GETTING OUR PRIORITIES RIGHT (GOPR)
Updated Good Practice Guidance for use by all practitioners working with children, young people and families affected by substance use
Chapter 4
ASSESSING RISKS AND IMPROVING OUTCOMES
This chapter describes the key stages in both assessing and responding to any identified concerns about children and reviewing progress against outcomes. It reflects the Getting it right for every child (GIRFEC) practice model and also the principles of early intervention and recovery.
The Chapter is divided into four main sections. Specifically, it suggests:
- How services might assess risks and needs.
- How services should effectively plan care and provide supports for children and families - usually co-ordinated through the Child's Plan (see the Opening Policy Framework section for a description of this).
- Delivery of services and interventions identified in the Child's Plan.
- Describes the importance of setting targets, describing outcomes in care plans and reviewing delivery of these.
For practitioners' ease of reference, the key messages from this Fourth Chapter are summarised below.
SUMMARY MESSAGES FROM FOURTH CHAPTER - ASSESSING RISKS AND IMPROVING OUTCOMES
Assessing Risks and Needs
All services must look at the parent's alcohol and/or drug use from the perspective of the child to understand the impact that this has on the child's life and development.
Services should also consider each child in a household separately as their needs may differ significantly.
Assessment should be continuous to take account of changing circumstances that may impact on the child and family.
Children and parents should be included in the process to maximise chances of overall recovery.
Where the child's predominant needs are within universal services, it is likely that the Named Person will be in universal services and also act as Lead Professional to co-ordinate the help that is to be given.
Where a single agency assessment of a child/families risks and needs identifies that multi-agency support and care planning is required, the Named Person should arrange for this transition into multi-agency support.
They should follow locally agreed arrangements for this to happen and should use their assessment as the basis for agreeing that transition.
The Lead Professional should co-ordinate the delivery of any agreed Child's Plan. That is, the agreed action plan that sets out what actions are to be taken and by what service.
The Child's Plan requires that the views of the child and family are included.
Services should ensure that these key elements of the GIRFEC practice model are included in any local protocols.
The assessment, support and interventions set out in a Child's Plan should focus on the family strengths as well as the pressures that are impacting on the child's well-being - with actions designed to reduce these. These should be features of any Child's Plan - whether single or multi-agency. Any Plan should also focus on the child's outcomes.
Plans should also cover critical times where extra and seamless support for the family may be needed - e.g. where an adult is being released from prison or is accessing treatment.
Outcomes and Review
The Child's Plan will include targets and outcomes to be met by individual services delivering supports to a family.
Any planned withdrawal of a specific service should be communicated to the Named Person in the event that the Child's Plan needs to be adjusted to include any contingency measures.
Early and co-ordinated interventions focused on the recovery of the whole family are best to avoid problems becoming more complex, resource intensive, and difficult to manage further downstream.
The Child's Plan should be reviewed to regularly take account of any missed targets etc.
INTRODUCTION
157. Chapter 2 described early information gathering by services when considering adult alcohol and/or drug use and its possible impacts on children. Chapter 3 then described how services might safely share information to help them to identify risks to vulnerable children and families.
158. This fourth chapter now describes the next key stages - i.e. how services assess risks and needs and respond to any identified concerns.
ASSESSING RISKS AND NEEDS
GENERAL PRINCIPLES
159. This chapter reflects the Getting it right for every child practice model and also the principles of early intervention and Recovery as described in the Opening Policy Framework Section.
160. That Section set out that, where a family has been identified as requiring further support (whether single agency or multi-agency co-ordinated), a fuller assessment should be undertaken to determine the nature of the support that will be required. A child's Named Person should ordinarily co-ordinate this assessment.
161. It also described that any initial assessment by the Named Person may then lead to a multi-agency assessment meeting. Any assessment by the Named Person should also result in the development of a Child's Plan describing the actions to be taken, the key targets to be met, and by whom. A Lead Professional would usually be appointed at this stage to help co-ordinate the delivery of the actions included in the Child's Plan.
162. The GIRFEC diagram below describes the assessment routes (whether single agency or multi-agency) and the points where the Named Person and Lead Professional would usually have a role.
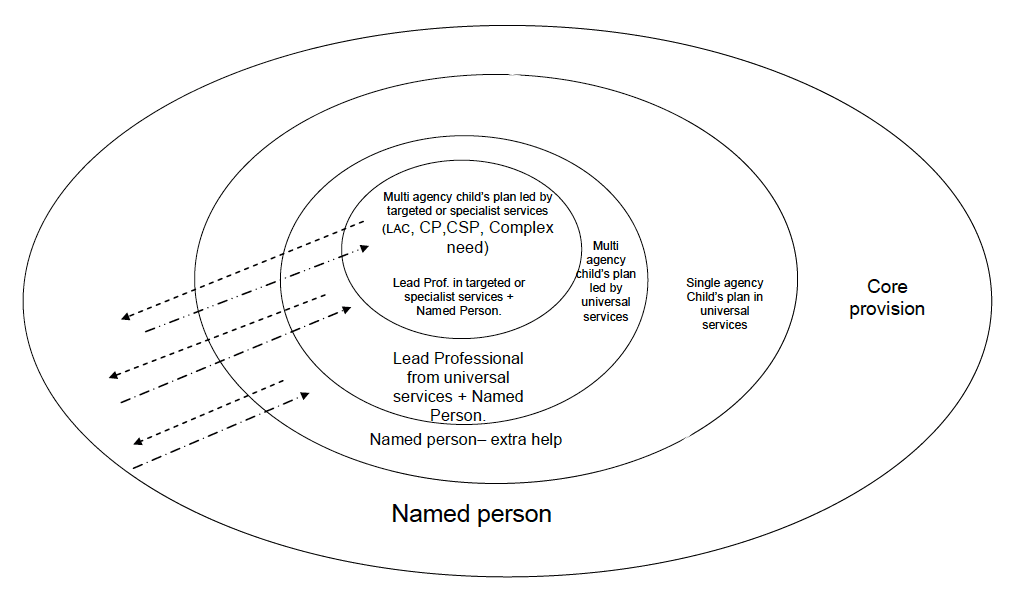
ASSESSMENT PROCESS
163. Generally - when assessing the well-being of any child and family - all services must look at the parent's substance use from the perspective of the child to understand the impact that this has on the child's life and development. Services should also consider each child in a household separately as their needs may differ significantly.
164. When assessing needs and risks, services working with children and families should might find it useful to refer to the Getting it right for every child My World Triangle to help them to understand what is happening around the child.
www.scotland.gov.uk/Publications/2008/09/22091734/9/Q/ViewArchived/On
165. Services should generally draw together information about:
- the child's age and stage of physical, social and emotional development;
- his or her educational needs;
- the child's health and any health care needs (eg. Hepatitis B vaccination);
- the child's safety while adults are using drugs and alcohol;
- the emotional impact on the child of frequent or unpredictable changes in adults' mood or behaviour, including the child's perception of parents' drug use, and;
- the emotional impact on the child and family of a parent diagnosed with a blood borne virus infection (HIV, hepatitis B and hepatitis C). Equally the impact of changes in adult mood and health upon commencement of anti-viral therapy as part of a parent's recover from drug use.
- the extent to which parental drug use disrupts normal daily routines.
166. A more detailed checklist for gathering information about problematic alcohol and/or drug use and its impact on families is available at Appendix 2. This checklist has been developed to reflect the GIRFEC practice model with a specific focus on drug and/or alcohol related questions.
167. Any service in touch with a family affected by parental alcohol and/or drug use can use this checklist, either in its entirety, or by selecting sections that are appropriate to their role. This will enable them to identify alcohol and/or drug related risks likely to affect the child's well-being and development. It will also enable them to highlight areas of strength within the family that may be harnessed to tackle problems.
168. Assessment cannot be seen as a one-off event - nor can it be separated from intervention. Concerns can reduce over time and can also increase. Equally, changes in a child or family's circumstances can strengthen or limit protective factors (see Chapter 1 for examples of these).
169. Assessment needs to be a flexible and ongoing process. At any given time, it should take account of current circumstances but also previous experiences and needs to consider immediate impacts as well as longer-term outcomes for children.
FLOWCHART - DESCRIBING BROAD STEPS TAKEN FROM IDENTIFICATION OF A CHILD IN NEED TO ASSESSING RISKS AND CARE PLANNING
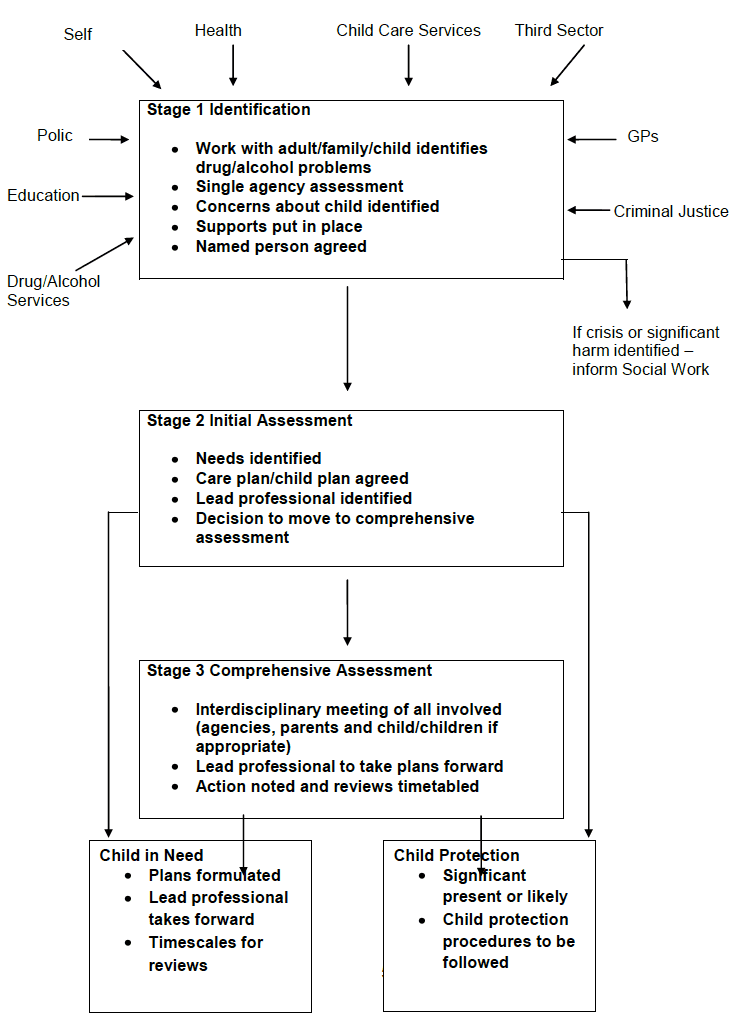
PRACTICE POINTS
170. In the Text Box below, a number of possible questions are provided for use by services to explore with families their needs, and also, to help identify risks to children. These questions also focus on those areas that the child and family themselves identify as difficulties and also strengths.
KEY PRACTICE POINTS
When assessing whether a child may need help services should consider the following questions:
Are there any factors which make the child(ren) particularly vulnerable? For example, the child might be very young, or has other special needs such as physical illness, behavioural and emotional problems, psychological illness or learning disability(ies)? Are there any protective factors (See Chapter 1 for examples of these) that may reduce the risks to the child?
How does the child's health and development compare to that of other children of the same age in similar situations?
Are children usually present at home visits, clinic or office appointments during normal school or nursery hours? If so, does the parent need help getting children to school?
How much money does the family spend on alcohol/drug use? Is the income from all sources presently sufficient to feed, clothe and provide for children, in addition to obtaining the alcohol/drugs?
Do the parents perceive any difficulties, and how willing are they to accept, help and work with professionals?
What arrangements are there in place for the child(ren) when the parent goes to get illegal drugs or attends for supervised dispensing of prescription drug(s)?
Is there evidence of neglect, injury or abuse, now, or in the past? What happened? What effect did/does that have on the child? Is it likely to recur? Is the concern the result of a single incident, a series of events, or the accumulation of concerns over a period of time?
Do parent(s) think their child knows about their problem alcohol or drug use? How do they know? What does the child/other family members think?
Do the parent(s) maintain contact with services? Who will look after the child(ren) if the parent is arrested or is in custody?
IMPORTANCE OF RELATIONSHIPS
INVOLVING CHILDREN IN ASSESSMENT AND DECISION MAKING
171. Research shows that the child's voice can often be lost in assessment and decision-making. Children and young people can often find it difficult to articulate their views and their experiences of living with a drug and/or an alcohol using parent. The reasons for this can be: loyalty towards the parent, distrust of services, fear of the family being separated, or fear for their own, or their siblings' safety.
172. When involving children, effective communication is therefore essential. To achieve this, practitioners should develop a positive, supportive relationship with the child.
173. Practitioners should also ensure that the key elements of Getting it right for every child (e.g. any agreed Child's Plan as supported by the GIRFEC National Practice Model requires that the child's views are included) are embedded in practice and included in local protocols. This, in turn, should ensure that children and young people are integral to the planning and assessment process.
174. When assessing risks and needs, services also need to recognise the important role family and friends are as a source of support for children, particularly grandparents and also teachers. It is essential that services foster good relationships here both to reassure the child and to ensure that their voice is heard.
INVOLVING PARENTS IN ASSESSMENT AND DECISION MAKING
175. Chapter 2 touched on the need to keep parents at the forefront of a co-ordinated response if services are to be effective in achieving overall recovery for the whole family. This is further evidenced by research into the perceptions and experiences of parents involved with child welfare services. This research found that to achieve positive outcomes for families:
- The quality of the relationship between the practitioner and parents is central to effective engagement and involvement of parents.
- Parents value honesty, reliability, good listening skills and practitioners who demonstrate empathy and warmth.
- Explicit use of counselling approach (both generic and adapted to parents with learning difficulties) to develop empathy and increase the potential for more productive relations.
- Explicit discussion with parents about their perceptions of how workers are using their professional power as a means of control or support - especially when working with resistance.
- Comprehensive, strengths-based assessment - including family and social networks and methods such as family group conferences - can be effective especially where involving fathers and father-figures.
- Drawing, where necessary, on the expertise of key professionals that have worked with adults with learning disabilities, for example, to maximise their involvement and participation.
PRACTICE POINTS
Generally it is good practice to work in partnership with parents and, where possible, parents should be included in any multi-agency meetings, in assessments and in developing care plans.
Achieving partnerships with parents and children in the planning and delivery of services to children requires that:
Parents have sufficient information, both verbally and in writing, to make informed choices.
Parents are made aware of the help that is available.
Parents are aware of the consequences of any decisions they may take.
Parents are actively involved - where appropriate - in assessments, decision-making meetings, care reviews and conferences.
Parents and children are given help to express their views and wishes and to prepare written reports and statements for meetings where necessary.
Professionals and other workers listen to and take account of parents' and children's views.
There should be clear and accessible means for families to challenge decisions taken by professionals, and to make a complaint if necessary.
Administrative arrangements take account of the needs of parents and children; for example, the timing, location, environment and conduct of meetings should take account of their needs.
CARE PLANNING FOR CHILDREN AND FAMILIES
176. Learning from the Getting it Right - Report on Angus Learning Partnership for Children Affected by Parental Substance Misuse (2011) emphasised the importance and value of simultaneously addressing the needs of the child and their parent(s) to achieve good outcomes for both.
177. The Getting it right for every child approach provides a series of common tools, language and planning processes that can improve the identification of the risks and needs in a child's life as part of a wider assessment of the child's development. In particular, and as mentioned above, any action to support a child should be co-ordinated through a single child's plan.
178. Both the family and the services involved should be clear about the purpose of the Plan and what is expected of each family member and service to achieve recovery.
179. Assessments and any care planning need to include a realistic appraisal of the timescales for change for the entire family. This is because there will be occasions where the timescales for the parent's recovery may not match the needs of the child and contingency measures may need to be agreed by services. For example, this may involve consideration of respite or temporary care arrangements, or intensive supports being offered in the short-term.
180. While effective drug and/or alcohol treatment is a positive outcome for the parent, recovery for the whole family will often include a number of interventions. These could include interventions designed to support children in their own right and/or to enhance parenting capacity and promote resilience. Support and treatment for the parent cannot therefore be seen in isolation from the wider family's needs. In effect, a family focus needs to be at the forefront of a co-ordinated multi-agency approach.
KEY PRACTICE POINTS - CHILD'S PLAN
A Child's Plan should ordinarily be agreed by services as part of assessment that leads to care planning to support a child.
Generally, the Child's Plan describes an agreed plan of action by involved services - describing the necessary supports and actions to be taken and by whom.
The appointed Lead Professional should normally help to co-ordinate the delivery by services of the Plan.
The Named Person will usually have general oversight.
Specifically the Child's Plan will include the following:
- The views of the child (according to age and stage of development) and the family/carers.
- Who is a partner to the plan.
- Reason for the plan.
- Summary of the child's needs against the GIRFEC well-being indicators (see opening Policy Framework section).
- Desired outcomes.
- Resources.
- Timescales for action and change.
- What needs to be done and by whom.
- Any contingency arrangements - where necessary.
- Arrangements for reviewing the plan.
DELIVERING AGREED INTERVENTIONS
181. Early identification of a need - and also timely interventions to support families and children - can prevent problems from escalating and becoming more complex, resource intensive and difficult to manage further downstream. Also, with the right intervention(s), parents can receive support to better manage their problem alcohol and/or drug use and any other difficulties they may be experiencing.
182. This can, in turn, leave them better equipped to parent more effectively and help reduce the impact of the problem of alcohol and/or drug use on the child.
183. As mentioned in the earlier part of this Chapter about assessment of risks and needs by services - the Lead Professional is ordinarily responsible for ensuring interventions and services are delivered in accordance with the Child's Plan.
184. To achieve this, regular and ongoing communications with involved services are essential here. For example, ongoing communication is the responsibility of all services to maintain. Failure to keep appointments by families - or a proposal to withdraw a specific support service - should always be communicated to the Lead Professional.
185. When designing interventions services also need to take into account the following factors:
- In many instances, children may be responsible for providing practical support to their parents and/or siblings.
- In addition, or at times alternatively, this may take the form of emotional supports.
- Children should not be expected to take on similar levels of caring responsibilities as adults or be responsible for the intimate care and supervision of their parents.
- In assessing the family as a whole, and the types of supports that may be needed - consideration needs to be given to the levels of responsibility that are being taken on by a child, the levels of emotional support they have access to, and also the setting of boundaries within the family.
- All of these factors should be taken into account together with the levels of physical caring that are actually in place for the child.
186. Also, resistance, both from parents and children, can be a barrier to a child receiving support. The parent may not want to recognise the impact on the child and the child may unwittingly collude in that.
187. Particular consideration needs to be given by services here to identifying either critical - or particularly difficult - times for children and an awareness of what these may mean.
188. Examples of these difficult times might include:
- a parent undergoing detoxification;
- relapse;
- discharge from adult services; or
- a parent in hospital;
- a parent undergoing testing or anti-viral treatment for an identified blood borne virus infection as part of their recovery from drug use;
- in prison; or
- experiencing an episode of domestic violence.
189. Close collaboration between services at such times is essential to ensure that adequate supports are in place for vulnerable children and their families. Types of intervention(s) that services may agree for a child and family must be dependent on their individual needs and circumstances. These should be identified at the assessment stage.
190. Examples of strategies or techniques that may be used by services - working directly with children affected by parental problem alcohol and/or drug use - might include:
- Social support - This may involve group activities offering mutual support and exchange of experiences.
- Information - On the substance use, potential consequences etc.
- Skills training - How to deal with problems, social skills etc.
- Coping with emotional problems - Helping the young person identify and discuss feelings.
KEY PRACTICE POINTS
What is important - practice points that help achieve change:
- Engagement - how projects have built relationships.
- Stickability - keeping with families looking at options and routes that will help them achieve change.
- Practical steps - boundaries, routines, support and input to help improve family life.
- Empowerment and self determination are key facets in developing approaches.
OUTCOMES AND REVIEW - INCLUDING REVIEWING THE DELIVERY OF THE CHILD'S PLAN
"The definition of outcomes is the impact or end results of services on a person's life. Outcomes-focused services and support therefore aim to achieve the aspirations, goals and priorities identified by service users (and carers) - in contrast to services whose content and/or form of delivery are standardised or determined solely by those who deliver them."
(Glendinning et al, 2006)
191. Goals that are included in any care plan agreed by services should focus on tangible outcomes that the child, family and services can agree upon. An outcomes focused approach should identify clear goals by which to measure improvement.
192. Outcomes will vary and should be developed in partnership with parents and children to ensure these are realistic and measurable. This both helps the parent and child see progress but also is a way for services to measure change.
193. Language in relation to outcomes needs to be clear and understandable so that everyone knows what is being worked towards. Examples of some outcomes captured through the Lloyds TSB Foundation for Scotland, Partnership Drugs Initiative (PDI) funding programme are described below:
- Increased/ consistent engagement with service.
- Increased level of referral to, and engagement with, other services (including dentists, health checks).
- Increased knowledge/awareness of impact of substance misuse on self and others.
- Reduction/abstained from substance use.
- Increased boundaries, structures, routines.
- Increase in parenting /life skills.
- Improved family relationships.
- Increase in child's safety.
- Increased coping mechanisms.
- Increased confidence/self-esteem.
- Increased participation in alternative activities.
- Increased access to/participation in school; nursery; education; employment.
- Increased positive engagement with community.
- Improved health and well-being.
194. It is helpful when considering desired overall outcomes for children and families for services to first set realistic shorter-term targets as well as longer-term goals. For example, a parent engaging with a service, or a child being removed from the Child Protection Register, to a longer-term goal, or core outcome, of an overall increase in the child's safety.
195. To ensure that any agreed Child's Plan and family supports remain effective, and on target, it will be necessary for relevant services to meet and review progress with the child (depending on age) and also the family. This will include evaluating the impact of the work done and any changes in the family's circumstances.
196. Consideration should also be given here to any targets that have not been achieved and to identify the reasons for this.
197. This may result in changes to the Child's Plan and supports to include a more appropriate response. Alternatively, it may be that a gap in resources is an obstacle and that further discussion between services is required. In some instances, the child and/or family's circumstances may have deteriorated and contingency plans will need to be considered.
198. Appendix 3 provides an example of an outcomes measurement tool that might be used to identify objectives for children and families and services.
WITHDRAWAL OF SERVICES
199. Services need to ensure that they do not withdraw support too early. Families can sometimes be left in a vulnerable position just as the situation appears to improve.
200. Any planned withdrawal of a service should be communicated to the Named Person - and also the Lead Professional if one is in place. They will then consider whether the Child's Plan needs to be reviewed.
201. Once a parent has stabilised and/or stopped their drug and/or alcohol use they must be given support to cope with everyday issues without resorting to substances as they may have in the past. This should be supported by a multi-agency approach wherever possible so that agencies can co-ordinate their activity and ensure good communication.
KEY PRACTICE POINTS
REGULAR REVIEW
Assessing children and their families is not a one-off event. Individual services should always be alert to changes in families' circumstances and whether children appear to be well cared for and thriving.
Those professionals in regular contact with families should be alert to increases in stress, changes in parents' alcohol and/or drug use or other changes in their circumstances, and should consider any detrimental impacts on their ability to look after children. These changes may signal a need for more help.
Services should regularly re-assess and review their clients' family and wider living circumstances. For example, parents using alcohol or drug services should be asked routinely about how they are coping with parenting responsibilities and given the opportunity to talk about stresses or worries.
When visiting families at home, practitioners - including specialist alcohol or drugs workers - should always observe and record the conditions in which children are living.
If the worker feels able, they should discuss any worries about the safety or well-being of the children with the parents. If problems persist they should refer the child and family to the social work service for help and any protection needed.
If a specialist worker is uncertain about whether the care of - or conditions for - the child(ren) are adequate they should seek advice from a senior colleague with responsibility for child protection. If in doubt, they should seek help from a service with responsibility for protecting children's welfare - the social work service, the Reporter or the police.
Throughout their involvement with families in which parents have alcohol and/or drug use problems, all services should continually consider:
- the extent to which parents may try to conceal their illegal drug taking/harmful drinking from services because they fear the negative consequences, and;
- how difficult parents may find it to change their alcohol and/or drug use and associated behaviours despite those negative consequences.
Services should acknowledge with parents that they recognise these factors and continually test the accuracy of information provided.
Parents may also find support and advice about their parenting, and possible risks to their children, difficult to accept. Professionals should be open about these difficulties and talk to parents about the importance of tackling problems early on.
Contact
Email: Graeme Hunter