Chief Medical Officer - annual report: 2020 to 2021
This report is focused around five key themes: the health of the nation, delivering personalised care, reducing health inequalities, sustainability of our workforce, and green and sustainable healthcare.
Green and Sustainable Healthcare
Green and Sustainable Healthcare
The global crisis of climate change is accelerating. As declared by the First Minister in 2019, we are in a climate and ecological emergency. Human activities are driving rapid changes in our climate, biodiversity loss and species extinction, with changes occurring faster than predicted.[117-118 ]If emissions continue to rise at current rates, we will be heading towards a predicted 4°C increase in global temperatures by 2100. It is a temperature thought to be incompatible with organised human society.[119 ]This emergency demands a rapid and comprehensive response, with unprecedented, far-reaching transformation required across our society
The WHO reports that one in nine of total global deaths per year is due to air pollution.[120]
The climate and ecological emergency is also a health emergency, as human health is inextricably linked to the health of our planet and its natural systems.[121] In 2009, The Lancet identified climate change as the biggest global health threat of the 21st century.[122] The threats to health come in the form of direct impacts due to weather, and indirectly through disruption to natural systems and societal systems. (Figure 1).
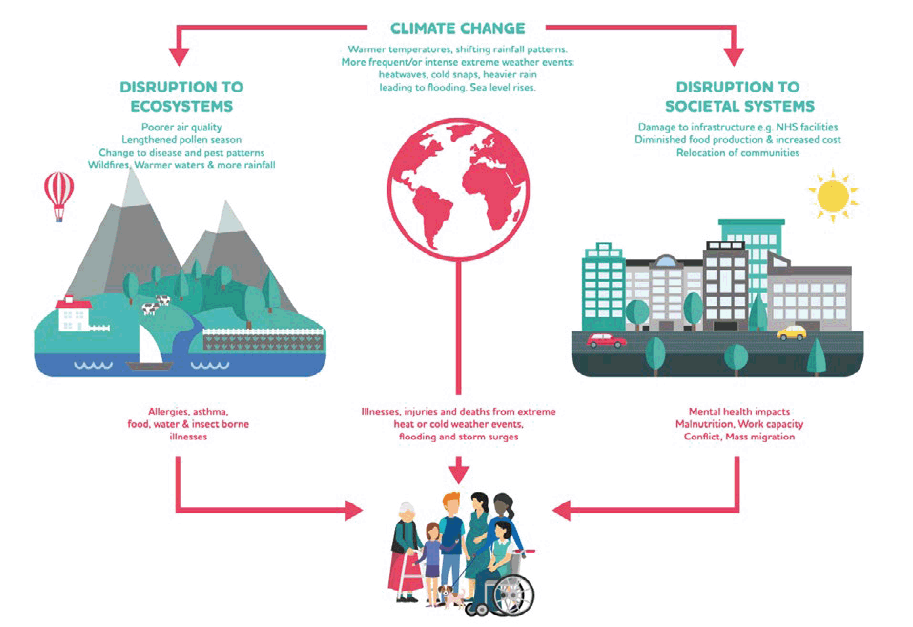
The COVID-19 pandemic is highlighting, yet again, the interconnected nature of our planetary systems, from the zoonotic origins of disease and their relation to our natural environment and food systems, to the greater vulnerability to disease resulting from social inequality, air pollution and other environmental factors.[123 ]
Last March, the whole world adopted varying degrees of curfew and lockdown measures that restricted human mobility. As social, economic, industrial and urbanisation activity decreased, nature took advantage showing dramatic improvements in the quality of our air, cleaner rivers, less noise pollution, undisturbed and calm wildlife.[123-124]
While carbon emissions have fallen dramatically due to lockdowns, this has only marginally slowed the overall rise in C02 concentrations, according to the World Meteorological Organization (WMO).[125 ]The global response to the COVID-19 pandemic, and the resulting decline in emissions in the early part of this year, shows the possibilities in terms of changing human behaviour to have positive impacts on the environment.
In November, Scotland hopes to host the United Nations Climate Change Conference of the Parties (COP26). It is an event of global importance that aims to accelerate action on the climate emergency. It provides a unique opportunity to secure fresh, ambitious and tangible global commitments to tackle the climate crisis and ensure a green recovery from the COVID-19 crisis. I very much hope it will inspire the people of Scotland to consider how we can build a greener future.
A Greener NHS Scotland
If the global health care sector were a country, it would be the fifth-largest greenhouse gas emitter on the planet.[126]
NHS Scotland is a significant contributor to the climate emergency. It emits a large amount of greenhouse gases, consumes huge amounts of resources and produces copious amounts of waste. We have a moral obligation to help tackle the greatest threat to human health, by reducing our impact on the environment. Responsibility rests with us all.
NHS Scotland has committed to being a 'net-zero' greenhouse gas emissions organisation by 2045, at the latest. This will require unprecedented change in how we work.
The following commitments were announced by the Chief Executive of NHS Scotland in June 2019:
1. NHS Scotland will be a 'net-zero' greenhouse gas emissions organisation by 2045 at the latest
2. All NHS Scotland new buildings and major refurbishments will be designed to have net-zero greenhouse emissions from April 2020
3. Each NHS Board should undertake a Climate Change Risk Assessment covering all operational areas and produce a Climate Change Adaptation Plan to ensure resilience of service under changing climate conditions
4. NHS Scotland transport Greenhouse Gas emissions from its owned fleet (small / medium vehicles) will be net-zero by 2025
5. The NHS supply chain will be reviewed to determine the extent of associated greenhouse gas emissions and environmental impacts
6. Each NHS Scotland Board should establish a Climate Change / Sustainability Governance group to oversee their transition to a net-zero emissions service
Our NHS Climate Change and Sustainability Strategy 2020-2025 is being developed with the aim of making NHS Scotland a world-leading sustainable healthcare provider. The new strategy, due to be published in spring, renews our commitment to delivering the UN Sustainable Development Goals, and a green, just and resilient recovery to the challenges of COVID-19.
In addition, a Sustainability Action brand has been developed to promote awareness of sustainability within NHS Scotland (Figure 2). All of us within NHS Scotland can use this brand and the accompanying toolkits to promote sustainability activities.

In Realising Realistic Medicine, we described creating the conditions to achieve the Realistic Medicine vision. The vision that "by 2025 we will demonstrate our professionalism through the approaches, behaviours and attitudes of Realistic Medicine". Achieving Scotland's climate goals and Realistic Medicine fit naturally together. To become a sustainable and greener healthcare provider, we must deliver safe, effective, personalised care, and reduce harm and waste through improvement and innovation. We can ensure that NHS Scotland contributes positively to the sustainability of our planet, by taking responsibility, individually and collectively, to become the stewards of our healthcare resources.
Connect and Collaborate
We cannot overestimate the power of human connection. Our ability to share ideas, spread good practice and innovate, all stem from it. If we value and strengthen our human connections, together we can change the culture of NHS Scotland, to become a greener, more planet friendly organisation.
The Scottish Environmental Anaesthesia Group (SEA-G) is a grassroots group of anaesthetists with 45 members across most acute hospitals in Scotland. They have addressed national meetings and have lobbied for environmental information to be provided from manufacturers at time of procurement. Issues discussed include; theatre waste segregation, ecological choice in drug and product procurement, and a re-appraisal of single-use culture.
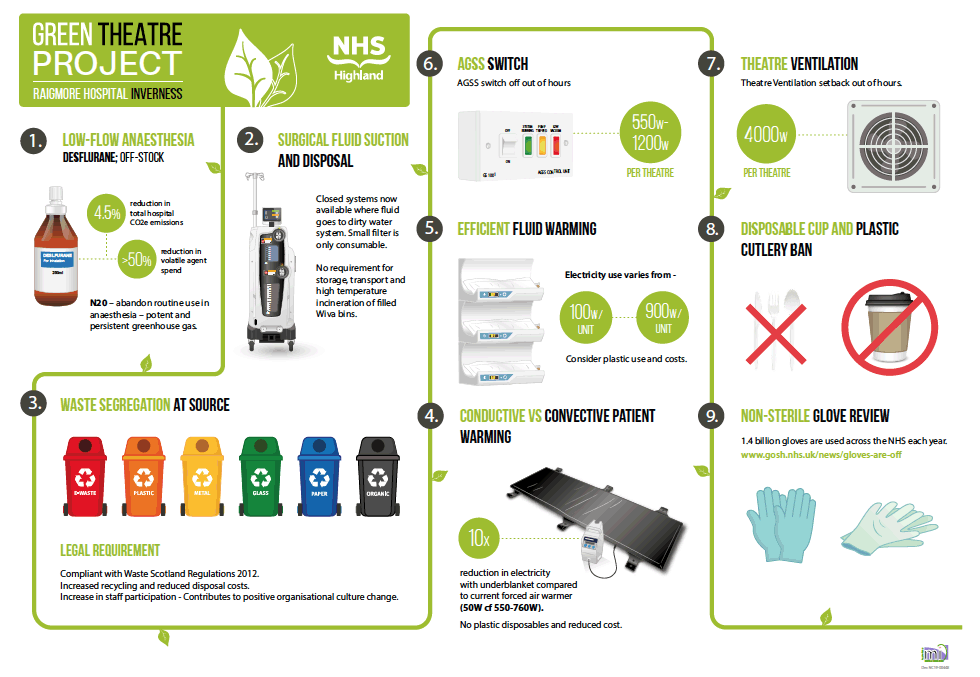
SEA-G have constructed a template for the peri-operative journey called the 'Green Theatre Project'. This initiative resulted in NHS Highland becoming the first health board in the UK to ban Desflurane as an anaesthetic gas at Raigmore Hospital. This has reduced Raigmore's CO2 emissions by 4.5%, with recurring savings of approximately £70,000. All whilst maintaining patient safety and care standards. If we are serious about reducing our carbon footprint, there is much we can learn from the Green Theatre Project (Figure 3).
The Green Theatre Project initially included a ban on disposable cups in the main theatre suite at Raigmore Hospital, where 78,000 disposable cups were being thrown away every year. The ban on single use items and the "gloves are off" campaign, which encourages healthcare professionals to reduce unnecessary use of non-sterile gloves, have been rescinded due to the pandemic. It is important to acknowledge that the COVID-19 pandemic has caused significant changes in the production and generation of single use plastic. While Personal Protective Equipment has played an important role in preventing the spread of COVID-19, the upsurge in demand for these items will challenge our efforts to curb plastic pollution and move towards more sustainable and circular systems. We need to be mindful of how we can mitigate this by focusing on what is within our sphere of influence in our places of work, such as recycling practices and purchasing recyclable and re-usable kit and materials where it is safe to do so.
The climate emergency has wide-ranging causes and impacts that extend far beyond the traditional boundaries of health and care. In order to tackle these issues we must broaden our horizons and collaborate with an increasing number of organisations outside of the health sector.
There is compelling evidence that shows the positive contribution that contact with nature can make to our health and wellbeing.[127] Our health is intimately linked to the sustainability of ecosystems within which we live our lives. Improving access to, and encouraging us to use our natural environments, could play a key role in delivering Scotland's public health priorities.
The "Our Natural Health Service Programme" (ONHS), is led by NatureScot (formerly Scottish Natural Heritage), in partnership with Scottish Forestry, NHS Scotland, Public Health Scotland, and Transport Scotland, and a range of other national and local organisations. It is a programme of work that I am particularly proud to be involved with and connects two important and accessible contributors to our health – physical activity and outdoor green space.
The OHNS NHS Greenspace Demonstration Project has been working with Health Boards to develop the potential of the NHS outdoor estate to deliver better outcomes for health, nature and the climate. The first phase resulted in greenspace improvements across a range of hospital and health centre sites in mainland Scotland. Overall, some 87 hectares of greenspace have been created or improved including 46 hectares of woodland brought back into sustainable management. On-site promotion of greenspace opportunities benefits staff, patients, visitors and the local community.
Through improvements to our greenspaces, we can promote more physical activity at work and improve staff wellbeing. It's an observation reinforced during the COVID-19 pandemic where we have seen staff using workplace greenspace to seek relaxation and solace during stressful times.
Another major element of the ONHS programme are the four Green Health Partnerships (GHPs) established in Lanarkshire, Dundee, North Ayrshire and Highland. Led by Health Boards and Local Authorities, these partnerships are demonstrating ways to increase our use of the natural environment as a health promoting asset.
Delivery of supportive green health projects has been impacted by COVID-19 restrictions, but many GHP projects have been re-purposed and helpful resources developed to communicate key messages about the benefits of contact with nature and to promote more use of local green space. The GHPs have produced 'Keeping Healthy in the Outdoors during COVID' videos, organised walking challenges, and distributed 'Green Health' packs to encourage outdoor exercise and an interest in nature.
Community Growing Initiative, Lanarkshire
This is an example project from Lanarkshire Green Health Partnership and is delivered by the Clydesdale Community Initiatives (CCI) which works with people experiencing severe and enduring mental health issues in the community or hospitals.
Participants are involved in activities such as creating and maintaining garden areas for vegetables and fruits, and planting beds for herbs and flowers at a variety of community greenspaces. They have the opportunity to acquire and develop vocational skills. Group work and peer mentoring is encouraged. Older inpatients with dementia reconnect with nature and experience the joy of seeing gardens grow. Some of the garden produce goes to local food banks to help others in need. This has been particularly welcome during the COVID-19 pandemic. During lockdown, CCI staff continued to provide support by providing tools, materials, and coaching videos to occupational therapists to help them engage patients in gardening activities.
As one member of the hospital staff noted:
"It's amazing to see the difference in Mr X. He just used to sit at the door and had no interaction with anyone. Now he's waiting on us coming with a huge beaming smile, and is sorry when the session ends!"
The Highland Healthcare Professionals for Climate group is a group of healthcare professionals brought together by a shared concern about the environmental crisis, and a recognition of the health benefits of addressing it. Created by GPs, the group has enabled practices across Highland to connect and share environmental action plans to make practices more sustainable.
The group advocate at local and community council level for active health infrastructure. Initiatives have included the cycle scheme 'WheelNess' (bikes provisions to over 220 people with financial or health barriers, developed and delivered by Cycling UK), and Couch to 5K programmes for both staff and the people they care for. They have secured funding for bicycle shelters for all Inverness GP practices, e-bikes that GPs can use for home visits as well as e-bikes for carers. They have also actively contributed to the rolling out of a network of walking, wheeling and cycling infrastructure along priority routes, to help people stay safe on essential journeys.
Quotes from participants of the 'WheelNess' (Widening access to cycling in Inverness) Scheme
"If I’ve done a 12-hour [nursing] shift and I’ve driven there and back, your feet are in absolute agony and your legs are swollen. But if I cycle home, I don’t have sore feet or legs..." "…It’s good for my fitness and for keeping my weight down."
I was spending £40 a week on taxis home from work. Now I use the bike six days a week and do about 35 miles a week. I have saved loads and can afford to buy healthy food for my son.
I would not have been able to provide vital COVID-related services without this loan. I do not drive, and the trike has allowed me to deliver weekly food shops and boxes of crafts for children and disadvantaged households.
The time to build on climate positive changes brought about by the COVID-19 pandemic is now. What can we do within our own spheres of influence to adopt and encourage greener practice and behaviours?
Communicate
Fostering a Culture of Stewardship for Greener, Sustainable Healthcare
To create a culture of stewardship - where we are mindful of the resources we use and share a vision of green and sustainable healthcare - we must ensure that future members of our health and care system feel engaged and empowered to move towards our goal. The GMC requires that:
"Newly qualified doctors must be able to apply the principles, methods and knowledge of population health and the improvement of health and sustainable health care to medical practice."[128]
It is evident that medical training must foster a culture of stewardship and evolve to teach our future doctors the principles of both planetary health, and sustainable healthcare. Our future clinicians must not only apply this knowledge as part of their everyday practice - green prescribing, promoting healthy, low carbon behaviours, shaping sustainable healthcare systems - but also use their position as trusted members of our society to influence the behaviours of their colleagues, as well as the people they care for.
The University of Dundee and NHS Tayside have worked towards embedding Planetary Health and Sustainable Healthcare into the core undergraduate medical curriculum. The university delivers modules, workshops, and student selected components that introduce students to the over-arching, recurrent themes of environmental sustainability and sustainable healthcare. The aim is to provide graduates with the knowledge and skills required to promote and support healthy, low carbon behaviours in the people they care for, shape sustainable healthcare systems and use their positions as trusted members of our society to influence wider environmental policy.
Personalised Approach to Care/Shared Decision making
We tend to choose less treatment, or more conservative treatment, when all the risks and benefits of various treatment options are fully explained to us. When there has not been a full discussion of our preferences, or what truly matters to us has not been elicited, we are less likely to comply with a prescription, and more likely to regret a procedure, increasing harm and waste. As waiting lists grow and access to conventional medical and surgical therapies are restricted for public health reasons, the need for personalised and value-based care is stronger than ever. A renewed focus on lifestyle changes, and a move away from traditional medical models of care, will undoubtedly be more beneficial for many of the people we care for and for our health and care system.
Reducing Harm and Waste
"A central theme of Realistic Medicine has been to engage clinicians in efforts to become stewards of NHS resources by helping them understand that it is their decisions that commit resources."
Sir Muir Gray
Sir Muir Gray is Director of the Value-based Healthcare Programme at Oxford University, and an internationally renowned authority on healthcare systems. He states that a major factor that affects the sustainability of our NHS is the relentless increase in volume and intensity of our clinical practice. He reminds us that in recent years, the NHS in the UK has experienced growth of around 4.5% per annum and that the majority of it has been generated by increases in the volume of clinical activity and innovation. A relatively small amount is due to the more complex needs of our ageing population.[129]
The Organisation for Economic Co-operation and Development estimates that up to one fifth of healthcare spending across member countries, which includes the UK, is wasted.[130 ]The question we must ask ourselves is whether we have gone beyond what Sir Muir calls the 'point of optimality' – the point of delivering the best balance of benefit-to-harm for the populations we serve.
We know that all healthcare has potential to cause harm - exposure to radiation from imaging, risks from procedures, and side effects from medication. Over investigation and overtreatment may not only cause harm to the people we care for, but they also waste our precious healthcare resources, consume our natural resources and contribute to environmental degradation.
The prescription of a medicine is the most common intervention in healthcare, but do we consider how prescribing impacts on our environment? 30-100% of every oral dose of a medicine is excreted unchanged, or as metabolites and enters our wastewater system. Wastewater treatment plants cannot completely remove medicines, and there is evidence of over 600 pharmaceuticals in our water systems.[131] While no clear link has been established between pharmaceuticals in the environment and direct impacts on human health, there is evidence that they can harm aquatic life, enter our food chains and lead to an increase in antimicrobial resistance.[131-132]
So what can we do? We can ensure appropriate prescribing of pharmaceutical products, have shared decision-making conversations to ensure compliance, and put systems in place in order to encourage the people we care for to order the precise amount of medicine they need. We can also encourage them to take unused, unwanted or out of date medicines to community pharmacies for appropriate disposal. These are means by which we can help reduce pharmaceutical waste and pollution.
The One Health Breakthrough Partnership (OHBP)
The One Health Breakthrough Partnership is a unique collaboration which was founded by NHS Highland, The Highlands and Island Enterprise, Scottish Water, Scottish Environment Protection Agency and The University of Highlands and Islands. Partners now include; Forrit, The James Hutton Institute, Talking Medicines, Glasgow Caledonian University, University of Strathclyde and The University of Edinburgh.
These organisations have come together to tackle pharmaceuticals in the environment with a vision for a non-toxic, sustainable environment. The partnership approach recognises that no single organisation can deliver this vision on its own. All partners have agreed to share knowledge and an initial programme of work is already underway.
NHS Highland worked with the OHBP to look at ways in which Caithness General Hospital can reduce water pollution caused by medicines, and was awarded certification to the Alliance for Water Stewardship (AWS) Standard in November 2019. Caithness General is the first hospital in the world to receive AWS Standard certification for its work to reduce the impact of pharmaceuticals on the environment.
The OHBP won an award at the 2020 Scottish Environment Business Awards. The Partnership was also "highly commended" and awarded runner up at the 2020 BMJ Healthcare Awards in the Environmental Sustainability and Climate Action category.
Become Improvers and Innovators
During this pandemic, there have been unprecedented advances in telemedicine across NHS Scotland, led by the Scottish Government's Technology Enabled Care Programme. The following case studies explore innovations that have the potential to have a significant impact on the carbon footprint of NHS Scotland.
Reducing Patient Travel Miles
Near Me
As mentioned earlier in the report, Near Me is a video consulting service that enables people to attend appointments from wherever convenient. At the start of the pandemic a rapid scale up plan was introduced to accelerate the use of Near Me across Scotland. There are currently around 20,000 Near Me consultations per week. This represents an estimated travel saving of over 28 million miles per annum. In the recently completed public consultation, where views on the benefits of video consultations were sought, environmental benefit scored highly among the general public.
Scale Up BP
Over 1.2 million GP appointments are taken up each year solely for checking blood pressure (BP). Many of these involve journeys by car or public transport. Scale-Up BP is a telemonitoring service for patients which allows them to check their BP in their own home and send this to their practice by text or internet. The GP sees a summary of these results and can contact people by video, phone, text or email to discuss results, and advise them on any therapy changes. In a large study in Lothian, patients using telemonitoring had 25% fewer face-to-face contacts than in the previous year. A significantly bigger reduction than in a closely matched comparator group who did not use telemonitoring. Over 15,000 people have now used Scale Up BP with an increase in uptake during the pandemic.
Measuring healthcare practices and outcomes against not only economic, but also environmental and social costs, gives us a better idea of sustainable value in quality improvement.[133 ]Incorporating environmental and social impacts into our clinical practices gives a more holistic view of the healthcare we provide, and can help us become a more sustainable healthcare system. This approach allows us to identify unique opportunities for improvement which might otherwise be missed, and helps ensure that improvements are sustainable in the widest sense.[133]
The following thought provoking case study encourages us to think about the impact of our clinical practices on the environment.
Environmental Impact of Inhalers[134]
Inhaler devices are the primary treatment for patients with asthma and COPD and are extensively prescribed. The options are a dry powder inhaler (DPI), which delivers a fixed dose of medication in a dry powder form, or a metered dose inhaler (MDI) which delivers the medication as an aerosol. Originally the propellants used in MDIs were chlorofluorocarbons (CFCs), but in response to concerns about CFCs causing stratospheric ozone loss, they have been replaced by hydrofluroalkane (HFA) propellants.
Unfortunately HFAs are potent greenhouse gases. Although less potent than CFCs, the global warming potential (GWP) of one of the common HFAs is more than thousand times more potent than carbon dioxide. The consequence of this is that MDIs have a substantial adverse environmental impact.
To illustrate this, a Ventolin (salbutamol) MDI has an estimated carbon footprint equivalent per dose to driving about a mile in a small car. Over a year this would be equivalent to 205KgCO2e, in comparison with 9.5KgCO2e for the Ventolin Accuhaler, which is a DPI. It is estimated that approximately 4% of the carbon footprint of the NHS results from the use of MDI inhalers.
All of the classes of inhaled medicines that are used are available in a DPI form, and from an environmental perspective it would be prudent to change prescribing practices towards using DPIs in comparison to MDIs. Prescribing practices are influenced by habit and tradition, and how familiar a clinician is with the alternative. The choice of inhaler device for a patient is also determined by the ability of the patient to use the device, price and preference. In 2017, 13% of inhalers in use in Sweden were MDIs, in comparison to 70% in the UK. This disparity can only really be explained by the non-clinical factors described above.
Although some DPIs are more expensive than MDIs, this is not always the case, and many inhaled medications are relatively cheap. For many patients DPIs may be more effective, as many individuals struggle to use MDIs. There is therefore important work to be done to change prescribing practice to reduce the environmental impact of inhaled medication.
Conclusion - Advocates for change
The time for sustainability by stealth and seeing it as a 'nice thing to do' or 'someone else's job' has passed. Improving population health and wellbeing is inextricably linked to action to tackle climate change.
There are many challenges. For example, although sustainability initiatives often reduce costs, how do we prioritise investment in stretched services? How do we balance essential infection control with the need to reduce waste in both packaging and single use products? The challenges may seem insurmountable, but I hope the case studies in this chapter have inspired you to explore how you and your organisations can deliver green and sustainable healthcare.
While the pandemic is not a solution for climate change, it can be an historic turning point in tackling the global climate crisis. We must learn from it and make significant advances to deliver the fairer, greener, more prosperous Scotland we all want to see. We all have a key part to play in this. Can we, through the principles of Realistic Medicine, practise sustainable and greener healthcare?
Considerations
- What can we do within our sphere of influence to practice greener and more sustainable healthcare?
- As we aim towards a culture of stewardship, how can we become more mindful of the NHS resources we use and use them more wisely?
- Consider how you can influence and empower your colleagues and the people you care for to practice climate positive behaviours that can have a positive impact on their physical and mental health.
Contact
Email: RealisticMedicine@gov.scot