Pandemic Flu: A Scottish framework for responding to an influenza pandemic
Pandemic Flu: A Scottish framework for responding to an influenza pandemic. This guidance was superseded by the UK Influenza Pandemic Preparedness Strategy 2011.
9 THE HEALTH AND COMMUNITY CARE RESPONSE
An effective well planned health and community care response is central to our aim of saving lives and reducing illness. TThe dual challenge for the health and community care response will be to deal with the increased demand for services, whilst also coping with the inevitable scarcity of professional skills and resources due to illness.
Depending on the severity of a pandemic, health and community care resources may be stretched far beyond their usual capacity. Therefore, although we must strive to maintain services as far as possible, the potential impact of a pandemic and the expected duration of one or more pandemic waves, will mean that available resources must be prioritised.
This section sets out the healthcare planning assumptions which should be used by responders, provides advice on the issues local planners should be considering and sets out the current status of work being taken forward centrally. Planning should also incorporate actions to be taken in the post pandemic phase to ensure that service recovery is built in and takes place as quickly as possible.
9.1 Aims
The health and community care aims are to reduce mortality and morbidity by:
- maintaining surveillance to detect the emergence of a novel virus strain or any illness attributable to it, monitor its spread and health impact, describe the illness and inform response
- providing prompt access to rapid and reliable diagnostic tests
- reducing the severity of illness and incidence of complications in infected individuals
- reducing disease transmission and rates of illness by applying individual and community infection control measures
- adjusting responses to reflect emerging epidemiological data
- developing surge capacity to meet expected demand, recognising that this will require a redefinition of boundaries between primary and secondary care
- making targeted and effective use of potentially scarce healthcare skills, facilities and resources
- reducing or ceasing non-essential activity as demand increases but maintaining essential care for emergencies or patients with chronic or other illnesses
- assessing all symptomatic patients rapidly and treating promptly with antiviral and other medicines if indicated
- providing effective treatment for those suffering complications
- educating the community and providing public advice and information
- vaccination, if and when suitable vaccines are available
- providing data to monitor the impact, effectiveness and adverse effects of interventions.
9.2 Key principles underlying planning and response
Health and community care organisations should apply the following general principles to their planning and response:
- Response arrangements should be based on strengthening and supplementing normal delivery mechanisms as far as is practicable
- Interventions will be applied where they achieve maximum health benefit, but may also be required to help maintain essential services
- Plans should be developed on an integrated multi-agency basis with risk sharing and cross-cover between all organisations
- Plans should encourage pan-organisational working, seeking to mobilise the capacity and skills of all public and private sector healthcare staff (including students and those who are retired), contractors and volunteers
- Although visiting all cases will not be possible, primary care plans should be based on influenza patients avoiding leaving home as far as possible
- Initial telephone-based assessment is likely to be necessary to meet demand
- Primary care response strategies should focus the available clinical capacity and skills primarily on treating those suffering with the complications of influenza or requiring other essential clinical care and assessing young children or patients in groups identified as being at particular risk
- Antiviral medicines should initially be available to all patients who have been symptomatic for less than 48 hours and ideally within 12-24 hours of reporting symptoms
- Response measures should maintain public confidence and feel fair
- Treatment and admission criteria should remain clinically based and hospital admission criteria should be applied in a transparent, consistent and equitable way that utilises the capacity available for the seriously ill and most likely to benefit
- Plans should recognise the need to respond to psychosocial issues and concerns such as anxiety, grief and distress and for sympathetic arrangements to manage additional fatalities.
9.3 Key planning assumptions for health and community care planning
To allow sufficient time to finalise and implement operational response arrangements, the Scottish Government Health Directorates will advise on the reduction of non-essential and elective NHS services and may begin to suspend some performance targets from the onset of UK alert level 2. Organisations should use the following planning assumptions to ensure that response arrangements are resilient and robust, but must be prepared to modify plans should emerging information vary.
9.3.1 Severity of illness
- Up to 50% of the population may show clinical symptoms of influenza (clinical cases) over the entire period of a pandemic (planning range 25% to 50%)
- up to 25% may develop complications (planning range 10% to 25% of cases)
- Up to 2.5% of those who become symptomatic may die (planning range 0.4 to 2.5% of cases).
- Up to 22% of influenza cases can be expected during the peak week of a pandemic wave.
- Up to 27.5% of symptomatic patients (including all symptomatic children under three) will require assessment and treatment by a general medical practitioner or suitably experienced nurse (planning range 13% - 27.5% of cases)
- Up to 4% of those who are symptomatic may require hospital admission depending on available capacity (planning range 0.55% to 4.0% of cases). Average length of stay for those with complications may be 6 days (10 if in intensive care).
9.3.2 Health and community care demand
- A short lasting pandemic of higher virulence would put greater strains on services than a more sustained pandemic of a lower virulence
- Hospitalisations and deaths will depend upon the age profile affected, virulence and specific complications associated with the pandemic virus, but demand is likely to be greatest in children and the elderly
- Total healthcare contacts for influenza-like illness could increase from around 90,000 during a 'normal' season to 2.7 million during a pandemic (at a 50% attack rate). Refined estimates of demand will depend upon early and continued surveillance data
- New healthcare contacts for influenza-like illness can be expected to exceed 10,000 per 100,000 population per week at the peak period (at a 50% attack rate). Peak consultations during seasonal influenza periods in recent years have been 400-900 per 100,000 per week
- Peak demand could be sustained for one to two weeks with local epidemic waves for 6-8 weeks
- Children within the normal weight range for their age who have high fever and cough or influenza-like symptoms should if:
i) aged under one year or at high risk of complications (due to severe co-morbid disease) - be seen and assessed by a GP or hospital emergency department
ii) aged 1 and 2 years (i.e. up to 3 years) - be seen and assessed by a GP or suitably experienced health care professional
iii) aged 3 years and over - be assessed by the telephone helpline staff using a clinically based paediatric triage protocol and referred for antivirals or to a medical practitioner if indicated - Assuming a complication rate of 25%, an attack rate of 50% and those under 3 needing to see a health professional, general practices can expect to see 3025 influenza patients per 100,000 population per week at the peak
- 2000 per 100,000 population may require hospital admission - an increase of at least 50% on normal demand
- Demand for hospital admission can be expected to increase up to 440 new cases per 100,000 per week at the peak and is unlikely to be met from available acute hospital capacity
- Demand for critical care beds could rise to 110 per 100,000 per week at the peak and would exceed available capacity
- An increase in the numbers suffering from influenza and its direct complications may be accompanied by other demand caused by anxiety and bereavement and service provision challenges exacerbated by depletion of the workforce and logistical difficulties
- The following tables estimate anticipated cases, healthcare contacts, GP consultations, Emergency Department visits, hospital admissions and deaths based on a uniform attack rate across all age groups.
Table 4 - Expected healthcare demand over the course of a pandemic, for 25%, 35% and 50% clinical attack rates and the upper end of the range for all other planning assumptions
Per 100,000 population |
|||
|---|---|---|---|
25% attack rate |
35% attack rate |
50% attack rate |
|
Clinical cases |
25,000 |
35,000 |
50,000 |
GP consultations |
6,875 |
9,625 |
13,750 |
Hospital admissions |
1,000 |
1,400 |
2,000 |
Deaths |
625 |
875 |
1,250 |
Table 5 - Expected healthcare demand during the peak of a pandemic, for 25%, 35% and 50% clinical attack rates and the upper end of the range for all other planning assumptions
Per 100,000 population |
|||
|---|---|---|---|
25% attack rate |
35% attack rate |
50% attack rate |
|
Clinical cases |
5,500 |
7,700 |
11,000 |
GP consultations |
1,800 |
2,500 |
3,600 |
Hospital admissions |
220 |
308 |
440 |
Deaths |
140 |
200 |
280 |
Assumptions:
- 22% of the total demand occurs in the peak week.
- All complications (@ 25% cases) and symptomatic children under the age of 3 (3.2% of the population) are consulted by a GP.
- Hospital admissions @ 4.0% of cases.
- Deaths @ 2.5% of cases.
9.4 General principles of containment and infection control
Specific infection control guidance is available for hospitals, primary care and some other settings but, generally, limiting the transmission of pandemic influenza requires the application of tried, tested and proportionate basic infection control measures such as:
- staff and public education
- local risk assessments to inform decisions on control and protective measures as required by the Control of Substances Hazardous to Health Regulations 2002
- documenting proportionate procedures, operational protocols and checklists
- the consistent application of good hygiene and infection control measures
- timely recognition of symptomatic patients
- segregating (isolating) symptomatic patients in their homes and limiting external contact
- using voluntary quarantining measures if necessary
- clustering symptomatic patients who are in hospital, residential homes or other closed establishments in specific wards or designated areas
- ensuring that staff are well informed about and adhere to procedures for the prevention of influenza transmission
- providing personal protective equipment if occupational risk assessments have indicated that to be necessary and ensuring that staff are trained in its correct wear, limitations and use
- implementing enhanced cleaning routines to minimise the risk from contact with hard surfaces.
Further guidance on infection control measures is available at: www.infectioncontrol.hps.scot.nhs.uk
9.4.1 Face masks/respirators in care settings
Various types of surgical face masks and respirators are available, offering differing levels of protection and meeting agreed European and/or international normative standards. WHO recommends the use of surgical masks and particulate respirators at 95% efficiency by healthcare workers during a pandemic and that symptomatic patients could themselves wear surgical masks to protect others if circumstances make it absolutely necessary for them to leave home and logistical arrangements allow. Standard Health and Safety Executive guidance calls for higher specification FFP3 respirators for healthcare workers whenever respiratory protection is indicated in the UK, although it recognises that this may not be sustainable in the special circumstances of an influenza pandemic. Based on available evidence, current UK pandemic influenza infection control guidance is:
- fluid-repellent surgical masks should be worn by healthcare workers who may be in close and/or frequent contact (within one metre) with symptomatic patients
- FFP3 standard disposable respirators should be worn when carrying out clinical procedures likely to generate aerosols of respiratory secretions from infected patients (e.g. dental drilling, intubations, aspiration), although such procedures should be avoided as far as possible. It should particularly be noted that fit testing and specific training are essential for these respirators.
9.4.2 Other personal protective equipment
If close contact with an influenza-infected patient is considered inevitable or highly likely, health workers should adopt sensible barrier precautions in addition to face masks. Disposable protective equipment, such as aprons and gloves, provide a physical barrier and help avoid spreading contamination. Although the ocular route is not regarded as a major route of transmission for normal human influenza viruses, it is nevertheless biologically plausible and eye protection (preferably disposable) may be necessary when carrying out aerosol-generating procedures or if risk assessment indicates that this is necessary.
9.4.3 Clinical Guidance
The British Thoracic Society, British Infection Society and Health Protection Agency have produced joint provisional guidelines for the clinical management of patients with an influenza-like illness during a pandemic. They describe the clinical features, assessment and treatment of adults and children in hospital and community settings. The guidelines are regularly reviewed and updated and may need to be varied to reflect capacity, shortages or constraints as the pandemic develops.
Guidance on the clinical management of patients with influenza-like symptoms during a pandemic is available from:
British Thoracic Societywww.brit-thoracic.org.uk/PandemicFlu.html
Scottish Government Health Directorateswww.scotland.gov.uk/pandemicflu
Health Protection Scotlandwww.hps.scot.nhs.uk/resp/index.aspx
9.5 Prioritisation of Services
National planning assumptions for healthcare demand and staff absence rates during a pandemic indicate that high demand for services and high levels of staff absence will converge over an extended period of time. In these circumstances it is unrealistic to expect the NHS to maintain current levels of service in some areas over the course of an outbreak.
The capacity to deliver continuity of essential and emergency influenza and non-influenza services throughout an outbreak must be protected and preserved. To achieve this, the scaling-back, limiting or temporary cessation of other services in both primary and acute settings must be considered inevitable. The extent to which other services will be affected will only be determined when the actual characteristics of the emergent virus are known.
A strategy for service prioritisation is being developed on a UK basis. It is intended that this work will lead to the development of a common understanding across services of what the priorities are and to assist a nationally consistent approach to the application and removal of service restrictions. Further guidance in this area will be published in due course.
9.6 NHS Performance Targets
Consistent with and subject to the work described above, it is necessary to take a view on the status of NHS performance targets (and especially access targets relating to maximum waiting times for elective treatment) during a pandemic. The existing range of key objectives for the NHS covers Health Improvement, Efficiency, Access and Treatment ( HEAT). Within these key ministerial objectives, key targets exist across a number of areas in the acute sector e.g.:
- Waiting times for elective outpatient appointments, diagnosis and treatment
- Cancer and coronary care treatment
- Hip fracture surgery
- A&E waiting times
We propose to take the following approach:
- All elective targets and the A&E target should be suspended during a pandemic influenza outbreak. The Scottish Government Health Directorates would continue to monitor NHS Boards' performance to help identify "hot spots" in the care system and to ensure that the local, regional and national response to the pandemic was delivering appropriate care to patients.
- The following Scottish Government HEAT targets will remain in place through an influenza pandemic:
- Access to cancer diagnosis and treatment following urgent referral
- Access to specialist hip surgery following fracture
- Access to cardiac intervention.
- However, Boards' performance against these targets would be interpreted in a pragmatic way in accordance with the circumstances and the priority attached to patients by the clinicians responsible for their care.
- A sensitive approach to the reinstatement of targets should be taken over an agreed period of time, and according to the circumstances immediately following the pandemic
- These proposals are subject to the work being carried out on prioritising services and may be revised.
9.6.1 Trigger for suspension of targets
We propose that target suspensions would begin at Phase 6 Alert level 2 - the point at which the pandemic reaches the UK - as rapid spread to all areas of the UK could be expected at that point. NHS Board Chief Executives would be notified by the Health Directorates that specified targets were being temporarily suspended when this point was reached.
9.6.2 Further Work
Further guidance will be issued in due course on a wider range of targets. This may cover primary care, community care, NHS24 and the Scottish Ambulance Service.
9.7 Workforce arrangements and personnel policies
Considerable pressure will be experienced by NHS and local authority staff during a pandemic. Part of this pressure will be caused by the likelihood that staff will be pushed hard by the demands of a pandemic and, at the same time, the availability of those staff will decline due to the spread of the virus and staff becoming ill. Planning needs to take place both locally and nationally to deal with the consequences of this pressure.
A strategy is being developed centrally by a Workforce group and a full report will be available from that group in due course. The work undertaken centrally will aim to ensure that local policies can be fully and legally implemented and that any national legislative and policy barriers to local actions have been removed.
National action will encompass the following:
- relevant legislative and contractual barriers to redeployment and the use of students and retired staff
- professional constraints
- working hours and pay and rewards
- updating staff absence policies
- altering arrangements for certification of sick leave (at UK level)
- disclosure requirements
- training for redeployment.
This will facilitate local strategies which should focus on the following:
- redeployment of staff and making use of skills in a flexible way to cover for absences
- redeployment of staff from areas where work has been cancelled to priority areas
- management of the flow of staff between the NHS and community care settings
- considering the use locally of medical students and available retired staff and retaining and regularly updating registers of those available
- considering the use of allied professions and non medical staff to perform medical duties
- removing local contractual barriers
- communicating the messages to staff in advance about redeployment
- provision of local training.
9.8 Access to Care
Normal patient pathways and service delivery arrangements will need to be adapted in a pandemic as additional demand saturates or threatens to overwhelm available capacity, staffing or other resources. These alternative arrangements and strategies need to be developed in advance and implemented as demand increases. Plans should be able to accommodate alternative service delivery arrangements such as:
- the introduction of a telephone-based initial assessment and triage of all symptomatic influenza patients by trained lay-operators following clinically approved algorithms to authorise antiviral collection and refer influenza patients to further services as appropriate
- the provision of a wider range of treatments by health professionals (e.g. nurses, paramedics, pharmacists, dentists) following agreed guidelines and using 'prescription only' medicines under agreed authorisations
- care in the community by GPs and community-based health teams of patients who under normal circumstances would be admitted to hospital
- treatment of patients in areas of a hospital not normally used for providing acute medical care by medical and nursing teams who do not normally manage such patients
- treatment of patients in private health facilities not normally used for acute medical care by medical and nursing teams who do not normally manage such patients.
- and any other specific local contingencies that have been identified as necessary
9.8.1 Delivering care in a community setting
Additional demand for healthcare will mean that most influenza patients will require an initial assessment, and the majority of their subsequent care and support, outside of hospital healthcare settings. Patients will need to access care (including self care) from their own home or residential settings as far as possible to help reduce and limit the spread of infection.
Developing effective arrangements that ensure a sustainable community-based response should therefore be a pivotal component in all local plans. Arrangements should provide for:
- patient assessment
- access to antiviral and other medicines
- treatment of complications
- if necessary and available - access to hospital care, home care and care homes.
GPs and community health teams will continue to provide the initial health response. While normal primary and community care delivery mechanisms may remain adequate and maintainable in the very early and latter phases of a pandemic, services will need to adapt quickly in response to escalating demand. Ceasing non-clinical activities and similar measures may make some additional capacity available. However, pressure on individual practices will be heavy, additional demand for care in the home will be high and single-handed or smaller practices are likely to experience disproportionate difficulties caused by the absence of key staff.
In addition to maintaining essential provision for non-influenza patients, the resources and skills available in general medical practices should focus primarily on patients who:
- are suffering influenza complications
- are less than three years of age
- have relevant pre-existing medical conditions
- are in identified 'at-risk' groups
- are not responding to treatment
- need higher levels of care but cannot be admitted to hospital
- are pregnant
- are dying
- have died - including bereavement support.
9.8.2 Local influenza health coordination
Each territorial NHS Board will need to establish and resource an effective mechanism for directing and coordinating the local response.
Unless other local arrangements are in place, Community Health Partnerships, under the direction of their NHS Board, should carry out the local coordination of community services. In terms of functionality they should:
- act as a focal point, providing a link to and oversight of the local health response
- monitor and coordinate the overall health response on a pan organisational, whole systems basis
- maintain the continuing provision of general practice and primary care services both in and out of hours
- collect, collate and report information on the local health situation
- link with community care and other agencies to support the delivery of care and maintain patients at home
- provide a local link and health input and advice to the wider local coordination arrangements
- ensure that national messages are cascaded, reinforced and that the public are well informed and advised of local response arrangements.
9.8.3 Primary Care
NHS Boards' response plans should be developed in consultation with local professional representative committees and should include the following components:
- reinforcing individual practice and inter-practice service continuity arrangements
- developing mutual aid
- enhancing out-of-hours arrangements
- providing for those who are unregistered or away from home
- identifying inter-profession support opportunities.
9.8.4 Supplementing Primary Care
Normal primary care arrangements are likely to require significant supplementation as the pandemic wave(s) develop, and an effective support system during the peak week(s) of a pandemic should incorporate:
- 24x7 telephone-based access via a national influenza line for the majority of those patients who believe they are symptomatic, with an appropriate and timely response across Scotland
- the use of non-clinical staff to provide initial telephone assessment for most patients and either to authorise the collection of antivirals or refer patients to their GP as appropriate
- secure systems allowing for the collection of an antiviral treatment course and self-care leaflet by the patient's friend or relative from a designated collection point or, exceptionally, home delivery
- advice to parents/guardians of symptomatic children weighing 15 kg or less (under 3 years of age) to contact their general practice for assessment and antiviral solution
- prompt reference to a GP if history/signs/symptoms indicate influenza complications or failure to respond to treatment
- agreed and consistently applied clinical criteria and thresholds for hospital admission
- continuing provision for emergency treatment and for maintaining other essential primary care
- social support to help maintain patients in their home or residential setting
- protocols for the management of patients presenting in other settings. There should be recognition that some symptomatic patients will present at accident and emergency departments, general practice, pharmacies or other health facilities irrespective of advice or plans
- arrangements for targeted vaccination when/if a suitable pre-pandemic or specific vaccine becomes available.
9.8.5 Telephone-based access arrangements (national influenza line service)
Face-to-face clinical assessment for every patient will not be feasible at the peak of a pandemic, even assuming that most would be well enough to attend surgeries or other healthcare facilities. Department of Health analysis suggests that general medical practices will not be able to expand their collective telephone call-taking capacity sufficiently to meet the level of demand anticipated. Whilst patients may still choose to make contact via their GP surgery, call centres using trained call takers operating to a clinically-based algorithm offer a viable and acceptable alternative.
To provide public information and advice before and during a pandemic, the Government - in conjunction with the Central Office of Information, NHS Direct and NHS24 - will establish a national influenza line service at WHO international phase 5 (see figure 3).
From UK alert level 2 ( WHO phase 6) the service will expand to provide initial patient assessment and antiviral authorisation and both functions will then remain operational until the impact of the pandemic and the threat of further waves subside.
The key objectives of the national influenza line service are to:
- provide pandemic influenza related advice and information
- provide access to pandemic related literature
- provide situation reports and daily updates
- provide access to a mechanism for rapidly assessing those suffering influenza-like symptoms
- authorise access to antiviral treatment (if that is indicated)
- give information on the nearest antiviral medicine distribution point
- refer to some other part of the health and community care system if that is a more appropriate disposition
- facilitate the capture of critical surveillance information (number of people calling who are symptomatic, demographics of those accessing treatment, take-up of treatment etc.) to inform the local and national pandemic response.
Initial assessment will focus on confirming that the caller has signs and symptoms of influenza, no indicators of complications, is aged three or over, has been symptomatic for less than 48 hours and antiviral treatment is not otherwise contraindicated. Suitably trained staff using a clinically based decision tree algorithm will perform these tasks and authorise the collection of antiviral medicines for the patient. Analysis suggests that, at a 50% clinical attack rate, such a service might need the capacity to handle a minimum of 11,000 influenza-related telephone calls per 100,000 population and 28 staff per 100,000 population per day to provide 24-hour cover during the peak week.
The Department of Health is developing a suitable national algorithm and producing model protocols/guidelines to allow the supply of oseltamivir following a telephone assessment. It also proposes to make the necessary amendments to medicines legislation to enable alternative prescription and supply arrangements in a pandemic and will be consulting on the proposals.
Further guidance on the provision of care in a community setting is available at: www.scotland.gov.uk/pandemicflu
Figure 3 - A proposed model of care from a patient's perspective
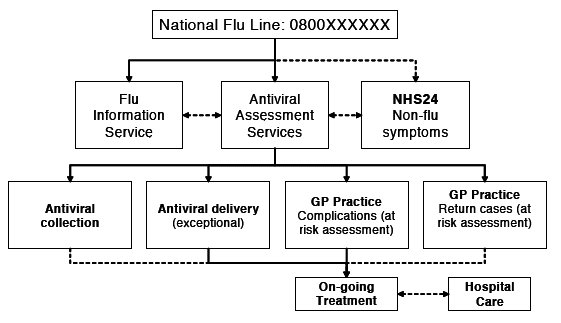
9.8.6 Providing rapid access to antiviral medicines
In order to limit the spread of infection and maximise individual health benefits, patients should take an antiviral medicine as soon as possible after the onset of symptoms - ideally within 12 but in any case within 48 hours. Therefore, rapid antiviral provision is an important planning aim. At the initial stages of a pandemic, any patient who has been symptomatic for less than two days should be offered treatment with antiviral medicines unless contraindicated, although this policy will be reviewed as information on the actual attack rate, clinical impact, optimum dosage regime, stock consumption, any resistance and timeframe within which treatment remains useful emerges.
A proportion of the national stockpile has already been pre-distributed to the NHS Boards (5% to mainland Boards and 10% to the island Boards). Subsequent supplies will be adjusted to reflect the actual attack rate, transient populations and supply position. Response plans should provide for local distribution to hospitals, health establishments, closed institutions and general practitioners, and should ensure that supplies are conveniently accessible to those local communities from pre-designated distribution points or collection centres (which are likely to include some community pharmacies) across the area. Storage and distribution arrangements should address the need to protect stock and staff security in consultation with the police and local pharmacy adviser. Self-management advice leaflets, information and contacts for support should also be available at these collection/distribution centres.
Plans should assume that a friend or relative will be available to collect the patient's antiviral treatment course from the designated distribution/collection point on production of authorisation from the influenza line or nominated health practitioner. Pre-pandemic messages will ask everyone to try to arrange such helpers, but for the small proportion unable to do so, alternative arrangements such as a home delivery service by courier/taxi should be developed.
9.8.7 Antibiotics and essential pharmaceutical supplies
Demand for essential medicines and over-the-counter remedies is likely to be high in a pandemic and re-supply may be uncertain. The Department of Health and the Scottish Government are reviewing available stock levels and working with the pharmaceutical sector and others to enhance stocks, improve supply chain resilience and consider other options for meeting demand and maintaining supply. Further clinical guidance on the prescribing and use of medicines during the pandemic alert and pandemic periods will be issued and there will be consultation on proposed changes to medicines legislation and related regulations, designed to ensure adequate patient access, with a view to implementing those changes in the event of a pandemic.
9.8.8 Acute Care
Adults and children with uncomplicated influenza infection do not usually require hospital treatment, but those with worsening pre-existing medical conditions or suffering influenza-related complications may need referral.
The interface between acute and primary care is crucial and joint review of agreed appropriate protocols are needed in the planning and clinical phases. Symptomatic patients will be advised to stay at home, seek help by telephone and not to attend surgeries or health facilities unless by prior arrangement. Contingency arrangements should recognise, however, that self-referral is inevitable. The level of self-referral is likely to be significantly higher for certain patient groups e.g. infants, children and patients with chronic conditions. Breakdowns, loss of confidence or access difficulties in community provision will exacerbate this.
Existing hospital capacity may only meet 20% to 25% of the expected demand at the peak. Normally there are some 28,296 beds (including day beds) in use in Scotland, of which 17,523 are acute beds and 467 are for patients requiring HDU or ITU care. It may be possible to release almost 33% of the total acute bed capacity within 5-10 days of ceasing elective work.
Even with additional capacity, and the implementation of measures to improve utilisation and supplement availability, the level of additional demand, combined with increased staff absences and possible increases in length of stay, will make hospital overcrowding inevitable and capacity a major limiting factor. Other limiting factors such as shortages of medical supplies, limited availability of diagnostic support services, and potential disruption to the supply of blood/blood products are also likely to have an impact.
Proportionate admission thresholds based on clinical management guidelines will need to be agreed and progressively applied. Consistency and equity in their application is important in gaining public understanding and maintaining confidence. Common understanding and interpretation of those guidelines by health professionals at the primary, secondary and community care interfaces are particularly important.
Plans should focus on ways of supplementing and making the most effective use of the staffing and beds, with particular attention paid to factors that facilitate rapid discharge or step-down arrangements. Plans should also address establishing alternative care sites; utilising private hospital/clinic facilities; staffing; and other options for increasing capacity. Up to 25% of symptomatic patients who would warrant hospital admission (if sufficient capacity were available) may require high dependency or intensive care ( HDU/ ICU). Most will have influenza-related pneumonia or a severe exacerbation of underlying co-morbid illness. The indications for such transfer are no different when compared to non-influenza patients.
Acute sector plans should detail:
- staff protection (physical and mental health and personal safety aspects), infection control and security aspects for supplies and entry/exit controls
- the core services and areas of operation which will continue during the pandemic
- arrangements for progressively winding down elective and non-essential activity before and during the pandemic phase
- for the clinical management and, if required, isolation and cohorting for:
i) non-pandemic influenza emergencies
ii) suspected or proven pandemic influenza patients
iii) patients at special risk e.g. immunocompromised patients and those with chronic diseases - the specific arrangement for adults and children in the clinical areas of:
i) Emergency Medicine departments
ii) Acute Medical and Admission Units
iii) HDU/ ITU Units
iv) Care of the Elderly - arrangements for discharge from hospital or to 'step-down' units
- the identification and training of redeployed staff
- arrangements to inform staff of clinical guidelines for patient management and to monitor and review the effectiveness of these arrangements.
9.8.9 Community Care
Effective arrangements developed jointly by health and community care agencies are critical to the relief of suffering and to achieving the wider public health aims of keeping symptomatic patients at home, caring for them in a community setting and reducing the demand on healthcare facilities. More than 110,000 people rely to varying extents on community care support provided by or through Local Authorities. Those services cover a wide range of needs such as care in residential/nursing homes, day centre provision, meals on wheels, home helps and personal assistant schemes. The 2001 census also indicated that in Scotland, over 60,000 people care for a relative or friend for between 20-49 hours per week and almost 116,000 people for over 50 hours a week. Many of these 'informal' carers will be affected over the pandemic period and alternative care arrangements may be required.
Community care providers are in regular contact with individuals in the community who might be more vulnerable to, or more affected by, pandemic influenza. In addition to maintaining services for those who will continue to rely upon them, community care providers must also anticipate additional short-term and short notice demand from those unable to cope independently or whose normal care arrangements have been disrupted. Voluntary, private or independent sector organisations provide many of the services on contract and all forms of community care provision need integration into local contingency plans.
Key challenges include:
- sustaining services that provide essential lifelines, e.g. meals on wheels, provision of community equipment, community alarm services
- meeting the additional pressures on already overstretched local community care services and intermediate care services due to the additional pressures on acute hospital beds
- ensuring that the lines of communication exist to relay essential national, regional and local messages to the diverse range of community care services (statutory, voluntary, independent and private)
- additional pressures on caring time to support care home residents and people cared for at home
- sustaining people with complex disabilities who are currently supported with intensive care packages in the community
- providing emergency respite care for vulnerable people looked after at home by informal carers while their carer is ill
- maintaining a balance between appropriate safety and infection control measures and ensuring that the quality of life of vulnerable adults is maintained as far as possible
- dealing with workforce and resource implications. This would include dealing with staff absences and redeployment to ensure adequate level of care services.
To help community care providers meet these challenges, further guidance is available. Planning for pandemic influenza in community care: An operational and strategic framework can be found at the following website ( http://www.scotland.gov.uk/pandemicflu). It deals with the impact of a pandemic influenza outbreak on community care, and how community care services should respond. There are key challenges in managing community care services, and the document sets out key planning considerations, and organisational and individual roles. It is intended for all involved in planning community care services, including managers of care at home services and managers of care homes.
9.8.10 Role of NHS24
Demand for health advice and information is likely to increase significantly during a pandemic. NHS24 will continue to play an important role in providing health advice and information through their normal telephone number, and via the NHS24 website ( www.nhs24.com). Demand on NHS24 core services is likely to increase and the primary focus of service continuity plans is the maintenance of core services in the face of high levels of staff absence.
In the event of the pandemic threat increasing, the Government will also activate a national influenza line service from WHO international alert phase 5. Initially the service will provide advice, updated information and access to literature. At UK alert level 2 ( WHO phase 6) the service will expand to provide rapid assessment and where necessary access to antiviral treatment for symptomatic patients
The Scottish Government and NHS24 will work with territorial NHS Boards to develop national influenza helpline services and local delivery arrangements.
9.8.11 Pharmacy
The contribution that pharmacies can make in a pandemic scenario will depend on the setting in which they routinely provide services and the qualifications, expertise and area of practice of their pharmacists. Community pharmacies are often located in the heart of communities. They can make an important contribution in support of self-care, dispensing/repeat dispensing of routine medicines, signposting other NHS services, supplying regular medicines to vulnerable people such as residents of care homes or those with long-term conditions and maintaining medicine supplies under contracts with other bodies such as hospices and prisons as far as possible.
To ease pressure on GP surgeries and community services, new powers may be given to community pharmacists (subject to consultation and parliamentary approval) to supply medicines and provide pharmaceutical services in a more flexible manner. Formal consultation will precede any proposed changes to legislation.
Hospital pharmacists and their staff will play an important part in making the best use of available medicines including the appropriate use of patients' own medicines and facilitating the discharge of patients with adequate supplies of medicines. Where there are shortages of some medicines, pharmacists are well placed to advise on the use of alternative medicines that have a similar effect. Pharmacies will play an important part in educating the community, providing positive health messages and advising patients and members of the public on medicine supply issues.
As the pandemic escalates some of the routine functions and services provided by pharmacies may have be reduced, or stopped for short or longer periods, as demands increase elsewhere. Specialist clinical pharmacists may be able to support doctors and other healthcare professionals in all settings, including primary care, hospitals and the community. Pharmacists working in primary care could also be deployed to support GPs in their practices or in community pharmacies.
9.8.12 Role of Scottish Ambulance Service
Demand on the Scottish Ambulance Service is likely to increase significantly in a pandemic. The primary focus of service continuity plans is the maintenance of capacity to answer all emergency and urgent calls, although some prioritisation and changes in normal performance standards may become unavoidable. Plans should recognise the need to facilitate rapid discharge or transfer arrangements and explore opportunities to utilise any organisational and communication capacity available from the curtailment of non-essential activities to support the delivery of home care to influenza sufferers.
Pandemic specific pre-hospital patient assessment and treatment protocols should recognise that hospital capacity will be extremely limited; emphasising treatment at home and ensuring that only patients with life-threatening conditions are actually conveyed to emergency departments. Local response plans should also consider the extent to which the field assessment and treatment skills of ambulance staff could be utilised to support the wider delivery of home care.
9.8.13 Dentistry
Current infection control advice suggests that health professionals should avoid aerosol generating procedures on symptomatic patients as far as possible during a pandemic and must wear respirators and suitable protective equipment where that is not possible. Many dental procedures have the potential to generate aerosols and risk assessments will therefore be necessary. Local plans should ensure that emergency care remains available throughout a pandemic, but dental practitioners may find normal demand reduced because of limits on the procedures they are able to carry out on those with respiratory symptoms and patients themselves deferring treatment or facing travel difficulties. Opportunities to use the assessment and treatment skills of dental practitioners or other health professionals to support the wider delivery of health care in a pandemic should be explored in local planning.
Specific infection control guidance for dentists can be found in the document " Pandemic Flu: Infection Control Guidelines for use in Hospitals and Primary Care Settings" at: www.scotland.gov.uk/pandemicflu
9.9 Coping with stress and bereavement
In the lead up to a pandemic, many people are likely to feel anxious, apprehensive, and to have an understandably subjective perception of the degree of risk. As the pandemic develops, many people may feel fear for their own health and that of their family and friends, grief for loss of relatives or friends, a sense of social isolation or other potential causes of psychological distress. Whilst many are likely to be resilient enough to cope with little or no professional or specialist intervention, some people may need or may welcome additional support.
Local plans should consider how to provide that additional support. For example, NHS Boards and community care services should consider how they can offer support both to their own staff and to patients and their families. This could include a range of measures such as:
- the important role of religious and community leaders
- self help material
- the role of specialist support services e.g. for mental health
- the role of voluntary organisations
- specialist counselling.
Support should be made available both during and for some time following a pandemic.