Chief Medical Officer's Annual Report 2014-15
The Chief Medical Officer Annual Report 2014 -2015 explores the challenges that face doctors today.
Chapter 2 Realism in Healthcare
This chapter outlines the various concerns that have arisen with regard to modern medicine over the last five to 10 years and how clinicians might address these issues. At its heart, the concern has been that in striving to provide relief from disability, illness and death, modern medicine may have overreached itself and is now causing hidden harm - or at best providing some care that is of lesser value. But the problem has gone beyond that into what may not really be considered illness, to the medicalisation of common life experiences.
Jacob Bigelow, Professor of Surgery in Harvard until his death in 1890, was famous for a number of reasons. He wrote and disseminated information about the first uses of inhalational anaesthesia in the United States, encouraging its spread. Less famously, he also wrote "the amount of death and disease suffered by mankind would have been less if all disease were left to itself". For much of history, his view was largely accurate: for centuries doctors had treated seriously ill people with purges, with bleeding, with leeches and with poultices of doubtful sterility. Despite the direct experience suggesting that the treatments offered no value, society had sought out treatment and advice from doctors driven more by hope than experience and struggling to accept the inevitable limitations of our short lives.
From around the beginning of the twentieth century, science gradually and incrementally discovered more of the biochemical and physiological aspects of disease and treatment, gradually more and more treatments were developed. In the United Kingdom a very significant advance was made by Dr Austin Belford-Hill, who pioneered the use of Randomised Controlled Trials (RCTs) in his work on streptomycin in the treatment of tuberculosis. This was the first example of applying rigorous and repeatable experimentation to establish the effectiveness of treatment. It was followed by an increase in proliferation of RCTs which helped establish the effectiveness of many treatments in use today, as well as dismissing a great number to history. The dawning of the age of evidence based medicine followed with considerable energy devoted to standardising healthcare based on evidence derived from these trials. It is easy to understand this progress and to assume that all treatment now offered is likely to be effective and unlikely to cause much harm. Unfortunately, this is not universally the case. This chapter will lay out the reasons why we should continue to remain curious about the overall effectiveness of modern medicine and why we should re-calibrate our approach to medicine in many settings.
It has been argued that evidence-based guidelines developed for people with single diseases should not necessarily be extrapolated to the management of patients with multiple conditions, given the possibility that this may result in over-treatment and over-complex medication regimes. This is a common problem for patients as our population becomes increasingly elderly and accumulates ever more long-term chronic conditions. This is not to suggest that guidelines for single conditions should not be used, because currently we have little evidence for what should replace them. There is, however, a need to balance this with the risks inherent in the resulting complex treatment regimens where less appropriate polypharmacy itself may cause harm and hospital admission.
However, doctors need support in choosing, with their patients, not to apply evidence based guidelines: the strength of guidelines can make doctors feel unable to deviate from them, driven by feelings of peer pressure, assumed patient demand, concern about litigation and an understandable, emotional need to "do something" in the face of long-term conditions.
Since 2004 the GP contract has introduced a Quality and Outcomes Framework, incentivised by performance related pay, encouraging doctors to use evidence based guidelines, mostly developed for people with single diseases to treat patients who very often have multiple conditions. This has coincided with an aging population and older patients who have accumulated multiple, long term conditions. The widespread use of guidelines has contributed to the massively increasing volume of medication taken by the population each year. Twenty per cent of the adult population in Scotland is taking more than five medications every day. With the increasing complexity of multiple drug regimes come the inevitable loss of uptake, increased potential for interactions and side effects, and a significant increase in the risk of unintended harm, such as falls, confusion and hospital admission.
There is evidence that doctors tend to underestimate the frequency and impact of side effects from treatment and fail to understand the total "treatment burden" that may be forced upon patients. This may involve complex medication regimes, multiple side effects (for which other medications may be required) and specialist and generalist follow-up appointments. It is argued that it will be in the better interests of patients for intelligent, patient-centred use of evidence-based guidelines, a reduction of over-literal interpretation of evidence, and support for doctors who provide a skilled and generalist view using their clinical judgement to advise patients and then make shared decisions on realistic goals and treatment options.
While evidence-based guidelines will continue to inform the management of people with complex, interrelated conditions, we must acknowledge that a focus on biochemical and physiological outcomes alone may frequently fail to support people to achieve their own realistic and holistic goals; asking "What matters to you?" becomes one of the fundamental questions underpinning the discussion with patients.
In 2012, the King's Fund produced a challenging paper entitled "Patient's Preferences Matter". This collated a great number of studies that showed across a wide range of specialties and settings that:
1. Doctors often fail to take into consideration patient preferences in suggesting and providing treatment. Treatment that does not coincide with the patient's preferences may ultimately be wasteful (in that it doesn't provide value for them). This can be seen in the use of heroic, complex and uncomfortable treatments as a patient approaches the end of life. It also appears to be demonstrable in many more settings.
2. Patients tend to choose less treatment when they are provided with greater detail of the impact, potential benefits and harms of a proposed intervention.
3. Doctors generally choose less treatment for themselves than they provide for their patients.
4. Despite our beliefs that treatment is based on evidence, the complexity of presentations possible means that 30-45% of care is not based on available evidence - partially a reflection of gaps in available evidence, and partially a reflection of the impossibility for clinicians in keeping up with the increasing volumes of guidance.
These conclusions are followed by discussion of variation in treatment and investigation rates: it is well known there is considerable variation between geographical areas that is not related to measurable patient need - and the strong suggestion from the paper is that the supply of treatments is determined by variation in doctors views far more than any differences in disease prevalence, or patient preferences in different populations. This observation - mirrored in the "NHS Atlas of Healthcare" produced by the NHS in England - suggests that a proportion of medical care may be prompted by "supplier induced demand"; healthcare that is provided in excess of patient/population potential to benefit, that is driven by a range of factors including legitimately held medical views, pressures from the manufacturers of medicines or equipment, perceived risk of litigation, and patient expectation in populations where treatment levels are high.
There has been an increasing trend to treat or intervene to address risk (rather than symptomatic illness). This can greatly improve outcomes - as seen in careful management of diabetes in pregnancy - but it can also result in large numbers of the population taking medicines, or undergoing screening, when they would never themselves have developed the condition in question. Increased use of medical approaches to reduce risk may result in less implementation of strategies for lifestyle changes, or treatment being provided to older patients who will not live long enough to derive the potential benefits, and, of course, will cause direct harm in a small number of cases - as well as producing the psychological adjustments that occur when a patient is labelled as having a disease. While the reduction in heart disease rates can be attributed to the use of primary prevention with statins, and better control of hypertension and diabetes, trends show that the fall in heart disease rates pre-dated widespread use of these treatments, and has continued at the same rate as before. One explanation may be that the majority of the decrease has come about from the improvement of lifestyles and environment.
In an era when we have constrained resources, this overuse of medical interventions is of serious concern: It is certain that it co-exists with undertreatment of patients who might benefit, and the intensity with which modern medicine can consume resources, may mean that society is less able to progress improvements in poverty, education, housing and environmental factors that may more simply (and with less side effects) produce significant benefits in both life experience and the incidence of diseases.
Possibly of greater concern is the issue of "heroic" medicine when we are faced with the likelihood of death. A study in the United States asked relatives to assess the quality of death that had been experienced by their relatives. Using matched data it was possible to calculate the cost of treatment in the last six months of that patient's life. The results showed that there was an inverse correlation between the quality experience of death and the resources used. What does this suggest? Overall there is a thread that the intensity of treatment did not result in better outcomes, and reduced the quality of some lives of the patients who were dying.
This should not prompt a trend towards therapeutic nihilism - but suggests that much greater consideration needs to be given to recognising the progression of disease to a point where death is inevitable, and greater care taken to communicate effectively to patients and their relatives in order to help them make appropriate choices. While it is easy to assume that patients and relatives will cling to treatments that may prolong life, and easier still to avoid the emotionally challenging acknowledgement of the ultimate futility of treatment in the face of advanced disease, we owe it to our patients to give honest assessments of prognosis, and clearer descriptions of the likelihood of benefit from treatments that will often be invasive, unpleasant, toxic and occasionally cause death.
Figure 1: From Early Palliative Care for Patients with Metastatic Non-Small Cell Lung Cancer. New England Journal of Medicine.
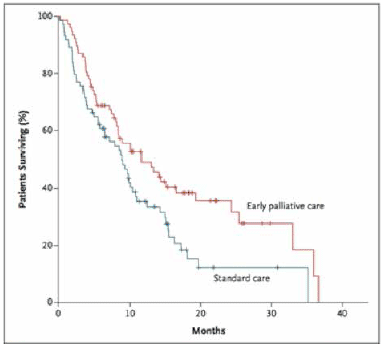
Atul Gawande spoke passionately of this issue in the 2015 Reith Lectures, and in his book "Being Mortal": He describes a study in patients with stage 4 lung cancer: half were given conventional chemotherapy, and comparable patients were assigned to a hospice at home programme, which focus strongly on symptom control, and achieving patient-focused goals that related to social interactions and enjoyment of life. Survival in the group treated with hospice at home care was better than those given conventional treatment - and it is certain that their experience of the last few months of life was more rewarding, and, more under their control. Atul Gawande powerfully speaks of the importance of asking the simple - but emotionally difficult - questions of "What do you understand about your illness at the moment?", "What matters most to you thinking about the future?" and "What would good look like?". He shows that an integrity and honesty in initiating these conversations, and ensuring that the patient has both the time and confidence to make their own fully informed decisions, results in a better experience of the remaining time, and less regret for patients and their relatives. It doesn't mean that no patients choose aggressive treatment - but it does allow patients to feel in control, and to allow an honesty of communication that acknowledges the approach of death, and the emergence of the priorities that mean most to the patient. Many doctors are adept at pursuing this approach, but many are not: we as clinicians have a duty to ensure that we are able to acknowledge our powerlessness at times, and ensure that a difficulty on our part in accepting the inevitable does not reduce the patient's experience of death.

For further information visit www.prudenthealthcare.wales
This section has highlighted some of the important emerging challenges to modern medicine. What action, if any, should we as clinicians take? Perhaps we should follow the example of the "Prudent Healthcare" movement in Wales - an initiative to ensure that healthcare that focuses on true value to the patient is delivered. Waste in healthcare should be assessed not in terms of what might be thrown away, but in interventions that don't add value for patients. Ultimately, this is a topic for a widespread debate amongst clinicians and the population which we serve, but the outcomes might be:
- More research to establish the additional benefits of medicines in the older patient, especially those who are already on multiple medications.
- Increased attempts to support individual and population lifestyle changes, avoiding a rush to intervene where a lesser intervention might suffice.
- Understanding that treatment of risk must be carefully thought through. Aiming to treat with a probability of benefit should be more prevalent than treating with a possibility of benefit.
- Standardising process where appropriate to get the best results, but allowing variation where this is a result of patients expressing their preferences.
- Clinicians should expect to be questioned if their practice varies from others, and be prepared to offer justification for the variation.
- Above all, we must continue to involve patients more and more in their treatment, understanding that they must be fully informed on their illness and prognosis, and the risks and benefits of their possible managements.
The National Clinical Strategy will be published later this year and will provide a guide to further address these complex issues. The "Creating a Healthier Scotland" national conversation started in August 2015 and will be continuing this year. This engagement with the people of Scotland over the future of our health and social care services will be instrumental in shaping care.
This is a difficult subject. We have moved far from Bigelow's assertion that overall clinicians would be better not to have intervened, but we must remain alert to the possibility that we may be over-treating patients to their detriment. Experience shows that this may be best achieved by honest, open and full discussion with patients.


Contact
Email: Diane Dempster