Scottish Health Survey 2012 - volume 1: main report
Scottish Health Survey 2012 - main report
7 Obesity
Linsay Gray and Alastair H Leyland
Summary
- In 2012, over a quarter (27.1%) of adults aged 16 or above were obese (body mass index (BMI) of 30 kg/m2 or above). Almost two-thirds (64.3%) were either overweight or obese (BMI of 25 kg/m2 or above).
- While men were significantly more likely than women to be overweight or obese (68.2% compared with 60.4%) in 2012, obesity prevalence among both genders was similar (26.6% and 27.5% respectively).
- The mean BMI for both men and women in 2012 was 27.3 kg/m2.
- Since 1995 there has been a significant increase in the proportion of adults aged 16 to 64 categorised as obese (from 17.2% in 1995 to 26.1% in 2012), although the level has remained fairly constant since 2008. Over the same period, the proportion who were overweight or obese increased from 52.4% to 61.9%, again showing some stability in recent years.
- The mean BMI of adults aged 16 to 64 increased from 25.8 kg/m2 in 1995 to 27.1 kg/m2 in 2012, with little change since 2008.
- Obesity prevalence increased with age among adults. In 2012, 9.9% of those aged 16-24 were obese; levels peaked at 36.4% of those aged 55-64, falling to 26.6% of those aged 75 and over. Overweight or obesity prevalence followed a similar age-related pattern, increasing from 33.9% of those aged 16-24, to 77.0% of those aged 65-74.
- In 2012, two-thirds (67.5%) of children aged 2 to 15 had a healthy weight (BMI >2nd percentile and < 85th percentile). Girls were more likely than boys to have a healthy weight (70.3% compared with 64.9%). Those aged 12-15 were least likely to be of healthy weight (59.5% of boys and 60.9% of girls).
- The proportion of girls falling within the healthy weight range has remained fairly stable since 1998. Among boys, there has been more variation over this period, although the proportion in the healthy weight range in 2012 (64.9%) was similar to that seen in 2003 (64.7%).
- In 2012 one in six (16.8%) of children were at risk of obesity (at or above the 95th percentile), with a further 13.8% at risk of overweight (at or above the 85th percentile, and below the 95th).
- Boys were at greater risk of being overweight (including obese) than girls in 2012 (33.6% compared with 27.4%). Boys were also more likely than girls to be at risk of obesity (19.7% compared with 13.7%). Children aged 12-15 were most likely to be at risk of obesity (26.1% of boys and 18.3% of girls).
- The proportion of boys at risk of obesity rose from 14.5% in 1998 to 19.7% in 2012. For girls, the proportion at risk was highest in 2009 (15.9%), and fell to close to the 1998 level in 2012 (13.7%).
- Less than 2% of children were at risk of underweight (at or below the second percentile) in 2012, with girls slightly more likely to be at risk than boys (2.3% compared with 1.4%). Older children (aged 12-15) were at greatest risk of being underweight (2.5% of boys and 5.2% of girls).
7.1 Introduction
Obesity has a major impact on quality of life and health across the lifecourse. Overweight and obese children have an increased risk of conditions such as hypertension, type 2 diabetes and asthma[126,127], in childhood, and if their weight continues to be unhealthy into adulthood they face an increased risk of numerous conditions associated with adult obesity, such as cardiovascular disease, osteoarthritis and cancer."[128,129,130] There is also evidence suggesting a link between overweight and obesity in midlife and dementia in old age."[131,132,133]
Scotland has one of the worst obesity records among developed countries. The estimated cost of obesity and related illnesses to the NHS in Scotland was in excess of £175 million in 2007/8[134]. With these economic and health costs, tackling obesity is a key priority for the public health sector in Scotland.
Each year, in addition to updating the obesity trends, the Scottish Health Survey (SHeS) annual report provides a broad overview of recent policy initiatives and developments relating to obesity. Recent developments include:
- The Scottish Government's Healthy Eating, Active Living: An action plan to improve diet, increase physical activity and tackle obesity[135].
- The Keep Well initiative[136].
- The Scottish Government's Obesity Route Map for tackling obesity and the associated Obesity Route Map Action Plan, published in 2011[137]. SHeS is the measurement tool for seven of the Route Map indicators, including the following long-term goals: the majority of Scotland's adult population in normal weight throughout life; fewer children in Scotland overweight or obese[138].
- The Scottish Intercollegiate Guidelines Network (SIGN) national clinical guidelines on obesity management[129].129
- The revised Scottish Government National Performance Framework indicators: 'increase the proportion of babies with a healthy birth weight'[139] and 'increase the proportion of healthy weight children'[140] - with the latter of these measured via SHeS.
- The NHS Scotland HEAT[141] target to deliver 14,910 child healthy weight interventions over the three years ending March 2014 (with at least 40% of such interventions delivered to children living in the two most deprived SIMD quintiles)[142]. 5,232 interventions were delivered between April 2011 and March 2012, and a further 4,951 by March 2013.
- The inclusion of child obesity rates as one of the national mental health indicators for children and young people in Scotland: 'percentage of children aged 2 to 15 with a body mass index (BMI) at or above the 95th percentile of the 1990 UK reference data)'[143].
In addition to these developments, many of the policy actions specifically targeted at improving diet (described in Chapter 5) and physical activity (described in Chapter 6) in the population are also relevant in the context of tackling obesity.
This chapter focuses on BMI, derived from the direct measurements of height and weight taken in the main SHeS interview. Trends in adult and child BMI are presented by sex. BMI prevalence of both adults and children in 2012 is also presented by age and sex. Waist measurements for a random sub-sample of adults are also being collected by interviewers in the 2012-2015 period; results of these will be presented in the 2013 report when two years' data have accumulated.
Future reports will present more detailed analyses of BMI data, for example by updating the tables on disease risk, and socio-economic factors, presented in the 2011 report.
7.2 Methods And Definitions
Full details of the protocols for carrying out height and weight measurements are included in Volume 2 of this report and are briefly summarised here.
7.2.1 Height
Height was measured using a portable stadiometer with a sliding head plate, a base plate and three connecting rods marked with a metric measuring scale. Participants were asked to remove shoes. One measurement was taken, with the participant stretching to the maximum height and the head positioned in the Frankfort plane[144]. The reading was recorded to the nearest even millimetre.
7.2.2 Weight
Weight was measured using Soehnle and Tanita electronic scales with a digital display. Participants were asked to remove shoes and any bulky clothing. A single measurement was recorded to the nearest 100g. Participants aged under 2 years, or who were pregnant, or chairbound, or unsteady on their feet were not weighed. Participants who weighed more than 130 kg were asked for an estimate of their weight because the scales are inaccurate above this level. These estimated weights were included in the analysis.
In the analysis of height and weight, data from those who were considered by the interviewer to have unreliable measurements, for example those who had excessive clothing on, were excluded.
7.2.3 Body Mass Index (BMI)
The Body Mass Index (BMI), defined as weight (kg)/square of height (m2), is a widely accepted measure that allows for differences in weight due to height. It has been used in each SHeS report to date BMI has, however, some limitations[145,146]., It does not distinguish between mass due to body fat and mass due to muscular physique. Nor does it take account of the distribution of fat.
BMI was calculated for all those participants for whom a valid height and weight measurement was recorded.
BMI classification: adults
Adult participants were classified into the following BMI groups:[147]
| BMI (kg/m2) | Description |
|---|---|
| Less than 18.5 | Underweight |
| 18.5 to less than 25 | Normal |
| 25 to less than 30 | Overweight, excluding obese |
| 30 to less than 40 | Obese, excluding morbidly obese |
| 40+ | Morbidly obese |
Other cut-off points can be used in analyses of obesity, for example, the World Health Organisation (WHO) cites evidence that chronic disease is an increasing risk in populations when BMI exceeds 21[148], while mortality rates do not necessarily correlate neatly with the categories presented here[149]. However, meaningful comparisons of prevalence estimates between countries require agreed thresholds and these categories correspond with the WHO's recommended definitions for underweight, normal, overweight and obese (though the WHO use three sub-classifications of obesity rather than the two presented here)[150].
Mean BMI prevalence for the five categories outlined in the table above are presented by age and sex in the tables. Although obesity has the greatest ill-health and mortality consequences, overweight is also a major public health concern, not least because overweight people are at high risk of becoming obese. Being underweight can also have negative health consequences. Three measures are presented in trend tables: the proportion either overweight or obese (BMI of 25 kg/m2 or more), the proportion who are obese (BMI of 30 kg/m2 or more), and the proportion morbidly obese (BMI of 40 kg/m2 or more). The latter group are at particularly high risk of morbidity and mortality[151].
BMI classification: children
BMI for children is defined in the same way as it is for adults: weight (kg)/square of height (m2). However, despite the relatively wide acceptance of the use of BMI as an adiposity indicator, the establishment of a specific obesity and overweight classification system for children and young people has proved to be difficult. Constant changes in body composition during growth mean that the relationship between weight-for-height and adiposity during childhood and adolescence is age-dependent, and this relationship is further complicated by both ethnicity and gender[152]. Several methods have been employed to define early life overweight and obesity, including body fatness as measured by skinfold thickness,[153,154], national BMI percentile charts,[155,156,157] weight-for-height indices[158], BMI percentile cut-off points[159], and international[160] and national[161] BMI cut-off points.
Percentile charts can be used to compare an individual child's BMI with the distribution of BMI in a reference population to see whether it corresponds with the average or is unusually high or low. Since a child's BMI changes as he or she ages, comparisons need to be age specific. For example, the BMI for a child aged 5 needs to be compared with a reference population for a large sample of 5 year olds rather than a sample of children with a wider age range.
The classification of children's BMI used in this chapter, set out below, has been derived from BMI percentiles of the UK 1990 reference curves[156,157] (referred to as the national BMI percentiles classification); these have been used in each SHeS to date. SIGN recommends that these reference curves and thresholds should be used for population surveillance in Scotland[129].
The use of reference curves require children's ages to be exactly matched to those in the reference population charts. This is a fairly straightforward process in clinical settings where an individual child's exact age can be compared with the look-up chart for their age. Matching exact ages to population charts in a survey dataset containing many children is somewhat less straightforward. SHeS uses a method developed by ISD Scotland that plots the exact ages of the children in the sample against the reference population data[162].
Although children's exact age was used to calculate the BMI grouping prevalence rates (based on the interview date and the date of birth), the results are presented using grouped ages based on age at last birthday.
The 85th / 95th percentile cut-off points are commonly accepted thresholds used to analyse overweight and obesity in children. These thresholds have previously been used to describe childhood overweight and obesity prevalence trends in the UK[163,164,165,166]. The national BMI percentiles classification has been shown to be reasonably sensitive (i.e. not classifying obese children as non-obese) and specific (i.e. not classifying non-obese children as obese)[167,168]. As noted in the introduction, one of the Scottish Government's national indicators relates to healthy weight in children, defined as neither underweight nor overweight or obese[140]. For this reason, the data have been categorised to show the total proportions that are: healthy weight, at risk of overweight, at risk of obesity, and at risk of underweight.
A number of changes have been made to the presentation of child BMI data since the publication of the 2011 annual report. These are as follows:
- The threshold used to differentiate between underweight and healthy weight has been revised from the 5th percentile to the 2nd percentile.
- The description of the weight categories has changed in line with recommendations in a joint statement released by the Scientific Advisory Committee on Nutrition (SACN) and the Royal College of Paediatrics and Child Health (RCPCH) in April 2012[169].
- Minor methodological changes have been made in relation to rounding.
- The approach to excluding BMI values at the extreme ends of the distribution has changed. To minimise the impact of error in either the height or weight measurements affecting the BMI data, ISD Scotland recommends excluding cases with BMI values at the extreme ends of the distribution. The data presented in the 2008-2011 SHeS annual reports defined such cases as more than three standard deviations above or below the mean for all children. In 2012, ISD revised the definition for this range to exclude a smaller number of cases (above or below seven standard deviations from the mean)[170]. The increase in child obesity since the reference curves were derived means that some of the previously excluded cases were likely to have been valid BMIs rather than erroneous measures. All time-trend figures for child BMI presented in this chapter have been re-run using the revised exclusion definition.
| Percentile cut-off | Description |
|---|---|
| At or below 2nd percentile | At risk of underweight |
| Above 2nd percentile and below 85th percentile | Healthy weight |
| At or above 85th percentile and below 95th percentile | At risk of overweight |
| At or above 95th percentile | At risk of obesity |
The impact of these changes can be seen by comparing the 1998 to 2011 figures in Table 7.3 with those in Table 5.2 in the 2011 report (Volume 2)[171]. The general effect is an approximate 2 percentage point increase in the proportion of boys categorised as being at risk of obesity in each of the years, a 1.5 percentage point increase in the proportion categorised as at risk of overweight, and a 1 percentage point increase in the proportion outwith the healthy weight range. There was an approximate 1 percentage point increase in the proportion of girls who were at risk of being overweight or obese, and a slight decrease in the proportion outwith the healthy range.
7.3 Trends In Adult Overweight And Obesity Prevalence Since 1995
7.3.1 Obesity and morbid obesity
Since older adults were excluded from the survey in earlier years, the trend figures presented for 1995 onwards are for adults aged 16 to 64 only. The figures for all aged 16 and over are shown from 2003 onwards. Obesity prevalence (BMI ≥ 30 kg/m2) has increased significantly, by around nine percentage points, since 1995, from 17.2%, to 26.1% in 2012. The rapid increase observed between 1995 and 2003 (23.0%), however, does not appear to have been sustained in more recent years, with the proportion of adults categorised as obese fluctuating between 25.7% and 27.4% between 2008 and 2012. Obesity prevalence among all adults (aged 16 and over) has followed a similar pattern to this since 2003. Trends in male and female obesity have followed a similar pattern over the years.
Morbid obesity prevalence (BMI ≥ 40 kg/m2) among men aged 16 to 64 increased from 0.5% in 1995 to 2.0% in 2012. The corresponding figures for women were consistently higher over this same period (1.3% in 1995 and 3.5% in 2012). Since 2003, the level of morbid obesity has remained at between 1.0% and 2.0% for all men aged 16 and over and between 3.2% and 4.1% for women. Figure 7A, Table 7.1
7.3.2 Overweight including obesity
Since 1995, the proportion of the population aged 16 to 64 categorised either as overweight or obese (BMI ≥ 25 kg/m2) has risen significantly from 52.4%, to 61.9% in 2012, an increase of almost 10 percentage points. As with the trend in obesity levels, the sharp increase in prevalence between 1995 and 2003 (60.6%) among both men and women has not been sustained in recent years. The proportion of 16 to 64 year olds who were overweight including obese has fluctuated between 61.9% and 63.3% since 2008 (61.9% in 2012).
Since 2003, the trend in the prevalence of overweight including obesity for all adults (aged 16 and over) has followed a similar pattern to that seen for 16 to 64 year olds. Figure 7A, Table 7.1
Figure 7A Prevalence of overweight and obese in adults 1995-2012 (age 16-64), 2003-2012 (age 16+)
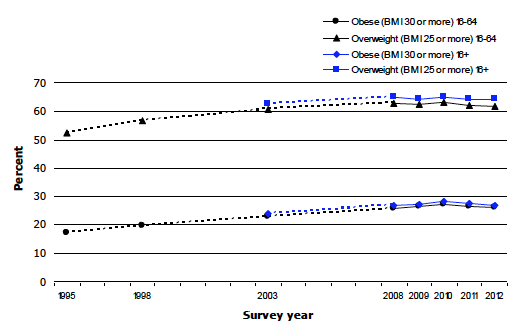
7.3.3 Mean BMI
The mean BMI for adults aged 16 to 64 rose from 25.8 kg/m2 in 1995 to 27.1 kg/m2 in 2012. The greatest increase occurred between 1995 and 2003 (26.9 kg/m2), with stability observed in more recent years. Since 2003, the mean BMI for all adults (aged 16 and over) has been similar to the mean for 16 to 64 year olds, fluctuating between 27.1 kg/m2 and 27.5 kg/m2 since then. Table 7.1
7.4 Adult BMI, 2012, By Age And Sex
In 2012, 27.1% of adults (aged 16 and above) in Scotland were obese (BMI ≥ 30 kg/m2) (Table 7.2). Obesity prevalence was similar among men and women (26.6% and 27.5% respectively).
Obesity levels were age-dependent for both men and women but with slightly different patterns. Among men, prevalence was lowest (8.8%) in the youngest age group (16-24 year olds). In line with the pattern seen in earlier years of the survey, prevalence then increased with age up to age 65-74 (38.5%) but was lower for the age 75 and over group (29.5%). The pattern for women was less clear, with the lowest obesity prevalence observed in the youngest age group (11.3%) and the highest for 55-64 year olds (35.0%). Among the remaining age groups, the proportion classified as obese ranged between 24.5% and 32.2%.
Figure 7B Men: Prevalence of overweight and obese, 2012, by age
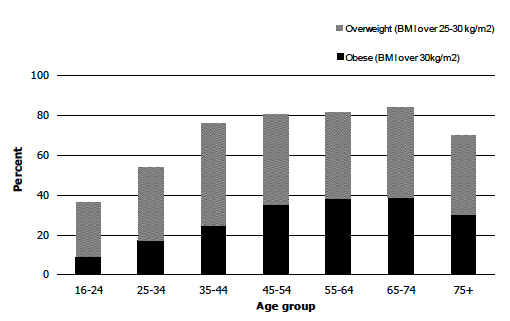
Figure 7C Women: Prevalence of overweight and obese, 2012, by age
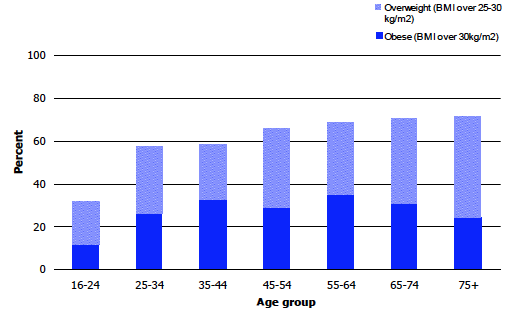
In 2012, almost two-thirds (64.3%) of adults were classified as overweight or obese (BMI ≥ 25 kg/m2). While there was no significant difference in obesity prevalence for men and women, men were more likely than women to be overweight including obese (68.2% compared with 60.4% of women).
As with obesity, prevalence of overweight including obese varied with age. Among men, the level was lowest among the youngest age group - 16-24 year olds (35.8%). Prevalence then increased with age, up to age 65-74 (84.2%), and was lower again for those aged 75 and over (70.0%). For women, overweight (including obesity) prevalence increased with age, rising from 31.5% of the youngest age group to 71.6% of those in the oldest age group.
In 2012, mean BMI was 27.3 kg/m2 for both men and women. In line with differences observed in overweight and obesity prevalence, mean BMI varied with age, being lowest for the youngest age group (24.0 kg/m2) and highest for those aged 55-64 (28.7 kg/m2) and 65-74 (28.6 kg/m2). Figure 7B, Figure 7C, Table 7.2
7.5 Trends In The Prevalence Of Child Healthy Weight, Overweight And Obesity Since 1998
The proportion of children aged 2 to 15 at risk of obesity rose from 14.3% to 16.6% between 1998 and 2008 but has remained stable since then (16.8% in 2012). Prevalence trends were slightly different for boys and girls. Among boys, the proportion at risk of obesity increased from 14.5% in 1998 to 19.7% in 2012, with some fluctuation between 2003 and 2010. Over time, the proportion of girls at risk of obesity has been more stable, fluctuating between 14.2% and 15.9% since 1998 (13.7% in 2012).
The proportion of 2 to 15 year olds at risk of overweight including obese rose from 29.1% in 1998 to 32.8% in 2008 but, since then, has fluctuated with no clear pattern (30.6% in 2012). Prevalence has changed somewhat for boys over the years but has been relatively stable for girls. Between 1998 and 2008 the proportion of boys at risk of overweight including obese progressively increased from 29.0% to 37.5%. The level then declined notably to 31.3% in 2009 and 32.9% in 2010; since then obesity prevalence in boys has been higher again at 36.2% in 2011 and 33.6% in 2012. Among girls, the proportion at risk of overweight including obese was 29.1% in 1998 and 27.4% in 2012 with similar rates observed in the interim years (ranging from 27.8% to 30.2%) and no statistically significant differences observed.
Healthy weight prevalence among children followed similar, but opposing, patterns to those described above for obesity and overweight (Figure 7D). In 1998, seven in ten (70.1%) children had a weight within the healthy range, decreasing to 66.2% in 2008, and then fluctuating between 69.1% and 67.5% between 2009 and 2012, with a low of 65.4% in 2011. Among boys, there was a sharp decrease in healthy weight prevalence between 1998 and 2008 (from 70.4% to 61.2%), with the level since then remaining similar to the level in 2008 (despite a large fluctuation in 2009). In 2012, almost two-thirds (64.9%) of boys were within the healthy weight range. For girls, the proportion falling within the healthy range was very similar across survey years, ranging between 68.4% and 71.5%, with prevalence at 70.3% in 2012. Figure 7D, Table 7.3
Figure 7D Percentage of children aged 2-15 with BMI in the healthy weight range, 1998- 2012, by sex
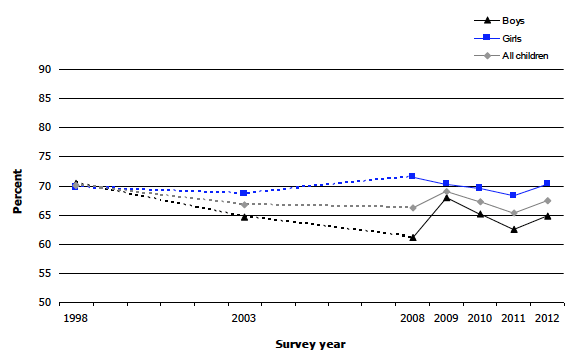
7.6 Child BMI Categories, 2012, By Age And Sex
This section focuses on 2012 prevalence for the three summary BMI groups discussed above (at risk of obesity; at risk of overweight including obese; and within healthy range). In addition, data for those at risk of underweight are also presented. Figures are presented by age and sex for children aged 2 to 15. The sample size for children is not sufficiently large to detect statistically significant differences between all of the sub-groups in individual survey years.
In 2012, one in six (16.8%) children (aged 2 to 15) was at risk of obesity. Prevalence was higher among boys (19.7%) than girls (13.7%). The proportion at risk of obesity increased with age, from 12.1% of those aged 2-6, to 22.5% of those aged 12-15.
Three in ten (30.6%) children were at risk of overweight including obese in 2012. The overall figure for boys (33.6%) was significantly higher than for girls (27.4%). Prevalence was highest among those aged 12-15 (36.1%). Boys' increased likelihood of being at risk of overweight including obese was true across all age groups but was particularly pronounced at age 2-6, with 32.7% classified as such, compared with 22.3% of girls.
Two thirds (67.5%) of children had a BMI within the healthy range in 2012, with girls significantly more likely than boys to be a healthy weight (70.3% compared with 64.9%). As with overweight and obese, healthy weight prevalence varied with age, with those aged 12-15 least likely to be a healthy weight (59.5% of boys of this age were a healthy weight, as were 60.9% of girls).
The group of children outwith the healthy range comprises those at risk of overweight, obese and underweight. At 1.9% in 2012, the proportion at risk of underweight was low among all children (1.4% of boys and 2.3% of girls). Prevalence varied by age group, particularly for girls (no girls aged 7-11 in the sample were at risk of being underweight, compared with 5.2% of girls aged 12-15). Table 7.4
Table list
Table 7.1 Mean adult BMI, prevalence of overweight and obesity, 1995 to 2012
Table 7.2 Adult BMI, 2012, by age and sex
Table 7.4 Children's BMI, 2012, by age and sex
Table 7.1 Mean adult BMI, prevalence of overweight and obesity, 1995 to 2012
| Aged 16 and over with valid height and weight measurements | 1995 to 2012 | |||||||
|---|---|---|---|---|---|---|---|---|
| BMI (kg/m2) | 1995 | 1998 | 2003 | 2008 | 2009 | 2010 | 2011 | 2012 |
| % | % | % | % | % | % | % | % | |
| Men | ||||||||
| 25 and overa | ||||||||
| 16-64 | 55.6 | 61.0 | 64.0 | 66.3 | 66.2 | 66.1 | 67.1 | 66.0 |
| 16+ | n/a | n/a | 65.4 | 68.5 | 67.9 | 67.8 | 69.2 | 68.2 |
| 30 and overb | ||||||||
| 16-64 | 15.9 | 18.8 | 22.0 | 24.9 | 26.7 | 26.6 | 26.7 | 24.8 |
| 16+ | n/a | n/a | 22.4 | 26.0 | 26.9 | 27.4 | 27.7 | 26.6 |
| 40 and overc | ||||||||
| 16-64 | 0.5 | 0.9 | 1.8 | 1.4 | 1.0 | 1.7 | 1.8 | 2.0 |
| 16+ | n/a | n/a | 1.6 | 1.4 | 1.0 | 1.6 | 1.7 | 2.0 |
| Mean | ||||||||
| 16-64 | 26.0 | 26.4 | 26.9 | 27.2 | 27.4 | 27.3 | 27.4 | 27.1 |
| 16+ | n/a | n/a | 27.0 | 27.4 | 27.5 | 27.5 | 27.6 | 27.3 |
| SE of the mean | ||||||||
| 16-64 | 0.07 | 0.07 | 0.12 | 0.13 | 0.13 | 0.15 | 0.14 | 0.16 |
| 16+ | n/a | n/a | 0.12 | 0.12 | 0.12 | 0.13 | 0.12 | 0.14 |
| Women | ||||||||
| 25 and overa | ||||||||
| 16-64 | 47.2 | 52.2 | 57.3 | 59.6 | 58.4 | 60.3 | 57.1 | 57.7 |
| 16+ | n/a | n/a | 59.7 | 61.8 | 61.0 | 62.4 | 59.6 | 60.4 |
| 30 and overb | ||||||||
| 16-64 | 17.3 | 20.9 | 23.8 | 26.5 | 26.4 | 28.1 | 26.3 | 27.4 |
| 16+ | n/a | n/a | 26.0 | 27.5 | 27.6 | 28.9 | 27.6 | 27.5 |
| 40 and overc | ||||||||
| 16-64 | 1.3 | 2.0 | 3.6 | 3.5 | 3.5 | 3.7 | 4.2 | 3.5 |
| 16+ | n/a | n/a | 3.4 | 3.4 | 3.5 | 3.2 | 4.1 | 3.2 |
| Mean | ||||||||
| 16-64 | 25.7 | 26.3 | 26.9 | 27.3 | 27.2 | 27.4 | 27.3 | 27.2 |
| 16+ | n/a | n/a | 27.2 | 27.4 | 27.4 | 27.6 | 27.5 | 27.3 |
| SE of the mean | ||||||||
| 16-64 | 0.08 | 0.09 | 0.14 | 0.15 | 0.14 | 0.14 | 0.14 | 0.16 |
| 16+ | n/a | n/a | 0.14 | 0.13 | 0.12 | 0.12 | 0.12 | 0.14 |
| All adults | ||||||||
| 25 and overa | ||||||||
| 16-64 | 52.4 | 56.7 | 60.6 | 62.9 | 62.4 | 63.3 | 62.2 | 61.9 |
| 16+ | n/a | n/a | 62.4 | 65.1 | 64.4 | 65.1 | 64.3 | 64.3 |
| 30 and overb | ||||||||
| 16-64 | 17.2 | 19.8 | 23.0 | 25.7 | 26.5 | 27.4 | 26.5 | 26.1 |
| 16+ | n/a | n/a | 24.2 | 26.8 | 27.2 | 28.2 | 27.7 | 27.1 |
| 40 and overc | ||||||||
| 16-64 | 1.2 | 1.4 | 2.7 | 2.5 | 2.2 | 2.7 | 3.0 | 2.7 |
| 16+ | n/a | n/a | 2.5 | 2.4 | 2.2 | 2.4 | 2.9 | 2.6 |
| Mean | ||||||||
| 16-64 | 25.8 | 26.4 | 26.9 | 27.2 | 27.3 | 27.4 | 27.3 | 27.1 |
| 16+ | n/a | n/a | 27.1 | 27.4 | 27.4 | 27.5 | 27.5 | 27.3 |
| SE of the mean | ||||||||
| 16-64 | 0.05 | 0.06 | 0.10 | 0.11 | 0.10 | 0.11 | 0.11 | 0.12 |
| 16+ | n/a | n/a | 0.09 | 0.10 | 0.09 | 0.10 | 0.10 | 0.11 |
| Bases (weighted): | ||||||||
| Men 16-64 | 3672 | 3673 | 2702 | 2238 | 2598 | 2487 | 2513 | 1706 |
| Men 16+ | n/a | n/a | 3217 | 2689 | 3129 | 2992 | 3003 | 2048 |
| Women 16-64 | 3632 | 3572 | 2776 | 2257 | 2553 | 2435 | 2478 | 1640 |
| Women 16+ | n/a | n/a | 3458 | 2828 | 3208 | 3046 | 3100 | 2063 |
| All adults 16-64 | 7757 | 7245 | 5478 | 4495 | 5151 | 4922 | 4991 | 3346 |
| All adults 16+ | n/a | n/a | 6675 | 5517 | 6336 | 6038 | 6103 | 4110 |
| Bases (unweighted): | ||||||||
| Men 16-64 | 3303 | 3110 | 2368 | 1822 | 2107 | 2020 | 2092 | 1381 |
| Men 16+ | n/a | n/a | 3016 | 2454 | 2817 | 2674 | 2745 | 1876 |
| Women 16-64 | 4005 | 3783 | 2908 | 2293 | 2678 | 2553 | 2596 | 1676 |
| Women 16+ | n/a | n/a | 3684 | 3019 | 3449 | 3327 | 3389 | 2221 |
| All adults 16-64 | 7776 | 6893 | 5276 | 4115 | 4785 | 4573 | 4688 | 3057 |
| All adults 16+ | n/a | n/a | 6700 | 5473 | 6266 | 6001 | 6134 | 4097 |
| a 25 and over = overweight / obese / morbidly obese | ||||||||
| b 30 and over = obese / morbidly obese | ||||||||
| c 40 and over = morbidly obese | ||||||||
Table 7.2 Adult BMI, 2012, by age and sex
| Aged 16 and over with valid height and weight measurements | 2012 | |||||||
|---|---|---|---|---|---|---|---|---|
| BMI (kg/m2) | Age | Total | ||||||
| 16-24 | 25-34 | 35-44 | 45-54 | 55-64 | 65-74 | 75+ | ||
| % | % | % | % | % | % | % | % | |
| Men | ||||||||
| Less than 18.5 | 6.6 | 2.3 | 0.2 | 0.6 | 0.4 | 0.5 | - | 1.7 |
| 18.5 to less than 25 | 57.6 | 43.8 | 24.0 | 18.7 | 18.1 | 15.3 | 30.0 | 30.2 |
| 25 to less than 30 | 27.0 | 36.9 | 51.0 | 45.9 | 43.7 | 45.6 | 40.4 | 41.6 |
| 30 to less than 40 | 8.8 | 16.1 | 21.9 | 31.7 | 34.8 | 35.7 | 29.4 | 24.6 |
| 40+ | - | 0.9 | 2.8 | 3.0 | 3.0 | 2.8 | 0.1 | 2.0 |
| All 25 and overa | 35.8 | 53.9 | 75.8 | 80.7 | 81.6 | 84.2 | 70.0 | 68.2 |
| All 30 and overb | 8.8 | 17.0 | 24.7 | 34.8 | 37.8 | 38.5 | 29.5 | 26.6 |
| Mean | 24.0 | 25.9 | 27.8 | 28.6 | 28.8 | 29.0 | 27.7 | 27.3 |
| Standard error of the mean | 0.38 | 0.35 | 0.30 | 0.28 | 0.30 | 0.26 | 0.39 | 0.14 |
| Women | ||||||||
| Less than 18.5 | 4.2 | 1.2 | 1.9 | 1.1 | 1.0 | 1.7 | 2.0 | 1.8 |
| 18.5 to less than 25 | 64.3 | 41.5 | 40.2 | 33.0 | 30.4 | 27.7 | 26.4 | 37.8 |
| 25 to less than 30 | 20.2 | 31.8 | 25.6 | 37.3 | 33.6 | 40.1 | 47.2 | 32.9 |
| 30 to less than 40 | 10.8 | 22.8 | 27.1 | 25.1 | 30.2 | 27.2 | 23.8 | 24.3 |
| 40+ | 0.5 | 2.7 | 5.2 | 3.5 | 4.8 | 3.3 | 0.7 | 3.2 |
| All 25 and overa | 31.5 | 57.3 | 57.9 | 65.9 | 68.6 | 70.6 | 71.6 | 60.4 |
| All 30 and overb | 11.3 | 25.5 | 32.2 | 28.6 | 35.0 | 30.5 | 24.5 | 27.5 |
| Mean | 24.1 | 27.1 | 27.7 | 27.7 | 28.6 | 28.1 | 27.6 | 27.3 |
| Standard error of the mean | 0.39 | 0.38 | 0.32 | 0.28 | 0.31 | 0.34 | 0.32 | 0.14 |
| All adults | ||||||||
| All 25 and overa | 33.9 | 55.5 | 66.5 | 73.2 | 75.0 | 77.0 | 71.0 | 64.3 |
| All 30 and overb | 9.9 | 21.0 | 28.6 | 31.7 | 36.4 | 34.3 | 26.6 | 27.1 |
| Mean | 24.0 | 26.4 | 27.7 | 28.2 | 28.7 | 28.6 | 27.6 | 27.3 |
| Standard error of the mean | 0.28 | 0.26 | 0.23 | 0.20 | 0.23 | 0.22 | 0.24 | 0.11 |
| Bases (weighted): | ||||||||
| Men | 321 | 345 | 342 | 380 | 318 | 215 | 126 | 2048 |
| Women | 255 | 306 | 367 | 387 | 325 | 241 | 182 | 2063 |
| All adults | 576 | 651 | 710 | 767 | 643 | 457 | 307 | 4110 |
| Bases (unweighted): | ||||||||
| Men | 162 | 211 | 315 | 374 | 319 | 332 | 163 | 1876 |
| Women | 184 | 269 | 419 | 429 | 375 | 322 | 223 | 2221 |
| All adults | 346 | 480 | 734 | 803 | 694 | 654 | 386 | 4097 |
| a 25 and over = overweight (including obese) | ||||||||
| b 30 and over = obese | ||||||||
Table 7.3 Proportion of children with BMI within the healthy range, and prevalence of overweight and obesity in children, 1998 to 2012
| Aged 2-15 with valid height and weight measurementsa | 1998 to 2012 | ||||||
|---|---|---|---|---|---|---|---|
| BMI status (National BMI percentiles) | 1998r | 2003r | 2008r | 2009r | 2010r | 2011r | 2012 |
| % | % | % | % | % | % | % | |
| Boys | |||||||
| Within healthy rangeb | 70.4 | 64.7 | 61.2 | 68.0 | 65.2 | 62.6 | 64.9 |
| Outwith healthy rangec | 29.6 | 35.3 | 38.8 | 32.0 | 34.8 | 37.4 | 35.1 |
| At risk of overweight (including obesity)d | 29.0 | 34.2 | 37.5 | 31.3 | 32.9 | 36.2 | 33.6 |
| At risk of obesitye | 14.5 | 17.6 | 18.7 | 17.0 | 17.8 | 19.7 | 19.7 |
| Girls | |||||||
| Within healthy rangeb | 69.7 | 68.7 | 71.5 | 70.3 | 69.5 | 68.4 | 70.3 |
| Outwith healthy rangec | 30.3 | 31.3 | 28.5 | 29.7 | 30.5 | 31.6 | 29.7 |
| At risk of overweight (including obesity)d | 29.1 | 30.2 | 27.8 | 28.9 | 29.6 | 29.1 | 27.4 |
| At risk of obesitye | 14.2 | 13.9 | 14.4 | 15.9 | 14.3 | 14.5 | 13.7 |
| All children | |||||||
| Within healthy rangeb | 70.1 | 66.7 | 66.2 | 69.1 | 67.3 | 65.4 | 67.5 |
| Outwith healthy rangec | 29.9 | 33.3 | 33.8 | 30.9 | 32.7 | 34.6 | 32.5 |
| At risk of overweight (including obesity)d | 29.1 | 32.3 | 32.8 | 30.2 | 31.3 | 32.7 | 30.6 |
| At risk of obesitye | 14.3 | 15.8 | 16.6 | 16.4 | 16.1 | 17.2 | 16.8 |
| Bases (weighted): | |||||||
| Boys | 985 | 1243 | 669 | 958 | 641 | 655 | 663 |
| Girls | 931 | 1182 | 621 | 924 | 612 | 621 | 620 |
| All children | 1916 | 2425 | 1290 | 1882 | 1253 | 1276 | 1283 |
| Bases (unweighted): | |||||||
| Boys | 1780 | 1208 | 652 | 967 | 662 | 643 | 630 |
| Girls | 1704 | 1215 | 640 | 914 | 569 | 626 | 644 |
| All children | 3484 | 2423 | 1292 | 1881 | 1231 | 1269 | 1274 |
| a Children whose BMI was more than 7 standard deviations above or below the norm for their age were excluded from the table. The 1998 to 2011 figures have been revised as prior to 2012 cases which were more than 3 standard deviations above or below the mean for all children were excluded. | |||||||
| b BMI above 2nd percentile, below 85th percentile. The 1998 to 2011 figures have been revised as prior to 2012 the range was above 5th percentile and below 85th percentile. | |||||||
| c BMI at or below 2nd percentile, at or above 85th percentile | |||||||
| d BMI at or above 85th percentile | |||||||
| e BMI at or above 95th percentile | |||||||
Table 7.4 Children's BMI, 2012, by age and sex
| Aged 2-15 with valid height and weight measurementsa | 2012 | |||
|---|---|---|---|---|
| BMI status (National BMI percentiles) | Age | Total | ||
| 2-6 | 7-11 | 12-15 | ||
| % | % | % | % | |
| Boys | ||||
| At risk of underweightb | 0.4 | 1.5 | 2.5 | 1.4 |
| Healthy weightc | 67.0 | 68.0 | 59.5 | 64.9 |
| At risk of overweightd | 17.7 | 12.0 | 12.0 | 13.9 |
| At risk of obesitye | 15.0 | 18.4 | 26.1 | 19.7 |
| Outwith healthy rangef | 33.0 | 32.0 | 40.5 | 35.1 |
| Overweight (including obese)g | 32.7 | 30.5 | 38.1 | 33.6 |
| Girls | ||||
| At risk of underweightb | 2.1 | - | 5.2 | 2.3 |
| Healthy weightc | 75.6 | 73.0 | 60.9 | 70.3 |
| At risk of overweightd | 13.0 | 12.8 | 15.6 | 13.7 |
| At risk of obesitye | 9.3 | 14.2 | 18.3 | 13.7 |
| Outwith healthy rangef | 24.4 | 27.0 | 39.1 | 29.7 |
| Overweight (including obese)g | 22.3 | 27.0 | 33.9 | 27.4 |
| All children | ||||
| At risk of underweightb | 1.3 | 0.8 | 3.7 | 1.9 |
| Healthy weightc | 71.3 | 70.4 | 60.2 | 67.5 |
| At risk of overweightd | 15.4 | 12.4 | 13.7 | 13.8 |
| At risk of obesitye | 12.1 | 16.4 | 22.5 | 16.8 |
| Outwith healthy rangef | 28.7 | 29.6 | 39.8 | 32.5 |
| Overweight (including obese)g | 27.5 | 28.8 | 36.1 | 30.6 |
| Bases (weighted): | ||||
| Boys | 220 | 231 | 212 | 663 |
| Girls | 218 | 218 | 184 | 620 |
| All children | 438 | 448 | 396 | 1283 |
| Bases (unweighted): | ||||
| Boys | 217 | 214 | 199 | 630 |
| Girls | 235 | 224 | 185 | 644 |
| All children | 452 | 438 | 384 | 1274 |
| a Children whose BMI was more than 7 standard deviations above or below the norm for their age were excluded from the table | ||||
| b BMI at or below 2nd percentile | ||||
| c BMI above 2nd percentile, below 85th percentile | ||||
| d BMI at or above 85th percentile, below 95th percentile | ||||
| e BMI at or above 95th percentile | ||||
| f BMI at or below 2nd percentile, at or above 85th percentile | ||||
| g BMI at or above 85th percentile | ||||
Contact
Email: Julie Landsberg