General Medical Services provision - patients displaying violent behaviour: comparative review
Nationwide comparative review of the provision of General Medical Services for patients displaying violent behaviour in Scottish GP practices.
Results
Responses were obtained from 13 Health Boards (Appendix 2); NHS Shetland provided no response. NHS Borders, Grampian and Orkney indicated they did not have CBSs, although NHS Borders provided details of their planned service. NHS Greater Glasgow & Clyde runs two separate services, Glasgow and Clyde. NHS Highland also splits its provision of CBSs; a response was only obtained from Argyll & Bute. Thus 11 CBSs are considered herein.
Question One: Eligibility and referral process
While four CBSs strictly only see patients subject to immediate removal, the remaining seven described various circumstances under which other patients may be seen (Q1A&B):
"On occasion there are patients who engage poorly or in a toxic fashion but who never the less may need an intervention or referral and we take these as well."
Ayrshire & Arran
"A patient who they (a practice) think has challenging behaviour."
"Patients … who have been deregistered from their GP practice for unreasonable/violent behaviour"
Dumfries & Galloway
"Any incident where a GP, or his or her staff, are abused, threatened or assaulted in circumstances related to their work, involving an explicit, or implicit, challenge to their safety, well-being or health."
"Patients who have been threatening where the Police have been called are more likely to be accepted onto the CBR register but this is not always the case. Each referral is assessed independently."
Clyde
"Patients who behave in an abusive, threatening, aggressive or violent way and do not respond to measures to contain this behaviour e.g. behavioural contract."
Lothian
Details of the proportion of patients subject to immediate removal in each service were generally unavailable, although Forth Valley indicated that 44% (18/41) of their current patients met this criterion.
Each CBS described a unique screening process for referrals, with timescales for this process varying from a few days to four weeks (Q1F&G). During this referral process, arrangements are consistently in place to ensure ongoing GMS provision, although there is variation in how this is achieved (Q3C). Both the number of referrals received and accepted in the past year varied from 1 to 27 (Figure 1) (Q1C&D). Although the documented 'referrals received' may underestimate the demand CBSs face:
"This figure is not an accurate reflection as there are a large number of enquiries dealt with verbally, e.g. to enquire whether the criteria has been met. (Referring) practices have different levels of tolerance."
Tayside
Moreover, Lothian identified the expectations of referring practices as among their main challenges:
"Expectation of referring practices that extremely violent patients will be accepted and expectation of referring GPs that all referrals will be accepted. Awareness of referring practices that there are steps that they can take with the patients prior to referrals e.g. behavioural contracts."
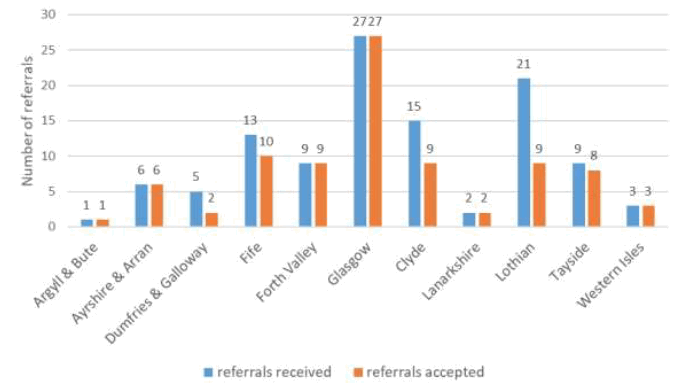
Referrals which were not accepted (25/111) generally represented difficult to manage, but not dangerous, patients; in these circumstances resolution was able to be achieved by other means (Q1E):
"Requesting multiple prescriptions, verbally abusive, can be seen as aggressive and difficult to manage, patients with significant mental health issues. Primary Care worked with the practices to encourage and support further engage with patient and try and resolve the issues. An example could be to support the practice to meet with patient, setting up protocols between the patient and the practice to outline what is acceptable behaviour within the GP practice."
Dumfries & Galloway
"These were difficult, but not dangerous patients. The referring practices were asked to keep them."
Fife
"Mainly verbal abuse or emotional response towards practice staff or other patients. Where there is no actual violence or threat of violence then the patient is not accepted. Patient will be informed by PSD that they have been removed from their GP list and will need to seek GP services elsewhere."
Clyde
"Referrals where not all avenues had been exhausted to dealing with the patients e.g. behavioural contracts. Or where referral to another agency would be more appropriate: e.g. addiction services or specialist dementia services."
Lothian
"Patient generally verbally abusive. Practice issued warning to patient that if behaviour continued they would be removed."
Tayside
Question Two: Service design
While Glasgow described designated service premises, the remaining CBSs are integrated within mainstream services: four in central out-of-hours/A&E departments and six within general practices (Q2D). Four CBSs operate from a single central practice while Clyde operate from three practices and the Western Isles from practices across the Uists and Barra. Argyll & Bute are forced to make interim arrangements for individual patients:
"Due to the remote and rural geography of Argyll and Bute we do not have permanent established Challenging Behaviour Services for the 28 GP Practices in the above 3 localities (in Oban Lorn & Isles, Mid Argyll Kintyre & Islay and Cowal & Bute). Alternatively, where incidences of violence occur interim arrangements are put in place as and when required. Frequently, the interim arrangements have to be put in place with the same practice that has removed the patient due to geography. An agreement is in place with NHSGG&C for the 5 GP Practices in Helensburgh & Lomond."
Argyll & Bute
While CBS patients in Dumfries & Galloway are seen in normal surgeries, simply with alerts in their records, the remaining 10 CBSs have security or Police present at appointments (Q2E). However, this is difficult to ensure in certain services:
"Police attendance at the patients GP appointments is a criterion of the contract agreement however due to the geography of Argyll and Bute and Police availability it is not always possible for the Police to attend. On occasion we have had the Police refusing to engage at all with the service. This makes the provision and implementation of the interim services DES very difficult."
Argyll & Bute
"Police presence is requested for the clinic, however this is not always guaranteed." Main challenge of service identified as "risk to staff safety at clinic due to no Police presence".
Ayrshire & Arran
In Clyde not all patients require Police presence, with patients evaluated and 'stepped-down' accordingly. Across services, where security or Police are present, they typically remain outside the consulting room, although in Glasgow security guards undertake additional security measures:
"Our security guards use a dedicated private room for screening patients, offering them dignity and privacy when this is taking place. We use a hand held metal detector, and patients are requested to remove items from their pockets in a secure box until after their clinical consultation. We do not allow patient to retain their walking sticks or crutches as these have also been used as weapons. Patients can used walking aids to go to the clinical room for their consultation but these are then removed by security personnel and returned after the consultation."
Four services indicated they have also implemented other safety measures:
"On occasion, practices providing the DES are offered advice from the local Community Police regarding the layout of the consulting room and changes that may assist with making consultations with violent patients safer."
Argyll & Bute
"The patient is seen in a room where there are 2 exits."
Forth Valley
"Patients are told that they must phone the practice and must not come into the surgery without an appointment even to pick up prescriptions or to accompany relatives or dependents."
Clyde
"The premises have also been inspected and recommendations made to ensure staff safety, e.g. panic alarms, room layout etc."
Tayside
Within CBSs, patients are typically offered longer appointments (Q2F) and are seen by either a GP alone (n=7) or with a nurse (n=4) (Q2E), with other interactions generally managed by practice staff as for other patients (Q2C). Across CBSs patients are able to be referred as normal to other services while four services receive specific additional support (Q2G):
"We have constant liaison with Forensic Psychology and Criminal Justice Service, together with ongoing support from our Clinical Director and Head of Homelessness. We have in addition to this, Forensic Psychology appointments on the same days as our CBRS Clinic, 2 per session."
Glasgow
"If the patient assigned to the DES is currently being seen by other services then support may be provided during the patients inclusion. E.g. assigned patient being seen by Community Mental Health service then patient attendance at GP appointments may be supported by CPN in attendance instead of the Police."
Argyll & Bute
"Supported by Clinical Psychologist who offers fortnightly appointment slots at practice."
Lothian
"Some input from substance misuse services."
Western Isles
The number of patients currently registered within each CBS varies from 0 to 36, with service capacity also varying considerably (Figures 2 & 3) (Q2A). While most services indicated an ability to cope with current demand and additional capacity, Fife raised significant concerns:
"The increase in referrals is becoming too demanding for the capacity the practice has". This was also identified as the main challenge faced by Fife "Number of referrals at the highest they have ever been. The practice providing the service is threatening to resign from the LES due to this and we are concerned no one else will pick it up."
Moreover, Glasgow cited increasing patient numbers as one of their main challenges:
One of the main challenges the service faces is "access to this service, given that CBRS has tripled in size this year with a plethora of new patients."
| Challenging Behaviour Service | Number of patients currently registered | Capacity (patient number) |
|---|---|---|
| Argyll & Bute | 0 | N/A |
| Ayrshire & Arran | 33 | 40 1 hour/week, maximum 3 patients/session |
| Dumfries & Galloway | 22 | "more" |
| Fife | not provided | 20 |
| Forth Valley | 36 | N/A |
| Glasgow | 75 | monthly 40 patients, annually 480 5 appointments/session, 2 sessions/week |
| Clyde | 29 | no limit but depends on appointment availability |
| Lanarkshire | 36 | 45 previously been able to be accommodated |
| Lothian | 28 | 40 260 appointments annually |
| Tayside | 8 | N/A but 8 is highest ever accommodated |
| Western Isles | 2 | N/A but never had more than 6 |

The cost of each CBS also varies considerably (Figure 4).
| Argyll & Bute | £750/patient |
|---|---|
| Ayrshire & Arran | £37,500 |
| Dumfries & Galloway | £6,355, £192/patient |
| Fife | £20,000 |
| Forth Valley | £25,000 |
| Glasgow | £68,600, £1372/patient (2017 data) |
| Clyde | £26491, £914/patient |
| Lanarkshire | £44,428, £1,100/patient |
| Lothian | £76,800, £1,920/patient |
| Tayside | cost neutral |
| Western Isles | £2,333/patient, historically £10,000/year but costs increasing |
Lothian and Glasgow were the only CBSs who described routine support available to staff (Q2I):
"Clinical debriefs prior to all practice sessions with all CBGP staff. Meetings with Clinical Psychologist. Committee meetings – quarterly."
Lothian
"We are a small, tight team and our Lead Clinician and Clinical Director offer support particularly following upsetting and difficult engagement, this is also available following disruptive and abusive incidents. We are also offered ongoing individual consultation with our colleagues at Forensic Psychology to "unload" following a challenging/abusive situation."
Glasgow
Clyde identified the lack of additional support as one of their main challenges. Although, as a number of services highlighted, all staff across CBSs would be eligible for occupational health support and several identified other support mechanisms that could be used:
"Primary Care team have a good relationship with the practice team providing this service, and if any concerns or guidance required by the doctors or any of the practice staff they would contact Primary Care team for support, and where necessary these would be raised with the Deputy Medical Director."
Dumfries & Galloway
"The staff would report any concerns to the Primary Care Manager/Associate Medical Director where appropriate support would be offered."
Forth Valley
"Staff members can speak to the lead GP and Practice Manager regarding any incidents or to raise concerns. Counselling."
Clyde
"Support from line manager is also available".
Lanarkshire
Furthermore, five services offer training to staff (Q2H):
"Team GP and Practice Nurse have both undergone breakaway training."
Ayrshire & Arran
"Personal safety training."
Fife
"All administration staff have been trained in violence reduction; stress at work and suicide prevention training."
Glasgow
"All staff have received violence and aggression training."
Lothian
"Aggression management training is arranged and provided for all staff required."
Tayside
Question Three: Accessibility
In 10 CBSs telephone advice is available during normal surgery hours. However, in Ayrshire & Arran contact is via an answering machine with responses given within 48 hours, a source of some complaints. Six services only offer appointments during restricted hours:
Ayrshire & Arran – 12pm on Tuesdays
Fife – 5-6pm week nights
Glasgow – Monday and Thursday 9.30am-12pm
Lanarkshire – Monday after 5pm
Lothian – Wednesday 11am-1pm and Friday 10.30am-12.30pm
Western Isles – typically after 6pm
The remaining five services place no restrictions compared to other patients (Q3A). However, for the four of these five services where security is required, the availability of security imposes some restrictions on availability. Moreover, appointment times are typically chosen with regard to the safety of other patients:
"The GP will choose an appropriate time for the patient to be seen; this would usually avoid busy periods e.g. baby clinics etc., and we would also try to avoid times when other potentially disruptive patients may be present e.g. drug clinics."
Clyde
"Within core hours 8am to 6pm, although, actual attendance at the surgery is managed to ensure limited exposure to other members of the public - normally over a lunch time period or other time when there are few patients in the waiting room."
Tayside
Across CBSs home visits are consistently not available (Q3D). Outside appointment times all patients are able to attend A&E, while patients from five CBSs cannot attend out-of-hours services (Q3B). Five CBSs indicated they notify these other services of CBS status via alerts.
Transport to CBSs is not provided, although three services reimburse travel expenses (Q3E). Tayside have received complaints regarding the need to travel to Dundee to access GMS.
Question Four: Return to mainstream General Practice
While the majority of services have no time limits or targets for return to mainstream GMS, Ayrshire & Arran indicated that "patients should spend no more than 12-months with the service" (Q4A). Data on the average duration patients remain in CBSs is not available, although responses indicated that there is substantial variation in duration, with decisions made on a case-by-case basis and some services retaining patients long-term. Across services, patients are reviewed for readiness to return at different intervals with decisions made individually by the GP (n=7) or by committee (n=4) (Q4D).
Each CBS has unique procedures for managing handover (Q4F&G). On discharge, patients are not typically able to return to their previous practice (Q4E). However this may be necessary in remote and rural settings, which is challenging:
"Due to the geographical nature of Ayrshire & Arran, on occasion the patient will return to their original practice as this is the only practice that covers the patients home address. However, there is considerable resistance to this."
Ayrshire & Arran
"The geography of Argyll and Bute means that in the majority of cases the patient has to return to their previous practice."
Argyll & Bute
Question Five: Service evaluation
Each CBS described a different approach to service evaluation (Q5C): seven indicated no formal evaluation process and four described a process of annual or periodic review.
For the majority (n=10), routine data collection solely centres around activity data including number of patients and costs, while audits and evaluation of patient experiences have not been undertaken (Q5A, D&E). However, Glasgow undertakes further data collection publishing an annual report; patient experience was also evaluated 14-months ago[17]:
"We also utilise GP EMIS to collate data on attendance and issue D.N.A. (did not attend) letters to patients who do not keep their appointments. GP EMIS and Docman allow us to receive electronic documents for any patients who attend any A & E departments and this is also recorded on patients electronic records. For severely disruptive patients, and we have a few, we also collect data on the frequency of their calls to CBRS together with the abusive language and disruption they cause."
While there is a general lack of formal outcome evaluation, two services capture information on subsequent violent behaviour in primary care, although this data was unavailable (Q5B):
"We carry out additional risk assessments when a CBRS patient causes an incident and record this on our own incident reporting system – Datix."
Glasgow
"The Primary Care team manage this service for the Board and would be made aware of any subsequent violent behaviour, annual reviews are undertaken by the DPCS practice to also capture this information and these reviews are considered by the Board."
Dumfries & Galloway
Question Six: Challenges encountered
The main challenges highlighted by CBSs fall into five broad areas: sustainability and expectations, safety concerns, difficult patients, lack of support and training and remote and rural service provision (Figure 5) (Q6A).
Six services reported no formal complaints while three received complaints relating to the need to be seen in a CBS, with Lothian describing "a number of patients who see the care arrangements as a breach of their human rights". Other complaints received related to location, limited clinic times and access (Q6B).
Figure 5. Main challenges encountered by Challenging Behaviour Services.
Sustainability and expectations
"Sustainability – have required to contract with new providers on a number of occasions." Forth Valley
"Number of referrals at the highest they have ever been. The practice providing the service is threatening to resign from the LES due to this and we are concerned no one else will pick it up." Fife
"Access to this service given that CBRS has tripled in size this year with a plethora of new patients." Glasgow
"Expectation of referring practices that extremely violent patients will be accepted. Expectation of referring practices that all referrals will be accepted. Awareness of referring practices that there are steps that they can take with patients prior to referrals e.g. behavioural contracts." Lothian
"The inability to engage with clinicians willing to support the Health Board to operate the scheme. We had to arrange for a 2C practice to operate this scheme as despite much advertisement and encouragement, both incentive and financially wise, we could not establish an independent medical practice, or individual GPs to work with the Health Board to operate the scheme." Tayside
"In Lewis & Harris, unwillingness of practices to participate in the DES." Western Isles
Safety concerns
"Interim DES arrangements being made with the same practice that removed the violent patient. Police non-engagement on occasion. Police availability to attend appointments." Argyll & Bute
"Risk to staff safety at clinic due to no police presence." Ayrshire & Arran
"Safety of administration team in reception area – registration desk is not fit for purpose. Mismatch between GP duty of care to protect staff from harm/provide safe working environment and patient need." Lothian
Difficult patients
"One or two drug seeking patients who live out with the practice area." Dumfries & Galloway
"Ongoing patient behaviours particularly verbal abuse." Forth Valley
"Patient's reluctance to accept that their own abusive and unruly behaviour was sufficient for them to be assigned to CBS. Unwillingness to attend and constant abusive phonecalls to advise why. Constant swearing and threatening phone calls from newly registered patients who do not want to engage with us. Constant verbal complaints from some patients who feel they should be prescribed opiates and controlled drugs. Refusal to follow protocols and patients arriving at other HSCP sites causing distress and disruption to services, even though they have been engaging at our current site." Glasgow
"Dealing with abusive patients." Lanarkshire
"Increasing number of angry patients." Lothian
Lack of support and training
"No additional support outside of the Police. Training for staff." Clyde
Remote and rural service provision
"Due to the remote and rural geography of Argyll and Bute we do not have permanent established Challenging Behaviour Services …. frequently, the interim arrangements have to be put in place with the same practice that has removed the patient due to geography." Argyll & Bute
Question Seven: Broader perspectives on violence in primary care and the role of CBSs
Drug-seeking behaviour was cited most often as the cause of violent behaviour (n=5) with other causes cited with varying frequency (Figure 6) (Q7A).
| Drug-seeking behaviour | 5 |
|---|---|
| Lack of services to meet needs of patients with complex problems | 3 |
| Poor interaction and social skills | 2 |
| Unreasonable patient expectations | 2 |
| Frustration in obtaining appointments and not getting own way | 2 |
| Being denied sick lines or medication where needed | 1 |
| Not being listened to | 1 |
| Feeling let down | 1 |
| Feeling powerless | 1 |
Patients seen in CBSs are also generally considered to have other underlying characteristics/problems: substance misuse (n=11), mental health (n=8), male (n=3),
ex-prison (n=2), anger management (n=2) and complex psycho-social needs (n=1) (Q7B). Other responses offer further insight into this group:
"Individuals who are, on the whole, misunderstood and/or ill."
Ayrshire & Arran
"Often minor disgruntlement in patients with poor coping skills that simply
need handling differently." Role of service described as to "make the patient realise the world and medical services are not against them."
Dumfries & Galloway
While all services cited their role in providing GMS, many also described other roles centring around active rehabilitation (Q4B&C and Q7C&D):
"The GP Practice should be taking steps to rehabilitate the patient to allow the patient to return to mainstream GMS when appropriate."
Argyll & Bute
"We explore the issues which led them to become involved with the service and treat those conditions that are amenable to such. At each appointment reference is made to the patient's pending return to GMS and how they might better relate to mainstream services."
Ayrshire & Arran
"Make the patient realise the world and medical services are not against them. Make the person feel treated normally with respect whatever is wrong and not label patient as a trouble maker."
Dumfries & Galloway
"This (addressing the underlying issues that led to a patients referral) is done opportunistically at consultations."
Fife
"Rehabilitation back to mainstream GP Practice, and addressing issues patient presents with – anger issues; abandonment issues; drug seeking behaviour; criminal activity; personality disorder. Baseline assessment … to assess the reason behind the disruptive behaviour which led to referral to CBRS."
Glasgow
"Patients challenging behaviour and its cause is addressed in appointments. Referrals to Psychology or Specialist Services as required. Patients are offered the opportunity to address circumstances: medical, social or relational that contributed to their challenging behaviour."
Lothian
Contact
Email: michael.taylor@gov.scot