Chief Medical Officer's Annual Report 2014-15
The Chief Medical Officer Annual Report 2014 -2015 explores the challenges that face doctors today.
Chapter 5 Changing Our Practice to Support Improvement
Scotland's medical staff, working with colleagues in health and social care, continue to be at the forefront of the wide range of improvements in the safety, effectiveness and quality of care and treatment that are being made within our National Health Service. Hundreds of doctors across the country have fulfilled a range of vital roles in making the changes and testing ideas on how to ensure that everyone in Scotland receives the highest quality of care possible - leading teams, encouraging junior medical staff to test their improvement ideas and emphasising the importance of time for learning and reflection amidst the demands of clinical practice.
Improvements in the quality of care are often dependent upon having the right conditions in place - positive relationships with colleagues, a learning culture and an understanding of tried and tested ways of implementing change in complex systems.
For several years, doctors have been the driving force behind quality monitoring work such as the Scottish Intensive Care Society Audit Group system - a system that is now being used to inform and design ways that routine data like these can be used to design routine quality monitoring and improvement systems across the country. Data are very powerful and important influencers. Surgeons and other clinicians have participated in the thousands of surgical safety "pauses" that take place across the country every week - collectively contributing to reductions in surgical mortality.
Through the Scottish Patient Safety Programme doctors of all grades and a wide range of specialties have changed the way they think about practice in respect of sepsis - more people than ever before are receiving timely antibiotics when sepsis is suspected, undoubtedly contributing to the 20% reductions in mortality from sepsis that have been observed. These improvements have been made possible through the engagement and enthusiasm of clinicians who have been willing to review the harms occurring within their teams and systems, consider learning from colleagues and then test ways of implementing this within their teams for every person that receives care from them in the future. It is this complete focus on design and the reliable delivery of care processes that has been at the heart of the significant improvements in quality and safety across the country.
The emphasis on using data to support discussions and learning in clinical teams, already an established approach within general medical practice, has been seen most strongly this past year through the work on measuring the safety culture of almost 950 general practices. Data that can be used for GPs and their practice colleagues for reflection, learning and consideration of how team-working can support improvements in the safety and quality of care.
The importance of taking time to talk with other members of the team about the quality, safety and flow of people through healthcare systems has been reflected in the safety huddles that are now taking place - as well as through the advice given to directors and senior managers by medical staff as part of the leadership walkrounds.
Doctors who are supported to engage with broader organisational perspectives and have opportunities to discuss issues and problems within their work are likely to find it easier to identify and implement quality improvements. A team culture focused on valuing doctors and providing support is essential and something that every member of the medical profession has a responsibility to nurture.
The literature that shows a relationship between organisational performance and the quality of clinical leadership emphasises the importance of ensuring that the work of doctors is aligned to strategic priorities and organisational goals. This is just as much the responsibility of doctors as their colleagues working in management. This will in turn influence and shape organisational culture and build positive working relationships with the wider team.
Doctors working on improvements need to be clear what the aim of the work is and be clear that they have the knowledge and skills to deliver this.
Medical staff meeting with patients and families where they have concerns or have been dissatisfied with the quality of care is an essential component of a learning culture - and must continue to be a prominent element of our approach to feedback and complaints. Clinicians can significantly influence the approach taken within teams - building on relationships with patients, their families and carers and taking early action when it is becoming clear that someone has cause for concern or complaint.
A recent article in the Harvard Business Review by Giona and Staats, focused on the reasons that organisations don't learn, has some useful insights that can be applied to the way we approach quality and systems improvement. They suggest that deeply ingrained human tendencies can interfere with strategic aspirations to become a learning organisation.
There is greater recognition that medical staff are not immune from the human factors that impinge upon performance, but there can still sometimes be a tendency to forget that doctors have the same fears as everyone else and that sometimes behaviours need to be more supportive of learning, reflection and change. A growth mindset has been shown to be important - emphasising a recognition of the potential that exists for continuous learning and improvement, not taking the view that the capacity for change and learning is fixed by some genetic predetermination.
We must all demonstrate through our actions that we are committed to ensuring that everyone has the opportunity to grow through challenge and opportunity for continuous learning. Clinical leaders need to challenge their own thinking and ask themselves whether they have a growth mindset. This will mean an enhanced awareness of opportunity for self improvement, more engagement with complexity and a greater persistence in the face of obstacles.
Time for reflection and personal commitment to "pause before action" can be very difficult for clinicians. However, reactive modes with no time for reflection are energy depleting and ultimately ineffective. Although it can be counter-intuitive to think that taking more breaks increases productivity, there is compelling evidence that achieving a balance of more frequent breaks and restoration leads to greater productivity. These are important areas that can contribute to feelings of personal control and mastery in the workplace - both of which can protect against burnout.
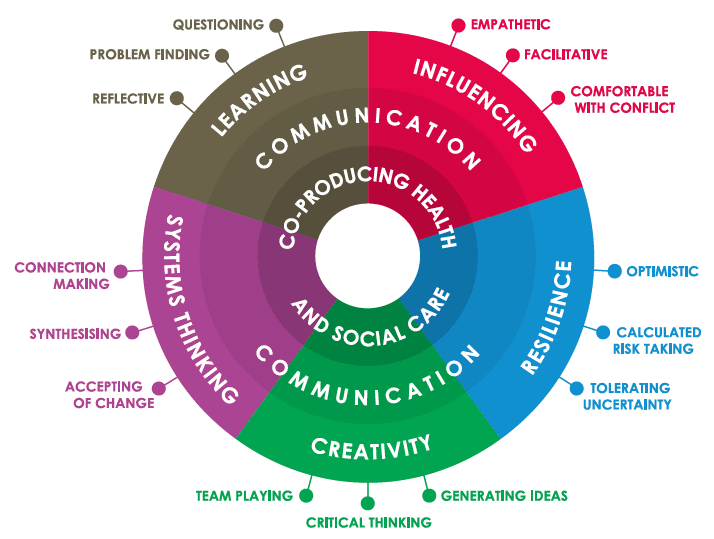
Figure 3: From Lucas, B & Nacer, H. (2015). The habits of an improver. Thinking about learning for improvement in healthcare. London: The Health Foundation. P.8.
Junior medical staff have reported that they often have ideas on how improvements might be made, though have little opportunity to implement them. This is changing as NHS Boards have enhanced their understanding and capacity of how to support a more widespread emphasis on quality improvement capacity and capability. It is increasingly being recognised that the development of a range of improvement science skills, although necessary is unlikely to be sufficient to create the sort of widespread learning culture we want to see in Scotland.
The Health Foundation recognise the importance of reflection, communication and collaboration as the basis for the development of "habits" that will help shape future activity. Their recent paper on this issue states that "The science of improvement and the art, craft and practices of improving quality require us all to change our habits." It has been suggested that these habits should be the primary outcomes of all learning activities, and that conversations about learning for improvement capability can be helpfully framed through the lens of five desirable improvement habits - learning, influencing, resilience, creativity and systems thinking. Each of these have "sub-habits" defined and outlined. They are habits that we could all benefit from reviewing - identifying the ones we have already acquired, considering how they might be best applied within our work and deciding how we might begin to develop new habits to support our collective work on quality and systems improvement. Communication is central to all improvement habits and sub-habits. (see Figure 3.)
Conclusion
Scotland's medical staff have been at the forefront of identifying, testing and implementing changes that have seen world-leading changes in the safety of care and treatment within NHSScotland. Quality monitoring systems have demonstrated the ways in which data collected at the point of care can be used to identify test of change, to make connections and prompt questions in support of improvement. Resilience in the face of rising demand, critical thinking and challenge of the status quo have been valued across multi-disciplinary teams. Medical staff lead and participate in hundreds of empathetic and facilitative conversations with patients, families and colleagues. The habits of improvement are in action across hospitals, clinics and care settings every day. The medical profession in Scotland is in a strong position to lead and contribute to the challenges of delivering safe, effective and person-centred care in the future. There is still much to do though - not everyone has developed the habits of improvement; and some may have habits that don't positively contribute to the learning and improvement culture that is vital to an engaged workforce and continuous improvements in quality.
What habits would you like to cultivate to develop, sustain and spread a learning and improvement culture across the country?

Contact
Email: Diane Dempster