Health and work strategy: review report
The report from the review of the Scottish Government's health and work strategy.
5 Health and Work: The Scottish Picture
Scotland's record in relation to health and work is a good one and is something we can be proud of. For too many people, however, the relationship between their health and work is not a positive one, with health related 'presenteeism,' absence and worklessness contributing to Scotland's persistent health and social inequality. It also presents a significant drag on the Scottish economy and national finances.
In addition to continuing to address these issues, there are a number of new and emergent risks to health and work that require an urgent response:
- The economic environment is changing.
- The nature of work is changing.
- The nature of the workforce is changing.
The Economic Environment
Scotland's Economic Performance
The tri-annual report into the state of the Economy published in February 2019 by the Chief Economic Adviser to the Scottish Government[25] provides a picture of the Scottish economy in an international context, including Brexit impact analysis. It paints mixed picture. Most positively, it highlights a record low level of unemployment and the maintenance of a historically high employment rate (75.3%), though it also reports low GDP growth that is lagging slightly behind the UK as a whole and a weakening in business confidence, issues it attributes to uncertainty related to Brexit, and in particular to concerns about the risk of a 'no deal' Brexit.
The report also highlighted a relative improvement in labour productivity (measured in terms of GDP/hour worked) in Scotland compared to the rest of the UK (rUK) over the last 12 months, though a persistent labour productivity gap remains between Scotland and the UK as a whole, with a significant gap remaining been Scotland and the UK, and other northern European countries.
Addressing this productivity gap and delivering sustainable inclusive economic growth are both outcomes that the Scottish Government is seeking to deliver through its Economic Strategy[9]. The Poverty and Inequality Commission have identified a number of actions that would support this[26], and a specific response from a health perspective could be stronger ring fencing of investment in supporting apprenticeships for young people with a disability of long term health condition. More generally, and indeed more significantly, persistent levels of sickness absence, presenteeism and health-related worklessness also present a significant brake on the Scottish Government's economic ambitions.
In light of the risks associated with Brexit or other economic shocks, it is vital that these issues are addressed, something that is recognised by Scotland's Economic Strategy, which, by seeking to invest in human capital, aims to achieve a "well-skilled, healthy and resilient population and an innovative, engaged and productive workforce[9]".
Brexit and Economic Shocks
It remains unclear when and on what basis Brexit will occur, however all of the economic modelling undertaken by the Scottish and UK Governments expects the impact of all Brexit scenarios to be adverse to a greater or lesser extent. Its impact is already being felt in a number of ways as reported by including in the labour market as the number of EU workers declines. Whilst this decrease currently appears to be offset by inward migration from other countries[27], it is unclear whether this will continue or whether the skills available will be matched to the vacancies that arise. Anecdotal evidence from the agriculture industry, for instance, suggests that recruitment is becoming increasingly problematic. With an already tight labour market, it is essential that as many people as possible are able to contribute economically with health and disability presenting significant barriers to this.
In addition, there are concerns that Brexit could lead to 'a race to the bottom' in terms of conditions of employment, and it is noted that other than through procurement arrangements or voluntary mechanisms, the current devolved settlement would make it difficult for the Scottish Government to project or even strengthen employment rights given these fall under the reserved powers of the UK Government.
The Fiscal Framework
The Fiscal Framework[28] that was introduced under the terms of the Scotland Act (2016)[29] has particularly significant implications for the Scottish Government's Budget by shifting the balance of its income from the block grant received from the UK Government to income received from taxes levied in Scotland. Put simply: where the Scottish economy performs relatively well, tax revenues will rise and pressures on spending will ease; where it performs relatively less well, the effect will be to reduce tax revenues, cut available funding and increase spending demands.
The relative burden of work related absence and ill-health in Scotland will therefore increasingly impact upon the Scottish Government, and conversely, improvements in its performance will bring direct financial benefits. Were Scotland to become an independent country, the cost burden relating to work related absence, or conversely the financial dividend, would of course be entirely a matter for the Scottish Government.
The Nature of Work
In recent years there have been a number of changes in the nature of work, in large part driven by global economic and technological developments, and by domestic Government policy, particularly in relation to austerity, culture and employment practice.
Technological Change
Technological change and associated working practices appear to accelerating as part of a 21st century industrial revolution. Pre-existing developments such as information technology (IT) and increased automation have now been joined by artificial intelligence (AI) and machine learning, robotics and the development of autonomous vehicles, all of which have the potential to impact positively and negatively.
For people with a long term condition or disability, these developments may open up many opportunities in terms of providing the adjustments, necessary for them to be able to remain in, return to or access work. Autonomous vehicles may enable easier and cheaper transport options and AI may lead to better voice recognition applications that would be beneficial to people with physical or visual disabilities.
Conversely, such developments can be expected to lead to significant job losses in certain industries with new opportunities emerging in other parts of the economy. This will inevitably lead to anxiety around job security, which if experienced in less skilled sectors of the economy is an additional risk to the health of those already exposed to the highest health risk. It will also require strategic foresight and investment in skills to enable displaced employees to take on new roles, assuming of course this is something they are able to do.
It is, of course, risky to make predictions about technologies that are not yet in widespread use, and other technologies will inevitable also emerge in the coming years. It will be a key role for occupational surveillance and public health observatory functions to consider the short, medium and long-term implications for health, with policy makers and those supporting the health of the workforce to be agile in their response.
Self-Employment, the 'Gig Economy' and Precarious Work
The last ten years have seen a significant increase in 'employment' in what has come to be known as the 'Gig Economy,' with examples routinely being reported of people on 'zero-hours contracts' and in-effect treated as self-employed, and thereby lacking the normal legal protections and support afforded to employees. It bears all of the characteristics of precarious work, though other than through its own employment practices and those of public sector bodies over which it can apply levers, using the Fair Work First approach to procurement and through wider advocacy, tacking such employment arrangements is otherwise beyond the powers of the Scottish Government.
Self-employment per-se, where it is a genuine choice, is of course an entirely legitimate career option, is an important sector of the economy in own right and is also potentially the starting point of the small, medium and even large employers of the future. Whilst enjoying many benefits associated with "Good Work"[20], particularly in relation to demand, control, voice and work-life balance, self-employment can also bring significant challenges like low income, long hours, and should ill-health occur there is the risk to an individual's income and indeed to the business itself.
Of particular note is that by rising by 26%, self-employment "has accounted for almost half of overall employment growth over the past decade and over 80% of the growth in the number of businesses in Scotland"[30].
Working Health Services Scotland, along with providing support for SMEs, uniquely offers support to the self-employed, and in light of the current trend is therefore a crucial element of the Fair and Healthy Work infrastructure.
Working Hours
Analysis published in 2019 by the Trades Union Congress[31] shows that workers in the UK are working the longest hours in the EU, with full-time employees in Britain working an average of 42 hours a week in 2018, nearly two hours more than the EU average - equivalent to an extra two and a half weeks a year - and more than four hours longer than the average in Denmark. A review of the evidence undertaken for the UK Department of Trade and Industry[32] concluded that long working hours are associated with a range of health problems, poorer performance and decreased productivity and that women are more likely than men to suffer health related problems, if they worked long hours.
The Nature of the Workforce
Ageing and Declining Workforce
The workforce is getting older and is decreasing as proportion of the overall Scottish population, with the projected changes in the age profile over next ten years detailed in figure two below, and projecting further ahead to 2041, this picture is projected to become even more pronounced[33].
| Age Group | Percentage Change |
|---|---|
| 0-15 | + 2 |
| 16-24 | - 9 |
| 25-45 | + 5 |
| 45-64 | - 4 |
| 65-74 | + 13 |
| 75+ | + 27 |
National Records of Scotland (2017)
Figure 2 – Projected Change in the Scottish Population by Age group (2016-26)
At the same time, the state retirement age for both men and women will rise to 66 in 2020 and to 67 in 2026, meaning that there is every likelihood that more people in the 65-74 age bracket will still be working, indeed 88,600 people aged 65 years and over were in employment in Scotland in 2018, almost twice as many as ten years ago, and the same period has also seen a jump of 131,600 number of people working aged 50-64[34].
Between 2016 and 2030, the average age of the workforce is projected to increase from 39 to 43[35], and with the average age of those working in the public sector already sitting at 45[36], this sector can expect to be particularly impacted.
For people of pensionable age there is projected to be an increase in the dependency ratio from 307 pensioners per 1,000 working age population in 2016 to 380 in 2041[33], which can only be expected to place additional carer pressures on those in employment.
Stalling Improvements in Health and Health Inequality
With an ageing workforce within an ageing population, the health or those of working age becomes even more critical. From around 2012-14, however, the rate of improvement in life expectancy and mortality has become substantially slower, with life expectancy actually falling in 2015-17, and mortality rates now increasing in the most deprived fifth of Scottish areas, developments described as "almost without precedent and requiring urgent action[37]," and in which austerity, pressures on services and influenza are implicated.
This slowing, and even reversal of improvements in health and the health inequality gap is mirrored by self-reported work-related ill health, which followed a generally downward trend to around 2011/12; since which time the rate has been broadly flat.[38]
Long Term Conditions
The trend towards an ageing workforce is leading to a rapid increase in long-term conditions with 40% of the workforce expected to have a least one such condition by 2030[35]. Whereas in the past, many especially smaller employers could say with some legitimacy that this was an issue they rarely faced, in just a few years' time it will become the norm for all employers to be managing employees with long-term conditions. In all likelihood, given the decline in the Fair and Healthy Work workforce, this will be without the advice or support they need to do so effectively.
Figure 3 - Health Status of the Scottish Population[39]
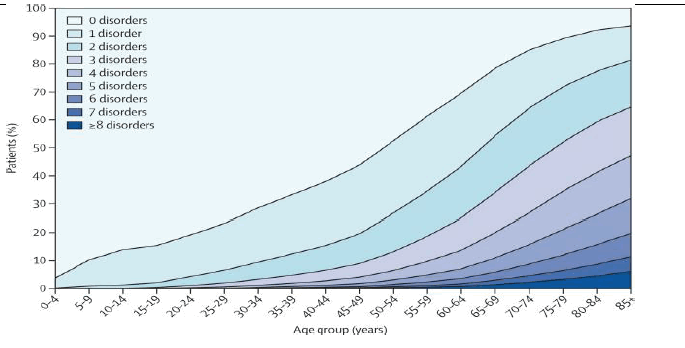
Figure 3 illustrates the nature of problem, and the combination of an aging workforce plus a stalling in improvements in health and health inequalities, mean that many conditions, that are associated with health inequalities or more natural presentation in older age, such as many cancers, cardio-vascular disease and dementia, all of which require highly specialist intervention, are likely to increase in prevalence within the workforce. This is in addition to other conditions, such as asthma, obesity and type 2 diabetes which are already impacting the workforce.
Arthritis and Muscular Skeletal Disorders provide a good illustration of the challenge we face given its role in accounting for 35% of new and long-standing cases of work-related ill health[38], together with being a significant cause of health related worklessness. Among people aged 45–64 the prevalence of arthritis is more than double in the most deprived areas (21.5%) compared to the least deprived areas (10.6%), figures that increase to 36.2% and 23.1% respectively in the 65-74 age group[40].
An ageing workforce, coupled with persistent health inequality and stalled health improvement, presents an unprecedented economic threat.
Mental Health and Wellbeing
Stress, anxiety and depression account for 44% of new and long-standing cases of work related ill-health[38], with a trend over time that has seen mental health issues being responsible for an increasing proportion of absences. The cost of poor mental health to UK employers alone is estimated to be between £33 billion and £43 billion (£3-£4 billion pro-rata for Scotland, and as much as £100 billion for the UK economy (£9 billion to Scotland) as a whole[15].
Recommendations for Employers
1. Produce, implement and communicate a mental health at work plan.
2. Develop mental health awareness amongst employees.
3. Encourage open conversations about mental health and the support available when employees are struggling.
4. Provide your employees with good working conditions.
5. Promote effective people management.
6. Routinely monitor employee mental health and wellbeing.
Additional Recommendations for the Public Sector and Large Employers
1. Increase transparency and accountability through internal and external reporting.
2. Demonstrate accountability.
3. Improve the disclosure process.
4. Ensure provision of tailored in-house mental health support and signposting to clinical help
Figure 4 – The Stevenson/Farmer Recommendations for Employers
Absences associated with mental health are also typically are of a longer duration than physical health related absences. They can also frequently be associated with other health conditions, and as such it is important that an individual's mental wellbeing is considered within any wider treatment plan.
The Stevenson/Farmer Review of Mental Health and Employers[15]makes six recommendations for all employers and recommends a further four standards for all public sector organisations and private sector organisations employing more than 500 staff (see figure 4), recommendations that are endorsed by this Review:
Sickness Absence and Presenteeism
In common with the already situation already detailed in terms of health improvement, health inequalities and self-reported health at work, working days lost per worker due to work-related illness also showed a generally downward trend up to around 2010/11, since which time the rate has been broadly flat[38], with muscular skeletal disorders and mental health when combined accounting for 79% of this.
The costs associated with sickness absence therefore remain significant, and largely unchanged since the detailed analysis undertaken by Professor Dame Carol Black[2], however this fails to tell the whole story.
Presenteeism, which is defined by the Chartered Institute of Personnel and Development (CIPD) as "people coming into work when they are ill," which may exacerbate their underlying condition or lead to the spread of infection within a workplace, has more than tripled since 2010[41]. Over half of the £3-£4 billion cost of poor health to Scottish Employers is estimated to be down to Presenteeism[15].
Presenteeism, and 'Leavism', a more recent phenomena identified by CIPD in which employees work through annual leave or use it to cover absences, and which is also on the increase, "are both less common in organisations that are focused on employee wellbeing"[41].
The Disability Employment Gap
The disability employment gap, despite significant efforts, remains stubbornly large, with the employment rate amongst people with disabilities at 45.4%, only roughly half the level of those without a disability (81.2%)[33]. The Scottish Government, in launching its 2018 Fairer Scotland for Disabled People: Disability Action Plan, is rightly ambitious in its objective of decreasing this gap. The Health and Work workforce has a role to play in this also, as does the wider Health and Social care system.
Regrettably, there are also factors that are working beyond this ambition, and which lie outwith the powers of the Scottish Government. An important example of this is the growing body of evidence that shows the impact of conditionality on people with underlying health conditions or a disability, the increased likelihood that their condition may lead to sanctions being applied (i.e. due to missing Job Centre appointments), and their being moved further from the labour market or accepting poor/precarious work to avoid the sanctions regime.
Research[42] published in May 2018 by a collaboration of universities including Glasgow and Heriot Watt found that welfare conditionality in overall terms failed to move job-seekers closer to the labour market, that in the case of disabled people it exacerbates existing illness and impairments, and expressed particular concern about the impact on those with mental health issues. It specifically concluded that 'benefits sanctions should not be applied to those in receipt of incapacity benefits." It is an issue that requires urgent action at UK level.
Gender Related Health
The number of women active in the labour market has also increased steadily over the last 50 years, whilst the rate of men has actually fallen, meaning that there are now similar proportions of men and women at work. The messages of this Review are therefore equally applicable to both genders, though there are also differences that need to be reflected in the policy and practice response.
It has already been noted that longer working hours have a more significant impact on women than men, and there is also evidence, despite legislation to tackle the gender pay gap, "female dominated occupational and industrial sectors tend to be low-paid and undervalued"[43]. Women are also much more likely to be in part-time work or unpaid work than men. Of the total number of employed women, 41% work part time, compared with 12% of employed men[44].
In terms of health, a review undertaken by the Work Foundation[45]reports that, whilst men die younger, tend to be less willing than women to seek health professional support and appear to be more significantly impacted by unemployment, women carry the burden of parenting and caring responsibilities and evidence suggest they are more likely than man to be disabled or have multiple long-term conditions. Male specific conditions such as testicular and prostate cancer commonly feature in workplace health interventions, but can the same also be said of female specific cancers, or "the multiple life phases that women experience that can all pose health challenges?[45]"
Given the role played by both men and women in the labour market and its importance for the economy as a whole, the conclusion must be that greater attention needs to be paid to gender differences in the workplace, and the impact they have in economic and health terms.
Resourcing Fair and Healthy Work
A significant part of the responsibility for delivering Fair and Healthy Work in Scotland rests on the workforce that supports employers, employees and those with health issues and disabilities who are seeking to enter work. This workforce is very small, predominantly comprising professionals working in Occupational Health, Condition Management, Employability, Local Authority Environmental Health Teams, the Health and Safety Executive and a small cohort within the Public Health workforce of national and territorial NHS Boards. Moreover, whilst this workforce is multi-disciplinary in nature and rightly sits across a range of sectors and organisations, the overall picture is one of at times unnecessary fragmentation and less than optimal coherence.
The Review identified concerns about the current capacity and sustainability of this resource, and its ability to meet the growing needs of employers and individuals in the future given the overall picture of a declining number of staff working in the field, a workforce which is also facing the same demographic issues as the wider workforce it supports. There has been some welcome new investment, such as in the Health and Work Support Pilot, and the Scottish Government's commitment to train 300 individuals to become Certified Disability Management Professionals[46], but in light of the challenges facing us there are relatively modest interventions.
Ten years ago, Health Works[4] estimated that no more than 15% of employers in Great Britain offer access to in-house occupational health services," a figure that the Society of Occupational Medicine reports has declined since this time, a figure which falls to just 3% if a tighter definition is used[47].
It is an issue that requires urgent action, particularly given the lead times for recruiting and training new staff, indeed work is already underway though COSLA and the Society of Chief Officers for Environmental Health in Scotland[48] to address matters in their field of work, and the development of Public health Scotland provides an opportunity to consider the resource and long-term arrangements for its contribution to Fair and healthy Work, most notably through the Healthy Working Lives Programme. At UK level, an Occupational Health Expert Group[49] has been appointed to look at the occupational health workforce to ensure sufficient capacity is available in the future.
The Review has noted the approach taken in other parts of Europe such as in Finland, a country with a population only half that of Scotland, whose national multidisciplinary Institute of Occupational Health employs around 750 whole time equivalent staff[50]. It is a scale of investment to which Scotland should aspire.
In summary, the Review takes the view that current provision in place is Scotland is inadequate to meet the needs that currently exist, and that the trends we are seeing in terms of the nature of work and workforce will significantly outstrip this provision. In light of the economic risks that are on the horizon, and the changes funding arrangements for the Scottish Government through the new Fiscal Framework, the Review concludes that there is a genuine case to be made for significant additional investment to be made in the multidisciplinary workforce that is dedicated to or contributory to Fair and Healthy Work.
Contact
Email: roderick.duncan@gov.scot