Coronavirus (COVID-19): mental health tracker study - wave 1 report
Findings of wave 1 of the Scottish COVID-19 (SCOVID) Mental Health Tracker Study based on questionnaire data collected between 28 May and 21 June 2020 (a period which coincided with the Phase 1 easing of lockdown measures).
3. Mental Health Outcomes
This section reports on the main mental health outcomes for the study, specifically looking at differences between particular subgroups in the sample (see section 2 for details). The main mental health outcomes focused on included: depressive symptoms, anxiety symptoms, suicidal thoughts, the general health questionnaire (GHQ), and mental wellbeing. The SCOVID Mental Health Tracker Study also included other correlates of mental wellbeing, such as loneliness and social support, and these are reported more briefly.
The findings from the Wave 1 SCOVID Mental Health Tracker Study suggest that a number of key groups report poorer mental health outcomes during the COVID-19 pandemic, including higher depressive and anxiety symptoms. Specifically, subgroups at a higher risk of poorer mental health outcomes include young adults (18-29 years), women (in particular young women), those with pre-existing mental health conditions, and those in the lower SEG. Respondents who identified as BAME (Black, Asian and Minority Ethnic) also frequently reported worse on some mental health indicators, however it must be noted that the sample size for the study respondents who identified as BAME is quite small and so this finding must be considered cautiously.
Respondents were asked to rate their mental health before COVID-19 and currently (during the COVID-19 lockdown). Overall, people felt that their mental health had worsened during the COVID-19 lockdown (see Table H in the annex). The percentage of people reporting their mental health was 'Fair', 'Poor', and 'Very Poor' increased compared to before COVID-19. Correspondingly, the percentage reporting their mental health was 'Very Good' and 'Good' dropped. Approximately 13.6% of the sample shifting from reporting better mental health prior to the COVID-19 pandemic to worse mental health.
3.1. Depressive symptoms
Wave 1 of the SCOVID Mental Health Tracker Study shows that approximately a quarter (25.3%) of the overall sample met the cut-off for moderate to severe depressive symptoms. This study's findings on moderate to severe depressive symptoms are based on participants' responses to questions on the mental health measure called the Patient Health Questionnaire (PHQ-9; Kroenke et al., 2001), which assesses frequency of depressive symptoms over the previous two weeks. For the purposes of this report, scores above the cut-off for moderate to severe depression are tracked so as to mirror the most commonly used indicator in mental health research, and which suggests that treatment (psychotherapy or medication) may be recommended. The following groups reported higher rates of moderate to severe depressive symptoms:
- Young adults (age 18-29 years old)
- Young women, in particular (age 18-29 years old)
- BAME groups
- Those with pre-existing mental health conditions
Looking more deeply at the findings shows that there were clear differences in depression scores according to age and sex, illustrated in Table 3.1. For example, in the overall sample, women were more likely to report symptoms that met the cut-off for moderate or severe depressive symptoms (27.6%) than men (22.7%). In addition, young adults (18-29 year olds) reported higher rates of depressive symptoms (44.7%), compared to 25.9% of those in the middle age group (30-59 years) and 9.2% of the oldest age group (60+ years). This means that during Wave 1 of this study, young adults were almost 5 times as likely to report symptoms indicating depression than the oldest age group. Furthermore, young women between 18-29 years old reported higher rates of depressive symptoms at 50.9%, compared to 38.9% of men in the same age group. This indicates that within Scotland, age and sex can have a bearing on a person's mental health and wellbeing experience during the COVID-19 pandemic, and more young adults and women reported moderate to severe depressive symptoms.
This study also measured how respondents' experience of depressive symptoms affected other aspects of their lives. For example, 44.3% of individuals who reported any depressive symptoms said these had made it somewhat difficult for them to do work, take care of things at home, or get along with other people, and 12.4% said it made it very or extremely difficult to accomplish these activities.
| 18- 29 years % (n=576) | 30- 59 years % (n=1174) | 60+ years % (n=749) | Total % (n=2499) | |
|---|---|---|---|---|
| All adults | 44.7 | 25.9 | 9.2 | 25.3 |
| Men | 38.9 | 22.5 | 9.7 | 22.7 |
| Women | 50.9 | 28.9 | 8.8 | 27.6 |
Beyond age and sex, respondents' backgrounds also had a bearing on the likelihood of reported rates of moderate to severe depression, illustrated in Figure 3.1. Respondents in the lower SEG reported higher rates of depressive symptoms (31.2%) compared to those in the higher SEG (21.9%). In addition, individuals who identified as BAME reported higher rates of depressive symptoms (37.4%) than those who identified as White (24.9%), although it should be noted that as the BAME group was a small proportion of the sample (4.9%), caution is urged in terms of interpretation.
Differences in occupation, financial, and home life circumstances also appear to correlate with varying rates of depressive symptoms, and indicate that those living with greater financial uncertainty or added responsibilities at home are at a greater risk for depressive symptoms. For example, 32% of respondents fulfilling key worker roles reported higher rates of depressive symptoms, compared to 23.7% of those who were not key workers. Also, respondents who reported a change to their working status (e.g., furloughed, lost job or reduction in pay) experienced higher rates of depressive symptoms (29.5%) than those that had experienced no change in their occupation (21.7%). While there were no differences in rates of moderate to severe depression between those who lived alone and those who lived with others (such as any family, friends or housemates), those with dependents under 5 years old (32.9%) and those that reported any caring responsibilities (34.3%) reported higher rates of depressive symptoms compared to those with no dependents (24.8%) or caring responsibilities (23.9%). The data also suggest that among carers with 5 or more hours of caring responsibility every week, the rate of depressive symptoms was 39.3%, which is 15.4% higher than those without any caring responsibilities.
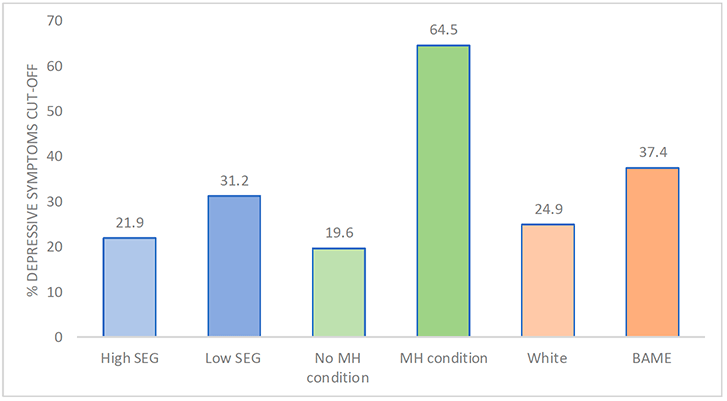
Chart description:
21.9 % of those in the high SEG and 31.2% of those in the low SEG reported moderate to severe depressive symptoms. 19.6% of those with no pre-existing mental health condition and 64.5% of those with a pre-existing mental health condition reported moderate to severe depressive symptoms. 24.9% of White respondents and 37.4% of those who identified as BAME reported moderate to severe depressive symptoms.
Finally, this study also offers insight into how an individual's health prior to the pandemic may be associated with their experience of depressive symptoms. For example, over two thirds of respondents with a pre-existing mental health condition reported depressive symptoms (64.5%), compared to just under one fifth of those without a pre-existing condition (19.6%). Respondents in the shielding category reported almost double the rate of depressive symptoms (44.8%) than those who had not been specifically asked to shield (23.9%). Interestingly, those in a high risk group (i.e., aged over 70 years old and/or with an underlying health condition) reported lower rates of depression (18.8%) than those not in a high risk or shielding group (27.3%). One possible explanation for why the 'high risk' group in the study sample might report lower rates is that the 'high risk' group is primarily made up of those aged 60+ years (73.7% aged 60+ compared to 17.8% in the non-high risk group) and overall, this older age group reported lower rates of mental ill-health and appears to be more protected for mental health.
3.2. Anxiety symptoms
Wave 1 of the SCOVID Mental Health Tracker Study indicated that nearly one fifth (19.1%) of respondents met the cut-off for moderate to severe anxiety symptoms. Anxiety symptoms were assessed using the mental health measure called the Generalised Anxiety Disorder (GAD-7; Spitzer et al., 2006) scale, which asks about frequency of anxiety symptoms in the last 2 weeks. For the purposes of this report, the clinical cut-off for moderate to severe anxiety was reported, indicating anxiety symptoms that may require further treatment. A number of subgroups reported higher rates of moderate to severe anxiety symptoms, specifically:
- Young adults (18-29 years old)
- Young women (18-29 years old)
- Those with a pre-existing mental health condition
- Those from the lower SEG
Looking more closely at the findings there were differences in moderate to severe anxiety symptoms according to sex and age, displayed in Table 3.2. For example, when comparing sex only, women reported rates of moderate to severe anxiety symptoms (22.1%) that were slightly higher than men (19.1%). There were also differences by age groups: young adults (18-29 year olds) were nearly 5 times more likely to report moderate to severe anxiety symptoms than older adults (60+ years), with 33.5% of young adults (18-29 year olds) reporting moderate to severe anxiety compared to 19.6% of 30-59 year olds and 7.2% of 60+ year olds.
When looking at groups by both gender and sex, further differences in the likelihood for experiencing moderate to severe anxiety arise. For example, young women aged between 18-29 years reported markedly higher rates of moderate to severe anxiety symptoms (43.0%) than younger men (24.6%). Older women reported the lowest levels of anxiety symptoms (4.9%) of the sample, which was nearly half that of the older men's rate of 9.7%. This suggests that younger women in particular report experiencing anxiety symptoms during the COVID-19 pandemic, and this difference lessens as they get older, and is almost reversed in the oldest age group with older men having higher moderate to severe anxiety rates than older women.
| 18- 29 years % (n=576) | 30- 59 years % (n=1174) | 60+ years % (n=749) | Total % (n=2499) | |
|---|---|---|---|---|
| All adults | 33.5 | 19.6 | 7.2 | 19.1 |
| Men | 24.6 | 15.1 | 9.7 | 15.8 |
| Women | 43.0 | 23.5 | 4.9 | 22.1 |
Beyond age and sex, respondents' backgrounds and financial circumstances also had a bearing on the likelihood of reported rates of moderate to severe anxiety, illustrated in Figure 3.2. About 7% more respondents in the lower SEG (23.6%) experienced moderate to severe anxiety symptoms than those in the higher SEG (16.4%). A marginal 2.3% difference in rates of moderate to severe anxiety was found between those who identified as BAME and those who identified as White, although this was not statistically significant.
Differences in working life, home life, and carer circumstances appeared to correlate with rates of moderate to severe anxiety symptoms. For example, in terms of occupational circumstances, nearly a quarter of key workers (i.e., those who were working essential jobs) reported moderate to severe anxiety, which is higher than those who were not fulfilling key roles (17.9%). In addition, respondents whose working situation had changed during the pandemic (e.g., furloughed, lost job) reported higher anxiety rates (22.7%) than those with no change (16.0%). Shifting focus to home-life circumstances, respondents living in households with dependents under 16 years old reported 5% higher rates of moderate to severe anxiety (23.0%) compared to those who had no dependents under 16 years (18.0%). Additionally, respondents who had caring responsibilities had almost a 10% higher likelihood of anxiety symptoms (26.9%) than those who did not have any caring responsibilities (17.7%). Further, reports of moderate to severe anxiety symptoms rose to a third (33.3%) for people who had caring responsibilities for more than 5 hours per week.
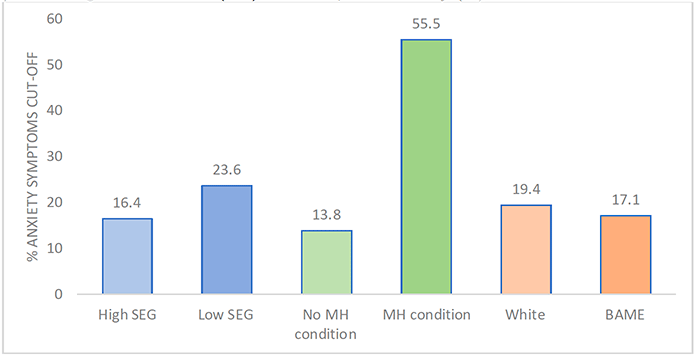
Chart description:
8.7% of those in the high SEG and 12.9% of those in the low SEG reported suicidal thoughts. 7.1% of those with no pre-existing mental health condition and 32.6% of those with a pre-existing mental health condition reported suicidal thoughts. 10.0% of White respondents and 17.9% of those who identified as BAME reported suicidal thoughts.
Finally, this study also offers insight into how an individual's health prior to the pandemic may be associated with their experience of anxiety symptoms. For example, over half of those with a pre-existing mental health condition (55.5%) met the cut-off for moderate to severe anxiety, compared to only 13.8% of those with no mental health condition. Additionally, respondents in the shielding group experienced higher rates of moderate to severe anxiety symptoms (29.1%) than those not asked to shield (18.5%). Interestingly, the high risk group (i.e., over aged 70 years old and /or underlying health condition) reported lower rates of moderate to severe anxiety (14.7%) than those who were not high risk or shielding (20.7%). One possible explanation for why the 'high risk' group in the study sample might report lower rates is that the 'high risk' group is primarily made up of those aged 60+ (73.7% aged 60+ compared to 17.8% in the non-high risk group). Overall, this older age group reported lower rates of mental ill-health and appears to be more protected for mental health.
3.3. Suicidal thoughts, suicide attempts, and self-harm
The Wave 1 data from the SCOVID Mental Health Tracker Study found that over one tenth of respondents experienced suicidal thoughts within the week prior to completing the survey. Respondents were asked: 'how often have you thought about taking your life in the last week?', and were provided with options that ranged from "Never", "One day", "Several days", "More than half the days", "Nearly every day", and "I would rather not answer". For the purposes of this report, respondents who experienced any suicidal thoughts in the week prior to the Wave 1 questionnaire (i.e., one day or more) were included in the suicidal thoughts findings. Respondents were also asked about their experiences of suicide attempts and self-harm in the prior week, however it must be noted that numbers for these measures were quite small and therefore comparison between groups was not possible.
The subgroups which reported higher rates of suicidal thoughts were:
- Young adults (age 18-29 years)
- Younger women
- BAME groups
- Those with pre-existing mental health conditions
There were some differences in rates of suicidal thoughts and self-harm by age and sex, illustrated in Table 3.3. In the overall sample, there were no differences between men (10.0%) and women (10.3%) in rates of suicidal thoughts in week prior to responding to the Wave 1 questionnaire. However, women reported more self-harm in the last week (2.1%) compared to men (0.5%), and this was highest for women aged 18-29 years old (5.3%).
The oldest age group (60+ years) consistently reported the lowest rates of suicidal thoughts, and this age group also reported no suicide attempts or self-harm in the prior week. In contrast, one fifth (21.1%) of young adults (18-29 years) reported suicidal thoughts, which was twice as high as those aged 30-59 years (10.2%) and 9 times higher than those aged 60+ years (2.3%). Young women reported the highest rates of suicidal thoughts in the past week (24.3%), higher than that of young men (18.1%). Similarly, young adults (18-29 years) reported the highest rates of suicide attempts (0.7%) and self-harm (3.0%) in the last week, compared to other age groups.
| 18- 29 years % (n=576) | 30- 59 years % (n=1174) | 60+ years % (n=749) | Total % (n=2499) | |
|---|---|---|---|---|
| Men | ||||
| Suicidal thoughts last week | 18.1 | 10.9 | 2.5 | 10.0 |
| Suicide attempt last week | 1.1 | 0 | 0 | 0.3 |
| Self- harm last week | 0.7 | 0.8 | 0 | 0.5 |
| Women | ||||
| Suicidal thoughts last week | 24.3 | 9.6 | 2.1 | 10.3 |
| Suicide attempt last week | 0.4 | 0.5 | 0 | 0.3 |
| Self- harm last week | 5.3 | 2.1 | 0 | 2.1 |
| All adults | ||||
| Suicidal thoughts last week | 21.1 | 10.2 | 2.3 | 10.3 |
| Suicide attempt last week | 0.7 | 0.3 | 0 | 0.3 |
| Self- harm last week | 3.0 | 1.5 | 0 | 1.4 |
Respondents' backgrounds also had a bearing on the levels of suicidal thoughts reported, and some of these are displayed in Figure 3.3. For example, individuals from the lower SEG reported higher levels of suicidal thoughts in the last week (12.9%) compared to those from the higher SEG (8.7%). Additionally, individuals from a BAME background reported higher levels of suicidal thoughts (17.9%) compared to those of a White background (10.0%), although it should be noted that the BAME group made up a very small proportion of the sample (4.9%) so these findings must be considered carefully. There were also differences in reports of suicidal thoughts by area lived, with 11% of people living in urban areas (city, small or large town) reporting suicidal thoughts in the last week, which is higher than the 7.6% of those from more rural areas (isolated, hamlet, village) who reported suicidal thoughts.
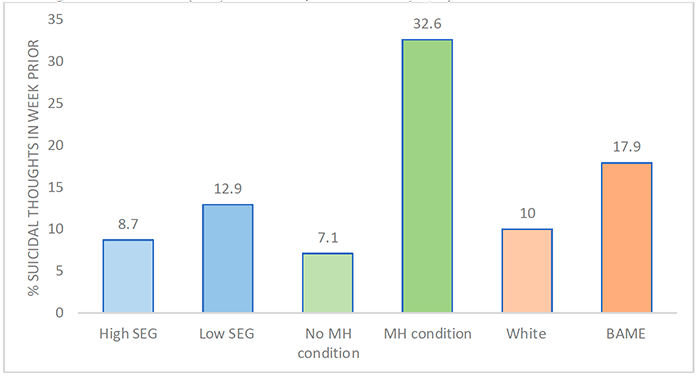
Chart description:
8.7% of those in the high SEG and 12.9% of those in the low SEG reported suicidal thoughts. 7.1% of those with no pre-existing mental health condition and 32.6% of those with a pre-existing mental health condition reported suicidal thoughts. 10.0% of White respondents and 17.9% of those who identified as BAME reported suicidal thoughts.
Differences in occupation, financial, and home life circumstances also appear to correlate with varying rates of suicidal thoughts. Respondents who reported fulfilling a key worker role reported higher rates of suicidal thoughts (15.6%) compared to those who were not in key worker roles (9.0%). Further, respondents who had experienced a change in working status (e.g., working from home, lost job or furloughed) reported higher rates of suicidal thoughts (12.1%) compared to those respondents who had not experienced a change (8.6%).
Having dependents and caring responsibilities also correlated with higher rates of suicidal thoughts. For example, people who had dependents under 5 years old were more likely to report suicidal thoughts (15.4%) compared to those who had no dependents under 5 (9.8%). In addition, people with dependents under 16 years also reported higher rates of suicidal thoughts in the last week (12.7%) compared to those without any dependents under 16 years (9.5%). There were differences reported in rates of suicidal thoughts in carers, as individuals with caring responsibilities (17.2%) were almost twice as likely to report suicidal thoughts than those with no caring responsibilities (8.9%). Differences in rates of suicidal thoughts also arose according to whether caring responsibilities were less than, or more than 5 hours per week: those whose caring responsibilities were over five hours per week (23.2%) were 2.5 times a likely to report suicidal thoughts compared to those with none or less than five hours per week (8.8%).
This study also offers insight into a person's health prior to the pandemic and their likelihood of experiencing suicidal thoughts. For example, as shown in Figure 3.3, there was a stark difference in the reporting of suicidal thoughts in those with or without a pre-existing mental health condition. Those with a pre-existing condition reported nearly 5 times more suicidal thoughts (32.6%) than those without a pre-existing mental health condition (7.1%). Additionally, respondents in the shielding category reported higher levels of suicidal thoughts (21.3%) compared to those who had not been sent a letter asking them to shield (9.5%). In contrast, respondents who were in the high-risk group for COVID-19 (i.e., aged 70+ and/or had an underlying health problem) reported lower levels of suicidal thoughts (6.8%) compared to those not in a high-risk group (11.3%). One possible explanation for why the 'high risk' group in the study sample might report lower rates is that the 'high risk' group is primarily made up of those aged 60+ (73.7% are aged 60+ compared to 17.8% in the non-high risk group) and overall, this older age group reported lower rates of mental ill-health indicators and appears to be more protected for mental health.
3.4. General Health Questionnaire
The General Health Questionnaire (GHQ-12) is a psychological measure that assesses mental distress and mental ill-health in the previous two weeks, including sleep, self-esteem, stress, despair, depression, and confidence. In this report, as consistent with other mental health research studies (McLean et al., 2018), GHQ-12 scores of four or more are reported because this cut-off is deemed a high GHQ-12 score and indicates the presence of a possible psychiatric disorder. In the Wave 1 SCOVID Mental Health Tracker Study, over one third (35.7%) of the sample recorded this high GHQ-12 score. Although there is no pre-COVID-19 comparison for this sample, the most recent Scottish Health Survey (2019) found that around one fifth (17%) of individuals out of a 4000 adult sample across Scotland had a high GHQ-12 score. This suggests that indicators of poorer mental health and the likelihood of possible psychiatric disorders are elevated during the pandemic. These groups had elevated rates of high GHQ-12 scores:
- Young adults (age 18-29 years)
- Younger women (age 18-29 years)
- Those with pre-existing mental health conditions
There were clear differences in GHQ-12 scores by sex and age, as presented in Table 3.4. Specifically, women were 10% more likely to have a high GHQ-12 score (40.8%) than men (30.3%). Additionally, over half (51.5%) of the younger age group (18-29 year olds) reported a high GHQ-12 score, compared to 38.5% of 30-59 year olds and 16.9% of 60+ year olds. Indeed, this may be the case more generally, the Scottish Health Survey (2019) data shows that 23% of those aged 16-24 years recorded a high GHQ-12, compared to 11% among those aged 75 or over. In the SCOVID Mental Health Tracker study, young women were also more likely to have a high GHQ-12 score (58.5%) compared to young men (45%).
| 18- 29 years % (n=576) | 30- 59 years % (n=1174) | 60+ years % (n=749) | Total % (n=2499) | |
|---|---|---|---|---|
| All adults | 51.5 | 38.5 | 16.9 | 35.7 |
| Men | 45.0 | 31.4 | 16.9 | 30.3 |
| Women | 58.4 | 44.7 | 22.1 | 40.8 |
Beyond age and sex, respondents' backgrounds also had a bearing on the likelihood of reporting a high GHQ-12 score, thus suggesting a possible psychiatric disorder, as illustrated in Figure 3.4. Specifically, individuals in the lower SEG were more likely to report a high GHQ-12 score (39.6%) than those from the higher SEG (33.4%). Those identifying as BAME were also more likely to have high GHQ-12 scores (44%) compared to White respondents (35.4%), although it should be noted that BAME group made up a very small proportion of the sample (4.9%), so this finding should be considered carefully.
Differences in home life and carer circumstances also appear to correlate with varying rates of high GHQ-12 scores, which may indicate that those living with added responsibilities at home are at a greater risk for a psychiatric disorder. For example, respondents whose household had dependents under 5 years old were more likely to have high GHQ-12 scores (41.1%) than those with none under 5 years (35.4%), and households with dependents under 16 years old were even more likely to have a high score (43.5%). In addition, nearly half (47.2%) of respondents with caring responsibilities recorded a high score, which was 13.7% higher than those with no caring responsibilities (33.5%), and those who cared for more than 5 hours per week had a still higher likelihood (52.0%).
Differences in occupation and financial circumstances were associated with different rates of high GHQ-12 scores. For example, a similar number of people whose work status had changed during the pandemic (e.g., furloughed or lost job) (42.5%) and key workers (42.7%) met the threshold for a possible psychiatric disorder. This was on average about 10% higher than those whose work status had not changed (29.5%) and those not fulfilling a key worker role (34.1%).
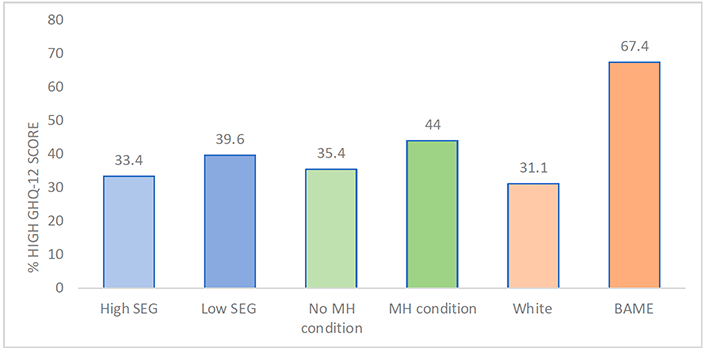
Chart description:
33.4% of those in the high SEG and 39.6% of those in the low SEG reported high levels of psychological distress. 35.4% of those with no pre-existing mental health condition and 44.0% of those with a pre-existing mental health condition reported high levels of psychological distress. 31.1% of White respondents and 67.4% of those who identified as BAME reported high levels of psychological distress.
Finally, this study also offers insight into the relationship between a person's health prior to the pandemic and their likelihood of meeting the cut-off for a possible psychiatric disorder, as indicated by a high GHQ-12 score. Two thirds (67.4%) of those with a pre-existing mental health condition recorded a high score, which was twice as many as those with no mental health condition (31.1%). Additionally, nearly half (47.5%) of those shielding had a high GHQ-12 score, which was over 12% more respondents than those not shielding (34.9%). Interestingly, the high-risk group (i.e., aged 70+ and/or an underlying health condition) reported lower rates of high GHQ-12 scores for a possible psychiatric disorder (27.9%) compared to those not in a high risk group (37.9%). One possible explanation for why the 'high-risk' group in the study sample might report lower rates is that the 'high risk' group is primarily made up of those aged 60+ (73.7% aged 60+ compared to 17.8% in the non-high risk group) and overall, this older age group reported lower rates of mental ill-health indicators and appears to be more protected for mental health.
3.5. Mental wellbeing
Mental wellbeing is an important indicator of mental health and can indicate how protected an individual may be from mental health problems such as depression and anxiety. Wave 1 of the SCOVID Mental Health Tracker Study measured a respondent's mental wellbeing using the Short Warwick-Edinburgh Mental Well-being Scale (SWEMWBS). This scale measures the frequency of thoughts and feelings of mental wellbeing over the past two weeks; includes items such as feelings of optimism, feelings of being useful, and feeling that one is thinking clearly.
For the Short Warwick-Edinburgh Mental Well-being Scale (SWEMWBS)[8], a score is created for each individual by adding together their responses to each question. The scores range from 7 (indicating very low wellbeing) to 35 (indicating very high wellbeing), therefore a higher score suggests better mental wellbeing. The scale was not designed to identify individuals with exceptionally high or low levels of mental wellbeing so cut off points have not been developed. Therefore, throughout this section average mean scores are reported for each of the subgroups to compare levels of mental wellbeing between groups.
Although there are no pre-COVID-19 average SWEMWBS scores for comparison in this sample, the Health Survey for England (2012), which drew on a sample of over 7,000 adults, found an average score of 23.61. This score is higher than the average mean score of 21.28 reported by the respondents in the Wave 1 SCOVID Mental Health Tracker Study. This suggests that in comparison to previous studies, mental wellbeing was lower during Wave 1.
In looking more closely at the data, some differences on mental wellbeing by age and sex emerge (see Table 3.5). The data suggests that older adults reported higher mental wellbeing than young adults. More specifically, respondents in the older age group (60+ years old) reported a higher mental wellbeing mean (23.82) than those aged 30-59 years (20.77), and compared to the younger age group (18-29 years), who scored the lowest (19.13). Further, although the mean mental wellbeing score among men was slightly higher (21.55) than women (21.07), this difference was not statistically significant.
| 18- 29 years (n=576) | 30- 59 years (n=1174) | 60+ years (n=749) | Total (n=2499) | |
|---|---|---|---|---|
| All adults | 19.13 | 20.77 | 23.82 | 21.31 |
| Men | 19.66 | 21.23 | 23.60 | 21.55 |
| Women | 18.56 | 20.37 | 24.02 | 21.07 |
Beyond age and sex, differences in respondents' backgrounds correlated with different mean SWEMWBS scores, as illustrated in Figure 3.5. For example, respondents in the higher SEG scored significantly higher (21.84) on the mental wellbeing scale than those in the lower SEG (20.40). Among different ethnicities, White people scored higher mean mental wellbeing scores (21.36) in comparison to those of BAME backgrounds (19.63), although it should be noted that the BAME group made up a very small proportion of the sample (4.9%) and therefore this findings should be considered carefully.
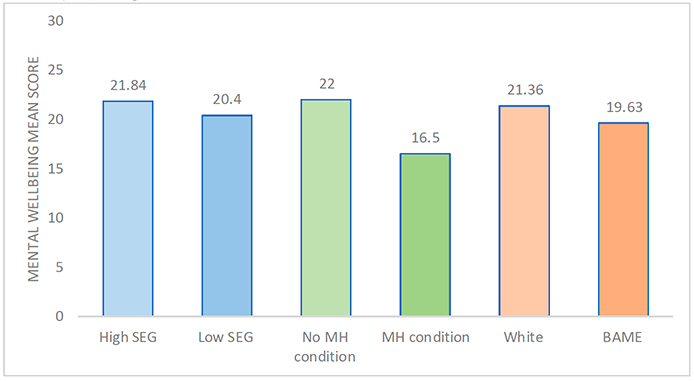
Chart description:
The mean mental wellbeing scores for those in the high SEG is 21.84 and for those in the low SEG is 20.4. The mean mental wellbeing scores for those with no pre-existing mental health condition is 22.0 and for those without a pre-existing mental health condition is 16.5. The mean mental wellbeing scores for White respondents are 21.36 and for those who identify as BAME is 19.63.
Differences in occupation, financial, and home life circumstances also appear to correlate with mental wellbeing scores and indicate that those who have less responsibilities and more financial security have higher mental wellbeing. For example, respondents who do not have a dependent under 16 years old in the household scored significantly higher on the mental wellbeing scale (21.51) than those who do have a dependent under 16 years old (including under 5 years) (20.55). Additionally, non-carers or respondents who were a carer for less than 5 hours per week had significantly higher mean mental wellbeing scores (21.41) than those who are carers for 5 hours or more per week (20.30). From an occupational perspective, non-key workers reported significantly higher mean mental wellbeing scores (21.46) than key workers (20.54). Furthermore, those who did not experience any change in their working status reported higher mental wellbeing (21.75) than those who did experience change in their working status, such as being furloughed or losing one's job (22.77).
From a health perspective, there were also differences in mental wellbeing suggesting different subgroups may be more protected from mental health problems. Specifically, respondents who indicated having no pre-existing mental health conditions scored much higher on average on the mental wellbeing scale (22.00) than those with a pre-existing mental health condition (16.50), who scored the lowest of all the subgroups. Additionally, those identifying as high-risk (i.e., aged 70+ and/or having an underlying health condition) recorded higher mental wellbeing scores (22.87) than those not identifying as high risk (20.84). One possible explanation for why the 'high risk' group in the study sample might report higher rates is that the 'high risk' group is primarily made up of those aged 60+ (73.7% aged 60+ compared to 17.8% in the non-high risk group) and overall, this older age group reported lower rates of mental ill-health indicators and appears to be more protected for mental health.
3.6. Other mental wellbeing indicators
Wave 1 of the SCOVID Mental Health Tracker Study assessed a range of other indicators and correlates of mental health and wellbeing. These included feelings of defeat, entrapment, loneliness, resilience, social support, life satisfaction, and distress. This section provides a brief overview of these measures, and findings suggest that the subgroups most at risk of poor mental health and wellbeing are:
- Young adults (18-29 years)
- Women
- Those with a pre-existing mental health condition
- Those in the lower SEG
3.6.1 Defeat and entrapment
Feelings of defeat and entrapment are important indicators of mental health, and have been associated with depression, anxiety, and suicidal thoughts. Defeat is a feeling of powerlessness in life and entrapment is a feeling of being trapped by circumstances or your own thoughts. In the Wave 1 SCOVID Mental Health Tracker Study, we assessed defeat using the short form of the Defeat Scale (Gilbert & Allan, 1998; Griffiths et al., 2015) and entrapment using the short form of the Entrapment Scale (Gilbert & Allan, 1998; De Beurs et al., 2020). All respondents are given a score for each measure by adding together each question response, with 0 indicating no feelings of defeat or entrapment and 16 indicating a very high level of feelings of defeat and entrapment.
There are no cut-off scores for defeat and entrapment measures to demarcate high or low levels of defeat and entrapment, therefore an average mean score is used to compare differences between the subgroups. Investigating the subgroups, there were some differences in relation to age and sex on feelings of defeat and entrapment. For example, young adults' (18-29 years) mean scores on defeat (5.40) were more than twice as high as the 60+ age group (2.27), and those aged 30-59 years had a defeat score (4.45) nearly twice as high as those aged 60+ years. Similarly, for feelings of entrapment, young adults (18-29 years) scored higher on entrapment (5.30) than those aged 30-59 years (4.16), which was nearly 3 times as high as those aged 60+ years (1.84). Regarding the differences by sex, women reported higher mean scores on defeat (4.42) than men (3.55), and women reported higher levels of feeling entrapped (4.01) than men (3.38). This suggests that young adults and women were at higher risk for feeling defeated and entrapped during the COVID-19 pandemic and lockdown.
Other background and health factors appear to correlate with differences in feelings of defeat and entrapment. Respondents in the lower SEG felt more defeated (4.63) than those in the higher SEG (3.44). In addition, those in the lower SEG scored higher on entrapment (4.42) than those in the higher SEG (3.30). Moreover, respondents who indicated having a pre-existing mental health condition scored over 2.5 times higher on defeat (8.78) than those with no pre-existing mental health condition (3.31). Similarly, the entrapment mean score among those with a pre-existing mental health condition was over 3 times higher (8.88) than of those with no pre-existing mental health diagnosis (2.69).
3.6.2 Loneliness
Loneliness has been associated with poorer physical and mental health, and was a particular concern during the COVID-19 lockdown as people became physically isolated from friends and family. In Wave 1 of the SCOVID Mental Health Tracker Study, we measured loneliness using the UCLA Loneliness Scale (Hughes et al., 2014), which assesses 3 aspects of loneliness; namely lacking companionship, feeling left out, and feeling isolated from others. We asked people how often they felt each of these aspects of loneliness before the COVID-19 lockdown and during the 7 days prior to responding to the Wave 1 questionnaire.
A total loneliness score was created by adding the responses to each question together, creating a score between 3, indicating no loneliness and 9, indicating high levels of loneliness. As there is no cut-off score demarcating high and low loneliness, mean scores were reported when comparing the different subgroups in terms of perceived levels of loneliness pre-COVID-19 and reported levels of loneliness in the week preceding respondents' participation in the study, referred to as 'Wave 1' loneliness, or 'during lockdown'. The mean score for loneliness for the whole sample pre-COVID-19 was 4.67 and the mean loneliness score increased to 5.18 for Wave 1. This suggests that overall, people felt more lonely during the COVID-19 lockdown compared to before COVID-19.
There were a number of clear differences in terms of levels of loneliness by age and sex. For example, loneliness increased for both men and women from pre-COVID-19 to the Wave 1 period, however loneliness was higher for women than men both before and during the lockdown. Additionally, all age groups reported an increase in perceptions of loneliness from pre-COVID-19 to during lockdown, however this increase was higher for those in the older age group (aged 60+ years). Despite this, young adults had the highest levels of loneliness at both pre- and during COVID-19 lockdown.
Subgroup analyses indicated that respondents' background and health may also correlate with higher levels of loneliness. Overall, all groups felt that their loneliness levels had increased from pre lockdown levels. During Wave 1, respondents in the lower SEG reported higher mean loneliness scores (5.44) than those in the higher SEG (5.02). Additionally, those who identified as BAME reported more loneliness during the lockdown (5.68) compared to White respondents (5.16). Finally, individuals with pre-existing mental health conditions reported much higher loneliness during Wave 1 (6.43) compared to those with no pre-existing mental health conditions (4.99). This suggests that those with a pre-existing mental health condition were at particular risk of experiencing loneliness during the lockdown.
3.6.3 Resilience
How resilient a person is can be important for understanding their capacity to cope with difficulties and recover from hardship and stress. Being resilient can be protective for mental health problems, including depression, anxiety, and suicidal thoughts. This may be particularly important during the COVID-19 lockdown period as individuals will have experienced much more stress and uncertainty than normal, and those who are resilient may have greater capacity to recover from this stress. In Wave 1 of the SCOVID Mental Health Tracker Study, resilience was assessed using 4 questions from the Brief Resilience Scale (BRS; Smith et al., 2008).
Respondents received a total score by summing the responses to each question, and this ranges from 4, indicating very low resilience to 20, indicating very high resilience. As there are no cut-off scores to demarcate high and low resilience, mean scores were used to compare the different subgroups on resilience average. Respondents were asked to rate their perceptions of their resilience pre-COVID-19 lockdown and in the 7 days prior to responding to the Wave 1 questionnaire, referred to as Wave 1 resilience, or during lockdown. Across the whole sample, respondents felt their resilience had reduced marginally during the COVID-19 lockdown, as the mean resilience score decreased from 10.82 to 10.30.
The subgroup analyses reveal some differences in mean resilience scores by age and sex. Both women and men felt their resilience had decreased during lockdown, although women reported lower mean resilience than men overall. Specifically, mean resilience scores for women were 10.72 pre-COVID-19 and 9.95 during Wave 1, and men's mean resilience scores were 11.19 pre-COVID-19 and 10.73 during the lockdown. Similarly, levels of resilience decreased significantly over time for each of the age groups, with the older age group (60+ years) reporting the highest levels of resilience than both pre-COVID-19 and during Wave 1.
Respondents' perceptions of their resilience and ability to cope with stress varied by background and health status. All groups reported that their perceived resilience had reduced a little from pre-COVID-19 levels. In addition, resilience was higher for those in a higher SEG (10.71), compared to the lower SEG (9.91) during lockdown. Individuals with a pre-existing mental health condition also reported significantly less resilience during Wave 1 (6.41) compared to those with no mental health condition (11.0).
3.6.4 Social support
Questions in the Wave 1 SCOVID Mental Health Tracker Study assessed sources of emotional and physical support and feelings of connection to those around you. Good support networks are important to protect against poor mental health, including against depression, anxiety, and suicidal thoughts. Social support was measured using four questions from the ENRICHD Social Support Instrument (ESSI; Mitchel et al., 2003) that assess how often an individual feels they currently have emotional and physical support.
Responses are summed into a total score, with a potential range from 4, indicating low social support to 20, indicating very high social support. Therefore, higher scores represent higher levels of social support. There were some differences in perceptions of social support by age and sex. For example, individuals aged 60+ years reported the highest levels of social support (15.14), followed by those aged 30-59 years (14.03) and those aged 18-29 years (13.74). In contrast, there were no significant differences in social support between men (14.30) and women (14.32).
Respondents' background and health status also correlated with different levels of social support, with those most at risk of negative outcomes such as depression and anxiety reporting lower social support. Specifically, individuals in the higher SEG reported more social support (14.68) than those in the lower SEG (13.63). Additionally, those from a BAME background (13.46) reported lower mean levels of social support than people of a White (14.34) background. Finally, individuals with pre-existing mental health conditions reported the lowest levels of social support (12.25) compared to any subgroup, and much lower than those with no pre-existing mental health condition (14.6). This suggests that those with a pre-existing mental health condition, in particular, have less sources of social support, a key protective factor for poor mental health.
3.6.5 Distress and stress
Distress is a feeling of acute anxiety and pain, and it is a correlate of current and future mental wellbeing. To measure levels of distress, we asked respondents to indicate on a 10-point scale how distressed they had felt in the past week, on a range of 0, indicating feeling no distress, to 10, indicating feeling extreme distress. For the whole sample the average level of distress was 3.81, which suggests mild levels of distress on average. As there is no cut-off for high and low distress, the subgroups are compared on their average mean scores.
Different levels of distress were found for age and sex. Specifically, women reported higher levels of distress in the week prior to the Wave 1 questionnaire (3.19) than men (2.36). Additionally, levels of distress varied across the different age groups, with young adults (18-29 year olds) reporting the highest levels of distress (3.97), followed by 30-59 year olds (3.13). The lowest levels of distress were reported by the 60+ group (1.38), whose levels of distress were half that of the younger age groups.
Levels of distress varied according to respondents' background and health. For example, as shown in Figure 3.6 those from lower SEG reported a significantly higher mean distress score (3.12) than those in the higher SEG (2.60). Individuals from BAME groups reported higher levels of distress (4.13) than those from the White ethnic group (2.74), although the BAME group made up a very small proportion of the sample (4.9%). Of all the subgroups, the highest levels of distress were seen in those with a pre-existing mental health condition (5.13), which was more twice the level of distress in those with no previous mental health diagnosis (2.45).

Chart description:
The mean distress scores for those in the high SEG is 2.6 and for those in the low SEG is 3.12. The mean distress scores for those with no pre-existing mental health condition is 2.45 and for those without a pre-existing mental health condition is 5.13. The mean distress scores for White respondents are 2.74 and for those who identify as BAME is 4.13.
Sources and outlets for stress
Experiences and outlets for stress for all respondents are summarised in Table 3.6. Looking at sources of stress, around a quarter of respondents reported worrying about money (25.2%) and almost half of respondents felt cut-off from their friends and family at the time of the Wave 1 questionnaire (45.8%). Additionally, just over 10% felt that they did not have enough space in their home (12.2%) and were arguing more with people they live with (12.8%). Some outlets for stress were reported, with a quarter of people feeling able to connect with nature (27.5%) and being able to enjoy spending time with family (25.1%). The findings suggest that individuals were not experiencing only stressors, or only outlets for stress, but instead experienced an overlap of these factors.
| Item | % |
|---|---|
| I feel cut off from my friends and family at the moment | 45.8 |
| I have been sleeping badly | 35.2 |
| I have less of a sense of purpose at the moment | 30.1 |
| I am able to find ways of connecting with nature | 27.5 |
| I am worrying about money | 25.2 |
| I am enjoying spending more time with my family | 25.1 |
| I am finding the current restrictions on socialising difficult to cope with | 23.1 |
| None of these | 15.1 |
| There is not enough space in my home | 12.2 |
| I have been having more arguments with the people I live with | 12.8 |
| Husband/wife/partner | 8.7 |
| Child (including stepchildren) | 2.9 |
| Parent | 2.2 |
| Other family | 1.2 |
| House/flatmate or lodger | 0.3 |
The reporting of sources of stress varied by respondents' age and sex. Overall, the older age group (60+ years) reported fewer sources of stress than the younger age groups (18-19 years and 30-59 years). For instance, 45.1% of 18-29 year olds said they had been sleeping badly compared to around a quarter (26.5%) of the 60+ group, and both the younger age groups were more likely to report worrying about money (35.6% of 18-29 year olds and 31.0% of 30-59 year olds) than the 60+ group (8.1%). Around a fifth of 18-29 year olds felt there was not enough space in their home (22.1%) and had been arguing more with those they lived with (22.1%), at rates higher in comparison to older groups. Additionally, women were slightly more likely to report feeling cut off from friends and family (48.7%) compared to men (42.7%). Women felt that they were struggling with the restrictions on socialising (25.7%) more than men (20.3%). Additionally, women were also more likely to report poor sleep (40.9%) compared to men (29.2%) as well as having less of a sense of purpose (35.7%) compared to men (24.5%). Further, women were more likely to report feeling there was not enough space in the home (14.1%) compared to men (10.1%) and an increase in arguments with those they lived with (16.4%) compared to men (8.8%).
3.6.6. Life satisfaction, worry and rumination
In the Wave 1 SCOVID Mental Health Tracker Study, respondents were asked about their current life satisfaction with the question 'All things considered, how satisfied are you with your life as a whole nowadays?' They were asked to rate their life satisfaction on a scale from 0, indicating extremely dissatisfied to 10, indicating extremely satisfied. The average mean life satisfaction for the sample was 6.3, which suggests that overall respondents were moderately satisfied with life. Although there is no pre-COVID-19 data on this scale, the Scottish Health Survey (2018) found that people reported an average mean score of 7.7 overall, which is higher than the mean score reported in Wave 1.
In the wave 1 SCOVID Mental Health Tracker Study, the highest level of life satisfaction was reported by the 60+ group. The lowest levels of life satisfaction were reported by respondents with pre-existing mental health conditions.
Respondents were asked about their worry and rumination about COVID-19, as this is likely to have an impact upon their mental health and wellbeing. Worry is defined as negative, repetitive thoughts about future events which have the potential to be stressful or upsetting, and rumination is defined as negative, repetitive thoughts about upsetting emotions or events which have happened in the past (including today).
Respondents were asked how often, in the past two weeks, they worried or focused on COVID-19-related things that may happen in the future. COVID-19-related worry was measured on a scale ranging from 1, indicating never to 7, indicating very often, meaning that the higher the score, the more often respondents tended to be worried about COVID-19-related issues. Overall, respondents scored an average of 3, which indicates mild worry about COVID-19. Older respondents (60+) had lower worry than the younger respondents (18- 29 and 30-59 year olds). Women scored slightly higher than men, those in the BAME group scored higher than White respondents, and respondents with a mental health condition also scored significantly higher than those without a mental health condition. No differences were found between socioeconomic groups.
To measure COVID-19 rumination, respondents were asked how often, in the two weeks prior to the Wave 1 questionnaire, they ruminated over COVID-19-related things that had happened to them or upset them in the past. COVID-19-related rumination was measured in frequency through a scale ranging from 1, indicating never to 7, indicating very often, meaning that the higher the score, more often respondents tended to ruminate about COVID-19-related issues. Overall, respondents scored an average of 3, suggesting mild rumination. Older adults scored significantly lower than middle-aged and younger adults. Women scored slightly higher than men, those in the BAME group scored higher than White respondents, and respondents with a mental health diagnosis also scored significantly higher than those without a mental health condition. No differences were found between SEGs.
Contact
Email: Social_Research@gov.scot