Strokes: progressive stroke pathway
The progressive stroke pathway, produced by the National Advisory Committee for Stroke (NACS), sets out a vision of what progressive stroke care in Scotland should comprise.
2. Introduction
Stroke develops as a result of problems with the blood vessels supplying blood to the brain.
There were 3,754 deaths in Scotland in 2019 where cerebrovascular disease, including stroke, was the underlying cause. While there has been a decrease in deaths due to stroke over the last decade, it is important to note that it remains a leading cause of death and the leading cause of disability in Scotland. This highlights that there is still work to do to improve prevention of, and outcomes from, stroke and to ensure that people across Scotland have equitable access to treatment and care.
Stroke remains a national clinical priority for Scottish Government. The 2019/20 and 2020/21 Programmes for Government made a number of commitments on stroke, including commitments to develop a national thrombectomy service and to 'scope out and define what a progressive stroke service looks like'.
This document defines a progressive stroke pathway in the Scottish context and sets out a vision of stroke services in Scotland. It has been produced by the National Advisory Committee for Stroke (NACS) in collaboration with the groups and individuals outlined in section 13 (Acknowledgements)We are grateful to the many health care professionals who shared their expertise with us, and to the National Stroke Voices who shared their lived experience of stroke to support the development of this document. A refreshed Stroke Improvement Plan will follow to support in the delivery of this vision.
The infographic below depicts an overview of the 'Progressive stroke pathway' defined in this document. This pathway includes prevention, recognition of stroke, transfer to hospital, hyperacute and acute care through to rehabilitation and supported self-management.
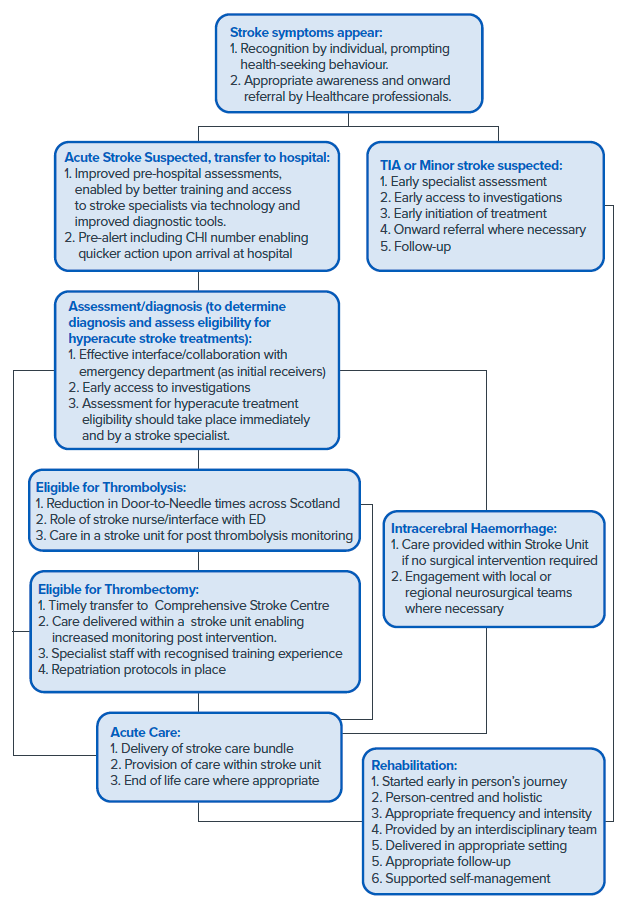
There are number of principles underpinning delivery of a progressive stroke pathway. These include the principles of Realistic Medicine, the importance of good information technology (IT) and digital systems to facilitate seamless delivery of care, and an effective research environment.
2.1.1 Realistic Medicine and shared decision making
Delivery of a Realistic Medicine approach means ensuring that people who experience stroke are supported to take part in shared decision making about their treatment and care, to ensure that what matters to them is at the heart of the delivery of care throughout the whole pathway.
This should be incorporated into all aspects of the progressive stroke pathway. Specific shared decision-making tools, including those which facilitate sharing of individualised information about patients' diagnosis, prognosis and treatments and goal setting, can support such an approach.
Involvement of specific healthcare staff such as speech and language therapy for patients with communication difficulties, and clinical psychology for those with cognitive problems, can further enable communication and shared decision making.
2.1.2 Information technology (IT)
The delivery of a progressive stroke pathway is facilitated by digital health systems which facilitate networking between clinicians, the use of artificial intelligence (AI) in decision making, the ability to support the movement of patients across different NHS Boards and enable digital models of care to provide people with stroke access to remote care and self-management tools based on their needs and preferences.
In a progressive stroke pathway, stroke services should have access to systems which:
- Support shared electronic health record keeping, reduce duplication and allow information sharing across a network of care along the whole pathway.
- Plan, prompt and record important aspects of care digitally to optimise delivery whilst making best use of clinicians' time.
- Support secure communication (voice, video, text, shared documents and images) between clinicians working across networks.
- Alert a responsible clinician or team to referrals or abnormal investigations to maximise safety and minimise delays.
- Capture data in real-time for audit/quality improvement and monitoring as a by-product of clinical care.
- Support healthcare professionals in using "Tailored Talks". This is a tool which facilitates the provision of tailored digital information and/or signposting for patients, their relatives and carers.
- Establish electronic documentation for remote consultation outcomes (e.g. Clinical Portal) when cases are referred and discussed. An audit trail of referrals, decisions and outcomes will help inform practice development and processes.
2.1.3 Research
Clinical research has an important function in delivering progressive stroke services. It helps to produce the knowledge on which to base more effective stroke services and ensures that healthcare staff are aware of the most up-to-date evidence and the latest developments in diagnostics and treatment. To facilitate continued clinical research activity, it is important to:
- Maintain the research infrastructures (e.g., University departments, NHS Research & Development, the Scottish Stroke Research Network (SRN) and Cochrane Stroke Review Group) which have helped make Scotland one of the leading countries for stroke research worldwide.
- Ensure that stroke patients and their families or carers can shape and participate in research in all parts of their pathway, wherever they are being cared for.
Contact
Email: Clinical_Priorities@gov.scot