The best start: five-year plan for maternity and neonatal care
A five-year forward plan for the improvement of maternity and neonatal services in Scotland.
Chapter One: The Case For Change
Scotland's maternity and neonatal services are generally providing high quality care, with high levels of satisfaction amongst women and families who use those services. However, services have largely developed over time, rather than being designed around the needs of women and families, leading to different approaches and care across Scotland.
The changing needs of the population also mean that services will no longer be fit for the future. There are a number of drivers for change including population health and demographic trends, the need for quality improvement, workforce pressures and emerging evidence. Within the context of wider change within NHSScotland, this Review offers a unique opportunity to place the current and future needs of women and families and person-centred, relationship-based care at the heart of redesigned maternity and neonatal services.
1.1 Population health
While the general population is living longer and major advances have been made in tackling disease, complex health challenges remain which are of significance for pregnant women and families.
The Chief Medical Officer's Annual Report 2014-15: Realistic Medicine [1] , underlines the prevalence of key inequalities in our nation's health. Significant proportions of the Scottish population are dealing with the impact of co-morbidity, where they are living with two or more health conditions. This situation poses challenges for health and social care provision generally, driving a need to shift to truly person-centred services which focus on the holistic needs of people, rather than disease specific approaches to care.
While most women remain healthy, the above trends are evident among childbearing women, with a steady rise in older mothers and women with a range of other health issues and long-term conditions. These factors are associated with an increased need for intervention. In addition, women living in poverty, teenage mothers, women with mental health issues, and other vulnerable women are more likely to have poor pregnancy outcomes.
Maternal health and wellbeing is directly related to infant mental and physical health, underlining the importance of access to perinatal mental health services throughout the pregnancy journey. The provision of services for women with mental health issues is a key public health challenge. Significant numbers of women may be affected by mental illness in any one year, and mental ill-health is more common in deprived populations.
A significant proportion of the total burden of disease is preventable, and directly linked to risk factors including smoking, alcohol use, being overweight and lack of exercise. Long-term conditions are having a significant impact on the health of women. Health inequalities persist, with higher rates of obesity, alcohol-related mortality, smoking, alongside lower participation in physical exercise, in Scotland's most deprived communities.
Obesity is a significant issue, with almost two-thirds of adults classed as overweight or obese. Women are known to have higher rates of obesity than men and emerging evidence suggests that overweight children are more likely to become obese adults, with a higher risk of morbidity, disability and premature mortality in adulthood compared with healthy weight children. Maternal obesity is associated with poor maternal and infant outcomes, including premature birth, intrauterine growth restriction and increased chance of caesarean section. Almost half of women giving birth in 2014/15 in Scotland were classed as overweight or obese.
Alcohol sales data show that adults in Scotland drink almost a fifth more than our English and Welsh counterparts, and that our population has the highest rate of alcohol liver disease and cirrhosis in Western Europe. Smoking is the leading preventable cause of ill-health and premature death in Scotland, with half of all regular cigarette smokers estimated to die prematurely as a result of smoking. Smoking and alcohol in pregnancy are known to be harmful to both mother and baby, and whilst smoking rates are falling, this remains a significant contributor to maternal and infant ill-health.
Figure 1: Maternal body mass index at antenatal booking. Year ending 31 March 2015 [2] .
Data source: SMR02 ISD Scotland
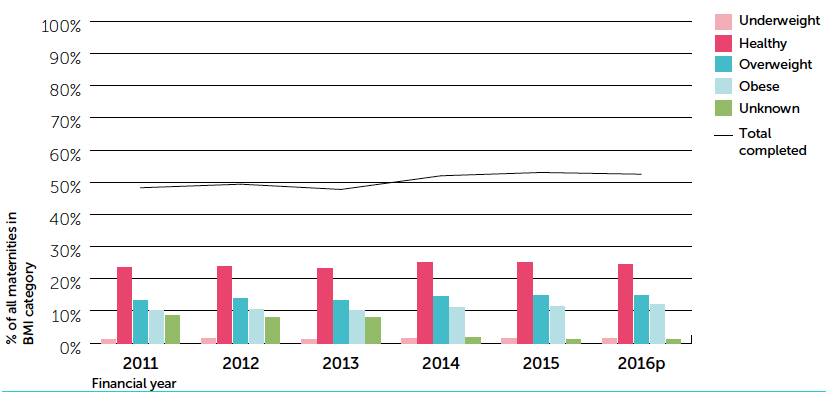
1.2 Opportunities to improve health
The correlation between maternal health and lifelong health, wellbeing and attainment of children is well evidenced. Ensuring the best start in life for children will have a profound effect on improving generational population health.
Previous reports and evidence have highlighted the critical role of the right maternity care in contributing to reducing health inequalities for women and families, and improving infant development, through early identification of needs and timely intervention.
Improving population health and reducing the inequalities gap requires a public health approach within our maternity and neonatal services which is universal, while taking account of the unique needs of each woman and her family.
Breastfeeding has a positive impact on short- and long-term maternal and child health, with children who are breastfed less likely to suffer childhood obesity, gastrointestinal infection or respiratory disease, and to have improved cognitive and behavioural development. Breastfeeding is also known to reduce the risk of maternal breast cancer. Yet rates of breastfeeding in Scotland are low overall.
Positive, person-centred care in pregnancy and after birth can have a significant impact throughout life. Conversely, poor care can have an impact on wider family health.
1.3 Learning from audits, reports and evidence
A range of national audits and reports have made recommendations for improvements in the care and services for women, babies and their families, including MBRRACE- UK Mothers and Babies: Reducing Risk through Audits and Confidential Enquiries across the UK [3] and the Scottish Maternity Care Experience Survey: 2015 [4] .
In addition, two significant recent investigations into maternity care, the Report of The Morecambe Bay Investigation: 2015 [5] and the Montgomery Judgement: 2015 [6] have implications for the way services are delivered in Scotland.
These audits and reports contain a wealth of information in relation to the current services, both in terms of strengths, and also areas of challenge where improvements are required. The case for these reports to be used to drive improvements and change is clear and this Review offers the opportunity to address a number of the issues raised.
1.4 Future service provision
The needs and expectations of childbearing women and their families are changing, and services should be streamlined and designed to respond across a spectrum of unique family requirements. This spans optimising the normal processes of pregnancy and birth for all women, whilst also ensuring women who need additional care and support have access to the interventions they need and the provision of intensive care for the few who need it. Models of care need to improve outcomes for all women and babies, paying particular attention to the most vulnerable families.
1.5 Workforce considerations
A significant range and number of the overall NHS workforce in Scotland support maternity and neonatal services, either directly or indirectly. Although different parts of the country have slightly different models supporting the delivery of maternity and neonatal care, similar issues are observed across Scotland.
Workforce supply: Issues such as recruitment, retention and age profile affect all maternity and neonatal units to some extent, however these are more acute in some areas, with particular challenges in some professional groups. The graphs at figures 2 and 3 show the age profile of midwives and neonatal nurses across the east, west and north of Scotland, which demonstrate some of the challenges in relation to the age profile of our current workforce.
Role development: Professional roles are continually evolving and changing, and need to support the model of care that is in operation now, as well as the future model. Unplanned, or unsupported, expansion of roles can lead to a lack of clarity within teams and growing service demand means it is increasingly important to fully utilise the skills and training of all staff.
Education and training: It is vital that this keeps pace with the skills requirements of the workforce, is relevant, accessible, flexible and fit for purpose. This applies to undergraduate, postgraduate and continuous professional development, in addition to skills maintenance.
Culture: The Morecambe Bay Investigation: 2015 and others, such as MBRRACE Confidential Enquiries, have focused on the important influence of workplace culture and behaviours on the quality and safety of the clinical care being provided. Across NHSScotland, much has been done to promote the standards of behaviour that are acceptable and to tackle bullying and harassment in the workplace. However, the NHSScotland Staff Survey: 2015 National Report [7] results demonstrate that there remains a need to secure sustained improvement in culture.
1.6 Views of service users
The views of current service users are critical in informing the future design of services to ensure that the changing expectations of women and their families are being addressed. A wide programme of engagement during this Review process ensured that these views have been given a high priority in influencing the shape of future service provision, building on evidence available from national surveys and third sector reports.
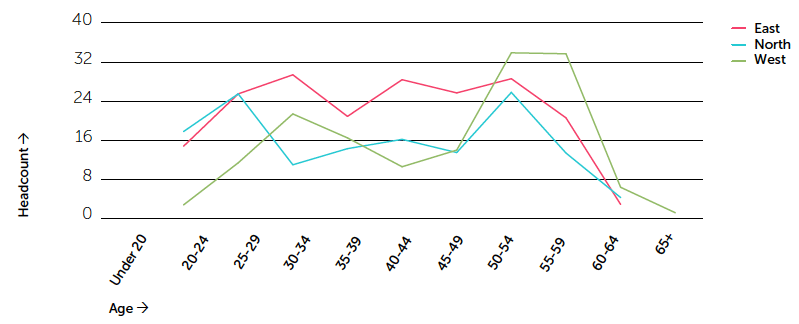
Figure 2: Midwifery age profile by region
Data source: Scottish Workforce Information Standard System ( SWISS) as at 30 June 2016
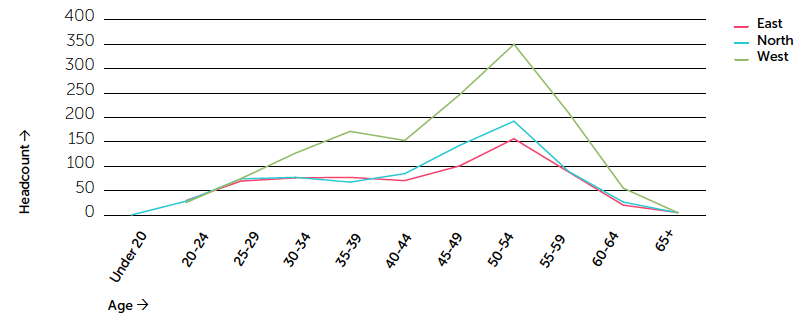
Figure 3: Neonatal nurse age profile by region
Data source: Scottish Workforce Information Standard System ( SWISS) as at 30 June 2016