careful consideration before decisions are made.
Recommendations
Adult social care support in Scotland requires greater investment. To secure better access to social care support, better terms and conditions for the social care workforce, better sustainability, the economic benefits of a strong social care sector, and to meet the aspirations and other recommendations we have laid out in this report, we recommend:
49. Prioritising investment in social care as a key feature of Scotland's economic plans for recovery from the effects of the Covid-19 pandemic.
50. Careful analysis by a National Care Service, with its partners in the National Health Service, Integration Joint Boards and beyond, of opportunities to invest in preventative care rather than crisis responses, to avoid expenditure on poor outcomes such as those experienced by people who are delayed in hospital.
51. Additional investment in order to:
- expand access to support including for lower-level needs and preventive community support;
- implement the recommendations of the Fair Work Convention;
- remove charging for non-residential social care support;
- increase the sums paid for Free Personal and Nursing Care for self-funders using care homes to the levels included in the National Care Home Contract;
- re-open the Independent Living Fund, with the threshold sum for entry to the new scheme reviewed and adjusted; and
- review financial support made available to unpaid carers and increase investment in respite.
52. Robustly factoring in demographic change in future planning for adult social care.
53. Careful consideration to options for raising new revenues to increase investment in adult social care support.
Contact
Email: Donna.Bell@gov.scot