Strokes: progressive stroke pathway
The progressive stroke pathway, produced by the National Advisory Committee for Stroke (NACS), sets out a vision of what progressive stroke care in Scotland should comprise.
11. Rehabilitation and long-term support
11.1 Stroke Rehabilitation
People who have had a stroke should have access to high quality, evidence-based, person-centred stroke rehabilitation which reflects their needs and preferences. Stroke rehabilitation aims to optimise function, reduce disability, promote independence and work alongside people and their families to achieve meaningful outcomes. It helps people to be as independent as possible in everyday activities and enables participation in education, work, recreation and meaningful life roles.
An inter-disciplinary team approach to stroke rehabilitation is essential, with the individual and their family or carers at the centre and given the opportunity to see the right professional at the right time to support their needs.
The United Nations has set out the right of people with disabilities to have access to rehabilitation to achieve participation and inclusion in all aspects of life. The World Health Organisation Rehabilitation in Health Framework highlights a tiered approach to rehabilitation which should be community based and focussed on the needs of the population.
Access to rehabilitation should be equally available to those in urban and remote and rural areas and across socio-demographic areas, using technology to deliver when appropriate.
Stroke rehabilitation should be based on a holistic biopsychosocial approach which seeks to understand the interactions of a diverse range of factors in a person's presentation (i.e. biological, psychological and social factors). This is essential for defining the aims of rehabilitation and to ensure that interventions are appropriate for, and meet the needs and preferences of, the individual. This shared understanding promotes interdisciplinary working between health and social care professionals to support effective and efficient stroke rehabilitation services.
The foundations of a progressive stroke rehabilitation service are underpinned by a holistic rehabilitation model and appropriate service infrastructure, leadership and expertise, as depicted in the infographic below. This model outlines the requirements of holistic patient assessment, interventions where individuals and practitioners work towards agreed goals, the importance of appropriate evaluation and an underpinning rehabilitation infrastructure that supports the provision of co-ordinated care.
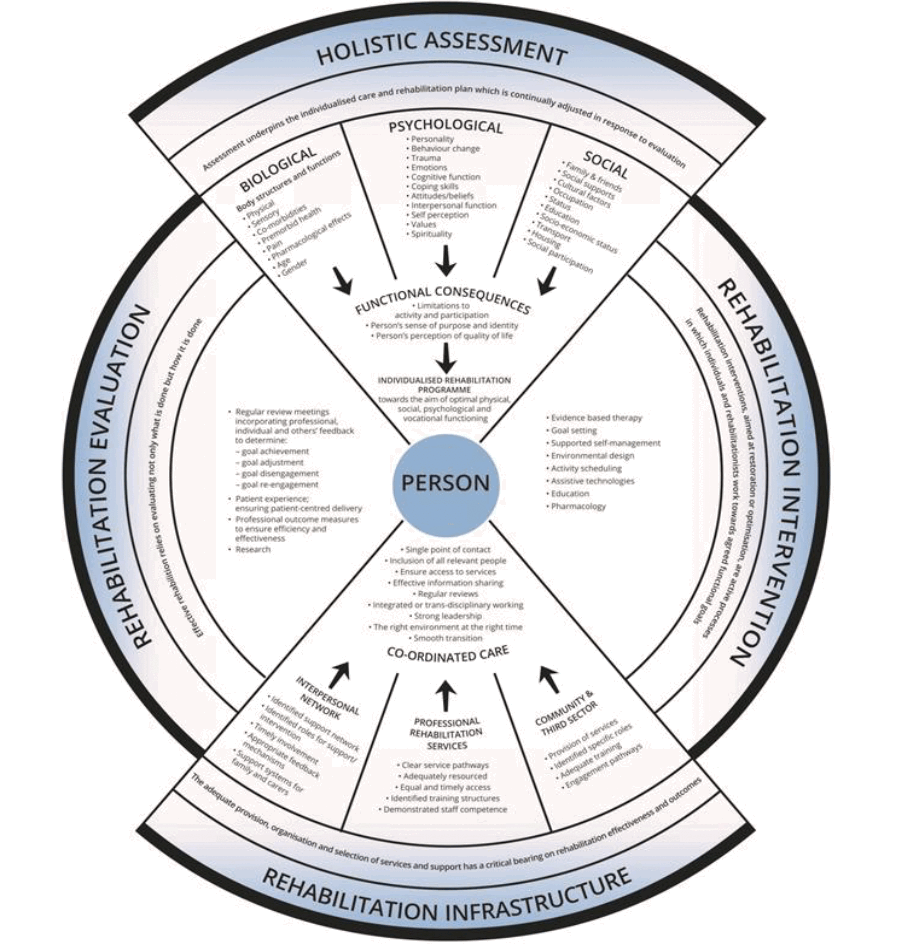
The core elements of rehabilitation include person-centred care, the setting of personal goals, and supported self-management. Personalised and evidence based therapeutic interventions delivered by stroke specialists should be offered to support recovery, adaptation to new functional status, and to support self-management and longer-term health and wellbeing.
11.1.1 Key principles of stroke rehabilitation
Person-centred - Person-centred care is about treating people as individuals and working with them to develop the knowledge skills and confidence to manage and make decisions about their own health and social care needs. Rehabilitation should be personalised, co-ordinated and enabling, and above all ensure that people are treated with dignity, compassion and respect. Person-centred rehabilitation considers the person's needs, capacity, preferences, wishes, values, lifestyle, environment, family and social circumstances. The rehabilitation team works in partnership with them to understand their priorities and to develop solutions.
Personal goals - Goal setting is the process by which the person with stroke (and their family or carers if they wish) and members of the stroke team identify individual goals which are meaningful, challenging and have personal value.
Supported Self-management - A person-centred approach in which the individual is empowered and has ownership over the management of their life and condition.
Co-ordinated Services- Areas in which Managed Clinical Networks (MCN's) operate with clear clinical and operational leadership are more able to connect services via clear service pathways. Stroke rehabilitation services should co-ordinate across clinical and service pathways and be tailored to individual needs based on a range of personal, environmental and social factors.
Rehabilitation team - Expertise from an interdisciplinary team who work in partnership with the person who has had a stroke and who collectively tailor rehabilitation input towards the person's goals. Where appropriate, this partnership should include family and carers.
Clinical Leadership - Clinical and service leadership should be provided by senior allied health professionals, medical, psychology and nursing staff, ensuring an equal focus on hospital and community rehabilitation pathways.
Appropriate care setting - In-patient rehabilitation is required for people with complex physical, cognitive, psychological and/or social needs, who could not be supported in a community setting. Rehabilitation of stroke patients in hospital should occur in an integrated stroke unit (a mixed acute and rehabilitation ward) or a specialist rehabilitation area. Early supported discharge (ESD) and community stroke rehabilitation services should be offered in a community setting whenever that best meets the needs and wishes of the patient.
Evaluation - Data on service delivery, patient outcomes and experiences should be collected systematically. Outcome measures used should be standardised, valid and reliable as well as being focused on what matters to patients,. The effectiveness of progressive stroke rehabilitation services will be reviewed via the Scottish Stroke Improvement Programme utilising rehabilitation data from the Scottish Stroke Care Audit and by at least one annual review.
11.1.2 Stroke Rehabilitation Service Provision
Stroke rehabilitation services should include inpatient rehabilitation, ESD and community stroke or neuro rehabilitation teams who work closely to ensure services are delivered in the most appropriate setting for each person's needs. This relies on having the right infrastructures in place, including sufficient access to rehabilitation professionals and close links with social care and the voluntary sector as part of an MCN.
Rehabilitation for people with stroke in all settings should ensure:
- That people receive a holistic assessment to determine their rehabilitation needs as quickly as possible.
- That the delivery of rehabilitation takes place in the most appropriate setting and at the right time for that person's needs.
To achieve this, stroke rehabilitation plans should be agreed and initiated in the acute phase and be available, according to need, along the entire stroke pathway.
The duration of stroke rehabilitation services should be led by the needs of the person who has had a stroke and be defined by their goals and should not be time limited. A clear life-long pathway for people to be able to re-engage with stroke rehabilitation services and to re-access specialist support should be available to patients and families.
It is important that families and carers are included in rehabilitation planning and goal setting, if agreed by the person who has had the stroke. If agreed, then carers should be
- Included in assessments to identify needs.
- Provided with tailored information about stroke and the caring role.
- Provided with advice, access to emotional support to adjust to their caring role and maintain their wellbeing.
- Signposted to peer support to reduce the impact of loneliness and social isolation if required.
Evidence supports increased frequency and intensity of therapy especially in the first six months post-stroke which can improve recovery rate and outcome. Provision of greater amounts of stroke therapy is associated with higher therapy and nursing staffing levels, a weekend therapy service and specialist stroke rehabilitation teams. Stroke rehabilitation services should therefore be available as required across the pathway seven days per week at an appropriate intensity with appropriate workforce skill mix.
Factors which impede the amount of therapy provision include time spent in information exchange and administration. Patient focussed reorganisation of working practices including shared documentation, and individual patient therapy timetabling is recommended to enable therapy provision in line with clinical guideline recommendations.
11.1.3 The Rehabilitation Team
Stroke rehabilitation services must include regular access to an inter-disciplinary team who work in a co-ordinated manner and collaborate towards common goals.
The inpatient stroke rehabilitation team should include stroke specialists in medicine, nursing, occupational therapy, physiotherapy, speech and language therapy, and dietetics. It should also ensure timely access to other specialist clinical services as required, such as orthotics, pharmacy, orthoptics, and social work. The psychological, emotional and cognitive effects of stroke should be understood and supported by the whole team. Specialist input from clinical psychology and neuropsychology should also be part of the core team and service provision throughout the patient journey from acute to longer term.
ESD and community stroke/neuro rehabilitation teams should include occupational therapy, physiotherapy, speech and language therapy, nursing and neuro/psychology, with easy access to other professionals as required.
Rehabilitation and recovery should be embedded within all aspects of stroke rehabilitation by all team members on a 24/7 basis. Teams should work to engage people in as much therapeutic activity (including specialist therapy interventions and self-practice) as required at a frequency and intensity that enables them to reach their rehabilitation goals.
The stroke rehabilitation environment should facilitate patient engagement in a range of physical, cognitive and social activities out with formal therapy time. This can be supported by staff, carers and volunteers. This whole system approach to stroke rehabilitation should be promoted to improve recovery and rehabilitation outcomes.
11.1.4 Rehabilitation settings
Inpatient stroke rehabilitation is required for those who have complex physical, cognitive and psychological needs which are unable to be managed in a community setting.
Community stroke rehabilitation can be offered by a range of services including ESD and community stroke/neuro rehabilitation teams, with varying intensity for up to seven days per week depending on the individual's needs.
All hospital in-patients with stroke who have mild to moderate disability should have the opportunity for early supported discharge which enables rehabilitation to commence in their home environment within one working day of hospital discharge and at an intensity and frequency that would be provided if they remained in hospital. To enable this, strong links are required between the inpatient and community rehabilitation teams,.
Regardless of the health board in which the patient receives acute stroke care, it is important that rehabilitation is provided in their local area. This should be facilitated by effective communication and clear referral pathways between health boards.
To ensure equitable access to ongoing support and self-management resources, all those who have had a stroke or TIA should be provided with high quality, tailored information at the point of discharge from outpatient clinic, emergency department or hospital and be followed up as soon after discharge as possible and thereafter, as indicated by the individual's needs, by a community stroke nurse or other stroke specialist healthcare professional to provide further specialist advice and support.
Everyone with residual difficulties following a stroke on discharge from hospital should be provided with a documented plan for community rehabilitation and self-management support.
In addition, everyone who has experienced a stroke should receive a review by a stroke specialist health care professional within six months of their event.
11.1.5 Key interventions delivered by a progressive stroke rehabilitation service
Many aspects of stroke rehabilitation require a tiered approach whereby aspects of care are the responsibility of the whole interdisciplinary team with specialists within the team focusing on more complex presentations. Each stroke rehabilitation network should have clearly defined pathways about how these services are provided.
Activities of Daily Living
Activities of daily living (ADL) include personal activities, e.g., washing and dressing; domestic activities, e.g., cooking and housework, and extended activities, e.g., work, driving and leisure. People experiencing difficulty with ADLs should be seen by an occupational therapist for assessment and the implementation of a personalised intervention programme. Evidence supports continued ADL training from occupational therapy and interventions can include direct training in an activity, training in adapted methods of performing an activity and the training in the use of adaptive equipment, assistive technology and environmental adaptation to maintain independence.
Arm function
Rehabilitation interventions that comprise intensive, graded practice of tasks and activities that focus on an individual's goals have been shown to be effective. Progressive arm rehabilitation, usually provided by occupational therapists and physiotherapists, comprises comprehensive assessment, person-centred goal setting and the provision of a structured, goal-orientated programme of intensive practice. This may include assistive technologies (e.g., functional electrical stimulation, mirror-box therapy and virtual reality) as well as involving their affected arm in activities of daily living as much as possible in order to increase the intensity of meaningful practice and to improve outcomes.
Bowel and Bladder rehabilitation
Bladder and bowel dysfunction (including urinary incontinence, faecal incontinence, constipation and nocturia) are common and can be persistent following stroke but are amenable to rehabilitation intervention. Progressive rehabilitation will feature structured assessment by a nurse to identify the type of bladder/bowel dysfunction, agreement of individual goals and a programme of mainly behavioural interventions targeted to the type of dysfunction, to support active recovery of bladder/bowel function and use of the toilet. Regular review of the rehabilitation programme and avoidance of containment approaches (including indwelling catheters) are key to recovery of independent bladder/bowel functioning and toilet use.
Balance, walking and mobility
Problems with balance, walking and mobility are likely to increase the risk of falls, deconditioning, becoming housebound and social isolation. People who have had a stroke should have their mobilisation needs assessed and once medically stable, they should be assisted to mobilise, overseen by a physiotherapist. Walking training should be task specific and include a cardiovascular component. Treadmill training with or without body weight support can improve walking and should be available for those who are able to walk independently. For those who are not able to walk independently after stroke, electromechanical-assisted gait training devices (i.e. automated electromechanical gait machines) together with physiotherapy can improve the ability to walk independently and this technology should be made available. Early access to orthotic assessment for the provision of an ankle foot orthosis (AFO) should be available, with reassessment when necessary, in order to facilitate walking and prevent falls. Functional electrical stimulation (FES) should be available to facilitate gait and prevent falls in those with persistent mild lower limb weakness.
Communication
Post-stroke communication disorders occur frequently. Aphasia and dysarthria each affect around a third of people following a stroke. People who are identified as having a communication disorder after a stroke should be assessed by a speech and language therapist and provided with an individualised rehabilitation programme using evidence-based interventions to reduce the impairment and/or support functional improvement and long-term adaptation. Such interventions may include group work, computer-based therapy, assistive technology and conversation partner training.
Cognition
Cognitive impairment is common following a stroke and can have a significant impact on social recovery and re-integration with overall poorer rehabilitation outcomes. Services should have a documented pathway for the identification and assessment of cognitive problems. Cognitive rehabilitation should be integrated into the broader rehabilitation programme and goals should include cognitive rehabilitation interventions with the aim of restoring, compensating or adapting for reduced cognitive ability.
Driving
A documented pathway should be available to advise on national and local services for further assessment and advice about resuming driving or alternative mobility options. Stroke service should ensure that driver status and intention to return to driving should be ascertained and advice and tailored information is made available.
Fatigue
Fatigue is commonly reported following stroke and can impact on longer term recovery and wellbeing. A range of physical and mental factors may contribute to fatigue and a documented pathway for the identification and assessment of fatigue and its impact on activity and participation should be available. Rehabilitation programmes should include strategies to anticipate and manage fatigue as well as education for patients and families/carers.
Pain management
Pain following stroke can be due to several causes including neuropathic pain, musculoskeletal pain and shoulder pain and subluxation. Each element requires specialised assessment and a range of evidence-based interventions which should be available in documented pathway.
Physical activity, exercise and fitness training
Physical activity, exercise and fitness training should be provided through partnerships between health and exercise professionals, the third sector and local authority services. Exercise and fitness training should begin, as appropriate, in hospital and continue in the community. It should be provided by therapists or exercise professionals who have evidence of stroke specific knowledge and skills to adapt and tailor exercise programmes for people after stroke.
Physical activity should also be encouraged. Many people who have had a stroke experience barriers to becoming more active and sedentary behaviour tends to persist after stroke,. Evidence-based counselling strategies are effective to encourage stroke survivors to engage and maintain physical activity after stroke and these should be provided as required along the entire stroke pathway.
Posture and movement – spasticity services
Stroke services should implement a systematic approach to identify all those who need specialist spasticity assessment and treatment. Stroke services should also implement a documented programme for prevention and management, including self-management, of post stroke spasticity. All those who need it will have access to a specialist spasticity service which may include Botulinum toxin injections, electromyography (EMG) or ultrasound guided approach, appropriate clinical expertise to deliver, and co-ordinated multidisciplinary community follow up including occupational therapy, orthotics and physiotherapy.
Positioning and seating
Following stroke, many people will find it challenging to control their position when in bed and when sitting in a chair. Effective positioning and seating is essential for reducing the risk of aspiration, falls, skin breakdown, and contracture development in addition to providing maximum comfort and supporting participation in ADL. All staff from statutory and voluntary sector organisations and carers involved along the whole pathway should be aware of correct positioning. People with stroke, their carers, and all services should have access to clinicians with training in postural management. Appropriate beds, specialist chairs and positioning equipment should be available from inpatient and community rehabilitation services when required.
Psychological Care (cognitive and emotional)
In the aftermath of stroke, patients and families experience a wide range of psychological, cognitive and emotional difficulties which impact profoundly on function and rehabilitation.
Stroke services should implement a documented programme for promoting awareness of, screening for and treatment of psychological consequences of stroke, led by a specialist clinical/neuropsychologist as detailed in the National Model of Psychological care for stroke. Psychological care should be available to all patients in line with local delivery plans.
Relationships and sexuality
Sexuality includes physical and psychosocial aspects of intimacy. Approximately 50% of individuals experience sexual dysfunction following stroke, however it is not commonly included as part of a rehabilitation programme. Services to address these aspects of life after stroke are variable and professional education is lacking. Education with regards to sexuality following stroke should be provided to the stroke rehabilitation team and specialised support should be made available to those who require it.
Swallowing
Post-stroke swallowing difficulties (dysphagia) are common and can persist long-term. Management of such difficulties should be led by a dysphagia specialist, such as a trained speech and language therapist (SLT), and should include evidence-based rehabilitation and restorative strategies which aim to improve oropharyngeal function. Management of swallowing difficulties will additionally include compensatory strategies, swallowing manoeuvres, sensory modification and texture modification of food and fluids as appropriate. All interventions should take into consideration the factors which may limit ability to participate, such as physical and cognitive impairment, as well as encompass shared decision-making and a shared responsibility for management of risk. There should be access to instrumental assessments such as videofluoroscopy and flexible endoscopic evaluation of swallowing (FEES) to determine the specific rehabilitation programme/management approach. There should also be pathways for people with long-term dysphagia to re-access services for review.
Technology and tele rehabilitation
Stroke rehabilitation services should include the use of robotics and software programmes which support rehabilitation interventions as appropriate.
Vision
Comprehensive assessment and rehabilitation services should be provided to all those with visual problems due to their stroke including:
- Comprehensive visual screening completed before discharge.
- Direct referral to appropriate professionals for assessment of suspected visual problems.
- Follow up to determine the level of spontaneous recovery of visual problems.
- Provision of treatment and rehabilitation, tailored to the specific visual problems by the most suitable profession in that locality (this may vary across NHS and Social Care areas).
- Provision of tailored information and clear explanation of visual problems, and their possible impact, at each possible opportunity.
- Ensuring individuals have knowledge of, and access to, relevant low vision services initiating direct referral if required.
Vocational rehabilitation
Stroke rehabilitation services should identify work status and offer advice, signposting and referral for specialised return to work support as appropriate.
A documented pathway should identify local and regional access to specialised vocational rehabilitation services.
11.2 Supported Self-Management and Longer-term support
Supported self-management and longer-term care & support should be an integral element of stroke rehabilitation pathway and should be provided in partnership with health, social care and the voluntary sector.
Supported self-management is a core component of person-centred care and is an interdisciplinary approach which supports people to develop skills, knowledge, and confidence to manage the impact of stroke and to maintain an ability to engage in meaningful activities and life roles.
Not everyone who experiences a stroke or TIA will have ongoing rehabilitation needs identified at the time of their discharge. However, feedback from people with lived experience was that often, this meant that there was a missed opportunity to identify routes to access support.
Everyone who experiences a stroke or TIA should receive tailored information provision and be signposted to community-based support and advice. It is important that people who have had a stroke or TIA are provided with the necessary skills, resources and support to continue self-management in the longer term along with management of other long-term conditions they may have.
There is considerable variation across the country in the longer-term support for people who have had a stroke. This may comprise nurse or other healthcare professional follow up, peer support groups and exercise classes. In some places these aspects of care are provided directly by NHS stroke services, in others they are commissioned from charities including Chest Heart and Stroke Scotland (CHSS) and the Stroke Association.
Primary care services are the main source of medical care for stroke survivors in the longer-term after their stroke. It is common practice that routine annual reviews for people with stroke take place alongside reviews of other long-term conditions. In addition, people who have had a stroke identify health issues that arise and contact primary care services for assessment.
Primary and secondary care services should communicate effectively to enable the provision of patient-centred care, for example primary care may identify a further rehabilitation need and refer the person back to the community rehabilitation team.
People with lived experience of stroke highlighted that a key issue was the lack of a 'joined up' approach, and outlined how important it would be to have a person who could support them by signposting to advice and support services, and act as a point of return for when issues arose further down the line in their journey.
''One of the big aspects is going to be having someone who is responsible for ensuring that the service is joined up. I think that's what's missing'' – National Stroke Voices participant.
It is therefore important that people who experience stroke are provided with clear and easily accessible contact information once discharged from community services, enabling the provision of continued advice, support and signposting. A clear life-long pathway for people to be able to re-engage with stroke services and re-access specialist support should be available to patients and families.
To ensure equitable access to ongoing support and self-management resources every person who has had a stroke should be contacted by a community stroke nurse or other appropriate stroke professional as soon as possible following their discharge from outpatient clinic, emergency department or hospital to provide review and an opportunity to access specialist advice and support.
11.3 Recommendations
1. Stroke rehabilitation services should be underpinned by a holistic rehabilitation model, appropriate service infrastructure, clinical leadership and expertise.
2. Stroke rehabilitation in all settings should be person-centred and optimise outcomes with evidence-based interventions, enabling appropriate long-term support and self-management.
3. Rehabilitation should be a process that begins as soon as a stroke is diagnosed and continues as long as required. The duration of stroke rehabilitation should be needs led and not time limited.
4. An early holistic assessment of a person's rehabilitation needs should be provided by specialist stroke teams and a personalised, documented rehabilitation and self-management plan agreed with the person who has had a stroke and, if they wish, their family/carers.
5. Stroke rehabilitation services must include a specialised and coordinated team who work in an interdisciplinary manner and collaborate towards common, person-centred goals.
6. The psychological, emotional, cognitive effects of stroke should be understood and supported by the whole team. Specialist input from clinical psychology and neuropsychology should be part of the core team and service provision throughout the patient journey from acute to longer term.
7. Evidence based stroke rehabilitation services should be available in inpatient and community settings seven days per week at an appropriate intensity, with an appropriate workforce skill mix.
8. Each stroke rehabilitation network should have clearly defined pathways about how key stroke rehabilitation interventions and services are provided.
9. Stroke rehabilitation services should be provided as part of a managed clinical network which includes inpatient rehabilitation services, ESD and community stroke or neuro rehabilitation teams who work closely with social care and the voluntary sector to ensure services are delivered in the most appropriate setting for each person's needs and ensure equity of service provision across all geographical and socio demographic areas.
10. Inpatient stroke rehabilitation is required for those who have complex physical, cognitive and psychological needs which are unable to be managed in a community setting.
11. Community stroke rehabilitation can be offered by a range of services with a range of intensities according to individual needs, including Early Supported Discharge and community stroke / neuro rehabilitation teams.
12. Clinical and service leadership should be provided by senior allied health professionals, medical, nursing and neuropsychology staff, ensuring an equal focus on hospital and community rehabilitation pathways
13. Every person who has had a stroke should be followed up by a community stroke nurse or other appropriate healthcare professional, as soon as possible following discharge from hospital and thereafter, as indicated by the individual's needs, ideally in their own home.
14. A clear lifelong pathway for people to re-engage with stroke rehabilitation services and re-access specialist support should be available to patients and families
15. A formal review should also be carried out for everyone who has experienced a stroke, six months post event, to provide another opportunity to access specialist advice and support, regardless of the rehabilitation needs identified at the time of their discharge from hospital.
16. People who have had a stroke should be signposted to relevant resources and support to continue self-management in the longer term along with management of other long-term conditions they may have.
17. Demonstration of a person-centred approach should be evaluated via the approach used by stroke rehabilitation services to deliver activities which are deemed to be central to person centred care e.g., regular holistic assessment of need; goal setting; supported self-management and family/carer involvement, as well as the patient experience of these activities and the treatment and communication they experience with the professionals working with them.
Contact
Email: Clinical_Priorities@gov.scot