Chief Medical Officer - annual report: 2020 to 2021
This report is focused around five key themes: the health of the nation, delivering personalised care, reducing health inequalities, sustainability of our workforce, and green and sustainable healthcare.
Health of the Nation
A healthier population could be one of our nation's most important assets and must be our ambition. In this chapter I share key statistics and figures that demonstrate the current health of the nation amidst the COVID-19 pandemic. I will provide a summary of the current issues affecting Scotland's population health with a particular focus on the urgent need to tackle health inequalities, which have been magnified during the pandemic.
Stalled Life Expectancy Trends
Improving the length of time people live in good health is a core objective of the Scottish Government's National Performance Framework (NPF), and of the United Nations, through their Sustainable Development Goals (SDGs). Until around 2012, average life expectancy had been increasing steadily in Scotland. This increase has subsequently stalled with little or no improvement since then. Of concern is emerging evidence that healthy life expectancy has also stopped improving over the last decade.[1-3]
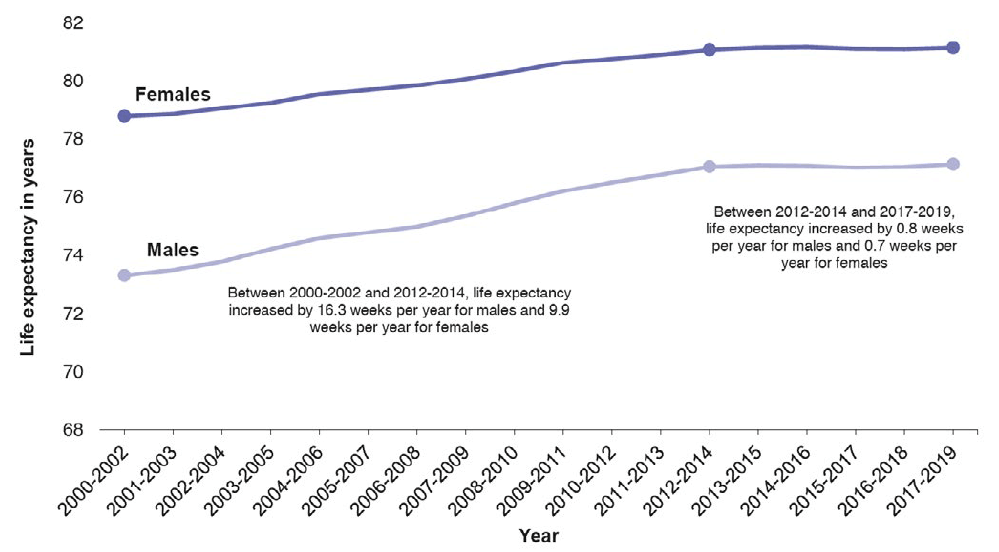
Since 2012, life expectancy trends have stalled not only across Scotland (Figure 1), but also in England, Wales, Northern Ireland, the USA and some European countries.[4] In Scotland, there has been an accompanying rapid increase in inequalities in life expectancy, with life expectancy noted to be decreasing in the most deprived 40% of areas.[1] A particular concern is the rise in drug-related deaths which has impacted mostly on adults aged 35-55 years living in disadvantaged areas in our cities and urban areas.[5]
The reasons for these trends have been fiercely debated. Several studies attribute our stalling life expectancy to the consequences of austerity-driven constraints on health, care and other public spending, and their impact on public services.[6-8] A reduction in people's income is also thought to have led to worsening health outcomes.[9 -11] Across Great Britain, the incomes of the poorest tenth of households are estimated to have decreased by 8% in real terms between 2011/2 and 2021/2.[12] It is also thought that austerity led fiscal policies have resulted in welfare cuts, increased barriers to receiving benefits and failing wages that have not increased in line with inflation. These are all factors that may contribute to a real loss of income for many.[12] Modelling of the impact of these changes in income predicts marked reductions in life expectancy and increases in inequalities.[13]
A range of studies suggest changes to economic and social policies have impacted on our health through increased insecurity, poverty, material deprivation, destitution and stress.[14-18 ]
Other studies, while acknowledging that austerity may have contributed toward some excess deaths, suggest that that there could be other explanations such as the growing complexity of medical conditions in our ageing population, the contribution of decelerating improvements in cardiovascular disease (CVD) mortality, and periodic bad flu seasons.[19-20]
It has also been noted that the slowdown in mortality improvements is occurring at a time when health and care services have experienced increasing demand and unprecedented financial pressures. There is evidence that increased pressure on services is associated with worse mortality trends and may be a contributory factor to life expectancy trends. [21-22]
What impact will COVID-19 have on life expectancy?
Predicting the impact of COVID-19 on life expectancy is difficult for several reasons. The large numbers of deaths that COVID-19 has caused, or hastened, among people with pre-existing conditions and frail older people may be counter-balanced by fewer deaths in the future. Some of our excess deaths could be offset by fewer deaths from air pollution and transport accidents.[19] The indirect impact of COVID-19 caused by socio-economic factors could also have an adverse impact on health and mortality overall and are difficult to quantify. The overall impact that this pandemic is likely to have on life expectancy will become clearer in due course.
The Impact of COVID-19 on Health and Wellbeing
The COVID-19 pandemic is one of the biggest population health challenges we have faced. Figure 2 shows the adverse impact the pandemic may have had and may continue to have on the health and wellbeing of our population. It includes both the direct impact of the virus as well as the unintended consequences of the control measures we implemented to reduce the spread of the virus.[23-24]
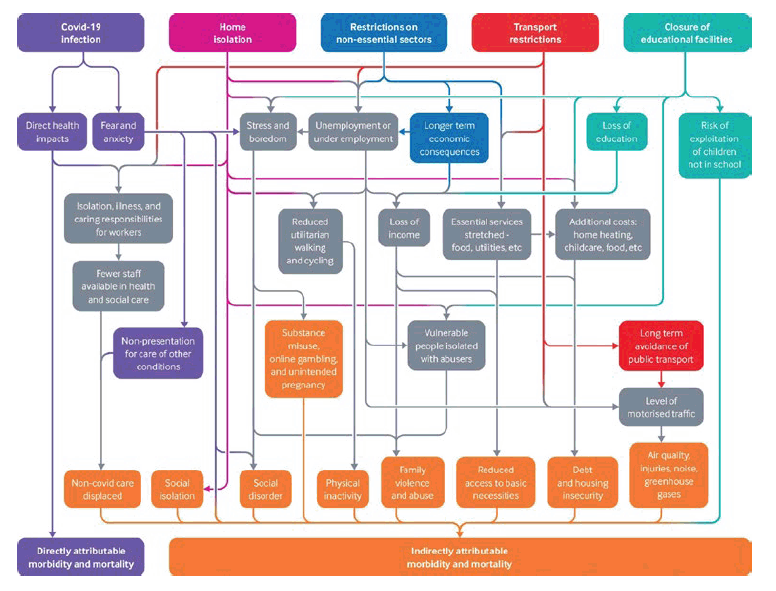
Direct COVID-19 Impacts
Direct Deaths from COVID-19
Figure 3 shows the weekly number of deaths in Scotland where COVID-19 was mentioned on the death certificate, either as the confirmed underlying cause of death, or a contributory cause. There is near real-time, daily published data available from both National Records of Scotland (NRS) and Public Health Scotland on the number of people who received positive COVID-19 tests, and the number who died within 28 days of a first positive test. Under the wider measure produced by NRS, as of the 14th of February, there have been a total of 9053 deaths registered where COVID-19 was mentioned on the death certificate.[25]
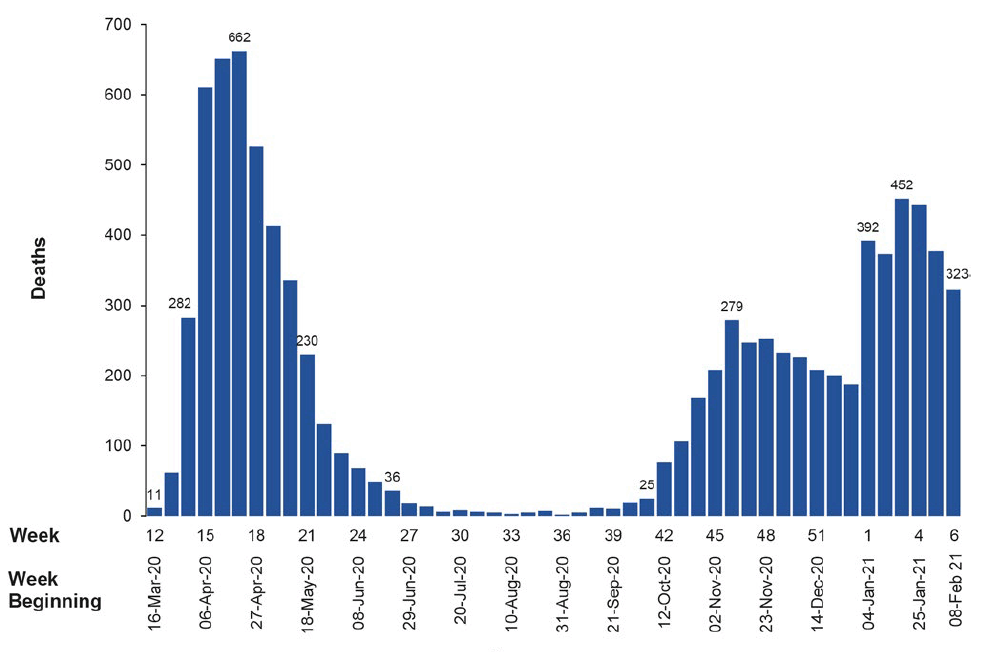
The majority of those who have died directly from COVID-19 so far have been elderly or those with pre-existing health conditions. While the number of years lost in terms of average life expectancy in this cohort may be small, the rapid spread of the virus may cause a high level of excess mortality through direct and indirect effects, thus having a substantial impact on our life expectancy trends.[24]
There is concern that there may be long-term health consequences for a proportion of people who have been infected with COVID-19 (often described as long COVID). As this is a new virus, the proportion of people affected, the range of symptoms they experience, and the length of time they experience them for is not yet fully understood.[26] Guidance to help us care for people who have signs and symptoms of long COVID has been developed.[27]
Excess Deaths
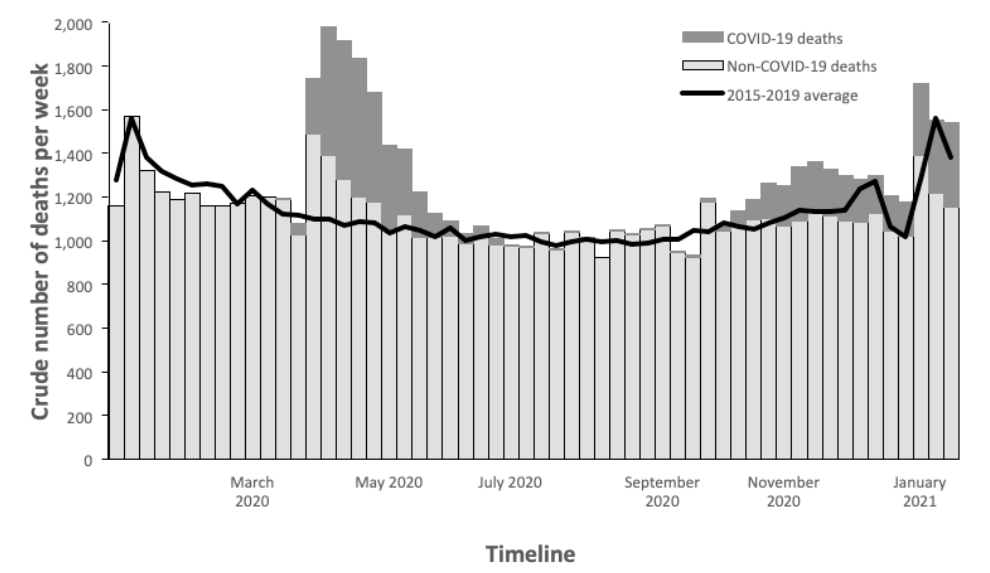
Excess deaths in Scotland are defined as those in excess of a pooled average for the same weeks during 2015-19. Excess deaths include deaths caused by COVID-19 and those resulting from other causes.[28] In Figure 4, excess deaths are shown by the difference between the solid black line, which shows the weekly average for deaths over the previous five years, and the top of the grey bars which shows the total number of deaths since the start of 2020. The number of deaths certified as COVID-19 are indicated by the size of the dark grey bars. This shows that about a third of the excess deaths during the first wave in April-May were not certified as being due to COVID-19. Through the summer and early autumn, deaths returned to the long-term average. During the second wave from November onwards, COVID-19 accounts for all of the excess deaths in Scotland, with other deaths being slightly lower than the long-term average.[28]
Indirect COVID-19 Impacts
There have been wide indirect impacts on our health, society and the economy as a result of the measures introduced to control the pandemic.[29] These impacts, along with the direct health impacts of COVID-19, have informed and supported decision making through the Route Map process and Local Protection Levels, as detailed in the Framework for Decision Making – Assessing the Four Harms of the Crisis.[30]
Indirect Impacts on Health
The pandemic has prompted rapid and radical change in how we deliver health and care services in Scotland. On the 17th of March last year, NHS Scotland was placed on an emergency footing to enable our services to cope with potential demand levels from COVID-19 cases. Our NHS Boards were asked to suspend all non-urgent elective treatment which has affected referral and treatment pathways since then. Our national screening programmes were temporarily suspended. Urgent care, cancer care, mental health, maternity and paediatrics services were maintained throughout. Since the implementation of Re-mobilise, Recover, Re-design: The Framework for NHS Scotland in May, our Health Boards have started to gradually and safely restart services. Activity rates across most specialities have increased since April-May, but have not yet returned to pre-pandemic levels.[31]
In terms of indirect impacts on our health, a sizeable proportion of the excess deaths in Scotland during the COVID-19 pandemic have not been coded as being directly due to COVID-19. This amounts to about one-fifth of excess deaths in weeks 12 to 25.[32 ]This finding may be supported by various hypotheses about non-COVID-19 excess mortality, including undiagnosed COVID-19, reduced use of health services by those that would have benefited from them, and unintended consequences of measures taken to control the spread of the virus. [32-33]
Throughout the pandemic we have been concerned that people with symptoms and conditions unrelated to COVID-19 requiring urgent attention, such as those associated with strokes and heart attacks, have not sought our help. There are also concerns that pauses in national screening programmes might cause delayed or missed diagnoses of cancer. There were substantially fewer referrals for outpatient appointments and mental health services between April and June.[33 ]The longer-term impact of delayed or missed diagnoses or treatment is yet to be determined.
Despite our considerable efforts to persuade people who need medical attention to access services, there appears to be hesitancy from a portion of the general public to seek non-COVID-19 healthcare treatment. Evidence suggests that since the end of October to present, between 24-33% of the general public surveyed 'agreed' or 'strongly agreed' that they would avoid contacting a GP practice at the moment, even if they had an immediate medical concern.[33 ]This is also reflected in the ongoing lower use of services than we would expect in, for example, relation to cancer services.[31] The 'NHS is Open' campaign which was launched in April aimed to encourage people not to delay seeking medical advice when required. There must be a continued, consistent and concerted effort to keep reminding people that primary care and hospitals are open and urgent care remains available.
Societal Impacts
The COVID-19 pandemic has had a major impact on our health, economy and society, with damaging impacts on our way of life and wellbeing. Scotland's Wellbeing: The Impact of COVID-19, brings together evidence on the ways that the pandemic has affected Scotland's progress towards our National Outcomes, which are set out in our National Performance Framework.[34]
There has been significant disruption to the delivery of education and to the social lives of our children and young people.[34] Intensive efforts will continue to be required to mitigate against longer-run negative impacts for children and young people, whilst keeping the spread of the COVID-19 virus to a minimum. It will not be easy, and we will need to continue to make some difficult decisions in an attempt to get the balance right.
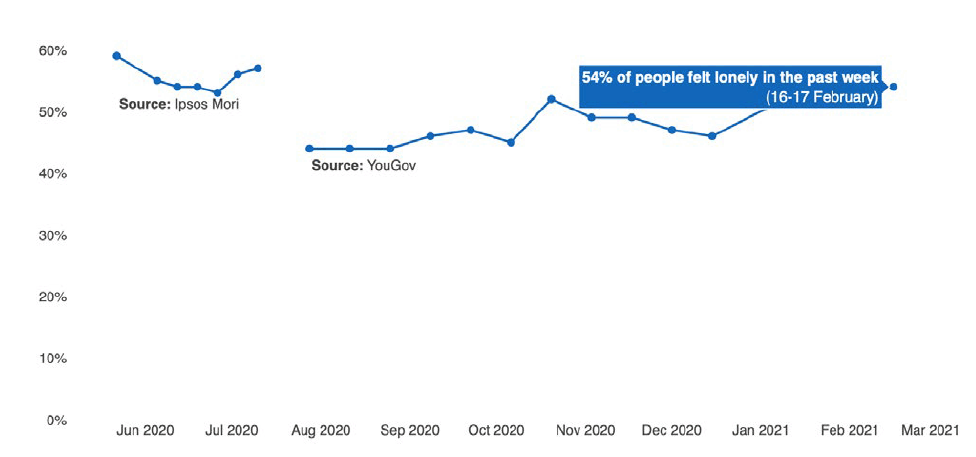
Isolation and loneliness in particular continue to have profound impacts on individuals and communities. Figure 5 shows that a large proportion of our population continue to experience high levels of loneliness, even when restrictions on socialising have been eased slightly.[35] Current levels of loneliness (54%) are substantially higher than the benchmark figure of 21% pre-COVID-19 obtained from the 2018 Scottish Household Survey.[36]
Economic Impacts
COVID-19 and the restrictions needed to contain it have had deeply negative impacts on our economy, fair work and business outcomes. Many people have been made redundant, furloughed or have had their working hours or wages cut. This has resulted in unprecedented levels of financial distress and hardship particularly for those experiencing socio-economic disadvantage. There has been an increased uptake of Scottish Welfare Fund crisis grants and a doubling of the number of people claiming out of work benefits.[37] While these safety nets will be a lifeline for many, we know that the rise in unemployment is likely to have a negative impact on our population's health in the long term.
Inequalities in COVID-19 Impacts
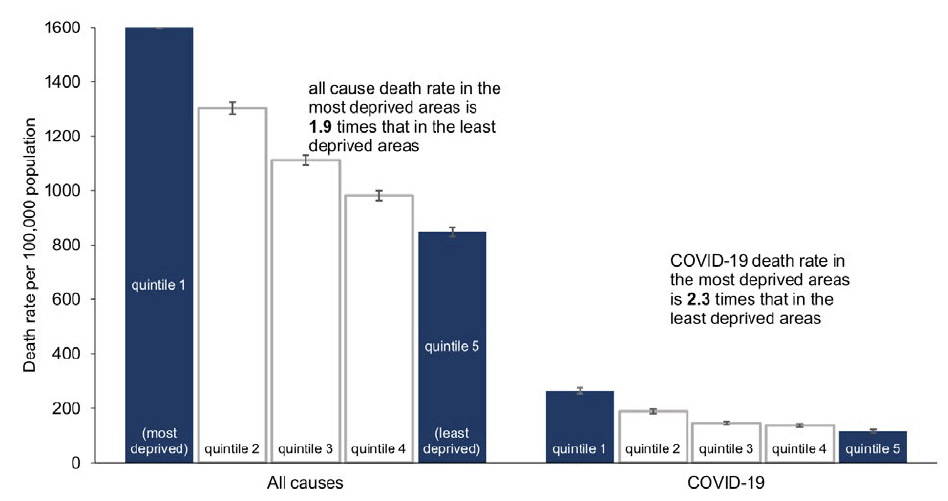
The direct and indirect mortality impact of COVID-19 has not affected all of us equally. The direct impact has been substantially higher for older people, for those with pre-existing medical conditions, and amongst those who are obese.[38] There are also systematic differences in COVID-19 impacts across our population. Those living in the most deprived 20% of areas were on average more than twice as likely to die from COVID-19 than those living in the least deprived 20% of areas. COVID-19 has widened the health inequalities gap even further (Figure 6).[39 ]Among black and minority ethnic groups it has been found that those reporting either South Asian or Chinese ethnicity had substantially higher mortality rates than those reporting White ethnicity, even after adjusting for other factors.[40]
The indirect impacts of COVID-19 and the measures to control it are still emerging. Children, young people and young adults are likely to have been disproportionately impacted by disruption to education and loss of employment in the hospitality sector.[41] Some groups (including people who were shielding, people living alone, and single parents) have experienced more marked social isolation.[41] The economic impacts and associated unemployment, underemployment and income loss have been most profound for people in lower-skilled and lower-paid jobs, and those working in certain sectors such as tourism and hospitality.[41]
Prior to the pandemic, there were already marked inequalities across many domains in our society, including income, wealth, living standards, labour market participation, health, education and life chances (chances of achieving positive outcomes and avoiding negative outcomes throughout the course of our life). Emerging evidence suggests that COVID-19 has exacerbated many pre-existing inequalities and exposed the vulnerability of some of our population to adverse shocks.[41]
Conclusion
The COVID-19 pandemic will have very significant and potentially long-lasting health impacts, arising from both the direct and indirect effects of contracting the illness and the interventions put in place to control spread of the virus.
It is also clear from emerging evidence that the impacts of the COVID-19 pandemic are large and unequal. The negative effects of the pandemic are borne disproportionately by people who already have fewer resources and poorer health. Action is needed, now more than ever, to address the health inequalities that exist in our society. Recovery and renewal of our public services, in the wake of the pandemic, could provide us with an opportunity to have a renewed focus on supporting our most vulnerable and disadvantaged communities.
Successfully reducing the health inequalities that exist in Scotland cannot be achieved by our health and care system alone. Addressing the wide range of issues identified in this chapter will require a significant whole system response. I will explore this further in the chapter on reducing health inequalities, where I set out some of the work that is being led by the Scottish Government, Health Boards and Local Authorities to reduce health inequalities. This is work which will undoubtedly help inform our long-term approach to making Scotland a fairer place to live.
Contact
Email: RealisticMedicine@gov.scot