Coronavirus (COVID-19): framework for decision making - assessing the four harms
Sets out the four harms process for assessment used to establish when coronavirus restrictions could be safely lifted after lockdown and the scientific evidence underpinning the decisions.
Harm 2
Introduction
The COVID-19 pandemic is having an impact on our health and social care in Scotland in a number of ways. This includes the impact on our health and social care services, how people are using those services, and how this impacts on health. We also know that the restrictions necessarily put in place to slow the spread of the virus can, in turn, affect many aspects of our population health.
These impacts are not directly attributable to the virus through illness or death from infection, but are the indirect impacts to our health from the requirement to suppress the virus and ensure capacity to respond. These impacts can occur through a wide range of health, family, social and economic mechanisms[42],[43].
When considering Harm 2, we take a number of factors into consideration. These include:
- The demographics and potential needs of those who would be impacted;
- Whether the intervention or change is universal or targeted and the number/percentage of people who would be impacted in Scotland;
- Whether the restriction or measure would affect excess mortality;
- Whether the restriction or measure would change health and social care service use; and
- The potential impact the change could have on people's physical and mental health
Throughout the pandemic, a number of key data and measures have been important in considering impacts for Harm 2 to inform decision making. These have included the anticipated impact on levels of excess non-Covid deaths, levels of use of Health and Social Care services (emergency and planned use), potential avoidance of health care for non-Covid heath issues and changes in population mental and physical health.
Distribution of Harms
We know that the wider health impacts of the pandemic are unevenly distributed across the population. Some groups are particularly vulnerable to the effects of both the pandemic and the potential impacts of social distancing and broader restrictions.
Distribution of harms is likely to closely mirror longer-term, pre-COVID-19 differences in health outcomes across Scotland and across certain demographic characteristics. While certain groups have a higher level of clinical, social or occupational risk of infection, they may also be at greater risk of severe COVID-19 and death.
ScotPHO have produced maps to illustrate a COVID-19 community vulnerability measure based on available demographic, social and clinical indicators relevant either directly to COVID-19 or to socio-economic factors that are likely to modify the impacts of the pandemic and efforts to delay it. Figure 10 shows a snapshot of clinical and social vulnerability at local authority level.
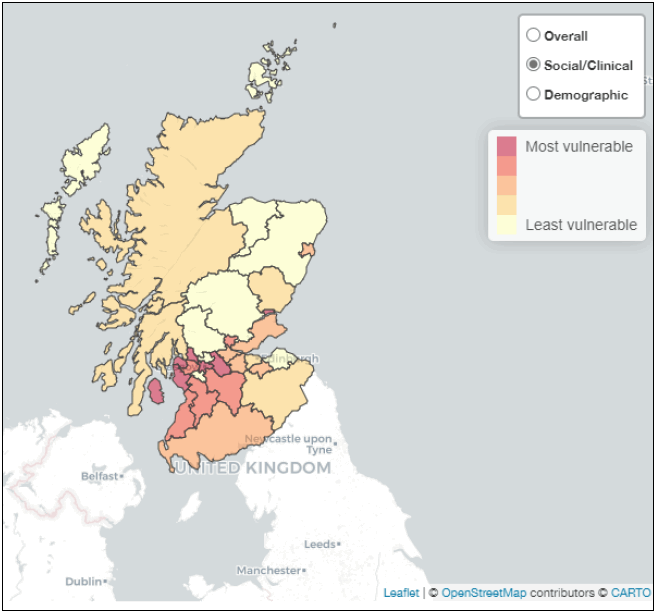
Around 180,000 adults in Scotland were defined on medical grounds as clinically extremely vulnerable due to having an existing health condition that puts them at very high risk of severe illness from COVID-19[44]. This group were contacted individually and advised to 'shield' themselves within their homes. An additional group of people were advised to follow enhanced social distancing, because pre-existing health conditions or circumstances mean they are at increased risk of severe illness from COVID-19[45]. While these were considered necessary to reduce the immediate harm from COVID-19, we know there will be impacts on the health and wellbeing of those shielding or taking additional measures.
Others may also be especially vulnerable to COVID-19's indirect health harms as they rely on health and social care services. These include the elderly, people with pre-existing health conditions (e.g. Chronic Obstructive Pulmonary Disease (COPD), diabetes, substance use), those with disabilities, and people who receive care at home and care home residents.
Excess Deaths
Excess deaths, over and above those from Covid-19, are one indicator of whether wider health impacts are happening. The National Records of Scotland (NRS) data show that Scotland experienced excess mortality in spring 2020.[46] NRS also have data which details the main causes and location of non-Covid excess deaths.[47] In Figure 11 excess deaths are shown as the difference between the weekly average for deaths over the previous 5 years (2015 – 2019) (the grey line), and the blue line showing total deaths in 2020. The other blue line below shows weekly totals for the number of COVID-19 deaths and shows the extent to which COVID-19 deaths have contributed to the number of excess deaths in 2020. There were 186 excess deaths in the latest week (week 48, ending 29 November). The number of deaths where COVID-19 was the underlying cause (215) was actually higher than the total number of excess deaths because deaths from respiratory causes (-32), circulatory causes (-27) and dementia/Alzheimer's (-4) were lower than the average for this time of year.
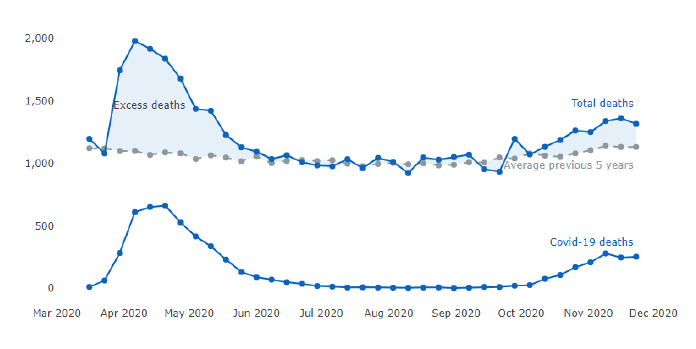
Excess deaths are typically seasonal, with more occurring in the winter, with cold weather and influenza outbreaks being the main causes. Many of the enhanced Infection Prevention and Control measures introduced throughout 2020, across social care and healthcare, could have some positive impact on seasonal outbreaks of other viruses (such as influenza and norovirus). This will be monitored closely.
Health Services
The Scottish Government's Scottish Health Survey (SHeS)[49] demonstrates that almost half of the population lives with a long-term condition (LTC), which may or may not impact on daily life and may require interaction with health care.[50] Prevalence data[51] also illustrate how many of us depend on the NHS or primary care to manage our health. It is important to monitor major health conditions and service use to assess any impacts which result from COVID-19 measures.
The pandemic has prompted rapid and radical change in how we deliver health and care services in Scotland, in some cases accelerating reforms and redesign which were underway pre-COVID-19. On 17 March, the NHS in Scotland was placed on an emergency footing to protect Intensive Care Unit (ICU) and other hospital capacity so that services could cope with potential demand levels from COVID-19 cases. Boards were asked to suspend all non-urgent elective treatment, which has affected referral and treatment pathways since then. Urgent care services, cancer care, mental health, maternity and paediatrics were maintained throughout. Some planned procedures and appointments had to be postponed and national screening programmes were temporarily suspended. From 19 June, Boards started to gradually and safely restart services.
Trends in activity in the NHS, from March 2020, compared to average rates from previous years are published on Scottish Government and Public Health Scotland dashboards.[52],[53] Changes in the use of health and social care services could stem from a number of factors.
- Reduced availability and accessibility (e.g. care and services were limited or postponed to prevent infection);
- Reduced demand for services (e.g. people felt they could wait or wanted to protect services for those with COVID-19, or because they were afraid of catching COVID-19); and
- A real change in demand (e.g. fewer traffic accidents or sports injuries, better IPC (infection protection and control) meaning fewer non-Covid transmissible infections).
Many changes observed in NHS activity indicators since March reflect the re-prioritisation of services and changes in how care is provided. For example, sharp reductions in acute bed occupancy and planned admission rates were largely because many procedures were postponed in March. Since the national "Remobilise, Recover and Re-design Framework" was implemented from late May, activity rates across most specialisms have been steadily returning to pre- COVID-19 levels.
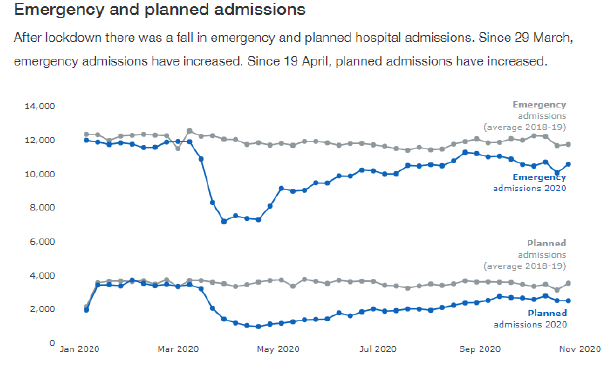
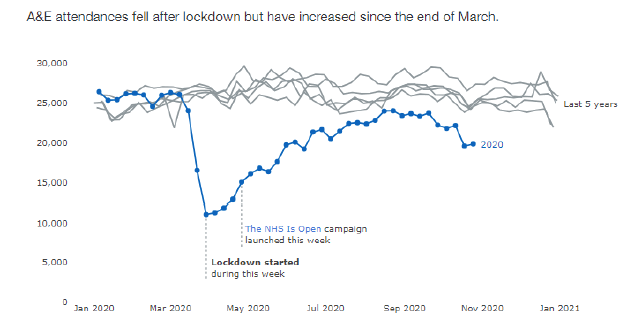
Other NHS indicators are driven by unforeseen need or demand. Accident and Emergency (A&E) attendances, emergency admissions and urgent referrals for investigation of suspicion of cancer symptoms all fell sharply in March though rates have been rising again since May/June. These changes in demand are of concern if people have not been seeking care and support for health problems, as we may have lost opportunities to intervene to improve outcomes for individuals and reduce future demand on services.
Service suspensions and disruptions over March-June have inevitably had an adverse impact on waiting times for secondary care. PHS publish NHS data, at different time intervals, for several important measures and trends (including Referral to Treatment Standards) which illustrate this impact, including the time a patient is waiting from referral to cancer investigation and treatments;[54] outpatient appointments; and various day case and inpatient treatments.[55] For example, Figure 14 shows trends in the number of patients on waiting lists and the number waiting more than 6 weeks for one of eight diagnostic tests, with a sharp increase in the latter indicator in March.[56] At 30 September 2020, 102,716 patients were waiting for the eight key diagnostic tests, This represents an increase of 4.2% (+4,148 patients) from 30 June 2020 and is 17.5% (+15,292) higher than at 30 September 2019. Of those waiting for a test, 53.3% had been waiting six weeks or less (42 days), compared to 35.4% at 30 June 2020 and 82.3% at 30 September 2019. Clearly, delaying tests for potentially serious conditions may have consequences for: eventual patient outcomes if treatment is delayed as a result; for the mental well-being of patients and those close to them given the anxiety delays can cause; for future service demand; and for system and staff resilience as backlogs are dealt with.
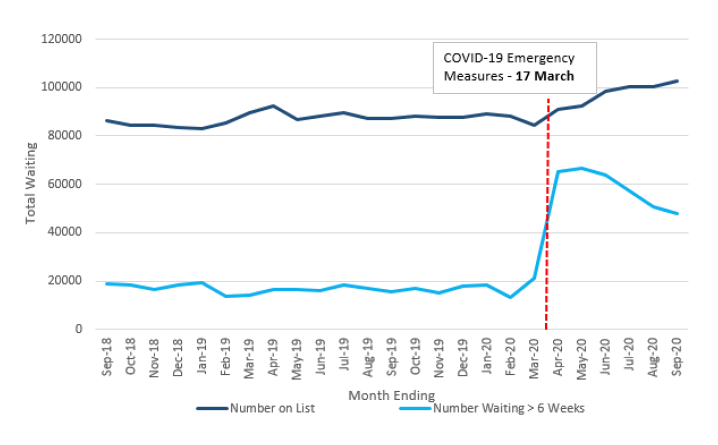
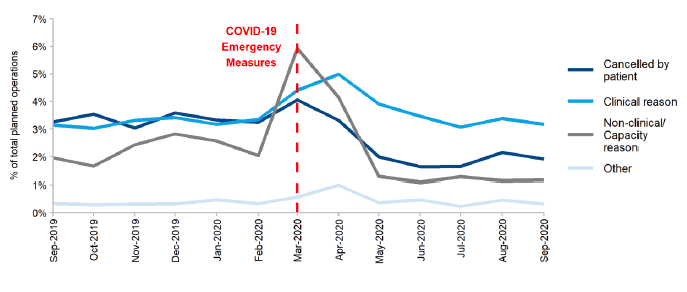
Figure 15, which is based on NHS Scotland data for cancellations on the day or the day before a planned NHS operation, show percentage trends in different reasons for cancellation. From February, with a peak in March, Boards cancelled many operations for clinical and non-clinical/capacity reasons to preserve ICU capacity. However, there was a gradual return towards more usual levels from May as the number of planned operations rose. The total number of planned operations during September 2020 was 17,056, an increase of 23.3% from 13,831 in August 2020 and a decrease of 38.4% from 27,704 in September 2019.[57]
Most people's interactions with health services are through primary care with their GP, a nurse or another member of the Multi-disciplinary Team. We know that there has been a change in the way in which care is provided by GP practices, with increased uptake of phone and video encounters, rather than face to face consultations in practices, where that is clinically safe to do so. The Scottish Government is currently working with stakeholders to expand the evidence base around current demand for GP services. GPs (for example, those in Deep End Practices) have also been documenting the impact of COVID-19 on their own practices.[58]
Throughout the pandemic, primary care remained available for non-urgent, non-COVID-19-related contacts with health services, patients being encouraged to contact NHS24 or to their GP or use NHS Inform. New community treatment centres were established to divert patients with COVID-19 symptoms away from general practice. There were major changes in how services are delivered including substantially increased reliance on the use of remote consultations either by telephone or the Near Me video consultation service and the roll-out of Pharmacy First.
Weekly polling data monitoring public agreement with the statement, "I would avoid going to a hospital or GP practice at the moment even if I had an immediate medical concern (not related to Coronavirus)" has indicated a reluctance by some to seek help even when needed.[59] From a high in April when 45% agreed or strongly agreed with this statement, the rate dropped and has been broadly flat for several months, with 25-30% agreeing.
The statement was changed in the week of 27-28 October to, "I would avoid contacting a GP practice at the moment even if I had an immediate medical concern (not related to Coronavirus)." The latest data (23-24 November) shows a similar proportion (26%) to previous weeks agreed with this statement. This continuing reluctance to contact services is concerning as it suggests a relatively high proportion of people are still not seeking medical help and work continues to encourage and inform people to seek care and advice. Responses have been broadly the same across different demographic groups.
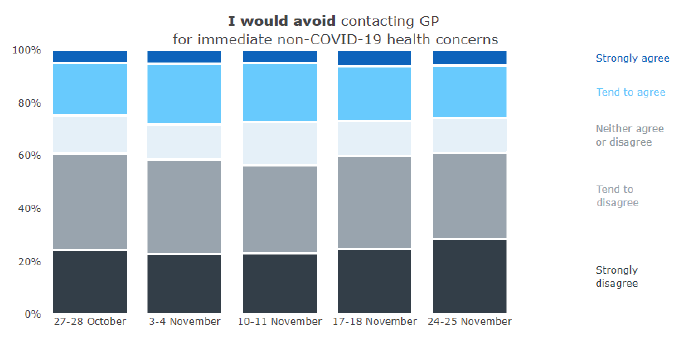
Base approx. 1,000 adults aged 18+, Scotland.
Source: YouGov Coronavirus tracker poll commissioned by the Scottish Government)[60]
We recognise that patient-reported outcomes and experiences since the onset of COVID-19 are a significant gap for person-centred care in current national data. In future, the Scottish Government's Care Experience Surveys will provide us with invaluable information about COVID-19's impacts. There is also an emerging evidence base from research which explores the experiences of particular groups of patients and their families which we will monitor.
Social Care and Support
Around 245,000 (1 in 20) people receive social care and support in Scotland and many are particularly vulnerable to COVID-19. The indirect impacts of COVID-19 and measures to contain it are particularly acute for people receiving and providing social care as they already experience socio-economic inequalities across age, disability and gender.[61] It is, therefore, critical to minimise adverse impacts and maximise benefits from our COVID-19 response to minimise compounding existing inequalities. The Scottish Government's Adult Social Care Winter Preparedness Plan 2020-21 (published on 3 November 2020)[62] and an accompanying Evidence Paper[63] describe direct and indirect health impacts of COVID-19 and actions to help mitigate these.
The recently published Evidence Paper notes a growing body of data and research which demonstrates clearly the significant health and social harms for people who receive social care and support, from restrictions on visiting, on activities inside and outside of home and on mixing with others.[64] There are also consequences from interrupted or avoided healthcare. These apply to those who live in care homes, who tend be much older, and those who receive care and support in their homes. Around 60,000 people in Scotland are receiving home care at any one point, while around 56,000 of these are receiving personal care. People receiving social care are often old and live alone, therefore visits from social care staff may be their only social interaction.
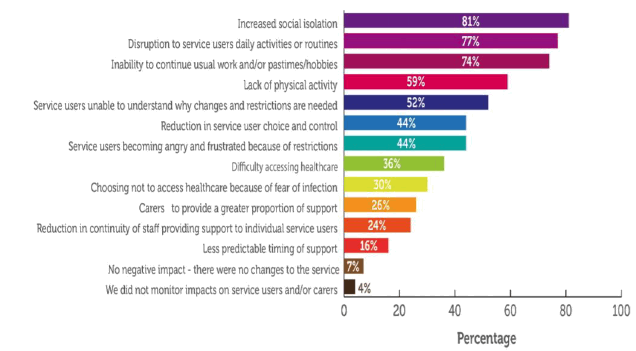
The Care Inspectorate inquiry into Care at Home and Housing Support, found that social isolation, disruption to daily activities, limitations on physical activity and the suspension of re-enablement had all adversely impacted on the health and wellbeing of people who experience care and for their carers. Loss of independence and reduced resilience will increase individuals' future need for care. Lockdown had left many carers exhausted and anxious about the future.
Unpaid carers play a core and essential role in supporting people with social care needs to lead safe, meaningful lives. There are an estimated 690,000 carers living in Scotland, including 29,000 young carers.[65] Carers are more likely to be female, be in the 55-64 year old bracket, have a long-term condition or illness and report lower overall general physical and mental health than the general population.[66] Caring can have adverse effects on carers' financial security, career prospects and well-being.[67] During COVID-19, the importance of unpaid care has increased due to changes in service provision, fewer opportunities for social care support and activities provided by the voluntary and statutory sectors, fewer opportunities for respite, and some families being reluctant to have relatives move into a care home. A UK-wide survey with over 5,000 carers (Carers UK 2020), carried out in April 2020, found that 70% of carers were providing more care due the pandemic and many were experiencing worry or hardship which could have adverse effects on their own health and well-being.[68]
Population health and wellbeing
The health benefits of the measures brought in to help reduce transmission of the virus are obvious, with a slower spread of infection reducing the risk to individuals and of health services being overwhelmed. However, there are unintended consequences for population health[69],[70]and balancing these considerations has been a key aspect of informing decisions around the nature and extent of restrictions and the mitigations in place to help to reduce harm.
General wellbeing, mental health and anxiety
There is increasing evidence that mental health is a significant determinant of overall health, establishing mental health and wellbeing as a major public health priority[71],[72]. It is clear from the evidence that the pandemic is taking a major toll on the population's mental wellbeing which has implications both in the shorter and longer-term for individuals and their families, but also for health services and the support available.
The Mental Health Research Advisory Group refocused its efforts to act as a forum for knowledge exchange to inform understanding and development of the Scottish Government's response to COVID-19 and mental health. They consider a wide range of evidence, including the Scottish Government's commissioned SCOVID Mental Health Tracker study[73]. SCOVID will cover a 12-month period from May 2020. July/August data is currently being analysed and Wave 3 is in the field.
In addition to financial pressures, evidence indicates a combination of social factors, including loneliness and social networks and friendships, are playing a key role in the impacts on mental health and well-being[74]. There is also evidence of longer lasting challenges and of differential impacts, particularly on women (especially young women) and on young people and potential widening of mental health inequalities as the impacts of COVID-19 interact with pre-existing risk and protective factors for mental health[75]. For example, Figure 18 presents some findings from Wave 1 of SCOVID and shows, overall, a quarter of those responding reported moderate to severe depressive symptoms and close to a fifth reported moderate to severe anxiety symptoms. Differential impacts between groups are clearly evident.
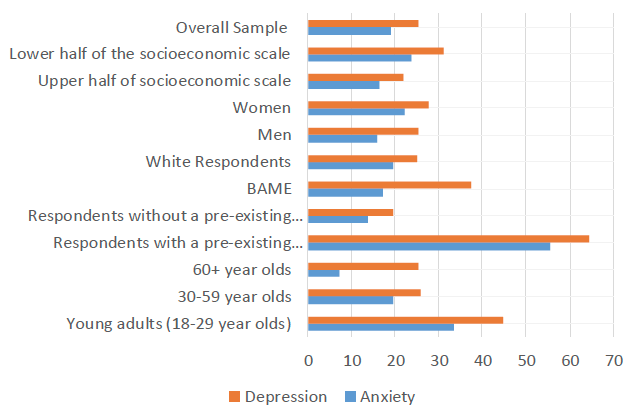
Exercise
Physical activity and sport are a powerful force in transforming lives. Strong evidence, prior to this pandemic has demonstrated the protective effect of physical activity on a range of conditions including coronary heart disease, obesity and type 2 diabetes, mental health problems and social isolation[76]. This reinforces the importance of tracking the impact of the pandemic on activity levels and taking consideration of sport and physical activity encouragement and opportunities when making decisions about the nature of restrictions.
SportEngland introduced a COVID-19 tracker survey from 3 April. This ran weekly to the end of May and approximately monthly since. It provides indications on people's physical activity behaviours and attitudes during the pandemic and across different population groups. This evidence is supplemented by other surveys, analyses and evidence, for example, Scottish Health Survey data from Aug/Sept 2020 on activity and sedentary behaviour will be available early 2021 and data from relevant COVID-19 Waves of the Understanding Society Survey are being analysed. An international review of the impact of COVID-19 on diet, physical activity and weight is available[77].
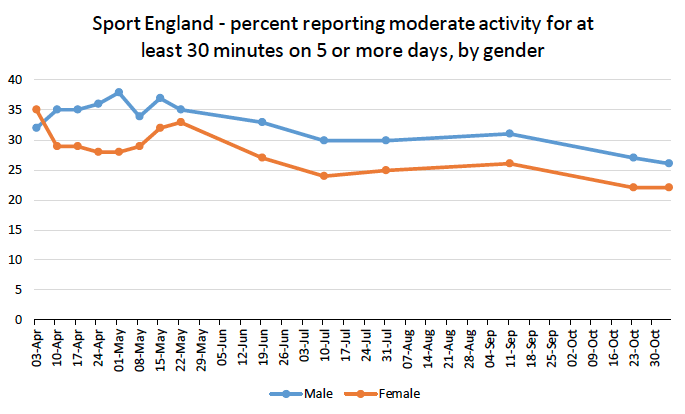
The evidence indicates a mixture of both positive and negative impacts on physical activity. Whilst some appeared to report doing more than previously, especially during the initial lockdown, a sizeable proportion reported doing less with indications that certain groups were particularly negatively impacted - older people, those on low incomes, people living alone, people self-isolating due to age or a health condition and people in urban areas[78]. Even where there were increases, such patterns do not appear to have been sustained, declining as restrictions eased. We are now moving into winter where the prospect of outdoor physical activity may be more challenging with potential for restrictions on indoor opportunities to have greater negative impact.
Food and alcohol
Poor diet is a leading risk factor for ill health[79] in its own right and as a contribution towards development of obesity. Obesity has been linked to a range of conditions including diabetes, cardiovascular disease, high blood pressure, certain cancers[80],[81], mental health problems[82]and dementia[83]. A concern is that observed negative impacts on diet, particularly indications of more snacking on high fat and sugar foods, will impact on diet quality and obesity levels in the longer term if sustained and in turn contribute to increases in these linked conditions.
Evidence also links being overweight or obese and an increased risk of suffering more severe outcomes from COVID-19[84]. The impact of our response to COVID-19 on factors such as diet that influence healthy weight are, therefore, of particular importance. In addition, the restrictions on hospitality and thus changing consumption environments, combined with mental health impacts are likely to influence patterns of both diet and alcohol consumption.
Food Standard Scotland have a regular consumer tracker survey and commissioned a COVID-19 Tracker Survey[85]. From these, and other evidence, the indications are of positive and negative impacts on diets. There are suggested increases in cooking more home-cooked meals from scratch, eating together as a family and a reduction in eating takeaway foods. However, of concern are indicated increases in snacking on unhealthy foods and generally eating more out of boredom[86]. It may be some time yet before it is clear what longer term impact this may have on population health, such as on levels of obesity. There are a wide range of actions already underway in A healthier future: Scotland's diet and healthy weight delivery plan to tackle diet and weight in Scotland, the importance of which are heightened by the pandemic.

Harmful alcohol consumption has been recognised as a major, long-lasting public health challenge in Scotland. Harmful drinking presents a risk of physical and mental health problems, as well as social and economic losses to individuals and society[87]. Some of the harms from chronic excessive alcohol consumption include high blood pressure, chronic liver disease and cirrhosis, pancreatitis, some types of cancer, mental ill-health and accidents[88]. People with problematic alcohol use are likely to have complex comorbidities meaning they are more at risk to harms from COVID-19, are more likely to engage in riskier behaviour and find it more challenging to comply with physical distancing[89].
Combined with substantial changes to the availability of alcohol in light of restrictions on hospitality settings and social gatherings, there is a clear need to understand the impact the pandemic may be having on harmful consumption behaviours. One concern is that the pandemic may lead to the establishment of harmful drinking patterns in a new cohort of people which, in the longer-term, may lead to the harms already outlined and have implications for alcohol support services. The pandemic is also having impacts on services supporting problem drinkers.
A number of measures are being tracked to understand the impacts, including service use and population consumption patterns, with surveys and sales data. COVID-19 has had impacts on alcohol use both at the population level and for those most in need of support. In addition, alcohol treatment services have been impacted with a significant drop in the number of treatment referrals, although this has been recovering to some extent[90].
Population level data suggests there has been a change to the way people drink, with some drinking less as a result of lockdown and feeling the benefits while others reported engaging in more harmful drinking behaviour[91]. It is not clear at this stage what the longer term impacts of these changes will be.Further research is taking place to better understand changes in patterns of consumption, including alcohol sales data. Sales data to date indicate a change in drinking patterns following a move from 'on-trade' (i.e. sales of alcohol in hospitality settings) to 'off sales' (i.e. alcohol purchased to be drunk in private settings).[92]
Drug Use
Drug related deaths in Scotland have been increasing in recent years which is a real cause for concern[93]. There are demonstrated benefits of problem users engaging with support services[94] but the evidence suggests that engagement dropped as a result of the pandemic and there is a risk that this further impacts on drug-related mortality further down the line. People with problematic drug use are likely to have complex comorbidities, meaning they are more at risk to harms from COVID-19 and are more likely to engage in riskier behaviour and find it more challenging to comply with physical distancing[95].
COVID-19 has had impacts on drug use both at the population level and for those most in need of support. A number of measures are being tracked to understand the impacts including service use, the illegal drug market and recreational use. Specialist referrals for drug treatment, use of needle exchange and Opium Substitution Therapy (OST) all dropped with lockdown and were not fully recovered by early July[96]. Drug-related A&E admissions spiked post lockdown which will be of particular relevance to monitor for those areas that moved into the new Level 3 and 4 restrictions. Survey results suggest that recreational drug use has changed – with an increase in cannabis but a decrease in stimulant 'party drug' use, whilst Opiate and Benzodiazepine use remains relevant[97].
Conclusion
In summary, changes in health care service demand and availability are likely to have short and long term consequences for disease prevalence, disability and mortality due to the changes in unscheduled and planned care, preventative services and people's willingness to seek health care.
As winter approaches, the negative impacts associated with Harm 2 may be further exacerbated. With fewer daylight hours and poorer weather conditions, people are more likely to stay at home, have fewer opportunities for outdoor exercise and mental wellbeing may diminish further.
Early evidence shows that the impacts of the pandemic are being felt most sharply by those already most disadvantaged including young people, women, minority ethnic groups, disabled people and those with pre-existing health conditions.
Contact
Email: covidexitstrategy@gov.scot