Chief Medical Officer - annual report: 2020 to 2021
This report is focused around five key themes: the health of the nation, delivering personalised care, reducing health inequalities, sustainability of our workforce, and green and sustainable healthcare.
Reducing Health Inequalities
In December, Professor Sir Michael Marmot published Build Back Fairer: his review on how the pandemic has affected health inequalities in England. His report highlights that:
- the pre-existing socio-economic inequalities in our society led to the disproportionately high number of deaths from COVID-19 in our disadvantaged communities;
- as we recover from the pandemic our nation's health must be the government's top priority;
- strong links exist between the economy and population health; it is, therefore, important that we create a more sustainable economy as we recover from the pandemic;
- to reduce health inequalities and build back fairer from the pandemic, multi-sector action from all levels of government is needed and we must create long-term policies which support equity;
- investment in public health is vital to mitigate the impact of the pandemic on health and health inequalities.
It is a comprehensive and sobering report and all of the above points apply equally here in Scotland.[62]We urgently need to address our health inequalities here in Scotland, which are the worst in western and central Europe.[63] The difference in life expectancy between the most and least deprived ten percent of areas in Scotland is alarming - approximately 10 years for females and 13 years for males.[64] Our premature mortality rates have worsened in our most disadvantaged communities, and inequalities in premature mortality have increased since 2012.[1]
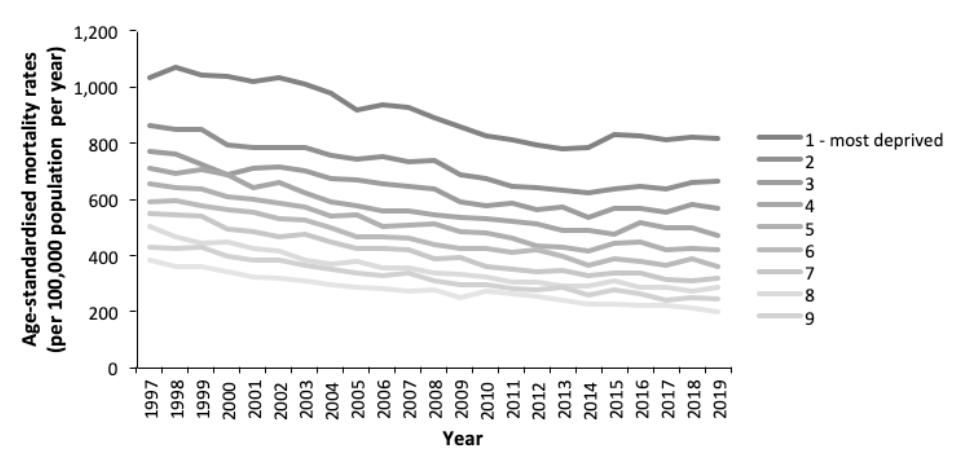
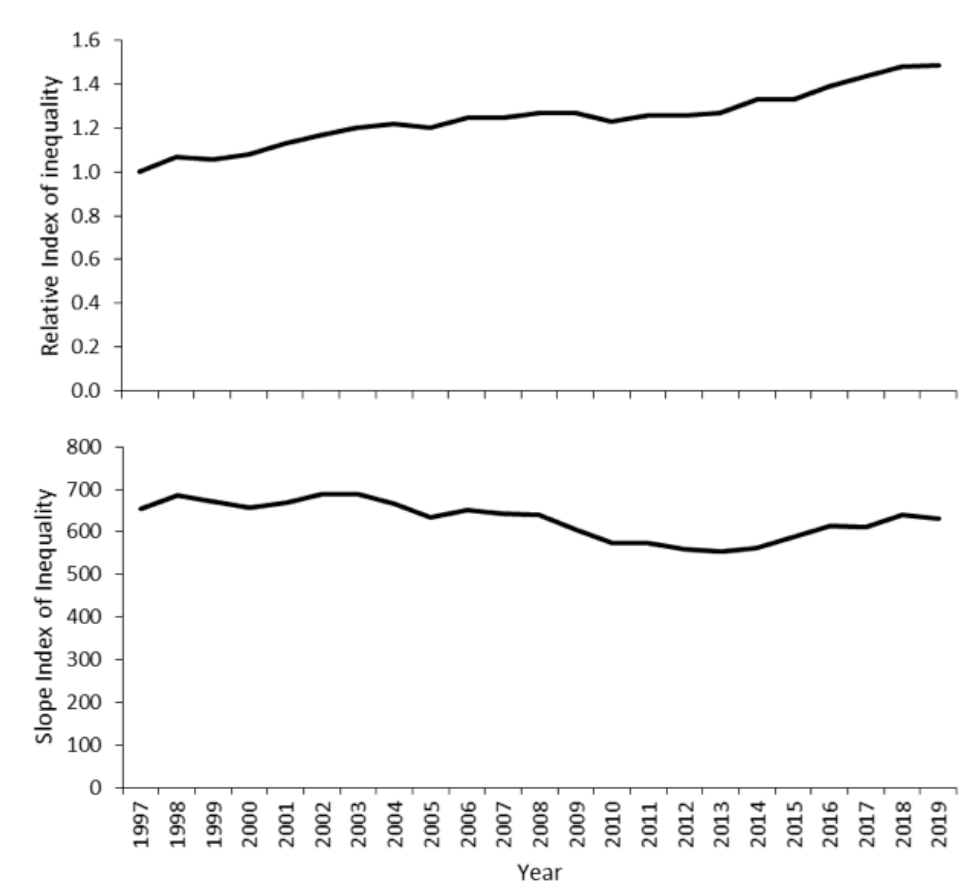
The widening inequalities shown in Figures 1 and 2 predate the pandemic. The direct and indirect impacts of the COVID-19 pandemic are known to have exacerbated these underlying trends.[39]
Although the health of individuals is influenced by genetics and health behaviours, at population level we know that the wider determinants of health such as economic, social and environmental factors are much more important.[65] Although most routine data highlight inequalities by area deprivation, inequalities are also marked when looked at by individual socioeconomic position and for particular disadvantaged groups, such as people who are care experienced, people experiencing homelessness, the Gypsy/Traveller community, and some minority ethnic communities.[66-69]
Inequalities in health are not inevitable, but do exist and are preventing people from living longer, healthier lives.[63,70] These inequalities cannot be resolved by providing good healthcare alone, and are largely determined by circumstances beyond an individual's control.[65]
Social Renewal Advisory Board
The Social Renewal Advisory Board was set up by Scottish Ministers to make proposals that can renew Scotland once we start to emerge from the pandemic. Its final report "If not now, when?" was published on the 21st of January, and proposes a course towards our future. The Board focused on three key principles:
- Money and Work: everyone should have a universal basic level of income from employment and social security.
- People, Rights and Advancing Equality: everyone should have equal basic rights, and access to goods and services.
- Communities and Collective Endeavour: we must work collaboratively to make our society fairer, by devolving more power to our people and communities.
The Scottish Government's Programme for Government (PfG) 2020-21, Protecting Scotland Renewing Scotland published in September, commits Scottish Ministers to take forward a range of proposals presented by the Social Renewal Advisory Board. You can learn more about the Scottish Government's response to the Board's recommendations here.
Build Back Fairer and "If not now, when?" bring to the fore the potential causes of inequalities and what we might do about them. Whilst the wider social determinants of health, such as sustainable employment, access to education, nutritious food, and good quality housing have the greatest impact on health inequalities, there is often a view that our ability as health and care professionals to influence these determinants is limited.[65 ]I am concerned that unless we act now the consequences of our inaction will be felt for decades to come.[23, 41, 71 ]If we wish to understand the lives of, and provide better care for the people who need our help the most, it is important that we fully understand the root cause of these inequalities.
As a GP, I saw the devastating effects of these inequalities on health and families play out before me, and like many people in Scotland I have experienced them first hand in my family. As advocates for those whose voice is often harder to hear, we have a moral responsibility as clinicians to promote agency and act for them when necessary.
Economic Factors and Inequalities
Economic factors are the biggest determinants of population health, and poverty is expected to rise as a result of the COVID-19 pandemic.[39, 72] There is an opportunity to develop an economy, as we come through the pandemic, that supports wellbeing, equity and sustainability. This will be crucial to improve health and reduce health inequalities in the future.
The COVID-19 pandemic has led to considerable worry about household food security. A survey by Food Standards Scotland in May found that 25% of people were either 'very worried' or 'somewhat worried' about their household not being able to afford food in the next month. Food banks and other food aid organisations also reported considerable increases in demand for their support as people experienced increased financial difficulties at this time.[73]
Measures taken to control viral spread during the pandemic have meant that many businesses and organisations were forced to temporarily close, or significantly adapt their ways of working. Unemployment is correlated with increased risk of poor physical and mental health, and an increase in the prevalence of health-harming behaviours.[74] Employability support is crucial in Scotland's economic recovery from the COVID-19 pandemic.
Financial difficulties can have a major impact on both physical and mental health. Welfare Advice and Health Partnerships have an important role to play in supporting people with financial concerns, and this video highlights how we, as professionals in health and care can help.
What matters to you? "Money to feed my children and heat my home"
Welfare Advice and Health Partnerships (WAHP) are a public health response to better support the wellbeing of people experiencing disadvantage. Developed in primary care, WAHP are embedded in over 100 GP practices across Scotland, mainly in our most disadvantaged communities. They provide people with expert and regulated social welfare legal advice. This includes support with income maximisation, welfare benefits, debt resolution, housing problems and employability support as well as representation at tribunals. They also link patients into other sources of support, if appropriate. The people they provide support for experience significant poverty and deprivation. For example a study of WAHP in 17 GP practices in Glasgow found that 53% of patients had a household income of less than £10,000 per annum, with 20% of those surviving on a household income of less than £6,000 per annum. Amongst the 654 people supported in the pilot, a total of £1.5 million in additional income was gained. WAHP empower GPs to ask patients 'what matters to you?' in the knowledge that any social or economic concerns can be dealt with by an expert in the practice which for many is a non-stigmatising and familiar environment. A GP recently said:
"Patients often present with stress and when you scratch the surface money is a big cause. I feel strongly that in deprived areas patients struggle with the idea of going somewhere unknown due to anxiety, transport issues, fear of the unfamiliar and this results in them not accessing health and social care services. GP practices are still one of the few places that they are prepared to go".
Everyone deserves the same start in life, and we must endeavour to support every child to thrive.[75] Significantly, more families are relying on benefits due to the pandemic, some perhaps for the first time.[76] We know that socio-economic disadvantage and child poverty are much greater in some areas than others. Scotland has ambitious income-based targets toward the eradication of child poverty set in statute through the Tackling Child Poverty Delivery Plan, but there is much more to do. Every child has the right to an education, to enable them to develop to their full potential.[75] We need to work towards reducing the attainment gap in education. The impacts on children due to reduced face to face learning during the pandemic also needs to be addressed, with a particular focus on children from disadvantaged backgrounds.[77]
Access to sanitary products is a basic health requirement but products are expensive, which can act as a barrier to access for some women and girls, resulting in significant emotional stress and reduced participation in society.[78] The Period Products (Free Provision) (Scotland) Act 2021, which was passed by the Scottish Parliament on 24th November and gained Royal Assent on 12th January, is a historic piece of legislation which ensures free period products are widely available. The Act is an excellent example of legislation that will help to tackle health inequalities.
Marginalisation and Inequalities
People at the margins of our society experience greater inequalities and lower life expectancy, such as people in or at risk of homelessness, people involved in the justice system, asylum seekers, refugees, and Gypsy/Travellers. This marginalisation can result in increased distress and use of emergency and Out-of-Hours medicine, custodial care, mental health and substance use interventions.[79]
We can help people regain control by placing them at the centre of their care through shared decision-making and adopting a rights-based approach. Survivors of trauma are at higher risk of a range of health, mental health and social issues. The 'Inclusion Health' approach recognises individuals' right to health.[79] It addresses inequality by responding to the urgent challenges of increasing homelessness and drug deaths which are marked by experiences of exclusion, violence and poverty.
A national training video has been designed to support workers build a personalised approach to care and make a positive difference to people affected by such adversity. I encourage you to watch it.
Migrant and/or Undocumented Children Guidance
Many of us will be involved in the care of migrant or undocumented children during our careers and it is important we are equipped with the knowledge to provide them with the best possible care. The health needs of children seeking asylum differ greatly from those living permanently in Scotland and such families are often frightened to access services. We need to ensure we appropriately assess and safeguard this group. The Royal College of Paediatrics and Child Health has published guidance on refugee and unaccompanied asylum-seeking children and young people. It aims to assist us in the assessment and management of children and young people of refugee background.
Ethnicity and Inequalities
Scotland is enriched socially, culturally and economically by the diversity of our communities. Nevertheless, inequalities remain in various aspects of life for minority ethnic communities in Scotland. Many people face poorer health outcomes due to a higher risk of poverty, lower employment rates and under-representation in our society.[69] It is important that we mitigate these inequalities. Simple measures like ensuring we use translator services and provide information leaflets in people's preferred language, or recruiting members from minority ethnic communities to help with health promotion such as awareness and uptake of cancer screening, can make a huge difference in improving the accessibility of healthcare for our minority ethnic groups.[80] The Scottish Government's approach to tackling race inequalities is outlined in the Race Equality Action Plan.
Ethnicity Coding
Some minority ethnic groups have been disproportionately affected by the COVID-19 pandemic and they face poorer health outcomes in general.[40, 69 ]This has unearthed longstanding issues with coding for ethnicity, which is a barrier to monitoring and ultimately understanding the health needs and outcomes of our minority ethnic communities. NHS Lothian has tackled this issue head on and succeeded in improving ethnic coding of hospital records from 3% to more than 90% during the pandemic.[81] We must strive to improve health informatics so that we can better understand the health needs of our communities.
Adult Social Care and Inequalities
Governments around the world have grappled with social care issues for decades. In September, the First Minister announced an Independent Review of Adult Social Care in Scotland, which was chaired by Derek Feeley, a former Scottish Government Director General for Health and Social Care and Chief Executive of NHS Scotland. The review was published in February and was well received by service users and providers. It outlines Mr Feeley's recommendations on how we can support improvement in adult social care in Scotland to enable better outcomes for all. This video outlines the findings from the review and the vision for world leading social care. It is vital that we take these forward and transform services.
Social Connectedness and Inequalities
Loneliness and Isolation
To be healthy, we need to feel included in society. Loneliness can have a big impact on health.[82] We should support people to access programmes to help reduce isolation and loneliness within our local communities. The Glasgow Health and Social Care Partnership (GHSCP) has supported the Wellbeing for Longer Fund in Glasgow. Programmes include the Scottish Ballet working with people with dementia, Golden Generations supporting older people with digital inclusion, the Glen Burn Centre My Life My Choice programme offering photography, as well as a range of other physical activity and cooking programmes.
Digital Connectivity
Digital connectivity has proven to be vital for our health and wellbeing during the coronavirus pandemic, whether supporting our health service, enabling people to work and study from home, or staying connected to friends and family. Yet there remains a digital divide in Scotland which we must address if we are to support people to flourish.[83] We must build on the work of the Connecting Scotland programme and continue to invest in Scotland's digital connectivity infrastructure to help ensure that everyone in Scotland, even in rural areas, can access superfast broadband through the Reaching 100% Programme (R100).
Health Behaviours and Inequalities
As well as having a devastating impact on the wider determinants of health, the pandemic continues to impact on many people's health behaviours, which will not be observed equally across our society.[34] Smoking, alcohol consumption, poor diet and obesity are major contributory factors in the leading causes of preventable deaths in Scotland, such as cancer and diseases of the circulatory system.[84]
International evidence points towards commercial determinants of health driving these consumption behaviours, and we know that these are also compounded by adverse economic and social circumstances.[72] People living in our most economically disadvantaged communities are five times more likely to die from heart disease and twice as likely to die from cancer as people living in our least deprived areas.[1] We must do more to support people to adopt healthy behaviours to reduce preventable deaths and related health disparities in Scotland.
Smoking
Five times as many people smoke in our most disadvantaged communities compared to our most affluent.[85] Smoking prevalence also significantly exceeds the national average in other groups such as in men aged 25-54, those facing unemployment, individuals with no or limited qualifications, those with a limiting long-term physical or mental health condition, White Polish communities, LGBT+ groups, single adult and single parent households.[85 ]The Scottish Government's Tobacco Control Action Plan sets out how we will reach our goal of creating a tobacco-free generation by 2034. Actions include targeted smoking cessation support, early intervention, environmental measures and fiscal policy to reduce uptake of smoking. The smoking ban in prisons has had a significant impact on reducing smoke exposure in this high-risk population.[86]
Alcohol
There is a stark health inequalities gradient to alcohol-related harm in Scotland. In 2019-2020, alcohol-related admissions to acute general hospitals were seven times higher in our most disadvantaged areas compared to the least.[87] While the Scottish Government's Alcohol Framework aims to encourage a change in culture around alcohol, where lower alcohol consumption moves the population closer to the recommended 14 units per week maximum, we must be mindful that the challenges brought about by the pandemic may well encourage people to drink more. Our Alcohol Brief Intervention service has been expanded to our pharmacies, criminal justice settings and community services to ensure it is accessible to people from our disadvantaged communities. Minimum unit pricing has also improved health behaviours around alcohol.[88] While still far too high, notably, the number of alcohol-specific deaths is now sitting at its lowest level since 2013.[89]
Obesity
The inequality gap in obesity rates is widening and has become particularly pronounced in women over recent years. In 2019, obesity prevalence was 40% in our most disadvantaged communities compared to 18% in our most affluent.[85] We now see these trends in children. We want to live in a Scotland where everyone eats well and is able to maintain a healthy weight, yet we know people living in poverty have a higher obesity prevalence which contributes to poorer health outcomes.
The Scottish Government's ambition is to halve childhood obesity by 2030, and to significantly reduce diet-related health inequalities.[90] We need to focus on measures to transform the overall environment that influences what we buy and eat. I welcome the Scottish Government's intentions to introduce legislation on restricting food promotions as soon as possible. We must also continue our work with Food Standards Scotland and Public Health Scotland to support a targeted approach to improve healthier eating for people with low incomes.[91]
Physical Activity
We know that regular exercise improves our physical health, boosts our immune system, enhances our mental health and supports management of our weight.[92-93 ]As professionals in health and care we need to promote these benefits and do what we can to encourage and support people to adopt active lifestyles equally across society. During the pandemic many people have lost access to gyms and recreational sport. Fewer of us are travelling to work, resulting in a reduction in active travel. Many of us are also juggling working from home, home schooling and the challenge of trying to keep ourselves and our children active.
A series of evidence-based blogs and infographics have been created by the Edinburgh Napier University, with contributions from the Physical Activity for Health Research Centre at the University of Edinburgh and the University of Stirling to motivate people to keep active during the pandemic. They are targeted at adults and those working from home; vulnerable groups, school aged children and babies and toddlers. These resources provide practical examples of activities that don't require specialised equipment and explain how keeping in touch with friends can help motivate you to keep active.
I would encourage us all to share these infographics on social media within our communities and utilise them to encourage people to exercise. We need to continue to promote the message that:
- something is better than nothing - even a 10-minute walk around the block can boost mood;
- there are great benefits to leaving the house for exercise at least once a day;
- for those of us who are shielding or unable to leave the house, all movement around the house is good. Lack of movement means loss of muscle strength and risk of falls for frail older adults;
- for those recovering from feeling unwell with potential COVID-19, avoid strenuous activity as you recover. Start slowly and build up activity. As things return to normal - keep activity levels up.
We must also ensure equity of opportunity to participate in physical activity. The Scottish Government's Active Girls programme is working to address issues around body image as a barrier to participation, and the Football Fans in Training programme engages men and women from our most disadvantaged communities in accessible physical activity. Moreover, Scottish Leisure Trusts such as the Fife Sports and Leisure Trusts, provide extensive programmes committed to provide physical activity to all, regardless of age, health or status. These programmes are delivered in local community venues allowing for better accessibility. Programmes promote improved physical and mental health, improve quality of life, help with disease prevention and increased social connectedness.
As professionals in health and care it is our responsibility to promote health and prevent disease. Conversations about health behaviours can be uncomfortable for people, and those who care for them. We need to normalise these discussions and conduct them in a sensitive manner so that people feel listened to, and adequately supported to make a change. We should also utilise expert services such as smoking cessation support and weight management services. We need to focus on prevention and early intervention. We must take action to empower communities by co-creating services with those most at-risk and implementing population wide measures to support people to adopt healthy behaviours.
Drug-related Deaths
We are in the midst of a drug crisis, with more drug deaths per capita in Scotland than any other European country. Drug-related deaths increased by 6% in 2020, with over 1,200 deaths.[94-95] These deaths continue to have a devastating impact on our communities and families across Scotland. That is why tackling drug-related harm must continue to be a priority. The impact of drug harms and drug deaths is felt far more significantly in our more deprived communities.[94-95] Helping to reduce harm and the number of deaths will have a positive impact on health inequalities. People who die as a result of drug use die at a much earlier age than from alcohol or smoking. The recent increase in drug-related deaths is one of the main causes for our stall in life expectancy in Scotland, which had been increasing over recent years.[1]
The rise in drug-related deaths requires substance use to be treated as a public health, rather than criminal justice issue. In response to the continuing rise in drug-related deaths the First Minister made a statement to Parliament on the 20th of January, setting out a new national drugs mission and five priority areas for reducing drug deaths. The First Minister also announced the appointment of a dedicated Minister for Drug Policy, and announced additional funding over the next five years. It is expected to improve drug treatment services in Scotland, providing fast and appropriate access to treatment, residential rehabilitation, and support to front-line and third sector services. We also want to introduce a range of evidence-based public health measures, such as overdose prevention facilities, and drug checking services, as well as expanding the provision of heroin assisted treatment across Scotland.
Central to the new mission is the need to increase the number of people who engage with treatment or recovery services. By working together, we will better understand what more can be done to help create a supportive culture in our communities and help shape Government policy and treatment services that people value. It is vital we continue to listen to and learn from communities and people with lived experience. The Drug Deaths Taskforce has developed a Stigma Strategy to tackle the stigma associated with substance use, which we recognise as one of the main barriers stopping people reaching out for help from services.
The Drug Deaths Taskforce recently published a Forward Plan outlining actions it will take over the next two years. This includes bringing in national standards for Medication Assisted Treatment (MAT), which uses licensed medications such as methadone and buprenorphine. The plan will also look to continue to improve public health surveillance to better equip us with the information needed to tackle this crisis.
The COVID-19 pandemic has accelerated the rapid implementation of a number of new and innovative approaches across Scotland, including the Scottish Ambulance Service national programme of take-home naloxone distribution following non-fatal overdose. We must retain and build on our successes to reduce the levels of harms associated with drug use.
Deep End GP and the Wider Primary Care Team: At the Front Line of Health Inequalities
"The availability of good medical care tends to vary inversely with the need for it in the population served. This inverse care law operates more completely where medical care is most exposed to market forces, and less so where such exposure is reduced. The market distribution of medical care is a primitive and historically outdated social form, and any return to it would further exaggerate the maldistribution of medical resources."
Julian Tudor Hart[96]
The impacts of the 'inverse care law' are felt most acutely by our most disadvantaged communities.[96] People are more likely to have multiple complex health and social problems and use unscheduled (emergency and out-of-hours) care more often.[97] These complex issues cannot be addressed in a single appointment but are best supported through relationships of trust which we can build over time.[98] It is important, therefore, that we apply Sir Michael Marmot's principle of 'Proportionate Universalism' – that services are universal, but additional resources are targeted to where needs are greatest.[99]
Pioneering work has been undertaken in this field by the Deep End GP group. There is evidence of improved patient enablement with longer consultations in very deprived areas.[98] The CARE Plus study demonstrated improvements in quality of life and wellbeing by targeted longer consultations that took an empathic, person-centred approach.[97] General Practitioners reported that the extended consultations provided them with a window of opportunity for health screening, health promotion and more in-depth assessment of medical problems in a cohort of people who might otherwise have been missed.[97] The Scottish Government funded project Govan SHIP built on the excellent research from Care Plus, and implemented it in four Deep End practices in Govan.
General practice and the wider primary care team, by virtue of being embedded within communities, can play a pivotal role in mitigating the effects of health inequalities at a number of levels: through clinical care; wider patient advocacy; community engagement; and influencing the wider health agenda.
Community Link Workers are practitioners based in, or aligned to, a GP practice or cluster. They work directly with people to help them access services beyond medicine, and provide them with the support they need to improve their health and wellbeing. There remains plenty of scope for GP practices to learn from and adopt this approach.
Conclusion
The levels of social, environmental and economic inequality in our society are damaging our health and wellbeing. As we emerge from the COVID-19 pandemic there is an urgent need to do things differently, and build a fairer, healthier society based on the principles of social justice.
Whilst the wider social determinants of health, such as sustainable employment, access to education, nutritious food, and good quality housing have the greatest impact on health inequalities, there is often a view that our ability as health and care professionals to influence these determinants is limited. I am concerned that unless we act now the consequences of our inaction will be felt for decades to come. It is important that we fully understand the root causes of these inequalities, if we wish to understand the lives of, and provide better care for, the people who need our help the most.
This will require a whole-system approach.[71] As healthcare professionals we need to understand the challenges the people we care for are facing, and continue to seek out new ways of delivering personalised care. We also need to consider how our workforce can be made more diverse, using our anchor institutions to influence and deliver change in our communities.
We must recognise the power of our health and care system as an employer, asset owner, and purchaser to transform the way we support our local communities. We cannot do it alone. We need to broaden our reach and connect with those who can positively influence the wider determinants of health. Together we can focus on improving the wellbeing and quality of life of the people we care for.
Public Health Scotland (PHS), Scotland's new national organisation for public health, is ideally placed to help us. It has produced a range of materials, measures and tools that aim to help us reduce inequalities, at national and local levels. In previous CMO Annual Reports, we have highlighted tools such as the Scottish Burden of Disease study and the Scottish Atlas of Healthcare Variation, which can help us eliminate unwarranted variation in health. On International Human Rights Day, PHS also published training materials on reducing health inequalities, which will provide useful knowledge and skills to professionals in health and care. In September, PHS published its first strategic plan and I fully support its ambition to create 'a Scotland where everybody thrives' .
Considerations
- What will we do to tackle health inequalities in our everyday practice?
- What will we do to ensure more equitable access to the services we provide?
- How can we help the people we care for, by promoting agency and supporting access to the services they need which often sit beyond healthcare?
Contact
Email: RealisticMedicine@gov.scot