National cancer plan: progress report - August 2022
Scotland's national cancer plan comes to completion in March 2023. This report uses insights from the available evidence to update on progress against all 68 actions in the plan as at 31 August 2022.
Data on Cancer in Scotland
Definition of Data Areas and Subsets
The National Cancer Plan committed to capturing and analysing a number of data areas and subsets, with some in development. These data are captured in order to monitor actions and make evidence-based decisions in the ongoing recovery response. They will also illustrate the indirect impact of the COVID-19 pandemic on individuals with suspected or confirmed cancer, including their referral and wait for services.
Data on cancer incidence, cancer stage distribution, waiting times and mortality are included here to provide context for later action updates. Action updates incorporate data on screening, diagnosis and treatment to support this report on progress. Most data are taken from publications released by Public Health Scotland (PHS) since March 2020. This report has collated data that was available up to August 2022.
In addition to the statistics gathered by Public Health Scotland, Quality Performance Indicators (QPIs) are used across NHS Scotland to monitor performance. The overarching aim of the cancer quality work programme is to ensure that activity at NHS board level is focussed on those areas that are most important in terms of improving survival and patient experience whilst reducing variance and ensuring safe, effective and person-centred cancer care. Links to the Quality Performance Indicators for different tumour types can be accessed via Healthcare Improvement Scotland web pages.
Most data are derived from the Scottish Cancer Registry, with the exception of the Detect Cancer Early Staging figures that use QPI audit information to provide the most recent information from Health Boards. Cancer Registration is the collection, maintenance and management of data on every new diagnosis of cancer occurring in a population. The Scottish Cancer Registry database holds information on all the new cancer cases registered since 1958 when the registry began in Scotland.
This data landscape is summarised in the table below.
Table 1: Cancer datasets and source organisations in Scotland
Source Organisation
Care Opinion
Cancer Dataset
Patient and carer experiences of services
Source Organisation
Health and Social Care Alliance Scotland
Cancer Dataset
Source Organisation
Healthcare Improvement Scotland (HIS)
Cancer Dataset
Quality Performance Indicators (QPIs)
Information on all new cancer cases registered in Scotland since 1958.
Original source of most PHS datasets
Source Organisation
Scottish Government
Cancer Dataset
Cancer Patient Experience Survey
Source Organisation
Public Health Scotland (PHS)
Cancer Dataset
Systemic Anti-Cancer Treatment (SACT) activity
The statistics presented in this report focus on quantitative data and evidence to understand the impact of the COVID-19 pandemic on service delivery and patient outcomes. While qualitative data about the experiences of people living with cancer and receiving palliative care are not included in this report of progress, such evidence has been used to guide longer-term recovery. For example, the analysis of Care Opinion is routinely captured and presented to the National Cancer Recovery Group. This analysis includes evidence to improve understanding of how to address persisting health inequalities.
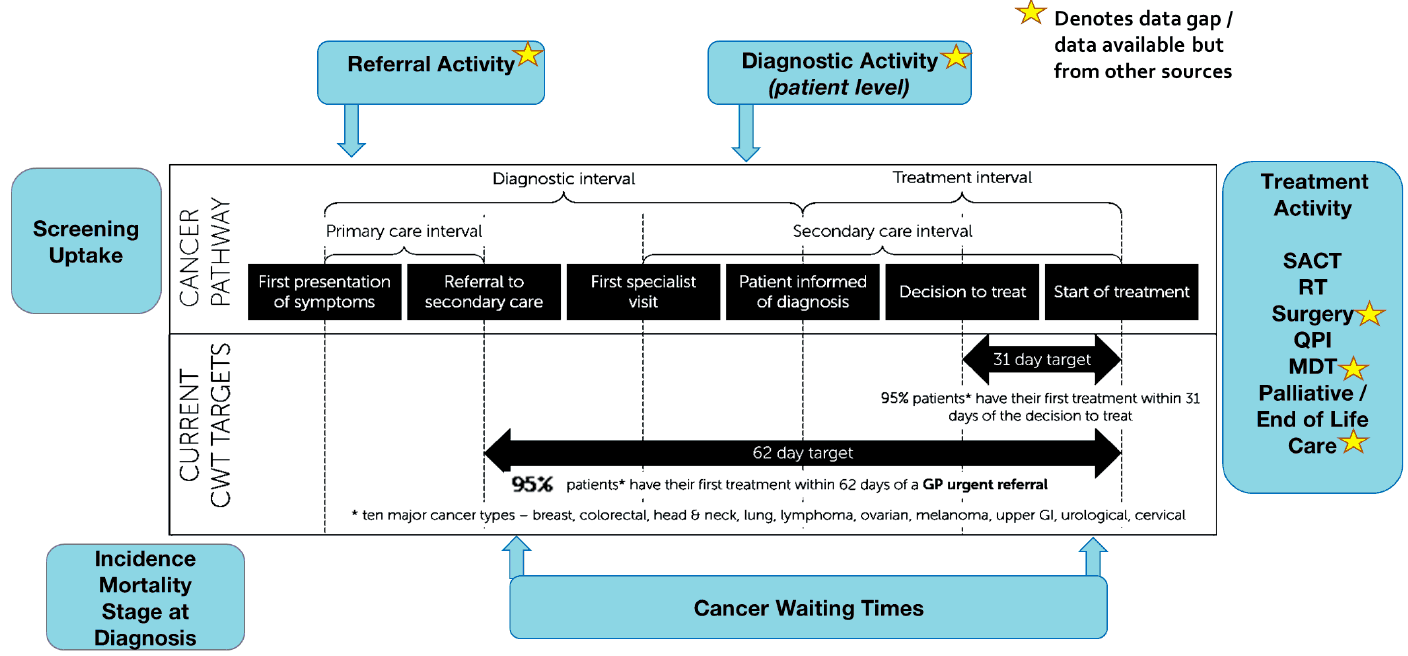
Figure 1 below shows the connection between cancer pathways and the metrics used in this report based on a graphic created by Cancer Research UK. The figure includes nationally available and published routine data sets that have been used in this report, in addition to data available from other sources or data gaps that Public Health Scotland are addressing. This figure is illustrative and not exhaustive of all the issues in the cancer data landscape. For instance, for ‘stage at diagnosis’ data, only three cancer sites stage data are routinely made publicly available.
Cancer Incidence in Scotland
Cancer incidence refers to the number of new cases of cancer diagnosed in a population over a specific time period, usually a year. The phrase ‘incidence rate’ refers to a standard measure of the frequency of cases within a specific period of time relative to a fixed population size, usually 100,000 people.
The most recent Public Health Scotland release of data on cancer incidence in Scotland (April 2022) provides an annual update of cancer incidence statistics in Scotland from January 1996 to December 2020. All cancer types are included. Public Health Scotland advises that, generally, cancer incidence statistics should be interpreted within the context of long-term trends. These reported statistics, however, demonstrate the impacts of the COVID-19 pandemic on cancer services.
Incidence of cancer between 2019 and 2020
- Overall, the rate (-9%) and number (-8%) of new cancers fell between 2019 and 2020. There were 30,395 cases in 2020, down from 33,156 in 2019. Most of the decrease is likely due to under-diagnosis caused by the pandemic. The reduction in cancer registrations is much larger than would have been expected had the pandemic not happened. See Figure 2 below.
- Many cancers showed bigger falls in incidence in 2020 compared with 2019:
- the top four cancers in Scotland fell: lung (7%), female breast (11%), prostate (10%) and colorectal (19%); while cervical cancer incidence fell by a quarter (24%).
- It also appears that pausing screening services led to an under-diagnosis of the early-stage breast (-20%), colorectal (-33%) and cervical (-45%) cancers compared with the number of early detected cancers in 2019.
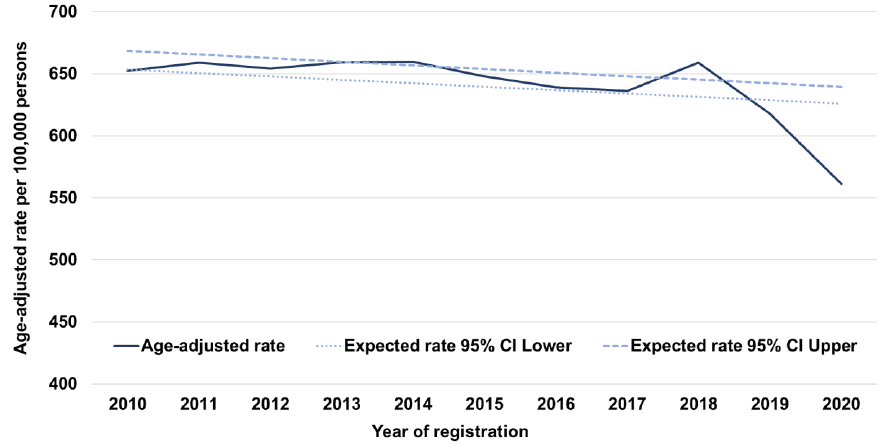
* Note truncated y-axis. ** The Poisson Regression Model is explained in the Public Health Scotland report on Cancer Incidence in Scotland mentioned above.
Incidence of cancer and health inequalities
- Overall, the pandemic appears not to have widened socio-economic inequalities in cancer incidence (33% higher in more deprived areas pre-pandemic compared with 30% in 2020). These short-term reductions in differences between most and least deprived are more likely to indicate a greater level of under-diagnosis of cancer because of the disruptions of the COVID-19 pandemic rather than greater falls in cancer occurrence in more deprived areas.
- Evidence is mixed across cancer types, however lung cancer diagnoses fell by 12% in people from the most deprived areas and by 5% in the least deprived areas. However, some cancer types fell to a greater extent in people from less deprived areas. Cervical cancer diagnoses almost halved (46% reduction) in the least deprived areas but fell 16% in the most deprived areas.
Summary of key points
After many years of increases, figures on new cancer diagnoses highlight decreases in numbers in 2020. Nearly 2,800 fewer cancer diagnoses were made in 2020 compared to the previous year – a fall of 8%. Even larger decreases have been recorded for specific cancers – diagnoses for colorectal and cervical cancer fell by a fifth and a quarter, respectively.
Outcomes from cancer are better when diagnosed at the earliest stage. However, it appears that the pandemic had a greater effect on these more treatable cancers. Diagnoses of early-stage cancer decreased more than for late-stage disease. Early-stage breast, bowel and cervical cancer diagnoses probably fell most because of the pauses in cancer screening programmes (see information about screening).
A supporting statement by Public Health Scotland on cancer incidence concluded that the COVID-19 pandemic had a huge impact on all aspects of cancer control in Scotland, causing widespread disruption from the end of March 2020. All cancer screening programmes were paused for several months and urgent referrals for suspected cancer fell substantially as patients followed the 'Stay at home; protect the NHS' message. Patients being less likely to seek help and delays in investigations may have led to people who developed cancer symptoms during 2020 not being diagnosed. Some will have died of COVID-19 before they were diagnosed with cancer in 2020.
Cancer Stage Detection
When the first national lockdown due to COVID-19 was imposed in March 2020, clinical services within primary, secondary and tertiary care were severely affected in numerous ways. Public Health Scotland has documented measures that will have impacted on the Detect Cancer Early programme. In addition to the impacts of the pause to cancer screening programmes, delays in investigations and patients being less likely to seek help, there was a significant shift in GP appointments from face to face to telephone, possibly making it more difficult to elicit signs and symptoms of some cancers. Further, there was confusion caused by the overlapping 'persistent cough', breathlessness and fatigue symptoms that could indicate either COVID-19 or lung cancer, which may have led to some referrals for lung cancer being delayed.
Public Health Scotland have released data examining the impact of COVID-19 on the cancer staging distributions. The report focuses on 2020 Q2 - Q4 data (April – December 2020) in comparison with the expected numbers of people diagnosed with early stage disease (Stage 1) using the most recent pre-pandemic Detect Cancer Early (DCE) data (2018 and 2019). The report presents data analysis published by Public Health Scotland from the DCE audit dataset for patients diagnosed with cancer during the full two-year period 1 January 2019 to 31 December 2020.
The Detect Cancer Early programme aims to increase the proportion of people diagnosed with early stage disease (Stage 1). The programme concentrates on breast, colorectal and lung cancers, which collectively account for a significant proportion of all cancers diagnosed in Scotland.
The DCE figures presented below use the QPI audit data, as this provides the most up-to-date information. Therefore, these figures are not directly comparable to Public Health Scotland cancer incidence data, which uses information from the Scottish Cancer Registry. Data in the Scottish Cancer Registry are subject to change in future publications, as submissions may be updated to reflect a more accurate and complete set of data from NHS Boards.
Diagnosis of breast, colorectal and lung cancer from April to December 2020
- During the nine months of the pandemic in 2020 (April-December), there were 2,681 patients diagnosed with breast cancer, 1,958 patients diagnosed with colorectal cancer and 3,287 patients diagnosed with lung cancer. These numbers are 19% (breast), 25% (colorectal) and 9% (lung) lower than would have been expected in this period had the COVID-19 pandemic not happened.
- The fall in numbers in 2020 Q2 is due to the initial lockdown. In the remaining months of 2020, numbers of people diagnosed with breast and lung cancer started to return to pre-pandemic levels, although colorectal figures remain well below previous years. See Figure 3 below.
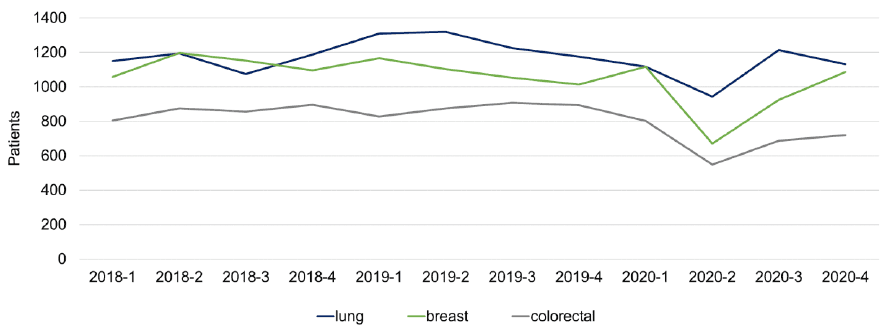
Stage of breast, colorectal and lung cancer diagnosis, April to December 2020
- For breast cancer, there were large falls in Stages 1 and 2 (35% and 15% respectively). In contrast, there were small increases in Stages 3 and 4 (5% and 7%), with the biggest increase seen for those of unknown stage (34%).
- For Colorectal Cancer, there were substantial drops (30% and more) in the numbers diagnosed with Stages 1, 2 or 3 colorectal cancer; whereas there was only a 4% drop for Stage 4 (also known as metastatic disease) colorectal cancer.
- For Lung Cancer, there were falls of 11%-13% for Stages 1, 2 and 3; but only a fall of 4% for stage 4 diagnoses, which was only lower than expected in April 2020.
Summary of key points
In the second quarter of 2020, during the first lockdown, there were sharp falls in the numbers of people being diagnosed with breast, colorectal and lung cancers. In the remaining months of 2020, the numbers of people diagnosed with breast and lung cancer started to return to pre-pandemic levels, although colorectal figures remain well below previous years. For breast cancer, the most substantial reduction occurred in earlier stages of cancer (Stages 1 and 2), with small increases in the numbers diagnosed with later stages of cancer (Stages 3 and 4). For colorectal cancer and lung cancer, there was a substantial reduction for Stages 1, 2 and 3, with a smaller decrease in the numbers diagnosed with Stage 4 cancer.
Cancer Mortality
Cancer mortality refers to the number of deaths from cancer in a population over a specific time period, usually a year. The phrase ‘mortality rate’ refers to a standard measure of the frequency of deaths within a specific period of time relative to a fixed population size, usually 100,000 people.
Using death registration data supplied by the National Records of Scotland (NRS), Public Health Scotland has released analysis to provide some interpretations of the risk factors that cause cancer and changes in survival for the most common causes of cancer death in 2020.
While interpretation of cancer mortality statistics should always be within the context of long-term trends, these statistics provide an opportunity for cancer mortality to be considered within the context of the COVID-19 pandemic.
Mortality statistics are different from the analysis of "age-standardised net survival", which measures the survival of cancer patients after taking into account the background mortality that they would have experienced if they had not had cancer. The latest cancer survival statistics released by Public Health Scotland capture data on people diagnosed with cancer during 2015 to 2019. Data on those diagnosed in 2020 will be available for future releases.
Numbers of deaths from cancer registered in Scotland in the last decade
- The number of deaths has increased over the last decade. This is largely because the number of older people, who are at greater risk of developing cancer, has increased and as such the number of cancer cases increased. See Figure 4.
- The age-adjusted cancer mortality rate for all cancers combined has decreased by 11% over the 10-year period of 2010-2020, with a greater decrease in males than in females (decreases of 13% and 7%, respectively).
- Of the most common cancers, liver cancer had the biggest increase in mortality rates in the last decade (38%). Survival from liver cancer is poor in most cases. The main risk factors for liver cancer are obesity, alcohol and infection with hepatitis B and C viruses.
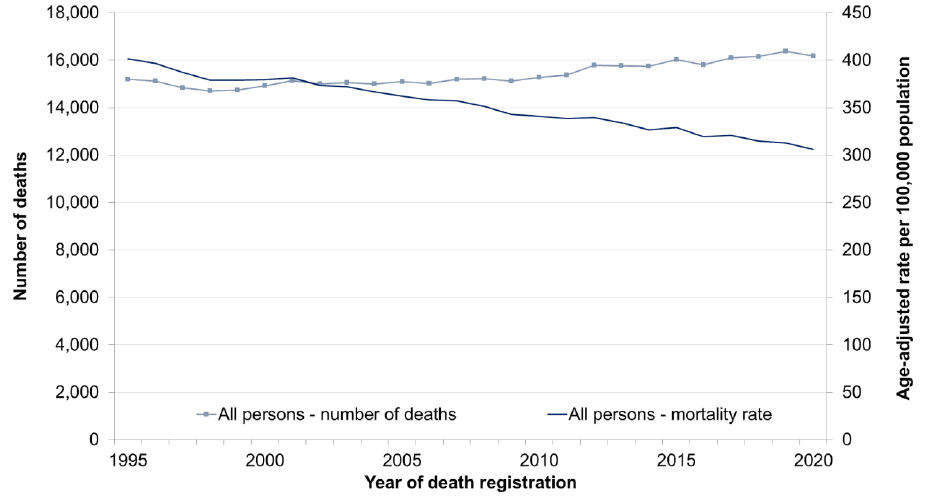
Numbers of deaths from cancer registered in Scotland during 2020
- There were 16,184 deaths from cancer (excluding non-melanoma skin cancers).
Most common cause of death from cancer in 2020
- Lung cancer continues to be the most common cause of death from cancer in Scotland (3,874 deaths in 2020). Nearly a quarter of all deaths from cancer in Scotland are attributed to lung cancer which is more than double that of colorectal cancer, the next most common cause of death from cancer.
Mortality rates for cancers in 2020 and the relationship with deprivation
- Considering all cancers combined, mortality rates were 78% higher in the most deprived areas compared with the least deprived. The most deprived areas have incidence rates that are 34% higher than the least deprived areas. This suggests that a combination of higher incidence and poorer survival from cancer in more deprived areas contribute to the excess mortality from the disease.
Summary of key findings
Cancer mortality, reflecting disease incidence and survival, continued to decline in 2020. Lung cancer was the most common cause of death from cancer. Deprivation continues to have a major influence on cancer mortality rates, just as it does with early detection and diagnosis. The impact of socioeconomic deprivation that is evident in the detection and diagnosis of cancer during this period is also evident in mortality rates. While the statistics here are considered in the context of the pandemic, any reductions in cancer diagnoses and treatment in 2020 are unlikely to have affected mortality that year. It will take several years to understand the true impact of the disruption to services on cancer mortality.
Contact
Email: CancerPolicyTeam@gov.scot