The best start: five-year plan for maternity and neonatal care
A five-year forward plan for the improvement of maternity and neonatal services in Scotland.
Chapter Four: The Review Process
The Minister for Public Health announced the Strategic Review of Maternity and Neonatal Services in Scotland in early 2015. The Review focused on creating a refreshed model of care and approach to maternity and neonatal services and to examine choice, quality and the safety of those services in light of current evidence and best practice, in consultation with service users, the workforce and NHS Boards.
The Review team was requested to make recommendations for a Scottish model of care that contributes to the Scottish Government's overall aim of delivering person-centred, safe and effective care [31] .
The full remit for the review is detailed at Appendix D.
The Review sits within the context of the Scottish Government's Transformational Change plan, which aims to define a new approach to improving the health of the population. Its main focus is on prevention and tackling health inequalities, supported by high quality health and social care systems when and where people need them, and developing new models of care at local, regional and national level.
4.1 Establishing the Review
The Review group consisted of representatives from the key professional groups involved in managing and delivering maternity and neonatal services, representatives of the Scottish Government, staff side organisations, third sector representatives and academics working in maternal and infant health research.
The full membership of the Review group is shown at Appendix E.
4.2 Structuring the Review
The Review group established four Sub-Groups, bringing together over 100 professional and frontline staff from maternity and neonatal services, academics, the third sector and professional organisations, as well as service users.
The Sub-Groups covered:
Maternity Models of Care and Neonatal Models of Care: reviewing existing service configuration and current models of maternity and neonatal care, in the national, regional and local context, considering relevant evidence and making recommendations for the future model of care.
Evidence and Data: expert academics and professionals reviewing and analysing the current data and evidence (including best practice) to inform future service provision and the discussions of other Sub-Groups, in terms of quality, safety and choice, inequalities and resource.
Workforce planning and development: reviewing the current workforce complement, key workforce strengths and challenges and considering the future workforce requirement for a safe and sustainable service across NHSScotland.
The Sub-Groups carried out their work between January and July 2016 and reported their recommendations to the Review group in August 2016. The full membership of the Sub-Groups is shown at Appendix F.
4.3 Engagement
Listening to the views of service users, staff and service providers was critical to the Review and an extensive engagement programme was undertaken in all of Scotland's NHS territorial Board areas [32] . A series of meetings and events was held to gather the views of wider stakeholders, including professional organisations and the third sector.
The overall process included the following engagement activities:
4.3.1 With service users:
The Scottish Health Council delivered a programme of public and service user engagement, across all NHS territorial Board areas to gather views from people who had used maternity and neonatal services in the last five years [33] .
Figure 7: Review Governance Structure
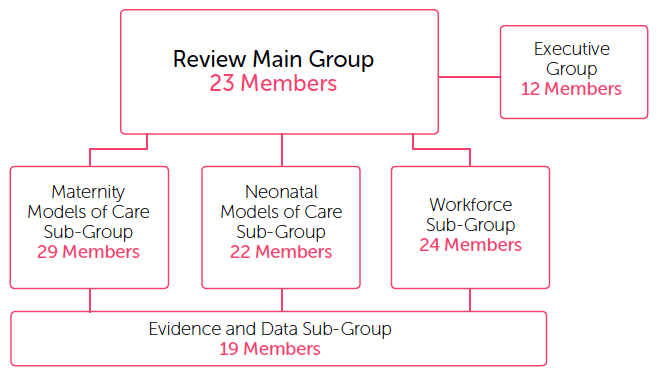
- In addition, five bespoke service user events were arranged to engage service users in remote and rural areas, vulnerable groups and mother and toddler groups.
- Over 600 women and partners participated in the engagement and 16 babies were in attendance.
4.3.2 With the maternity and neonatal workforce:
The Review Chair and a small team visited all 14 NHS territorial Boards to engage with frontline staff and management teams who work in maternity and neonatal services. These sessions provided an opportunity to hear a range of views from over 600 multidisciplinary staff, in both maternity and neonatal services, and also associated professionals such as sonographers, GPs, allied health professionals and health visitors.
4.3.3 With third sector organisations:
- Twenty-five organisations, including pregnancy and neonatal support organisations, fathers' groups and bereavement organisations attended a third sector event.
4.3.4 With other key professional groups:
- A range of other stakeholders were also consulted including the Scottish Partnership Forum [33] , the Neonatal Surgeons Group, GPs and the Scottish Ambulance Service.
- Members of the Review group led on engagement with the professional groups that they represented.
4.3.5 Surveys of service users:
- An online survey [34] was undertaken of families with recent experience of neonatal care, with over 500 responses received.
- The Review group considered recent information from the Scottish Maternity Care Experience Survey: 2015 which described the experiences of maternity care of over 2000 women who gave birth in 2015.
4.3.6 Scope of the engagement process:
The overall engagement process included the following activities:
Figure 8: Scope of engagement
| Workforce |
Women and Families |
||
|---|---|---|---|
| 14 NHS Territorial Board visits to engage with staff 41 Sessions to speak with maternity and neonatal staff in all NHS Boards 600 Staff engaged |
65 Focus groups facilitated by the Scottish Health Council in all NHS Board areas |
500 Service users attended the focus group sessions |
2000 Women shared their experiences of care Scottish Maternity Care Experience Surveys 2015 |
| 504 Responses to the Neonatal Experienced Survey |
+5 Additional events Orkney, Shetland Edinburgh, Glasgow Forth Valley |
||
| Professional, Third Sector Organisations and other Groups |
Communications |
||
| 25 Voluntary organisations attended the third sector event |
25+ Professional organisations and groups engaged in the Review: GPs, Royal Colleges, Scottish Partnership Forum, Neonatal Surgeons Group, Scottish Ambulance Service |
41 Enquiries to the Review Mailbox |
30 Blog posts published |
4.4 Communication
A monthly newsletter and blog site [35] provided updates to our stakeholders on progress during the course of the Review. A mailbox was established to gather comments and questions and over 40 enquiries and submissions were submitted from a range of individuals and organisations, which were shared with our Sub-Groups. Dedicated pages on the Scottish Government website [36] were kept up to date with information and news and over 30 blogs were posted during the Review.
4.5 Evidence and data
The critical importance of grounding the Review in a strong evidence base was recognised and agreed by the Review group. The Evidence and Data Sub-Group was tasked with reviewing the evidence base relevant to models of maternity and neonatal care. The work was conducted by researchers with extensive experience in systematic review and evidence synthesis, working closely with all the Sub-Groups to ensure relevance and timeliness. The key messages from the evidence summaries are included in the following sections.
The Evidence and Data Sub-Group produced a series of eight efficient evidence reviews, with input from colleagues on the other Sub-Groups. A protocol for a systematic, efficient, and quality controlled review process was developed and agreed. On the completion of each review, a summary of the relevant evidence and key messages was developed and organised according to the categories of the framework for quality maternal and newborn care from the Lancet Series on Midwifery framework for quality maternal and newborn care (Renfrew et al., 2014) [37] . These efficient reviews have sought all relevant evidence, assessed it for quality, and produced an accessible summary relating to the delivery of services. They provide our evidence base for the Review.
4.6 Outcomes from the engagement process
The engagement process with mothers, partners and families has provided significant insight into the current service provision. It has also identified areas where improvements should be made. Staff have highlighted many examples of innovative practice and service provision where teams across NHSScotland are working together to provide high quality, person-centred care. They also outlined opportunities for improvement.
What women and families told us about services
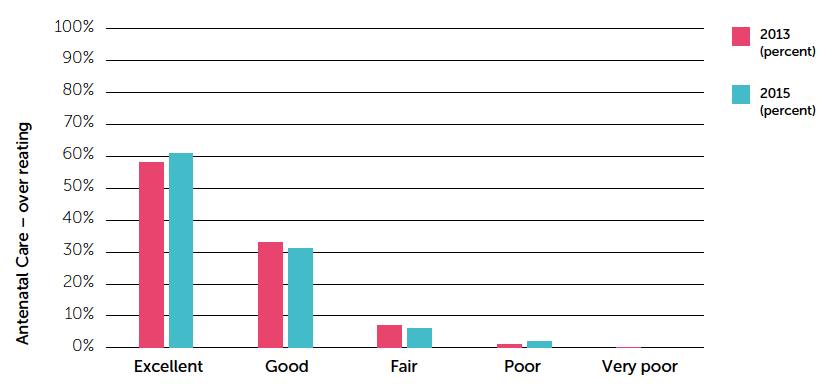
In general, the quality of maternity care in Scotland is rated very highly by service users, with 92% of women rating their antenatal care as 'good or very good' [38] . Women reported very positive experiences of their care and treatment, during that phase of their maternity journey. However, there were other key elements of overall maternity care which were viewed as less positive.
Many parents of babies who received neonatal care expressed gratitude to the staff for the life-saving treatment their babies received, the positive atmosphere in the neonatal units, and the commitment and compassion of NHS staff. They also appreciated the support offered in planning for their discharge.
Figure 9: Overall rating of antenatal care
Data source: Scottish Maternity Care Experience Survey: 2015
In the overall engagement process, service users and families also highlighted a number of areas where they considered improvements could be made.
What we heard:
Continuity of Carer
A strong theme was a desire for continuous care and continuity of carer throughout the maternity journey, delivered by the same person throughout pregnancy, labour and birth, and following the birth. Women indicated that they wanted to form a relationship with the professionals caring for them and preferred to be cared for by one midwife, or a small team of midwives, through their maternity journey to ensure consistent practice and advice.
'The midwives were excellent, but I never saw the same midwife twice - it was a different midwife every time. I was recovering from surgery and it would have been beneficial to see the same midwife.'
Scottish Maternity Care Experience Survey: 2015
Family-centred care
Partner support
Many women stated that they wanted to have their partners with them throughout their labour and birth. However, only 58% of women reported that their partners were able to stay with them during their postnatal stay in hospital. Where partners were fully involved, including being able to stay with mothers before, during and after the birth, women stated that their presence assisted in reducing anxiety and isolation, with partners providing emotional and practical support to women in hospital.
The partners who contributed to the engagement programme indicated that they wanted to be an integral part of the whole antenatal, intrapartum and postnatal journey in order to promote family attachment and bonding and support the mother with personal and baby care.
Breastfeeding
Many women described good support and advice in relation to breastfeeding. However, others described a more challenging situation with limited support both in the early period after birth and on an ongoing basis. Women felt it was important that their decision to breastfeed or formula feed their baby was respected and supported.
'I had difficulties breastfeeding and I felt like I had too many people telling me different ways of trying to breastfeed. Although they were just trying to be helpful, I just needed a bit of consistency.'
Scottish Maternity Care Experience Survey: 2015
Bonding and attachment
Many women with babies in neonatal care reported that they would have preferred to have the opportunity for more direct skin-to-skin contact with their baby. They suggested that good staffing levels, space, privacy and a more comfortable environment would assist in this aim.
Emotional support
Parents of babies in neonatal care will often need additional emotional support, and families expressed great appreciation of the care and compassion demonstrated by staff in supporting them at this difficult time. Many parents wanted more information on how to access counselling as this was provided in a range of ways across Scotland, with a lack of uniformity and approach.
Bereavement
Bereaved parents expressed the need to be supported in a personal and sensitive manner, depending on their individual circumstances, with a clear desire to have services provided for them in discrete, dedicated areas to allow them the space and privacy to grieve.
Person-centred care
Throughout the whole pregnancy journey, women stated that they would value further information to assist them in their decision about the place of birth and, in particular, on pain relief. A minority reported being offered limited, or no choice over their preferred place of birth. Women also stated that they sought modern facilities within their chosen birthing environment, including hypnobirthing and birthing pools and wanted home birth to be a real option.
Following birth, practical help and assistance with personal care, baby care and infant feeding were important to women. The area of service where women commented most negatively related to postnatal care, with women reporting not always getting the help and assistance required due to perceived pressures on staff time and a lack of continuity in their care.
'The midwives on the ward were too busy and did not have time to help with bottle feeding, changing nappies or bathing. As a first time mum, I felt that I needed more assistance.'
Scottish Maternity Care Experience Survey: 2015
Women and families were anxious about being separated from their baby and wanted separation to be minimised. Mothers told us that being in a postnatal ward without their baby, alongside other mothers and babies was upsetting, and that they would have preferred to have been cared for nearer their own babies.
The need to improve communication and information in relation to the progress of their baby was a key issue for many families who highlighted a lack of clarity which caused additional stress. Parents reported inconsistencies in advice and approach to parental involvement as being of concern as they wanted to be fully involved in the care of their baby, whilst recognising that might not always be possible.
Access to services
Local access to services was an important issue for many women. In remote and rural areas, women reported having to travel long distances for appointments while, in a more urban environment, local transport arrangements were highlighted.
In island communities, there was a desire to have as much care as possible provided locally, although women did recognise the need to ensure that services were safe and sustainable. Travel challenges leading to lengthy periods away from home were particularly difficult for families with other children or caring responsibilities.
For parents of babies in neonatal care, both travel time and expense were highlighted as an issue, and this was also highlighted in the Bliss 2014 report: 'It's not a game' [39] . Parents told us about complex and lengthy journeys to get to the unit, often with limited access to local accommodation. These concerns disproportionately affect those on lowest incomes and those living furthest from the unit.
'My boyfriend had to book a hotel to stay in for four nights, which cost us money we didn't have.'
Scottish Health Council Report: 2016
Digital information and technology
Women and families want to be able to access high quality, up-to-date, unbiased electronic information about pregnancy, birth options, caring for their baby, and neonatal care. Women and families expect information to be available on the internet or through technology such as mobile apps, rather than through the traditional paper-based routes. There is also an expectation that all health professionals will be able to access relevant maternity and neonatal records to facilitate understanding and to improve communication. A general desire was expressed to move towards electronic records and away from paper-based systems to enable smoother care transitions.
Communication
The quality of communication has also been a recurrent theme in the feedback from women and families. Many women reported good communication from staff, particularly during labour, and spoke very positively about the caring and compassionate approach from staff. Professionalism and confidence in the staff were all highlighted as being important during labour and birth and, generally women reported that the current service did deliver on these key elements of care.
However, some women stated that staff had limited time to listen and respond to their concerns and, in particular, younger mothers reported not being listened to. Women described seeing many different staff during their pregnancy and being frustrated at continually having to repeat their story. Inconsistencies in communication between community and hospital staff, and inconsistent advice from different members of staff within a care setting were also highlighted.
Women whose first language was not English raised the importance of translator support, and the need for information to be provided in their own language.
Figure 10: Extracts from Patient Opinion - from mothers and families who have had recent experiences of maternity services in Scotland (2013 to the present day)

What healthcare professionals told us
NHSScotland healthcare professionals and frontline staff have immense pride in the service that they provide and staff showcased their examples of innovative good practice happening in NHS Boards. Staff did, however, highlight a number of challenges in delivering services in the current manner.
What we heard:
Maternity and neonatal staff
Maternity care staff highlighted:
- Continuity of carer is important but challenging in the current system, particularly for women with complex care needs.
- National care pathways are seen as overly restrictive and inflexible, with too many women categorised as high risk.
- The issue of the sustainability of some of the rural community maternity units, especially where a very small number of women are accessing the facility, with the consequent challenges of staffing and skills maintenance.
- The sustainability/desirability of continuing to offer home birth in view of the declining home birth rate in some areas needs further consideration.
- The rate of medical intervention in maternity care is increasing, and there is a rising caesarean section rate, with the associated implications for women and babies.
Neonatal staff described some very positive developments in promoting safety, such as daily safety huddles and innovations in terms of family-centred care, such as the development of transitional care to keep mother and baby together.
However, they also reported a range of issues, including:
- Pressures on availability of neonatal cots, often linked to staffing challenges, and the complexities associated with arranging transfers.
- Improvements needed in facilities available for parents, especially when babies were in units for lengthy periods, or were being treated outwith their local area.
- The consistency and quality of information for parents and the need for wider use of electronic technology.
- The need for an improved model of neonatal community care to allow babies to be discharged earlier with appropriate support.
- The variability in the provision of Allied Health Professionals across Scotland.
Digital information and technology
Emerging innovative practice relating to the use of information and information technology was evident in a number of NHS Boards. However, during the engagement process staff indicated that there was significant further potential in this area including:
- A more structured and systematic use of telemedicine to enhance care for multi-professional and service user consultations and for education and training.
- Clarity on the use of data and streamlining of the multiple requirements for data entry, including the development of a national dataset and dashboard to allow benchmarking across Scotland to drive improvement.
- Improvements to communication and information sharing within different care settings in NHS Boards (particularly community and acute care), and between NHS Boards.
- The development of a uniform electronic maternity record.
Quality and safety
In relation to quality and safety, staff also highlighted a number of areas where there had been significant improvements in recent years. In particular, they indicated that there had been a renewed focus on quality and safety with daily safety briefings, huddles and handover meetings being routinely in place which served to promote communication, teamwork and patient safety.
Staff also raised a range of other issues including:
- The positive benefits of multidisciplinary training in developing team working and a mutual understanding of roles and responsibilities.
- The need for a rigorous approach to learning from adverse events across the full range of maternity and neonatal services.
- The need to ensure that the routine examination of the newborn is systematically undertaken to a high standard and audited.
Workforce
Staff outlined a range of forward-thinking, flexible and innovative approaches to staffing maternity and neonatal services, and this was particularly evident in more rural areas. It was also evident that existing midwifery and neonatal workforce planning tools are being widely utilised to assist in meeting the needs of the service.
However, a number of key staffing issues were also highlighted:
Sustainability of service delivery
- Increasing workload and the impact on contact time with women, related to the expansion of the midwifery role.
- In relation to medical staffing, covering middle grade rotas and the impact of resident consultant cover were raised as important issues.
- Recruitment and retention in a number of staff groups, in addition to the age profile of the midwifery and neonatal nursing workforce, was identified as a real concern in some areas.
- The availability of a range of staff to support maternity and neonatal services, including allied health professionals, sonographers and administrative and clerical staff.
Skills and training
- The need for a clear career pathway from registration to enhanced clinical roles in midwifery, including the development of advanced practice roles.
- Variability in the models of theatre staffing with a clear need to ensure adequately trained and dedicated staff are in place.
- The need for protected time for training of nurses and midwives.
- The Neonatal Qualified in Speciality training course is highly regarded by staff and should continue to be available.
- A requirement for further clarity and development of the roles of support staff, with the associated training needs.
Remote and rural issues
The need for a broader, and different, skillset in remote and rural settings to deliver local services safely.
The need to develop locally accessible training and learning options for staff to maintain essential skills, and expanding the use of technology for training. The ability to formally rotate through larger units to maintain and develop staff expertise in a systematic manner was highlighted.
Recruitment and retention is particularly challenging in remote and rural areas.
What third sector organisations told us?
During the engagement process, the Review team met with a number of third sector organisations providing a range of services. They provided a key insight to the challenges faced by their organisations in seeking to support families in their maternity and neonatal journey.
Awareness
One of the key issues highlighted by third sector organisations related to their ability to ensure that families were fully aware of their services and how to access them. They indicated that this was often a real challenge and stated that a uniform approach to raising awareness would greatly assist in linking their services to families who could benefit from their input.
Bereavement
A number of third sector organisations provide specific services for bereaved families and they want to ensure that their services are highlighted to bereaved families at the right time and in a sensitive manner. NHS services are provided in most NHS Boards but their precise configuration is variable and third sector organisations believe that they are well placed to support families, provided those families are made aware of their services at the right time.
4.7 Outputs from evidence
4.7.1 Efficient evidence reviews
Eight efficient evidence reviews [40] were developed and signed off by the Evidence and Data Sub-Group. Six reviews were prepared by the Evidence and Data Sub-Group and two by the Maternity Models of Care Sub-Group, in collaboration with the Evidence and Data Sub-Group.
The list of authors and sponsors of the efficient evidence reviews is detailed at Appendix G. A summary of the conclusions of all the efficient evidence reviews is detailed below. The full conclusions are shown at Appendix H.
Definitions of Models of Care
No single, uniform definition of either a maternity or neonatal model of care was identified by this efficient evidence review. Crucially, in reports of maternity models of care, the primary focus of existing studies is on who is delivering the care and making decisions (i.e. midwife, obstetrician) and/or the location of the care. Whereas, in reports of the neonatal models of care, the focus is on whether or not the family was involved in the care and/or decision-making.
A generic definition was used to guide our thinking in considering models of maternity and neonatal care: 'an overarching design for the provision of a particular sign for the provision of a particular type of health care service that is shaped by a theoretic basis, EBP (evidence-based practice) and defined standard. [41]
Guided by this definition, an approach was developed to models of care that included consideration of a theoretical basis, the evidence base, and defined standards to inform the work. This approach distinguished between:
- Models of care (i.e. the overarching design and characteristics of the service).
- Service configuration (i.e. numbers and types of units and their geographic distribution).
- Workforce (i.e. skill mix, numbers and distribution of staff).
- Characteristics of care providers (i.e. multidisciplinary working, education and training).
The categories developed by the Lancet Series on Midwifery framework for quality maternal and newborn care (Renfrew et al., 2014) were used to distinguish between what care is provided, how that care is organised, the qualities of respectful care, engaging women and families, and valuing normal processes, and who should provide that care. These characteristics are all important and have an impact on outcomes, but they act in different ways and all need to be understood and considered.
Improving Care, Services and Outcomes for Women and Babies from Vulnerable Population Groups
This efficient evidence review identified the following key aspects of high quality care for women and babies from vulnerable groups:
- Continuity of carer is important to enable all women to develop respectful and trusting relationships, with non-judgemental staff who are empathetic and knowledgeable about the woman's individual needs.
- Positive staff attitudes and knowledge could be improved by culturally sensitive training and education on care for women from vulnerable groups.
- Effective communication, such as good interpersonal skills, is important, alongside providing assistance for women with low literacy or for whom English is not a first language.
- There should be a universal model of effective multi-agency care for all women. Women with particular needs - clinical, social and psychological - should have additional multi-agency services appropriate for and proportionate to their circumstances.
- Services should be highly accessible (i.e. multiple barriers addressed), and of a high technical quality for all women, with the ability to incorporate additional care for specific conditions.
Models of Maternity Care for Critically Unwell Women
This efficient evidence review indicated that both critical care and maternity/obstetric needs must be considered, with normal midwifery care continuing to be provided for all women, even when critically unwell. It was found that the potential to address this issue could, in part, be facilitated by training midwives in critical care skills and training critical care nurses in midwifery skills. This review confirmed that women and babies should be kept together whenever possible which is clearly in line with the expectations of mothers and families and will assist with bonding and attachment, as well as issues such as breastfeeding.
Organisation of Services for Childbearing Women and Babies across the Continuum
A number of overarching principles were outlined within this efficient evidence review. In particular, it indicated that quality care should not dichotomise safety and choice. Instead, the service should ensure safety by implementing effective practices, tailoring care to the needs of women and babies, treating all women and babies with respect and compassion, and enabling the woman and her partner to make truly informed decisions.
The review also concluded that there should be a universal model of care that runs across the whole continuum from pregnancy through to the early weeks after birth. Throughout this journey, all women and babies should receive midwifery care and those with additional needs should receive the specific additional care they require, in conjunction with ongoing midwifery care. The care provided should aim to optimise the normal processes of pregnancy, labour and birth, postpartum, early life, and breastfeeding, and avoid unnecessary intervention.
The review also stated that care should be provided by a multidisciplinary team with the appropriate skill mix to care for a woman and baby's individual needs. This care should be integrated across the continuum - from pregnancy to postpartum - and across all settings, from home to hospital.
Models of Care for Infants requiring Neonatal Services and their Parents
The review identified a number of key principles for neonatal care, including the provision of a family-centred model of care which would provide families with the opportunity to have as much contact with their baby as possible. The review also concluded that, as far as possible, parents should be included in the decision-making process and in providing aspects of care for their baby.
The review found strong evidence for the provision of kangaroo skin-to-skin care for babies in neonatal units and early support for breastfeeding or feeding with breast milk, both of which result in improvements in clinical and psycho-social outcomes. Providing this routinely for all babies and parents will require changes in care and improved facilities for parents.
The review also indicated that rationalisation of intensive care services may provide the optimal outcomes for very sick infants.
The review also outlined that, when moving babies any distance from their home, services should consider supporting parents to remain in close contact with their infants and also facilitate a return to more localised care as soon as possible to ensure parental involvement can be optimised.
The review also indicated that low staffing profiles and over-crowding can be associated with poorer outcomes for infants requiring neonatal care.
Whilst studies on supported early discharge show positive results, further research to examine the safety, efficacy, acceptability, and resource implications are needed.
Improving Inter-professional Working
This efficient evidence review found that inter-professional education has positive effects on team working abilities as it offers participants the opportunity to gain a better understanding of their colleagues' roles, which has been identified as a barrier to good inter-professional working. In addition, opportunities for health professionals from different disciplines to regularly meet and discuss the needs of women and babies in their care has been associated with improved collaborative care, including management of risk.
The review suggested that this type of arrangement will also give health professionals a chance to understand each other's roles and competencies and develop trust.
This review also found that standardised approaches to improving communication, in terms of record-keeping for women and babies and interfaces between levels of care and in emergency situations (e.g. SBAR - Situation, Background, Assessment, Recommendation tool), can help make inter-professional working easier and reduce errors.
Place of Birth
This efficient evidence review indicated that there is high quality evidence to support the promotion of real choice for women about the location of their maternity care through pregnancy, labour and birth, and following birth. Studies have demonstrated that midwifery care settings including home birth, freestanding midwifery units and alongside midwifery units, are a safe option for the majority of healthy women with uncomplicated pregnancies. Models of care should relocate and support maternity professionals to reflect the shift from hospital-centred to community-centred care and team systems should be implemented that support the provision of community-based maternity care, including intrapartum care.
The review concluded that evidence-based accessible information and decision aids for women, families and health professionals should be developed to enable real choice about the options available to them.
The review found that care should be delivered in appropriate community settings. The way in which these should be configured is likely to vary across settings and local developments should be evaluated.
Continuity Models of Care
In line with the findings of the review that examined care across the continuum, this efficient evidence review concluded that midwife-led continuity models of care throughout the child birth journey have been found to have a range of benefits in relation to birth outcomes with no identified adverse outcomes. Where women require interdisciplinary team care due to complications, it is of benefit for them to also receive continuity of carer that enables them to build relationships with the health professionals providing their care.
4.7.2 Further data analysis
In addition to the efficient evidence reviews, Information Services Division, part of NHS National Services Scotland, conducted a series of data analyses as part of the work of the Evidence and Data Sub-Group including:
- International Comparative Analyses of Scotland's Perinatal Outcome Indicators [42] .
- The number of beds available in maternity and neonatal services and bed occupancy rates 2001-2015 [43] .
- The number of women giving birth in different types of facility, overall activity (attendances and admissions) in maternity services and total expenditure on maternity care 2012/13-2014/15 [44] .
- The number of babies admitted to neonatal care and total expenditure on neonatal care 2012/13-2014/15 [45] .
- The level of neonatal care provided (e.g. intensive care, high dependency) and characteristics of admitted babies (e.g. gestation, birth weight) 2012/13-2014/15 [46] .
These data were available to inform the work of the Sub-Groups.
4.8 Additional Evidence
Three additional pieces of work were generated by the Evidence and Data Sub-Group to inform the Review and implementation of the findings.
Economic Considerations
This paper sets out a framework and associated actions for consideration of the economic implications of the Review recommendations. It proposes that the main recommendations from this Review are analysed further in terms of which changes are likely to result in cost savings, and which will result in cost increases over time. It also proposes that a programme of work on priority setting is devised at national or NHS Board level on significant areas of resource use, informed by service users and clinicians.
Maternity and Neonatal Health Outcomes
This commentary considered the consequences of short and long term pregnancy and birth health outcomes. It outlines how poor pregnancy and birth outcomes carry with them a 'long reach' throughout life exemplified by the:
- Considerable burden of lifelong disability among very low birth weight infants.
- Long-term consequences of undertreated postnatal depression and the impact on families.
- Short- and long-term impact of breastfeeding on a child and woman's health.
The social and economic consequences of these short- and long-term outcomes have been shown to be extensive. For example, as breastfeeding rates, like most other health behaviours, are socially patterned, this also has the effect of increasing inequalities in health.
International Comparative Analyses of Scotland's Perinatal Outcome Indicators when compared to other EU Countries
This paper presented comparative outcomes across a range of indicators and concluded that:
- Perinatal mortality is consistently higher in Scotland than Scandinavian countries.
- Maternal mortality is uncommon in high income countries, and is slightly higher in the UK as a whole than other Western European countries.
- Prematurity and low birth weight rates are higher in Scotland than in Scandinavian countries.
- Maternal smoking rates are relatively high in Scotland compared to Europe.
- Scotland has the highest rate of maternal overweight and obesity of any of the countries studied.
- Scotland has a noticeably lower proportion of spontaneous vaginal deliveries than any of the Scandinavian nations or the Netherlands.
- Home births are generally uncommon in the countries studied, with the exception of the Netherlands (16.3% in 2010).
- Although Scotland has a high number of very small maternity units, collectively they account for a low proportion of all births.
- Breastfeeding rates, in particular at older infant ages, are particularly poor in Scotland.