Coronavirus (COVID-19) - Near Me video consulting service: evaluation 2020 - main report
This report presents the findings of an external evaluation of the rapid scaling-up of the Near Me video consultation service across health and care services in Scotland during 2020, in response to the coronavirus pandemic.
2. Methods
2.1 Data collection
Data collection consisted of semi-structured and narrative interviews with health and social care staff and national stakeholders, patient and clinician post-consultation surveys and video appointment activity data.
The interviews were conducted between July and October 2020 via phone/video call. We purposefully selected a sub-sample of local NHS Health Boards for qualitative data collection, in order to analyse data within the organizational context. These were selected to explore variations in geography (urban, rural and islands), clinical context, local (NHS boards) and adoption progress. The selection was guided by initial scoping interviews with local project leads at each health board. The geographical areas covered by the NHS Health Boards are shown in Figure 2 below.
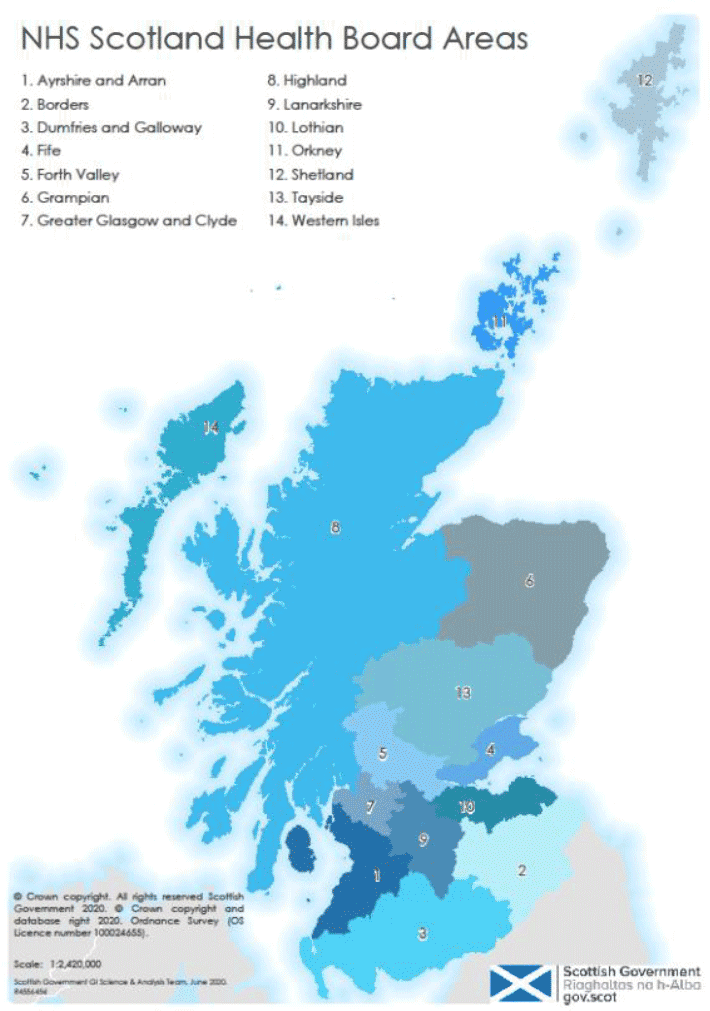
Figure description:
Map of Scotland showing the boundaries of the 14 NHS Scotland territorial (or local) Health Board areas.
Table 1: Participating Health Boards
Health Board / Site where interviewee is based
NHS Grampian
- Aberdeen Royal Infirmary
- Woodend Hospital, Aberdeen
- GP practices in Aberdeenshire
- Care Homes
NHS Greater Glasgow and Clyde (GGC)
- Glasgow Royal Infirmary
- Inverclyde Royal Hospital
- The Royal Hospital for Children
- Queen Elizabeth University Hospital
- GP Practices
NHS Dumfries and Galloway
- Dumfries and Galloway Royal Infirmary
- Child Health Care Centre, The Crichton, Dumfries
- Care Homes
- GP practices
NHS Highland
- Raigmore Hospital, Inverness
- Care Homes
NHS Forth Valley
- Falkirk Community Hospital
- Clackmannanshire Community Health Care Centre, Alloa
- Forth Valley Royal Hospital, Larbert
NHS Fife
- Queen Margaret Hospital, Dunfermline
- Stratheden Hospital, Cupar
NHS Orkney
- Balfour Hospital, Kirkwall
- GP practices
NHS Western Isles
- Uist and Barra Hospital, Benbecula
- Western Isles Hospital, Stornoway
- GP Practices
In total, we conducted 83 interviews. These are summarised in Table 2.
| Stakeholder groups | Interviews |
|---|---|
| Doctors | 30 |
| GPs (15) | |
| Consultants (15) | |
| Nurses | 5 |
| Allied health professions | 13 |
| Dietitians (2) | |
| Occupational Therapist (1) | |
| Physiotherapists (5) | |
| Speech and Language Therapists (5) | |
| Non-clinical managers | 6 |
| Care home managers | 5 |
| Admin / support | 3 |
| EHealth/IT staff | 4 |
| National level stakeholders | 17 |
| Total interviewees | 83 |
Interviews were conversational in style and lasted between 15 and 60 minutes. People were asked to talk about their experience of video consulting (or why they had chosen not to use this medium) and about national or local efforts to scale-up the service as part of the pandemic response. When interviewees talked in the abstract about problems and challenges, we asked them to describe specific examples of these. Most people were interviewed individually but some chose to be interviewed in pairs, and on two occasions as a focus group of up to seven (one with GPs and one with a service improvement team).
Of our 83 interviewees, 36 had been interviewed by our team previously for the pre-COVID-19 evaluation of this service. For those individuals, we also asked how things had changed since we spoke previously.
In addition to the interviews, we used Near Me activity data collected by the TEC programme team during the study period and patient survey data (18,915 responses) collected between 1 August 2020 and 25 September 2020. These user experience surveys were completed online, immediately after the video consultation.
An extensive Public and Clinical Engagement exercise was also commissioned by the TEC Programme during the study period, and has been published online [11]. We have drawn on the data and findings from this report as part of the analysis on patient and clinician perspectives. The engagement exercise combined the use of surveys (online, telephone and written) and focus groups with members of the public and health and care professionals. It should be noted that the majority of the surveys were conducted online, and so the findings could be biased towards those with digital access. However, a proactive approach was also taken to enrol individuals who may represent digitally excluded groups, using telephone and written surveys. In addition the Near Me team formally wrote to over 300 organisations, including professional bodies, seeking views.
2.2 Ethical Approval
The study received NHS Research Ethics Committee (REC) approval in June 2019 (ref 19/LO/0550) and NHS Research Scotland Permissions Coordinating Centre (NRSPCC) approval in October 2019, with subsequent amendments approved in June 2020 and local approvals obtained from R&D departments within each health board
2.3 Data analysis
Data collected by Oxford University were pseudonymised by giving each interviewee a different name (gender and ethnically matched). A spreadsheet of real names and pseudonyms was kept on an encrypted hard drive.
Data was managed and stored confidentially and securely at University of Oxford. We paid strict attention to the General Data Protection Regulations (GDPR) and followed data management and data security policies at the University of Oxford, which can be supplied on request.
Field notes and typewritten interview notes (along with selected audio transcripts) were organised into an Excel spreadsheet, in which each row represents an interviewee (or document) and each column represents a different thematic category. Descriptive statistics were used to analyse routinely collected video consultation and patient survey data. We used Mann–Whitney U and Spearman's Rho tests (non-parametric tests) of significance to analyse factors associated with survey responses and PEI scores.
Data synthesis was guided by the NASSS framework [5]. NASSS is a multi-level theoretical model which helps predict and evaluate the success of technology-supported health or social care programmes. As part of the evaluation undertaken before COVID-19 (up to March 2020), we assessed the challenges and enablers to scale-up across the sub-domains on the right of Figure 3. These were used as an analytic lens to explore recent changes and developments in the context of the pandemic, and implications for longer term sustainability.
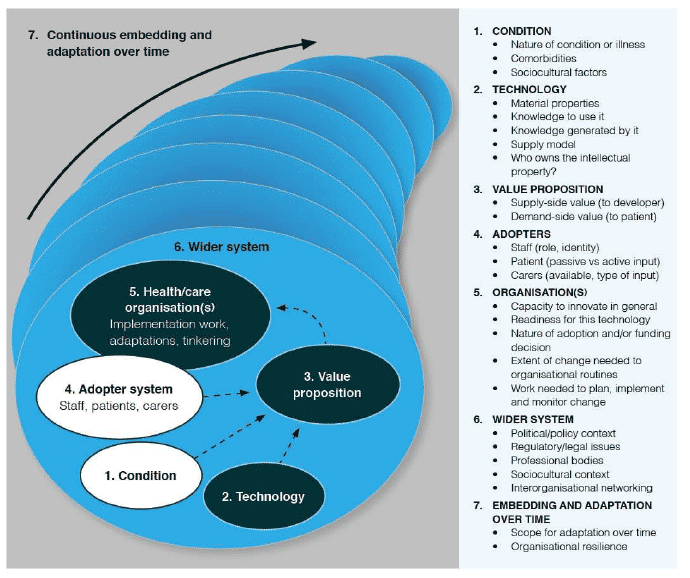
Figure description:
NASSS Framework: acronym for Non-adoption, Abandonment and challenges to Scale-up, Spread and Sustainability. This framework shows the types of individual and organisational challenges to the sustained adoption of technology-supported programmes in health and care.
Contact
Email: Socialresearch@gov.scot