Scottish Inpatient Experience Survey 2016 Volume 1: National Results
Report detailing the results from the Scottish Inpatient Experience Survey 2016.
Executive Summary
Background
Over 17,000 people took part in the fifth national Inpatient Experience Survey. The survey included a range of questions covering topics such as accident and emergency, care and treatment, staff, leaving hospital and care and support at home.
People reporting similar positive experiences
Overall, people reported a similarly positive experience to the previous survey, with 'overall' ratings improving or staying the same for all but two sections of the survey (leaving hospital and care and support services after leaving hospital) (Figure 1).
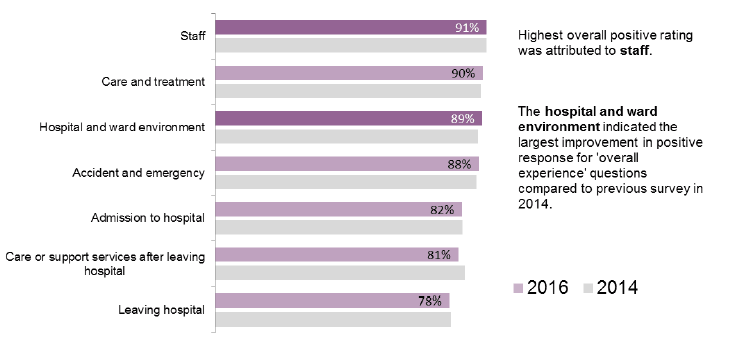
Figure 1 Positive response for 'Overall experience' questions
(%)
Improvement in experiences of care and treatment in A&E
People were more positive about the overall care and treatment they received in A&E than the previous survey. However, the results show that more could be done to keep patients informed about the length of time to be seen by nursing or medical staff in A&E: 23 per cent of people were not kept informed about how long they would have to wait.
People reported a similar positive experience to the previous survey for the overall admission to hospital experience.
People rate the hospital and ward environment more positively
There was significant improvement in peoples' rating of the overall ward and hospital environment, with improvements also being seen for ward cleanliness. Nevertheless, a sizeable proportion of people still were not aware which nurse was in charge of the ward, found the food and drink unacceptable or who found noise at night to be problematic.
Encouraging results for staff
As in the previous survey, staff received the highest overall rating of all survey sections.
The statements that received the most positive findings for staff related to confidence and trust in the doctors and nurses treating them ( 92 per cent and 91 per cent positive respectively) and whether doctors and nurses washed their hands at appropriate times ( 91 per cent and 93 per cent positive respectively).
Results for the three questions regarding help from staff: washing and dressing; going to the bathroom/toilet; and eating and drinking were all fairly positive and were similar to those seen for the previous survey in 2014. Although people were typically more positive about the staff that they did encounter, around one in ten respondents ( nine per cent) felt that there were 'rarely or never' enough nurses to treat them and over a quarter ( 27 per cent) did not know which nurse was in charge of their care.
Leaving hospital the lowest ranked section
As in previous surveys, peoples' departure from hospital continues to be viewed less positively than other aspects of their patient experience. Whilst still reasonably high ( 78 per cent positive), this area has the lowest overall rating of the aspects of care covered in the survey.
One potential explanation for the low relative rating may come from the finding that delays appear to be a problem for people: two in five ( 40 per cent) felt that they were delayed on the day that they left hospital with 47 per cent experiencing delays of up to two hours. The most common reason for this was a delay in getting medication, which accounted for 56 per cent of delays.
Wait for care and support services after leaving hospital
In general, people were less positive than the previous surveys regarding care and support services. One in six ( 17 per cent) indicated that they stayed in hospital longer than expected to wait for the care and support to be organised, this was a rise of three percentage points.
However around nine in ten people ( 88 per cent) felt that the care and support services they received after leaving hospital were right for them.
Patient safety
The survey found that one in five people ( 20 per cent) felt that they had experienced harm or injury relating to their inpatient care such as infections, bed sores, reactions to medications, or falls.
Eight per cent of people felt that they had experienced a clinical error during their stay in hospital, the most common being 'delayed or incorrect test results'.
The survey results further suggested that where people felt that clinical errors occurred, they were not always dealt with to their satisfaction. In over a third of instances ( 35 per cent), people reported that staff did not discuss the error with them and in 41 per cent of cases people were not satisfied with how the errors were dealt with.
The survey found that one in 12 people felt that either: their drip was not checked regularly enough; their drip was not changed when required; or their drip was not removed quickly enough.
In all these patient safety matters it is worth noting that these results reflect the perceptions of the patient and are not formal assessments from health professionals.
Person Centred Care
Collectively, the findings relating to aspects of person-centred care were mixed. People were positive about everyday aspects of person-centred care such as the way staff treated and listed to them, and the explanations provided about their care and treatment.
However, the results suggest that more could be done to take account of what matters to the person and involve them, and those that matter to them, in decisions about their care and treatment.
Board and hospital results available
The results presented in this publication focus on the national
picture. Reports for individual
NHS boards and
hospitals are available at:
www.careexperience.scot.nhs.uk/Results2016.html
Contact
Email: Nicola Kerr, nicola.kerr2@gov.scot