Understanding the patterns of use, motives, and harms of new psychoactive substances in Scotland
This report presents the results of mixed methods research on new psychoactive substance use.
2. Methods
This mixed-methods research was carried out between December 2015 and July 2016. Qualitative interviews and focus groups were used to identify key themes and concerns about motives and consequences of NPS use. This informed the design of two surveys, one exploring issues with those who use NPS in Scotland, and another aimed at staff working in services, where they may encounter people who have taken NPS. Models to estimate prevalence were explored using the survey data, data from the Scottish Drug Misuse Database ( SDMD) and the analysis of needle exchange data from existing Neo360 data sets for Glasgow and Lothian.
2.1 Ethics and Research Governance Permissions
Ethical approval for this project was given by the NHS West of Scotland Research Ethics Committee (15/ WS/2010). Research and Development (R&D) approval was granted for all 14 territorial health boards except Forth Valley for qualitative data collection, and all 14 territorial health boards for survey data collection. Pseudonyms have been used throughout for interview participants.
2.2 Prevalence Estimates
When attempting to quantify the number of people in a population that use drugs we have recourse to a number of different methods. [26] Traditionally, surveys based on random sampling have been used to give information on the extent of drug use among the general population, for example the Scottish Crime and Justice Survey ( SCJS). However there are limitations to this approach, particularly when trying to assess patterns of drug use amongst vulnerable populations.
Other approaches to estimate 'hidden' groups that may not be picked up in survey data (such as capture-recapture) have been used in Scotland to estimate national and local prevalence of problem opioid and benzodiazepine use. This approach uses multiple data sources to estimate the size of the hidden population of problem opioid and benzodiazepines users [27] , although estimates to date do not include problematic use of other substances such as cocaine. There are several challenges posed in estimating NPS use in this way. Recording of data on NPS within existing routine datasets is currently limited [28] . This is the case not just within Scotland, but across Europe and internationally, where the systematic collection of data on NPS in healthcare settings is scarce [29] . This means that sufficient numbers of NPS users do not appear in existing data sources to make a multi-source method such as capture-recapture viable.
In light of these challenges, the approach adopted for this study was to explore the multiplier method. We also estimated the number of injecting NPS users in two NHS areas: NHS Greater Glasgow & Clyde and NHS Lothian.
2.2.1 Multiplier Method
The multiplier method is a simple way of estimating unknown populations such as prevalence of drug use. The method uses the available information on the population in question as a benchmark, e.g. number of drug users in treatment, and applies a multiplier that is related to the population and has normally been derived from a small-scale study. For this study, this method involved using the number of NPS users from our quantitative ' NPS survey' who reported contact with drug treatment services. From this a multiplier was calculated and used in combination with the numbers of NPS users in treatment from the Scottish Drug Misuse Database ( SDMD). This provides data on the total number of people in Scotland who presented for initial assessment at drug treatment services.
The construction of the treatment multiplier used the 125 NPS users identified in the quantitative survey in contact with drug treatment services. 194 NPS survey participants answered this question giving a treatment rate of 64%. This was then used in combination with data from ISD on treatment numbers for 2014/15 to produce an estimate.
However, this estimate was not considered to provide a sufficiently robust prevalence figure for NPS use in this population. The analysis demonstrated that data sets were not sufficiently complete and too many assumptions had to be made. One major limitation of the SDMD data is it collects data on new treatment episodes and there is very limited follow up data available. In addition, the data from SDMD referred to both Mephedrone and 'other' drug users. It is unclear what drugs this 'other' category includes and it may not be mainly other NPS users. This adds to the uncertainty around the estimate and impacts on its robustness. More details on the calculation are provided in Appendix B.
2.2.2 Estimating the prevalence of injecting NPS takers using NEO data
For this estimation, data from pharmacies/needle exchange services in both areas were used and an estimate of the hidden population was made by examining the frequency of visits to the needle exchange by NPS injectors. Further information on the methods applied can be found in the technical report (see Appendix A).
2.3 Qualitative data
Qualitative data were collected from interviews with people who have taken NPS, as well as from focus groups with staff working in services likely to come into contact with NPS users.
Purposive sampling was used in recruitment for both interviews and focus groups as the aim of the qualitative component of the research was not to create a representative sample of people who had taken or worked with people who have taken NPS, but to ensure a diverse range of views to enhance the understanding of NPS use amongst vulnerable groups.
2.3.1 Interviews: Recruitment and Sampling
Purposive sampling was used to recruit 33 people who had taken NPS (self-defined) for interviews, including participants from both urban and rural areas, and men and women. In addition, participants were purposively recruited from the following groups:
- Vulnerable young people (aged 16-24) [30]
- People in contact with mental health services (formerly or currently in contact)
- People who inject drugs ( PWID)
- Adult homeless people (current or formerly homeless)
- Men who have sex with men ( MSM)
Participants were recruited for interview by circulating information to managers, lead contacts in Alcohol and Drug Partnerships ( ADPs), Managed Care Networks ( MCN), statutory and third sector settings, and across all Scottish health boards except NHS Forth Valley [31] . Potential participants were invited to make contact with a researcher by posters placed in service waiting rooms or where appropriate by being given the information by their key worker. Researchers also attended drop-in services where people were offered the opportunity to opt in to the study directly through the researcher who attended on the day. See Appendix C for a full list of interview participants.
2.3.2 Interviews: Data Collection
In-depth interviews were undertaken with 33 people who identified themselves as having taken NPS, from nine Scottish Health Boards. Around two thirds of participants were recruited from Ayrshire and Arran, Greater Glasgow and Clyde and Lothian, with smaller numbers from Dumfries and Galloway, Fife, Grampian, Highlands, Lanarkshire, and Tayside.
In line with findings from current research on people with drug dependencies [32] , almost half (48%) of interviewees belonged to two or more of the target groups. For example, many injecting drug users were also in contact with mental health services.
20 (61%) participants were men, and 13 (39%) participants were women. As one of the target groups was MSM, this increased the size of the male sample. The mean age was 32 (range: 16-61).
Of the total, 20 (61%) reported they no longer took NPS at the time of interview. No participant reported having taken NPS only. That is, all reported having, at some time, taken illegal or more traditional drugs.
Interviews addressed circumstances of NPS use initiation, NPS knowledge and what they perceived to be positive and negative effects and consequences. Sources of support in relation to first use of NPS and most recent use of NPS were also addressed (see Appendix D for topic guides). Interviews lasted on average 45 minutes, and participants were given a £10 high street voucher to thank them for their contribution.
2.3.3 Focus Groups: Recruitment and Sampling
Purposive sampling was used to recruit 42 staff working with clients who use NPS, including participants from both urban and rural areas, drug and non-drug services (e.g. sexual and mental health services). Four focus groups were undertaken in NHS Lothian, NHS Greater Glasgow and Clyde, NHS Highland, and NHS Grampian, with front line workers from across these and other areas. Focus group participants were purposively sampled for geographical range and type of service represented. A full breakdown of regional information for focus group participants can be found in Appendix E.
Focus group participants were recruited by asking managers and lead contacts at ADPs, NHS, Social Work and third sector organisations to cascade an email invitation to front line workers. It was also cascaded through Scottish Drugs Forum membership list and advertised on national bulletins, newsletters and via social media. The study was advertised across Scotland in NHS, statutory and third sector settings, and across all Scottish health boards, excluding NHS Forth Valley.
2.3.4 Focus Groups: Data Collection
42 statutory and third sector service practitioners contributed to the focus group discussions. Almost half of participants were from drug services, with small numbers from vulnerable young people's services, needle exchange, mental health, sexual health, criminal justice, housing and homelessness and social work services. Some services catered to more than one group. The breakdown is described in table 2.1 overleaf.
Table 2.1 Focus group participants (service practitioners) and service type
| Service Type | N |
| Drugs | 20 |
| Vulnerable young people | 7 |
| Needle exchange | 6 |
| Mental health | 6 |
| Sexual health | 6 |
| Criminal justice | 6 |
| Housing and homelessness | 5 |
| Social work | 4 |
Focus groups lasted, on average, for 90 minutes. Focus group discussion covered participants' estimates of prevalence and trends, their understandings of why their clients take NPS and what distinguishes them from clients who do not, and the consequences of NPS use.
2.3.5 Analysis of qualitative data
All interviews and focus groups were transcribed verbatim, anonymised, and analysed using the qualitative analysis software Quirkos to generate themes within the three key areas: prevalence, motives and harms. Additional themes around service provision and the then-forthcoming Psychoactive Substance Act were also coded. These themes formed the basis of closed option responses in the survey, but were also separately analysed thematically for the qualitative analysis. [33]
2.4 Quantitative Data
Quantitative data were collected from two surveys. The first survey sought to explore NPS use in Scotland, specifically amongst the vulnerable populations listed in section 2.3.1 (the ' NPS survey'). The second survey gathered data from staff within services ('the 'Staff survey'). Over two thirds of staff survey respondents worked in services that provided drug and alcohol support, and around one third worked in services that provided mental health services or housing and homelessness services.
2.4.1 NPS Survey: Recruitment and Sampling
Two sampling strategies were used to recruit 545 participants within the five groups of interest. The first combined purposive sampling of drug and alcohol services for geographical range and urban and rural characteristics with convenience sampling (whereby everyone who entered the waiting room was approached to participate in the survey during data collection). In a small number of cases, it was preferred that that workers would bring clients to researchers in a separate space. Face to face surveys happened primarily in drug services, homeless drop-ins, needle exchange sites, and in some areas mental health wards and vulnerable young people's services. Overall, uptake in vulnerable young people's services was limited compared to other target groups. Services which had large drop-ins or waiting rooms were the most effective in terms of recruitment. As there were larger numbers of people attending, researchers could directly approach people using the drop in or who were waiting for appointments. A substantial number of approached services were unable to facilitate survey data collection due to short timescales, workload considerations, participation in Care Commission inspections, and perceived lack of interest from service users.
The second sampling strategy was targeted recruitment for hard-to-access groups such as MSM and people in rural areas where it was not possible to recruit by attending services in person e.g. in parts of the Highlands and Islands. This involved promotion of the survey online with additional targeted recruitment of MSM which took place through a peer researcher recruiting in gay bars, and via a banner advert on Grindr, an online dating 'app' used by MSM. The online version of the survey was promoted through the SDF news bulletin, through Facebook and Twitter accounts, and was also promoted by many key stakeholders on social media. This dual-approach strategy was selected to ensure wide coverage of target groups across Scotland.
2.4.2 NPS Survey: Data Collection
The survey was developed as an online survey, compatible with administration via a handheld tablet computer so it could be administered offline with support of a researcher. Peer researchers received information about NPS, and training in administering surveys, from SDF and the University of Glasgow prior to data collection. Where requested by services, a project team member supported clients in completing the survey in place of peer researchers.
The survey explored last 6 month drug use, including alcohol, NPS and 'traditional' drugs, and focused on motives and health consequences of use for NPS categories in terms of the seven drugs wheel categories [34] . In addition to this, based on findings from qualitative stage, mephedrone (commonly understood by interview participants to be NPS despite having been controlled since 2010), ethylphenidate (understood by some, particularly homeless, interview participants to be NPS), GHB/ GBL (commonly used in chemsex), salvia divinorum, and benzodiazepine-type NPS were also explored. Finally, participants were asked about relationships and social harms in relation to their NPS use overall. Their views on services and on the then-forthcoming Psychoactive Substances Act were also sought.
Ten SDF peer researchers [35] administered the survey, helping and supporting service users to fill it in using a tablet. This ensured literacy was not a barrier to participation and that someone was able to brief people on the survey. It also ensured participants' consent, gave the opportunity to answer any questions about the study, and allowed for signposting to additional support where necessary. Peer researchers approached people in service waiting areas.
All participants in this survey were invited to provide contact details (recorded and stored separately from their survey responses) if they wished to be entered into a draw for a £100 high street voucher.
A total of 545 individuals were recruited to the NPS survey, which was completed by 424 participants (although not all participants responded to all questions). 59% (n=251) were recruited in treatment or service settings and 41% (n=173) online. [36]
The largest group represented were people who inject drugs ( PWID), totalling one third of all survey responses. There was significant overlap between the 'risk' groups which increased the size of the PWID sample. Vulnerable young people were the least represented in the sample, at 16%.
Table 2.2 overleaf presents an overview of the composition of the sample according to the target populations, and a breakdown by risk group of the 59% (n=252) of respondents who reported ever using NPS.
Table 2.2: Composition of respondents to NPS survey, by 'risk' group [37]
| |
All respondents | NPS users | ||
| Group | N | % | N | % |
| PWID | 141 | 33 | 136 | 54 |
| Mental health service users | 99 | 23 | 94 | 37 |
| Homeless | 92 | 22 | 76 | 30 |
| Vulnerable young people | 69 | 16 | 39 | 16 |
| MSM | 70 | 17 | 38 | 15 |
The survey respondents fell into a number of 'risk' group categories and highlighted the common issue that vulnerable populations often present with multiple issues and treatment needs. We tested whether contact with mental health services was independent of homelessness status, and of injecting status, and found that those accessing mental health services were at a greater risk of being homeless [38] , and of being PWID [39] , than those not accessing mental health services. Similarly, we tested whether homelessness status was associated with injecting status, and found that those who were homeless were more likely to be PWID [40] than those who were not homeless.
Respondents had a mean age of 36.7 (range 16-66). NPS users were slightly younger than the rest of the sample (average age of 35, compared to average age of 39). The overall sample was two thirds (66%) male, 73% male for NPS users. This is consistent with existing research that people who have used NPS tend to be younger, and tend to be predominantly male [41] .
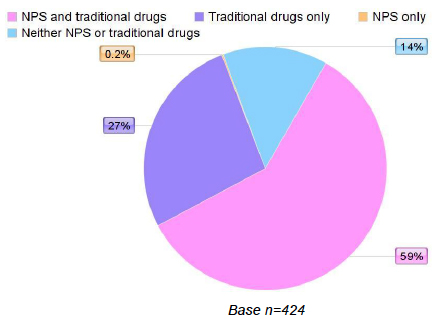
Figure 2.1. gives the breakdown of all drug use from the whole sample who completed the survey n=424.
Fig. 2.1 Reported drug use by survey respondents
2.4.3 Staff Survey: Recruitment and Sampling
The survey was developed as an online survey and checked it was accessible from different NHS and council systems. Managers of NHS, statutory and voluntary sector services across all 14 Scottish Health Boards were contacted regarding the staff survey, and asked to cascade an invitation email and link to the survey web URL to front line workers.
2.4.4 Staff Survey: Data Collection
Staff surveys were completed by 184 respondents within 13 Health Boards. Table 2.3 below presents the breakdown of services offered by the organisation which staff respondents come from. Staff respondents often worked in organisations where more than one service type was offered. 70% of respondents worked in drug and alcohol services, and around one third in mental health services or in housing support. Please note, as some workers offer services across two or more of these categories, these percentages will not total 100.
Table 2.3: Services provided by organisations of staff survey respondents
| Service Type | N | % |
| Drug & alcohol support | 128 | 70 |
| Mental health services | 61 | 33 |
| Housing and homelessness support | 56 | 30 |
| Sexual health services | 44 | 24 |
| Needle exchange | 39 | 21 |
| Specialist support services[42] | 13 | 7 |
| Other | 41 | 22 |
Table 2.4 presents a breakdown of the client groups that staff respondents work with. Due to the services provided, service providers tended to encounter several different types of client groups. Four-fifths of staff worked with people with mental health issues, and over 70% worked with homeless clients or injecting drug users.
Table 2 .4 Client groups that staff survey respondents work with
| Client Group | N | % |
| People with mental health issues | 154 | 84 |
| Homeless people | 136 | 74 |
| People who inject drugs ( PWID) | 132 | 72 |
| Vulnerable young people | 82 | 45 |
| Men who have sex with men ( MSM) | 56 | 30 |
| I do not work with any of these groups | 2 | 1 |
2.4.5 Analysis of survey data
The survey data were analysed using SPSS ( IBM SPSS Statistics 22). The descriptive analysis of the sample was carried out using frequency tables and cross tabulations with chi-squared tests performed to ascertain statistical significance. Where differences are statistically significant, this is reported in the text.
As previously stated, there were 424 respondents to the NPS survey, and 184 respondents to the staff survey. Not all participants completed all questions, and thus the data presented within this report should be interpreted in light of this.
It was also found that respondents who were a young person or an MSM were less likely to overlap with the other three 'risk' groups. In particular, vulnerable young people were less likely to also be a PWID, and MSM were less likely to be homeless.