The best start: five-year plan for maternity and neonatal care
A five-year forward plan for the improvement of maternity and neonatal services in Scotland.
Chapter Two: The Current Model Of Maternity And Neonatal Care
The quality of maternity and neonatal services that is currently provided to women, babies and families in Scotland is good. However, changes to the birth rate, demographics, new evidence, best practice and guidelines, along with advances in clinical care and treatment, mean that they must be continually adapted and updated. This Review provides an opportunity to consider all the elements of the service to ensure a person-centred, consistent, high quality approach across all services in the future.
The overall framework for the delivery of maternity and neonatal services, in terms of the principles for care and service standards, is established at a national level. However, there is no single prescribed model of service delivery, and individual NHS Boards design services locally for their own population.
Maternity services are provided in all 14 NHS territorial Boards, offering a range of midwife-led and obstetric-led care. Neonatal services are provided from 15 neonatal units across Scotland.
Figure 4: Maternity and Neonatal Services in Scotland by area
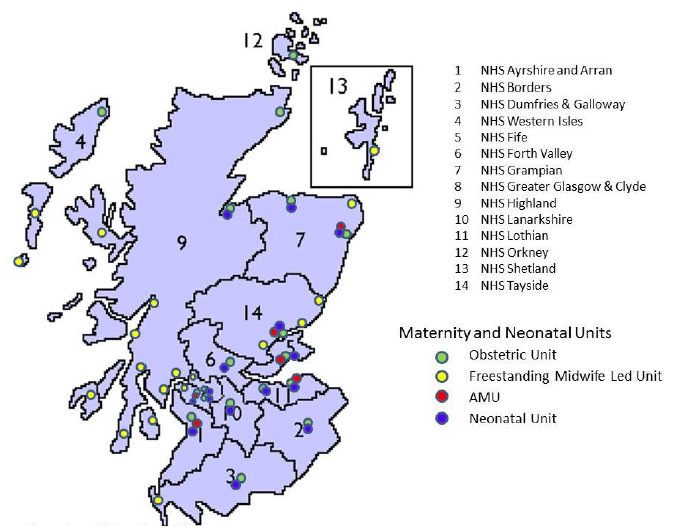
2.1 Service demand
The birth rate in Scotland has been relatively static in recent years, with around 54,000 births in 2015 [8] . Normal births have declined steadily and there has been a rise in interventions, largely from a rise in caesarean sections to 31.1% of all births in 2015 [9] , although there is significant variation in the rate across NHS Boards. This trend is converse to the aspirations outlined in the Chief Medical Officer's Annual Report 2014-15: Realistic Medicine, in terms of reducing intervention, overtreatment and unwarranted variation in clinical practice.
Outcomes and survival rates for all preterm and sick newborns have improved significantly over the last 20 years with enormous advances in newborn care. The majority of additional care provided to newborns is classified as high dependency or special care with only a small proportion requiring intensive care. However, for that small proportion, the complexity of neonatal intensive care has increased, particularly for those babies born before 26 weeks' gestation or with extremely low birth weights, those babies requiring complex modes of ventilation and nitric oxide and/or extracorporeal life support, and babies requiring complex surgery.
Current neonatal services in Scotland are geared towards intensive care provision, but while future neonatal care is likely to see continued advances in highly specialist, technically challenging management, it must be remembered that this is required for only a tiny proportion of babies born in Scotland. Furthermore, most of those babies requiring neonatal intensive care will only require such a high level of care for part of their neonatal care. Many more babies will require only high dependency and special care provision.
The percentage of babies born prematurely (before 37 weeks), or with a low birth weight has decreased slightly over the last 10 years. In 2014/15, 7.3% of babies were born prematurely and 6.2% had a low birth weight (compared to 8.2% and 7.6% respectively in 2005/06) [10] . However, improvements can be made to reduce this even further.
Figure 5: Maternity activity in Scotland 2014/15
Data source: SMR02 ISD Scotland
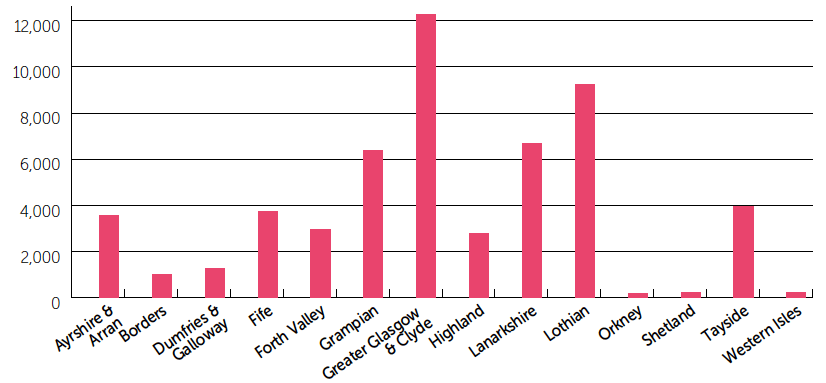
2.2 Maternity services
All women will see a midwife in pregnancy and some will also see an obstetrician and other health professionals, depending on their care needs. Most women give birth in hospital, however others may give birth at home or in a community midwifery unit. The availability of choice of place of birth varies across Scotland.
2.2.1 Antenatal care: Care of pregnant women before birth
Currently, antenatal care is delivered in both community and hospital settings. Pregnant women are encouraged to book directly with a midwife before their 12th week of pregnancy, as this will ensure that they are able to receive the best care and advice in the important early weeks of pregnancy.
2.2.2 Intrapartum care: Care of pregnant women during labour and birth
At present, most women have their baby in hospital, either in an obstetric unit or in a midwifery unit attached to the hospital (an 'alongside' midwifery unit). Only 2.6% of births take place in freestanding community midwifery units or at home. At present, the decision on where to labour and birth is based on the woman's preference and available choice locally, and by an antenatal risk assessment informed by the currently agreed NHS Quality Improvement Scotland [11] Pathways for Maternity Care: 2009 [12] .
Intrapartum care is currently provided in a choice of settings including:
Women without complications will be offered midwife-led care and women with more complex needs will be offered both midwifery and obstetric care, usually in obstetric consultant-led units.
There is currently considerable variation in the availability of choice of place of birth that women have in different NHS Boards. A full list of maternity units in Scotland is detailed at Appendix B.
During labour and birth, a number of women require the services of anaesthetic staff. This is most often for pain relief in labour or for an operative birth, and these anaesthetic services are essential, and integral, to the provision of a safe, high quality service for women.
'The doctors and anaesthetist both introduced themselves to me which I thought was very good as the first time you see them won't be when something goes wrong.'
Scottish Health Council: 2016
Figure 6: Intrapartum care settings
| Intrapartum Care Setting |
|||
|---|---|---|---|
| 18 Obstetric consultant-led units |
6 Alongside midwifery units with adjacent obstetric unit |
19 [13] Freestanding community midwifery units |
Home Birth And birth outside hospital |
2.2.3 Postnatal care: Care of women and their baby following birth
Women who have their baby in hospital or in a midwifery unit will often have a short inpatient stay in postnatal care, typically ranging from a few hours to one or two days. All women receive postnatal care in their local community for at least 10 days after birth, which is normally provided by a midwife in addition to routine GP care. Their ongoing care will usually be transferred from maternity services to the care of the health visitor around 10 days after birth, with continuing GP involvement as required.
Support for breastfeeding is often provided locally by health visitors, midwife-led clinics and a range of local support services, including peer support.
GPs will also undertake the six-week check for mother and baby and any further overall health support as required. Some women may also be offered an appointment with an obstetrician around six weeks after birth.
2.2.4 Vulnerable women
For many women, having a baby is a very difficult and challenging period in their lives and they will require additional support and care from a wider range of professionals which may not be confined to NHS services, but may include multiple agencies. The options for care for women and access to additional support are not consistent or equitable across Scotland. Some examples of good services exist but they are not available for all women.
2.3 Neonatal services
Neonatal care and services are provided to preterm babies, and term babies who have additional care needs. The intensity of care provided to babies in neonatal units is categorised in three levels:
Level One: Special Care Units
These units provide special care for the local population and a level of high-dependency care, through agreement with the three neonatal Managed Clinical Networks. Babies who require more complex or longer-term intensive care will be transferred to a neonatal intensive care unit.
Level Two: Local Neonatal Units
These units provide special care and high-dependency care and a restricted volume of intensive care (as agreed locally). Babies who require complex or longer-term intensive care will be transferred to a Neonatal Intensive Care Unit.
Level Three: Neonatal Intensive Care Units
These units provide the full range of medical (and sometimes surgical) neonatal care for the local population from a larger intensive care unit.
Transitional care has been established in some areas to support parenting skills and confidence as a key element of discharge planning. However, it is not universally available at present. In the transitional care model, the mother stays with her baby and provides care, supported by maternity and neonatal staff. There is, however, no single, uniform designation or model of transitional care at present.
Staff will determine the additional level of neonatal care that babies need. Some babies will only need neonatal care for a few hours, for others it will be much longer. Most recent data suggests that around 10% of babies born in Scotland will need some level of neonatal care [14] , with a quarter of these babies being admitted to neonatal intensive care.
A list of the current neonatal units and the level of service they provide is shown at Appendix C.
2.4 Transport services
The Scottish Specialist Transport and Retrieval Service ( ScotSTAR), is a branch of the Scottish Ambulance Service, and provides consultant-led transport services for all those babies who need ongoing care across Scotland, including planned transfers for investigations and transfers back to local units.
ScotSTAR also coordinates cot availability and neonatologist consultations. These services are provided from three regional teams-based in Glasgow, Edinburgh and Aberdeen.
In addition, the Scottish Ambulance Service operates a fleet of aircraft configured for neonatal transport. Neonatal units call a single referral line to request transport and all teams work to a standard of deployment within an hour for time-critical transfers.
The Scottish Ambulance Service also provide services to childbearing women who require transfer between care settings.
2.5 Scottish policy context
This Review sits within the overarching strategic context of the Scottish Government's 'Programme for Government' [15] and contributes to the delivery of key Scottish Government priorities, including:
- Tackling inequalities
- Reforming public services
- Improving outcomes for the population
Policies of particular relevance include:
- Getting it Right for Every Child ( GIRFEC) [16]
- The National Clinical Strategy for Scotland: 2016 [17]
- Chief Medical Officer's Annual Report 2014-15: Realistic Medicine
2.6 Maternity and neonatal policy context
There are a number of key existing policy frameworks that have been central to the overall strategic context for the delivery of maternity and neonatal services in Scotland.
The Refreshed Framework for Maternity Care in Scotland: 2011 [18] outlines the aim of improving maternal and infant health and reducing inequalities in maternal and infant health outcomes. It also established principles and service standards for maternity care across Scotland.
The Neonatal Care in Scotland: A Quality Framework: 2013 [19] , describes the delivery of high quality, evidence-based, safe, effective and person-centred neonatal care. Implementation of this framework is currently being supported through the three regional neonatal Managed Clinical Networks in the north, east and west of Scotland.
2.6.1 Quality and safety - audit and improvement activity
Scottish maternity and neonatal professionals work within a set of clinical and professional guidelines that define safe and effective service standards, including those provided by bodies such as the:
- British Association of Perinatal Medicine ( BAPM) [20]
- Royal Colleges
- National Institute for Clinical Excellence ( NICE) [21]
- Scottish Intercollegiate Guidelines Network ( SIGN) [22]
There is a broad range of ongoing audit and improvement activity which aims to improve clinical standards and outcomes across Scotland:
- The Maternal and Children's Quality Improvement Collaborative [23] ( MCQIC): was established in 2013 as a part of the Scottish Patient Safety Programme [24] .
- The Stillbirth Group - established in 2011, aims to reduce the rate of stillbirth in Scotland by raising awareness of risk, commissioning research, and promoting bereavement support and information.
- Mothers and Babies: Reducing Risk through Audits and Confidential Enquiries in the UK ( MBRRACE) - established in 2013, it investigates maternal deaths, stillbirths and infant deaths with the aim of providing information to secure continuous quality improvement.
- The National Neonatal Audit Programme [25] ( NNAP) - audits whether babies requiring neonatal care are receiving consistent, high quality care across the United Kingdom.
- The Royal College of Obstetricians and Gynaecologists ( RCOG) Each Baby Counts [26] programme which aims to reduce the number of avoidable harmful incidents occurring during term labour.
- UNICEF UK [27] audits of Baby Friendly Initiative ( BFI) [28] standards in maternity and neonatal units.
- The Royal College of Midwives Better Births Initiative [29] .
In addition, there are a number of other audits and review tools that are currently being developed and progressed in Scotland. These include:
- The National Maternity and Perinatal Audit [30]
- this audit will evaluate the UK quality of maternity and newborn care, and will be launched in 2017. - The Standardised Perinatal Mortality Review Tool
- the aim of this programme is to develop a tool to standardise review processes across the UK.
The tool is expected to launch in 2017.
2.6.2 Breastfeeding support
All maternity units in Scotland are UNICEF Baby Friendly Initiative ( BFI) accredited. Scotland's four largest neonatal units are near to full implementation of the neonatal BFI standards, and other units are working towards implementation. A Scotland-wide donor milk bank was launched in 2013 to provide equitable access to breast milk for the smallest and sickest infants across Scotland.
2.6.3 Perinatal mental health
The Scottish Government's new Mental Health Strategy, which will be published in early 2017, will set out shared priorities for action on perinatal mental health.