2015 Review of Public Health in Scotland: Strengthening the Function and re-focusing action for a healthier Scotland
The Public Health Review was asked to examine public health systems and functions and their contribution to improving population health and reducing (health) inequalities. This is the Report on behalf of the Review Group published with a Ministerial foreword from the Minister for Public Health
Part 1. Background, Context and Resources
Introduction
1. Scottish Ministers announced in November 2014 that they had asked for a review of Public Health in Scotland and had established a Review Group to take this forward and report back in 2015. The purpose of the review was to consider the role of the public health function in the context of the emerging policy landscape and current and future public health challenges, and to recommend how the function could be strengthened to respond more effectively to the opportunities and challenges.
2. There were a number of areas specifically identified for inclusion within the review and these formed part of the terms of reference agreed between Ministers and the group (Annex A). The group was asked to examine public health leadership and influence, both within the health sector and more widely, and to recommend how these could be developed further to deliver maximum impact. A second consideration concerned how public health featured in community planning and health and social care integration, and how the potential of partnership opportunities could be used to maximise the successful implementation of public health measures. The third area was workforce - workforce planning and development, succession planning and resourcing.
3. In establishing the review, Ministers sought recommendations that would strengthen the contribution of Public Health in Scotland; maximise the effectiveness and efficiency of the public health resource; achieve consistency where this would enhance quality and impact; and ensure the responsiveness and resilience of the public health function for the future.
4. The Review Group was convened in December 2014, under the chairmanship of Dr Hamish Wilson, with membership as listed in Annex B, and supported by a secretariat from within the Scottish Government. The review process (see Annex C) incorporated: analysis of population health in Scotland; stakeholder engagement through written responses and workshops; research analysis; and meetings with specific stakeholders.
5. The material described in Part 1 of this report reflects the population health and policy analysis undertaken to inform the recommendations and ensure these are made on the basis of a good understanding of public health. Part 2 of the report describes the key themes emerging from the engagement processes undertaken by the review, and the additional research evidence commissioned around the specific areas of public health leadership, partnership and workforce. The Review Group's recommendations take account of material described in both Part 1 and Part 2.
Public Health
6. Public health is the science and art of promoting and protecting health and wellbeing, preventing ill-health and prolonging life through the organised efforts of society. Some key features help to distinguish a public health approach from other approaches to improving health and wellbeing, such as those delivered through personalised health and care. Based on the definitions used by the Faculty of Public Health, we can describe public health as:
a. Being population based - concerned with the factors that make populations (e.g. communities, cities, regions, countries) healthier or unhealthier;
b. Emphasising collective responsibility for health, its protection and disease prevention - through the organised efforts of society;
c. Recognising the role of the state, and of the underlying socio-economic and wider determinants of health and disease, including the distribution of power, resources and opportunities within and across populations; and
d. Involving partnership with those who contribute to the health of current and future populations.
7. Professionals from medical, dental and other non-medical backgrounds train to become specialists in public health. This training involves competence in nine key areas (Table 1) relating to the three domains of public health practice - namely health protection, health improvement, and improving health services. Public health data analysis and intelligence provide a foundation for these three domains of practice.
Table 1 Core and Defined Competency Areas of Public Health Practice[1]:
| Competency Area | |
|---|---|
| 1 | Surveillance and assessment of the population's health and wellbeing. |
| 2 | Assessing the evidence of effectiveness of interventions, programmes and services intended to improve the health or wellbeing of individuals or populations. |
| 3 | Policy and strategy development, and implementation. |
| 4 | Strategic leadership and collaborative working for health. |
| 5 | Health improvement. |
| 6 | Health protection. |
| 7 | Health and social service quality. |
| 8 | Public health intelligence. |
| 9 | Academic public health. |
8. Health protection involves: immunisation programme effectiveness; ensuring the safety and quality of food, water, air and the general environment; preventing the transmission of communicable diseases; and managing outbreaks and the other incidents which threaten the public's health.
9. Health improvement incorporates a broad set of activities to create the circumstances for better health and reduced health inequalities within populations. It includes attention to: prevailing cultures and values; the health impact of policies and programmes across the wider determinants of health (housing, employment, transport, poverty, etc.); behaviour-change interventions; and support for community-led action to improve health.
10. Improving health services supports the planning and development of services to ensure that they meet the needs of the populations they serve. Activities include needs assessment; support for inequalities-sensitive services; clinical governance; audit; and effectiveness. Screening services - such as those to detect changes indicative of specific health problems including cervical cancer, breast cancer and bowel cancer - are also part of the public health contribution to health services.
11. Public health intelligence underpins all of the above three domains of public health practice. It includes the surveillance and monitoring of population health and the determinants of health and wellbeing; support for evidence-based practice; and assessment of the effectiveness of policies, programmes and services.
Population Health in Scotland
12. The nature and scale of the population health challenge changes over time, and each iteration takes longer to pass for the more deprived sections of the population than it does for the more affluent. During the 20th century life expectancy increased, communicable diseases became less common and better controlled, non-communicable disease became more prevalent, and an increasing proportion of people developed and lived with multiple morbidities. The burden of disease now lies with longer-term conditions and is associated with lifestyle, and the nature of wider social, economic and environmental factors in society. Scotland's health is also characterised by the years of life lost on account of deaths from 'external causes' such as suicide, violence, alcohol and drug-related mortality among young adults.
13. Some features of our population health in Scotland are particularly worthy of note:
i. We have lower life expectancy than our European counterparts, and there is no single explanation for this. On average people in Scotland die younger than in any other country in Western Europe, Scotland's life expectancy having increased more slowly than other European countries since the 1950s. Mortality rates in Scotland are higher than would be expected on the basis of population characteristics and levels of socio-economic deprivation. This phenomenon of 'excess mortality' is evident for Scotland as a whole, but is particularly concentrated in West Central Scotland.
ii. There are high levels of preventable mortality and morbidity in Scotland's ageing population. According to the UK Global Burden of Disease Study (Murray, 2010) the leading risk factors for disease are: tobacco and second hand smoke, high blood pressure, high body mass index, physical inactivity and low physical activity, alcohol use and poor diet. Underpinning these risk factors is a complex picture of economic, social, biological and environmental factors which influence behaviours and outcomes.
iii. Continued increases in the levels of overweight and obesity in the population have the potential to overturn the life expectancy gains achieved through behavioural and health service responses to heart disease and diabetes in recent decades. At present over 64% of the adult population in Scotland is overweight or obese (27% obese). In comparison with other Organisation for Economic Co-operation and Development (OECD) member states (Scotland, UK and 15 other nations) Scotland ranks fifth highest for overweight (including obesity) and sixth highest for obesity alone. At school entry just under 23% of children are at risk of overweight and obesity (with 10% at risk of obesity). Prevalence increases with age up to age 75. On the surface the rate of increase in obesity is slowing, however this masks the now-evident socio-economic inequalities, particularly marked for children.
iv. Health inequalities persist across a range of outcomes, including the marked difference in the number of years people live in good health between our most and least deprived citizens. There is a clear relationship between deprivation (however measured) and population health. Our more deprived citizens live shorter lives and more years in poor health. Moreover, the greatest health benefits from services, programmes and opportunities often fall to the more affluent. Tackling health inequalities is a matter of social justice, and involves actions that operate across the whole social gradient, as well as those tailored to the needs of the most vulnerable and 'at risk' groups (Marmot, 2010).
v. We have high levels of multi-morbidity - in particular concurrent physical and mental health conditions. A striking (and increasing) number of people are living with multiple conditions impacting on their health, wellbeing and ability to function. Mental illness is associated with a 15 year reduced life expectancy compared to the general population, mainly due to cardiovascular disease. Multi-morbidity is also associated with multiple medication and dependence on a range of health and social care services, including unpaid and informal caring. The ageing population contributes to this trend, yet many younger people are also living with multiple conditions, signalling a future challenge. The onset of multi-morbidity occurs 10-15 years earlier in people living in the most deprived compared with the most affluent areas of the country, and deprivation is particularly associated with multi-morbidity that includes mental health conditions. There are concerns too for the mental wellbeing of Scotland's unpaid carers. Mental wellbeing decreases as the number of hours spent caring increases. The number of hours spent caring is highest in deprived areas.
vi. Despite improvements in a number of dimensions of mental health, considerable challenges remain. Mental health problems are common and greatly affect life chances. Social inequalities in mental health are enduring and persistent. The UK Mental Health Foundation estimates that 1 in 4 people will experience a diagnosable mental health problem each year: source Office for National Statistics Psychiatric Morbidity Report (Singleton, Bumpstead, O'Brien, Lee, & Meltzer, 2001). The World Health Organisation (WHO) estimates 40% of the European disability burden is due to chronic mental ill health (World Health Organisation, 2001). Despite the ongoing reduction in suicide rates (overall and in terms of inequality), suicide is the leading cause of death in Scotland among people aged 15-34 years and is strongly related to deprivation. There is concern about the increasing prevalence of suicide among middle aged men (suicides in Scotland is most common among men aged 35 to 55). The incidence of dementia is also rising, reflecting efforts to increase awareness and improve diagnosis, and also associated with population ageing.
vii. Despite considerable improvements in dental health, marked inequalities still exist. Dental decay is the single most common cause for children being admitted to hospital for a general anaesthetic in Scotland and presents a particular burden for the most deprived groups. As a result of major effort there is no gradient in dental registration between the most and least deprived areas.
14. In summary, specific population health priorities in Scotland encompass health inequalities and their societal determinants, inactivity, nutrition, obesity, and poor mental wellbeing, concurrent with the demography of an ageing population. There are therefore pressing public health challenges at every level: ongoing challenges to support the shift towards prevention; to protect the health of the population and address risk factors; complex social, economic and cultural challenges; and new threats to health and wellbeing. The difficulty for public health is to combine focussed action on clear current priorities alongside wider system influence and 'holism' (it all matters). The overall challenge is to increase the years of life that people in Scotland live in good health - Healthy Life Expectancy (HLE) - and to reduce the inequalities in health that exist in Scotland.
15. Public Health has recognised that new population-based approaches are now needed, giving rise to the concept of a fifth wave of public health (Hanlon, Carlisle, Hannah, Reilly, & Lyon, 2011). Looking historically (Table 2) (Hanlon, Carlisle, Hannah, Reilly, & Lyon, 2011) and (Davies et al, 2014) the first wave of public health was associated with great structural work such as the provision of clean water to urban areas. The second wave saw the emergence of medicine as science. The third wave was characterised by the redesign of social institutions (including the establishment of the NHS and the welfare state) and the role of everyday life and lifestyles on our health was explored. The fourth wave has been dominated by recognition of the influence of social determinants. The best of what these previous four waves can achieve needs to be preserved. However, it is argued that a different approach - a fifth wave of public health - is needed in the 21st Century (Hanlon, Carlisle, Hannah, Reilly, & Lyon, 2011) (Davies et al, 2014) to address modern phenomena and epidemics. This approach would differ radically from its forerunners. It is likely to be characterised by enabling government, greater interdependence and co-operation across sectors and geographies, and involvement of the public more individually and personally in improving and maintaining their own health. Davies argues that a fifth wave which is 'cultural' in character is inevitable - essentially a society where healthy behaviours are the norm, supported by the physical, social and economic environment.
Table 2 Making the case for a 'fifth wave' in public health (Davies et al, 2014)
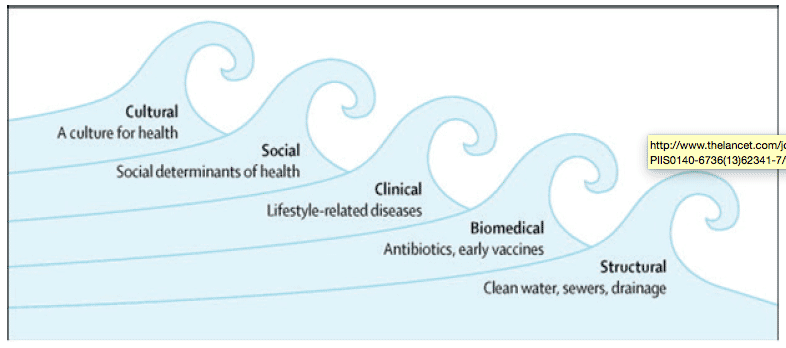
http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(13)62341-7/fulltext?_eventId=login
Policy context
16. In considering the future arrangements for Public Health in Scotland, the Review Group recognised the need for the public health function to align with and support the wider policy landscape and to be effective in helping to address current and future resource, sustainability, service and demographic challenges. There is an opportunity for the core public health workforce to be more directly influential, as well as being instrumental in advocacy and support for others in delivering public health outcomes.
17. The influential work of the Christie Commission on the Future Delivery of Public Services in Scotland (Christie, June 2011), which reported in 2011, highlighted, among other things, the need for public services to shift their focus more significantly towards prevention and to operate more effectively in partnership (including with the communities they serve).
18. The current priorities of the Scottish Government, reflected in the Programme for Government 2015-6 (The Scottish Government, 2015), combine an economic strategy centred on delivering inclusive growth; a clear and consistent focus on tackling inequalities; and a commitment to protecting and reforming public services.
19. Scotland's Economic Strategy (The Scottish Government, 2015) recognises that more equal societies form the foundation for more sustainable and resilient economies. Social and economic policy goals are integrated within the strategy, for example in its emphasis on Fair Work; education, skills and health; place and regional cohesion; and tackling cross-generational inequality. As well as recognising that a more equally healthy and skilled country is necessary, the strategy seeks to support a fairer distribution of economic and social benefit across the population.
20. In 2015 the Scottish Government also took forward a public discussion on what a Fairer Scotland would look like in 2030 and the actions that would be needed to make that a reality. This process involved public dialogues in a range of formats, considering policy priorities for tackling inequalities. Health inequality was a central part of this conversation.
21. The Parliament's Health and Sport Committee report in January 2015, and the subsequent Scottish Parliament debate on health inequalities, demonstrated cross-party political support for reducing inequalities and underlined the wider context for Public Health in influencing others to take action to address the social and wealth inequalities that drive health inequalities.
22. The Community Empowerment (Scotland) Act (2015) made provisions for a required focus on reducing socio-economic inequalities in relation to local and national outcomes, opening-up possibilities for greater power and decision-making at local levels. It seeks to ensure that individuals and communities are empowered and able to influence decisions, priorities and service delivery. This builds on the recognition of the contribution of Local Government in delivering local services responsive to need, providing enabling conditions for community wellbeing, and working in partnership to deliver priority outcomes.
23. Local Government is an essential partner with Scottish Government in public service reform. Public service reform in Scotland has included reinforcement of the important role for Community Planning Partnerships (CPPs), with shared ownership of priorities set out in Local Outcome Improvement Plans (LOIPs). CPPs provide the basis and potential for real collaborative working and leadership and influence to achieve effective public health measures through a whole systems approach at the level of Local Authorities and communities.
24. Greater integration of services is also being achieved by bringing together health and social care through the creation of Integration Joint Boards (IJBs). Together with NHS Boards and Local Authorities, these IJBs are required to demonstrate their contribution to tackling health inequalities and improving healthy life expectancy. Contributing processes include more joined-up working and budgets; a greater focus on prevention and population-based health improvement; and person-centred care.
25. During 2015-16 the Scottish Government is building on its 2020 Vision for Health with a national conversation on the future of health and social care to help shape a transformational change in Scotland's approach to population health and the delivery of health and social care services by 2030. The narrative for this national conversation includes a focus on prevention, with more effort, creativity and resources going into stopping issues of ill health before they occur, and with individuals and communities being responsible for promoting, and being empowered to manage, their own health and wellbeing.
26. In summary, new ways of working; a focus on inequality; a demonstrable shift to preventative approaches; and community empowerment are all prominent features of the language of public services and Government in Scotland, seeking innovative and effective ways to respond to increasingly constrained resources and growing demands and expectations. These policies offer opportunities for improved population health, and also require a more equally healthy population for their delivery.
27. Annex D sets out the main policy and legislative developments relating specifically to Public Health in Scotland since the late 1990s. These demonstrate a continued emphasis on the role of services in preventing ill-health and improving and protecting the public's health and well-being. There are consistent messages, for example in relation to the importance of early years and the need for health impacts to be taken into account in all areas of policy. Public health core work has drawn on a wide evidence base and developed into a very broad set of issues and programmes of action.
28. The current Review of Public Health in Scotland considers how the public health function can develop further and how it can provide leadership and action in partnership with others to increase its effectiveness in shaping policy and responding to the current and emerging population health challenges facing Scotland.
Public health capability and capacity
29. The organisational landscape within which the public health function in Scotland is structured is described in Annex E. This summarises the organisational responsibilities at national, regional and local levels, and the partnerships within which public health needs to operate to be effective. What follows is a description of the public health workforce and the capacity of the function within Scotland.
1. Core workforce
30. Public health is a multidisciplinary specialty in the UK, currently overseen by three Regulators: the General Medical Council (GMC), General Dental Council (GDC) and the UK Public Health Register (UKPHR). The UKPHR is responsible for regulating and keeping a register of accredited Public Health Specialists from disciplines other than medicine and dentistry.
31. There are three categories of specialists from disciplines other than medicine and dentistry in Scotland registered or aspiring to registration with UKPHR: generalist specialists trained through the conventional route, generalist specialists by portfolio and defined specialists by portfolio. The UK-wide Faculty of Public Health training scheme is expected to be the only future training route for all specialists, but does not provide the opportunity for NHS staff to train within current roles or for staff within other structures (e.g. local authority, third sector) to train.
32. A Public Health Skills and Knowledge Framework has also been developed and is overseen by the Public Health Online Resource for Carers, Skills and Training (PHorCast). Its purpose is to define skills required for public health in the broadest terms for employing organisations and practitioners to look at skills development and career pathways for the whole range of disciplines in public health, and to create pathways running from entry level to specialist level. NHS Education for Scotland (NES) and Health Protection Scotland (HPS) jointly sponsor work to promote the development of the health protection workforce. This includes implementation of the 'Framework for Workforce Education Development for Health Protection in Scotland' (NES /HPS) (from 2006) which is currently being reviewed.
33. Environmental Health in Scotland is a graduate only profession with Environmental Health Officers (EHOs) holding a degree level qualification awarded by a Royal Environmental Health Institute of Scotland (REHIS) accredited university. In addition, EHOs must also hold a Post Graduate Diploma in environmental Health awarded by REHIS before practicing as an EHO in Scotland.
34. The Centre for Workforce Intelligence (CfWI) was commissioned by NHS Health Scotland (NHSHS) on behalf of Scottish Government to carry out a mapping of the core public health workforce in Scotland. The approach taken was based on CfWI's similar workforce mapping exercise in England in October 2014. The CfWI has defined the core public health workforce as: "All staff engaged in public health activities that identify public health as being the primary part of their role."
35. There are some limitations of the data used in the report due to tight timescales for conducting the work. Data were collected from different sources and at different times. The report therefore provides an impression of scale and distribution of the public health workforce (see Table 3) rather than an accurate enumeration.
Table 3: Summary of the core public health workforce in Scotland (2015) (Centre for Workforce Intelligence, 2015)
| Role | Summary description | Estimated numbers (headcount) | |
|---|---|---|---|
| 1 | Public health and dental public health consultants, specialists and specialist trainees | Work at a strategic or senior management level or at senior level of scientific expertise to influence the health of entire communities | 189 |
| 2 | Directors of Public Health (DsPH) | Responsible for determining overall vision and objectives for public health both within local Health Boards (14) and national Health Boards (4) [these are also included within Public Health consultants above] |
[18] |
| 3 | Public health academics | Lecturers, researchers and teachers employed in higher education, whose primary focus is public health | 360 |
| 4 | Public health managers and practitioners | Work across the system and at all levels delivering public health programmes in health improvement, e.g. smoking cessation, alcohol dependency | 970 |
| 5 | Public health scientists | Perform scientific role in support of public health objectives | 50 |
| 6 | Intelligence and knowledge professionals | Staff employed in data analysis, informatics and presentation of public health information | 370 to 660 |
| 7 | Health visitors | Work as part of a primary healthcare team, assessing the health needs of individuals, families and the wider community | 2,185 |
| 8 | School nurses | Nurses who advise and support pupils within schools on preventing illness and remaining healthy | 500 |
| 9 | Public health nurses (excluding health visitors and school nurses which are listed separately) |
Nurses who advise people in the community on preventing illness and remaining healthy. Work mostly in health protection, e.g. TB, infection prevention and control, HIV | 640 |
| 10 | Environmental health professionals | Work in improving, monitoring and enforcing public and environmental health standards. Environmental health officers are core to the delivery of health protection in Scotland, including the joint health protection team. | 980 |
| Total | 6,250 to 6,540 | ||
36. Taking roles 1 to 6 and 10 from Table 3 as comprising the core specialist public health workforce in Scotland yields a headcount estimate of approximately 3000. Half of these - at least 1515 staff - work in the NHS (Table 4). A significant number of academic staff (at least 360) contribute to the core public health function from posts out with the NHS. Environmental Health Professionals make up 980 posts in the core specialist public health workforce - the majority working within Local Authority environmental health departments. In addition, a number of EHOs work within other statutory organisations such as the Scottish Environmental Protection Agency (SEPA) and the Health and Safety Executive (HSE). Some work within the NHS and others in private industry or the voluntary (third) sector.
37. Looking at the data further, Table 4 shows that, of the 1515 NHS staff, approximately 25% work within National Boards and 75% within Territorial Boards. The majority of public health and dental public health consultants, specialists, specialist trainees and public health practitioners work in Territorial Boards; and a significant proportion (75%) of intelligence and knowledge professionals work in the National Boards (estimated as 215 within National Services Scotland (NSS), 30 in Healthcare Improvement Scotland (HIS) and 20 in NHSHS, excluding the Scottish Public Health Observatory (ScotPHO) staff). The CfWI report notes (CfWI table 9 (Centre for Workforce Intelligence, 2015) that a further 400 to 500 staff in analytical roles (not recorded as core public health) work within Public Health Intelligence in NSS.
38. Table 4 Information in CfWI report on workforce within Territorial and National Boards (2015) (Centre for Workforce Intelligence, 2015) source Table 4, 5, 7, 8 and 9 of CfWI report
| Role | Territorial Board (WTE) | National Board (WTE) | Total NHS |
Other (WTE) |
Sum Territorial+ National + Other |
|
|---|---|---|---|---|---|---|
| 1 | Public health and dental public health consultants, specialists and specialist trainees | 145 (103.6) |
16 (12.9) |
161 (116.5) |
28* |
189 |
| 2 | Directors of Public Health (DsPH) | [14] | [4] Equivalent status |
18 | [18] | |
| 4 | Public health managers and practitioners | 895 (785) |
76 (45) |
971 (830) |
971 | |
| 5 | Public health scientists | 35 (in HPS) |
35 | 20** | 55 | |
| 6 | Intelligence and knowledge professionals | 83 (at least) |
265 (at least) |
348 (at least) |
26*** | 374 |
| Total | 1,123 | 392 | 1515 | 74 | 1589 |
[ ] DsPH have also been counted as Public Health consultants or specialists
*28 UKPHR defined generalist or defined specialists working for Territorial Boards and National Boards in senior posts not formally appointed as consultants
** Public Health England (PHE) staff working in Scotland at the Centre for Radiation Chemical and Environmental Hazards at Glasgow
*** ScotPHO staff
39. The report does not attempt to estimate the number of staff working in each of the public health domains. It instead refers to earlier work by ScotPHN, published in 2011, which identified 128 whole time equivalents as Consultants in Public Health employed in Scotland in February 2010, of whom 82% were Consultants in Public Health Medicine or Dental Public Health. A summary breakdown of their areas of focus indicated that:
- Around half of Territorial Health Board consultants had generic roles, while a quarter focused on health protection, a fifth on health and social care services and a sixth on health improvement.
- All but two of the 14 Territorial Health Boards had dedicated provision for health protection, but only about half had similarly dedicated consultant-level resource for health improvement and health and social care services.
- There was expert provision nationally at consultant level for health protection, health improvement and health intelligence, but none for health and social care services.
40. Most Boards have access to dental public health consultants, but over the years posts have been difficult to fill and some have been shared across Board boundaries.
2. Wider public health workforce
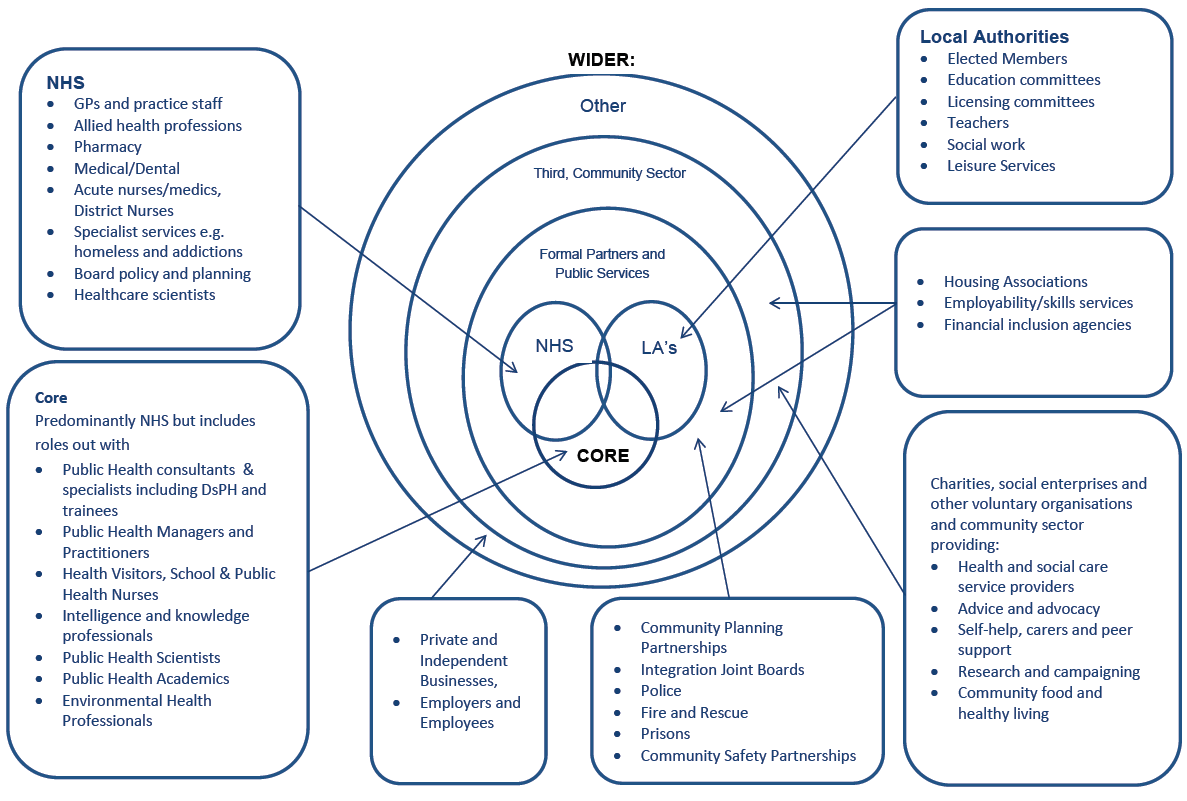
41. In addition to the core public health workforce, many other professional groups, practitioners in different disciplines, organisations and individuals make an essential contribution to protecting and improving the public's health and wellbeing. There is almost no limit to the range of groups and organisations whose staff fall into this category. Examples include: medicine; nursing; pharmacy; dentistry; allied health professions; police; fire and rescue services; teachers; social work and social care; licensing officers; welfare rights; housing; transport; planning; employability and leisure services; voluntary and community sector organisations (some focussed explicitly on health issues, such as community food and health initiatives and mental health projects; others contributing through action on wider influences on health, such as poverty and greenspace); and services located in government, scrutiny or private sector bodies, including those ensuring healthy and safe working environments; responsible for travel infrastructure; or setting welfare system parameters. Collectively these comprise the wider public health function. They clearly represent a considerable human resource, some of the potential of which remains to be realised.
42. The Scottish Health Promotion Managers' Group (SHPM) described Public Health engagement with the wider workforce as "principally driven by an acknowledged shared common agenda that is not always defined by traditional health outcomes but will include outcomes known to contribute to positive health outcomes such as educational attainment; financial inclusion; community resilience etc. The pursuit of such outcomes is a function of public health. The wider workforce includes both statutory partners/players with responsibilities defined in legislation (e.g. Community Safety Partnerships) as well as voluntary sector / charitable agencies whose contribution to health outcomes is determined by organisational constitutions and governance structures (e.g. Charities). Additionally the wider workforce may contain individuals and community activators or action groups with specific aligned motivations. All of these players should be recognised as legitimate and valued partners."
Table 5 Core and Wider Public Health Workforce
3. Resource Cost
43. In this report we have derived an estimate of core public health workforce costs. This estimate recognises the uncertainties associated with the staff numbers, uses available data sources to estimate salaries, and includes assumptions on staff grades and number of working time equivalents[2]. It is therefore presented as an indicative calculation for illustrative purposes. An estimate of staff costs associated with the core public health workforce, as defined by the CfWI, yields approximate workforce costs of £227 million per annum. This estimate includes NHS and non-NHS staff.
44. The estimate for the core public health function workforce (roles 1&2, 3,4,5,6 and 10, in Table 6) is approximately £126 million. The best estimate of NHS-funded core public health function workforce costs (roles 1&2, 4, 5 and 6, in Table 6) is £74 million. In the context of wider NHS workforce costs of £5.6 billion per annum, the public health function workforce (£74 m) equates to around 1.3%[3] .
Table 6 Core Public Health Function resource costs (source: Scottish Government analysts)
| Role | Estimated headcount from Table 3 | Estimate (staff cost £m) |
|
|---|---|---|---|
| 1 & 2 | Public health and dental public health consultants, specialists and specialist trainees includes role (2) DPHs | 189 | 17 |
| 3 | Public health academics | 360 | 20 |
| 4 | Public health managers and practitioners | 970 | 33 |
| 5 | Public health scientists | 50 | 2 |
| 6 | Intelligence and knowledge professionals | 370 to 660 | 14 to 30 |
| 7 | Health visitors | 2,185 | 68 |
| 8 | School nurses | 500 | 11 |
| 9 | Public health nurses (excluding health visitors and school nurses which are listed separately) |
640 | 22 |
| 10 | Environmental health professionals | 980 | 32 |
| Total Core Public Health as defined by CfWI | 6,250 to 6,540 | £219m to £235m Midpoint £227m |
Effective and resilient Public Health: capacity and cost-effectiveness
45. The OECD predicts that the cost of health care will double by 2050 based on current trends. A substantial proportion of costs are associated with health issues that may be reduced through effective population-based actions. For example, obesity accounts for 1-3% of total health expenditure in most countries; mental illness costs the economy £110 billion per year in the UK and represents 10.8% of the health service budget; the costs of health inequalities, in terms of total welfare loss, are estimated at 9.4% of GDP. Health and social care services alone cannot create the conditions required for a healthy, flourishing population. Moreover, the National Institute for Health and Care Excellence (NICE) has shown that many public health interventions are more cost-effective than clinical interventions (using cost per QALY) and some are even cost-saving (Kelly, 2012).
46. The case for investing in public health has recently been summarised by the WHO Europe (WHO, 2014). Recognising the significant and unsustainable increases in costs associated with ill-health, this report describes the economic and health benefits of taking a public health approach. It sets out the costs associated with failing to address current public health challenges, summarises evidence on the cost-effectiveness of public health approaches, and outlines the returns on investment achieved through delivery of preventive interventions.
47. It is estimated (WHO, 2014) that only 3% (range 0.6 - 8.2%) of national health sector budgets is currently spent on public health. Individual-level approaches cost five times more than interventions at the population level and, in general, investing in upstream population-based prevention is more effective at reducing health inequalities than more downstream prevention.
48. In Scotland we do not routinely estimate the total expenditure on public health. Within the Scottish Government Health Budget spend under the heading Improving Health and Better Public Health in Table 4.03 is an estimated £313.6 million in 2015/16 including £73.5 million for the Integration Fund[4]. This includes expenditure on immunisation of £20.9 million, central allocation of £40.09 million to tackle alcohol misuse and £55.6 million on health improvement and health inequalities. In addition a proportion of the expenditure of NHS Boards and National Boards in Table 4.02 of the Scottish Draft Budget 2015-16 (£9.47 billion) will be on public health departments and to support public health outcomes, and is at the discretion of Boards. The 2015/16 budget sees health resource spending increase by £409 million and takes total health spending to over £12 billion for the first time. While we cannot give an estimate of the percentage of public health expenditure, it will be a significant sum in its own right but a relatively small percentage of overall NHS spend. Improving Health and Better Public Health amounts to 2.6% of the total £12 billion NHS expenditure[5] .
49. At the heart of this current Review of Public Health in Scotland is the need to ensure that this expenditure delivers maximum value for money. This will require a public health function which is resilient, has the right capability and capacity, and is directed at those activities where it can make the most impact.
50. A resilient and effective public health infrastructure ensures that the core functions can continue to be delivered in light of new public health priorities, emergent challenges and changing contexts. Dimensions of public health capacity that should be considered in this regard are summarised in Table 7. There is also the need for strategic resilience within public health to sustain the capacity and the relationships within health protection to manage outbreaks and public health incidents. The skills and competencies need to be maintained and the capability to escalate and sustain a response needs to be assured.
Table 7: Dimensions of public health capacity ( Aluttis et al, 2014)
| Dimension | Description |
|---|---|
| Organisational structures | The infrastructural ability of a system to contribute to goals of public health |
| Resources | The allocation and provision of human and financial resources necessary to carry out public health activities |
| Partnerships | Collaboration between organisations for effective public health practice |
| Workforce | Qualified human resources with sufficient skills and knowledge; availability of training options |
| Knowledge development | The knowledge base that provides information on the health of the population and that supports evidence-based public health policy and interventions at all levels |
| Leadership and governance | The ability and willingness of governments to improve public health by developing and implementing effective public health policies and by expressing qualities in leaderships and strategic thinking |
| Country specific context | The political context and other characteristics of a country that may have an influence on public health policies and capacity building efforts |
51. In assessing where a public health function can make most impact there has been recent work in Scotland and internationally exploring the cost-effectiveness of population health interventions. Best preventative investments for Scotland - what the evidence and experts say (NHS Health Scotland, 2014) examined available evidence (which it stated was limited but growing) coupled with expert opinion to identify the best investments for preventing poor health, reducing 'failure demand' and narrowing health inequalities. In its summary it stated that "in general, prevention 'upstream', addressing the economic, social and environmental causes of health inequalities, is cost-effective. It is more likely to reduce health inequalities than either treatment of illness or 'downstream' measures to change behaviours delivered to individuals". ScotPHO has also modelled estimates of the impact of some interventions on health and health inequalities (The Scottish Public Health Observatory, 2014).
52. An international study ACE - Assessing Cost-Effectiveness in Prevention (University of Queensland and Deakin University, Melbourne., 2010), conducted in Australia, reviewed the cost-effectiveness of 150 preventive health interventions, addressing areas such as mental health, diabetes, tobacco use, alcohol use, nutrition, body weight, physical activity, blood pressure, blood cholesterol and bone mineral density. The largest impact on the health of the population arose from regulatory and tax measures. Other cost-effective measures included many screening programmes and immunisation and drug and alcohol treatment programmes, smoking cessation and preventative measures to improve mental health.
53. WHO has shown a wide range of preventive approaches to be cost-effective (WHO, 2014), including those that address environmental and social determinants of health (e.g. promoting walking and cycling, safer transport, green spaces, healthy employment), promote resilience (e.g. improving mental health and reducing violence), and support healthy behaviours (e.g. tobacco and alcohol legislation, reducing dietary salt and sugar, increasing physical activity, nursery toothbrushing), as well as vaccination and screening.
54. Focussing on the implementation of approaches, additional messages from previous UK reviews have emphasised the importance of population engagement with health issues (the 'fully engaged' scenario) to achieving a shift to prevention and the delivery of cost-effective interventions (Wanless, 2002 and 2004) and of taking action across the whole social gradient, not just with some segments in society, in order to reduce health inequalities (Marmot, 2010).
55. Two recent reviews have considered the focus of Scotland's approach to tackling health inequalities and how current resources are used: NHSHS's Health Inequalities Policy Review (Health Scotland, 2013) and Audit Scotland's 2012 report on health inequalities in Scotland (Audit Scotland, 2012). The latter focused on how resources are allocated and on delivery mechanisms through Primary Care, CPPs and NHS Boards, reporting that the Scottish Government allocated an estimated £1.8 billion over the three financial years from 2008/9 - 2010/11 for issues related to health inequalities. Although these two reports focus differently on the approaches taken in Scotland - the former being more concerned with the policy content, the latter with governance, resource allocation and delivery mechanisms - both sets of recommendations suggest the need for a clearer focus on population health in Scotland, greater coordination across structures and levels of action, and the need for partnership-based action informed by public health intelligence and evidence.
56. The subject matter of these recent reviews - addressing health inequalities - reflects the ongoing need to make progress on that issue. In a number of other areas of public health Scotland is recognised as being at the leading edge. The leadership shown on tobacco control; the government's commitment to tackling the price and availability of alcohol; the quality, uptake and effectiveness of our childhood immunisation programmes; the considerable improvements in oral health; the drop in violent crime achieved as a result of the country's focus on violence reduction and safer communities; and the investment being made to ensure that Scotland's children have a good start in life - all of these, and many other examples, illustrate public health achievements delivered through 'the organised efforts of society' for Scotland.
57. In each case, there has been bold, committed, leadership with local and national political support; effective partnership working; an applied evidence-base; clear accountability and monitoring processes; a critical mass of effort and investment; and action at national, regional and local levels.
Contact
Email: Gareth Brown