Chief Medical Officer's Annual Report 2014-15
The Chief Medical Officer Annual Report 2014 -2015 explores the challenges that face doctors today.
Chapter 3 Sharing Decision-making and Informing Consent: People and Professionals Combining their Expertise
This chapter examines the future challenge in healthcare of helping people and professionals to be more involved in developing shared or partnership decisions. It explains the need to leave behind the outdated "doctor knows best" culture to one where both parties can combine their expertise and be more comfortable in sharing the power and responsibility of decision-making. It requires system and organisational change to promote the required attitudes, roles and skills. We highlight examples of policy and practice in Scotland that are supporting this change.
Time for Change?
On 1 October 1999 in Bellshill Hospital, Lanarkshire, Nadine Montgomery gave birth to a baby boy who subsequently developed severe disabilities. This was due to a traumatic vaginal delivery as a result of shoulder dystocia. In March of this year, the Supreme Court, in a landmark ruling, awarded substantial damages to Mrs Montgomery and her son. The case was unique in that the medical decision-making and management of her obstetrician was not inappropriate or negligent. The basis of the claim was that Mrs Montgomery had not been fully informed and involved in that decision-making. Had she been so, she argued, she would have stated a strong preference to have her baby delivered by caesarean section.
With the volume and complexity of information we are increasingly asked to consider, shared decision-making represents huge challenges for all of us. When we account for the time constraints that professionals and their patients have together, it is no surprise we have evolved a system and culture which favours "doctor knows best" or medical paternalism. Here the balance of decision-making power within the professional patient relationship is shifted more heavily onto the clinician to decide in the best interest of the individual. Meanwhile people often happily cede control and entrust themselves into the hands of their professionals.
However, the Montgomery ruling now sets a legal precedent that this "parental" approach is insufficient and there is an imperative for a system and values change that rebalances decision-making power, where the expertise of professionals is valued equally to the expertise that people have about themselves. This shift can be challenging for both people and their professionals.
This imbalance in the relationship can be seen most markedly in the parts of our society where need is often greatest, particularly patients living with the highest degrees of socio-economic deprivation, leading to the perpetuation of health inequalities. Empowering these patients may be our greatest challenge, as they have traditionally often not engaged with the care service until further on in their illness journey. They can often be less confident and articulate when it does come to expressing their needs.
This contrasts with patients who are prepared to engage early with care services in order to ensure that their health needs are met. On occasion this can generate what is effectively more demand than need and further contribute to health inequalities. The "worried well" consuming resources while the "unworried unwell" do not come forward.
The Montgomery case took place 16 years ago and we could argue that the system has moved on. However, there are numerous examples of referrals to the Scottish Public Services Ombudsman (SPSO) and medico-legal process when individuals have had insufficient information, communication or understanding.
Studies have also indicated a significant proportion of people wish to be more involved in decisions about their care than they are currently allowed to be. These show that when people are more involved in decisions, they are more likely to adhere to treatment, less likely to suffer the consequences of over-investigation and over-treatment and be more satisfied with their outcomes and relationship with their professionals. Doctors often recommend end of life treatments and interventions that they would reject for themselves. This implies a lot of decision-making is based on unclarified assumptions and expectations.
Informed Consent
The goal of shared decision-making is to reach an agreed decision or state of mutual consent. A literal definition of consent, "feeling with", is derived from the Latin Con - with and Sensere -to feel. It is where each party feels the others' acceptance and agreement to participate. The Consent Form represents a legally signed record of that agreement and is required for most interventions and procedures.
Obtaining consent before a procedure is commonly a professional-centred process done by practitioners to patients. In the time limited setting of busy clinical practice it can be a rushed responsibility of the most junior staff member, just before the procedure, when the individual is not at their most empowered. Obtaining a signature of informed consent is insufficient as it is not an endorsement that an individual may have received enough information or that it has been heard and understood. It provides no clarification that true shared decision-making has been achieved. Indeed evidence suggests that oral and printed communication is often of a complexity that exceeds people's reading skills (functional literacy) and ability to make sense of it (health literacy). People often hide their lack of understanding and clinicians frequently overestimate people's abilities. As George Bernard-Shaw famously stated:
"The single biggest problem with communication is the illusion that it has taken place."
Furthermore, shared decision-making is not a one-way transmission of information about options and risks from the professional to their patient. It is a two-way relational process of helping people to reflect on, and express, their preferences based on their unique circumstances, expectations, beliefs and values. This can be a challenging communication process and individuals will equally need reassurance that their professional has understood them. Finally, and crucially, people need help to evaluate the medical options in the light of their preferences in order for both parties to agree on the best course of action.
There is a caveat in that people vary to the extent they wish to be involved in making decisions. Certainly it can only really take place when people have full decision-making capacity which might not apply for people with cognitive, learning or severe mental health difficulties. Similarly in emergency situations, where fear, pain and distress exist, professionals need to reach an agreement as to the extent their individual patient is willing and able to collaborate in decision-making. Many may be put off by low health literacy (poor understanding, confidence, knowledge and skills) which should be addressed by offering more time and support.
Because of the limitations of traditional informed consent procedures, some have advocated moving to a more person centred process of "request for treatment". This requires the person to record, in their own words, why they want a particular treatment, what they expect it to achieve and what their understanding is of the risks and limitations. It promotes the notion that decisions should be informed and considered before people request treatment. It highlights any lack of decision-making competency, unrealistic expectations or misunderstanding that needs to be addressed. The practitioner can then be sufficiently reassured before they agree to that request. Recommendations to replace informed consent with request for treatment features in the recent Scottish Cosmetic Interventions Expert Group Report.
Policy Landscape
Things were perhaps different in 1999, cultural attitudes have evolved, along with policies, guidelines and professional codes. Patients and carers are increasingly knowledgeable, confident and expect to share decisions. The role of community and third sector organisations and charities, for example the ALLIANCE (which is the national third sector intermediary for a range of health and social care organisations) have been instrumental in championing policies, meaningful information, advice, advocacy and support for people to be in the driving seat of their care. Modern media and the internet have made medical knowledge accessible and have provided opportunities for hosting online communities for peer support.
In 2012 Scottish Government published The Charter of Patient Rights and Responsibilities a key thread of which is around Communication and Participation: the right to be informed and involved in decisions about healthcare and services. It chimes with 2008 GMC Guidance on consent: www.gmc-uk.org/guidance/ethical_guidance/consent_guidance_index.asp.
"Fundamental to the doctor and patient relationship is the requirement that a patient with capacity to decide should be informed about the treatment options open to him or her; the risks and benefits of each option; and be supported to make their choice about which treatment best meets their needs."
Many professional bodies such as Royal Colleges have produced updated guidance on consent and shared decision-making.
Public information sources such as NHS Inform are encouraging people to play an active role in decision-making by making them aware of their rights regarding consent and promoting "It's OK to Ask" to ensure people get the most out of their healthcare appointments.
There are rising expectations and perhaps, to a degree, health consumerism. Faced with increased access to almost every other aspect of life it might not be unreasonable for patients to expect the same ease of access to healthcare professionals, both electronically and face-to-face. This expectation may be in addition to the existing access arrangements - NHS 24, A&E, NHS Inform, out of hours GP services.
There are 4.1 million outpatient appointments in Scotland per year, of which 2.7 million are follow up appointments. Might it be appropriate in some specialties for outpatient appointments to be tailored to more immediate access when the person has symptoms/needs to be seen rather than "routine follow up" arrangements? The Scottish Government Delivering Outpatient Integration Together (DOIT) team is working to streamline outpatient visits and is keen to have input from interested clinicians.
Shared decision-making is core to the safety, effectiveness and person-centredness of care and therefore resonates with Scotland's Healthcare Quality ambition. The person centred portfolio in Scottish Government is driving and supporting policies and quality improvements that help reshape health and care through the lens of people using services. For example, people with low health literacy face many barriers to shared decision-making. Low health literacy is a key determinant of poor health outcomes and a significant cause of health inequality. In response to this, Scottish Government produced "Making it Easy" which set out key actions to help NHSScotland rise to the challenge of responding to people's health literacy needs.
Changing Practice
Despite favourable policies, implementing shared decision-making in practice is problematic given the constraints of delivering healthcare. This may be particularly difficult in hospital settings where professionals and people may have little previous knowledge of each other. In part it needs to be addressed by pragmatic solutions that can dovetail into existing practice, but it also needs considerable organisational and whole systems change to support what is a fundamental shift in the relationship between people and professionals. At its core, it involves making those short and precious interactions that professionals and people have together, as productive as possible. This involves thinking outside of the consultation to prepare both parties beforehand and augmenting the process afterwards.
Simple approaches can readily be implemented within consultations to improve communication by avoiding jargon, and checking understanding, using techniques such as Teach Back. Teach Back involves a person paraphrasing, in their own language, what they have understood. It is a simple, yet powerful, method to screen for misunderstanding. NHS Tayside, are exploring how Teach Back can be routinely applied to informed consent procedures.
There is a great opportunity to build on existing tools and develop new innovations to support shared decision-making out with the consultation. Important approaches include:
- Personalised information sharing so that a person can have in advance, and reflect on, the same information that their professional has about them. The challenge is to provide this information in formats that are meaningful. IT developments such as shared medical records and patient portals (e.g. My Diabetes, My Way and Renal Patient View) can aid this process. It should also be helpful for people to provide personal information about themselves that they wish to share with their professional in advance.
- Shared decision aids are widely available for many conditions to help people explore their preferences with their professionals and find options that best match those preferences. However, they can be difficult for some and people may need help to use them.
- Information tailored to need: Written information has often proved disappointing, either because there is too much or challenges those with poorer reading skills. We need to look beyond relying exclusively on patient information leaflets. Digital technology now makes it feasible to provide information in more engaging, multimedia formats to enhance people's confidence and skills in sharing decisions.
- Written summary or audio recording: People can find it difficult to remember or interpret what has been discussed and it is helpful to leave with a record of their encounter. Professionals may find it challenging to have their consultations recorded but can take comfort that it can be highly valued by their patients.
A pragmatic example of how practice can be re-configured to enhance shared decision-making is illustrated by the Navigator Project (see below).
The Navigator Project at the Western General Hospital in Edinburgh set out to improve shared decision-making about treatment options for men diagnosed with early prostate cancer. They met with a "navigator" who helped explore what was important for them in terms of quality of life, life expectancy, acceptability of side effects etc. They then shared meaningful and tailored information. When they met with the specialist, both were able to have a more productive conversation about the choices they faced. They were then given an audio recording of that consultation so that they could replay it at home, perhaps with their family. Interestingly the study showed that those people who took part in Navigation opted for less invasive treatment and, at follow up, had less regret about the decisions they had made compared with those who received usual care. There are plans to develop an online tool to augment the navigation process.
Catering for this new type of relationship that our empowered "Google generation" has with those that deliver health and care, is one of our biggest challenges. We will need to create system and organisational change to embrace and promote it, mindful that those who are the least empowered will need the greatest help to flourish.
Such system change is articulated in models such as the House of Care (see Figure 2), which provides a useful representation of the components, all of which are required, to place collaborative, relational decision-making and planning at the heart of our system . Integrating these components into practice will take time but early progress is being made in Scotland with those adopting this approach with people living with long term conditions. A key initial phase of this is in developing the skills and values that healthcare professionals require for shared decision-making.
Figure 2: Scotland's House of Care
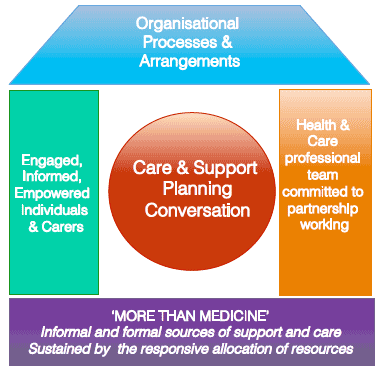
Finally, different groups whether they are nurses, pharmacists, allied health professionals, doctors, or in social, community or voluntary care have different skills, approaches and resources that can help and empower people to be fully involved in decisions. There are great opportunities to integrate this skill mix and share learning to enhance shared decision-making.
Conclusion
The traditional "doctor knows best" approach to decision-making has proved inadequate and there is now a cultural and legal expectation on both professionals and people to collaborate in partnership decisions. This sets all of us a challenge as to how we design and develop health and care services so that it brings out the best of the expertise of people and their professionals. There is a great potential to harness the support of friends and families, as well as the resources in local and online communities to help inform decisions. It will also require us to make healthcare simpler and more engaging so that it is responsive, particularly to those with the greatest health literacy needs and those with the least support. Professionals will need to develop the personal capabilities, within an organisational system, that helps them to communicate with and support people to make the decisions that are right for them. Decisions that help them live well, and indeed die well, on their own terms.


Contact
Email: Diane Dempster