Organisational duty of candour: guidance
This guidance focuses on the implementation of the legal duty of candour procedure for health, care or social work services.
Introduction
General
Openness and honesty should be central to the actions of those providing care to others. It should be at the heart of every relationship between those providing, receiving and/or experiencing treatment and care. Trust and effective communication can be difficult to maintain and easy to lose when things have gone wrong.
The new organisational duty of candour underpins the Scottish Government's commitment to openness and learning which is vital to the provision of safe, effective and person-centred health and social care. This guidance focuses on the implementation of the legal duty of candour procedure for all organisations that provide health services, care services or social work services in Scotland.
The organisational duty of candour provisions of the Health (Tobacco, Nicotine etc. and Care) (Scotland) Act 2016 (The Act) and The Duty of Candour Procedure (Scotland) Regulations 2018 set out the procedure that organisations providing health services, care services and social work services in Scotland are required by law to follow when there has been an unintended or unexpected incident that results in death or harm (or additional treatment is required to prevent injury that would result in death or harm).
Alongside the legal requirements in following the duty of candour procedure, this guidance outlines the issues organisations will want to consider at each point in the procedure; suggests best practice; and provides a checklist of the steps to be taken to fulfil the duty. Links to other helpful resources are included throughout and in Annex G.
This guidance is not intended to be a definitive interpretation of the legislation on duty of candour. However, following an unintended or unexpected incident, organisations are encouraged to follow the guidance in implementing the processes outlined. This will help ensure consistency of approach and equity of response across organisations in Scotland.
In this guidance the word must refers to actions that are a legal requirement as set out in the duty of candour procedure legislation. The remainder of the guidance provides details of best practice in following arrangements for notification, discussion, review and actions for organisations when there has been an unintended or unexpected incident resulting in death or harm. The guidance also includes several 'issues to consider' sections that outline areas to think about in support of implementation of the organisational duty.
Organisations may also wish to develop local guidance and procedures to support notification, meetings, review, training and support requirements in a manner that is tailored to the particular services they provide.
Every organisation covered by the duty of candour legislation is regarded as a 'responsible person' with the definition as set out in section 25 of The Act.
A 'relevant person' is the person who has been harmed during the incident, or where that person has died, or is, in the opinion of the responsible person, lacking in capacity or otherwise unable to make decisions about the service provided, a person acting on behalf of that person. This is set out in section 22(3) of the Act.
The need for candour
Enabling and managing risk is a central part of delivering high quality health, care and social work services. Candour promotes responsibility for developing safer systems; better engages staff in improving services; and creates greater trust in people who use these services, either first hand or on behalf of someone else.
Personalised discussions and communication, review processes that take account of what matters most to those affected and supportive responses following unintended or unexpected incidents all help to support and promote a culture of learning. Putting people at the centre of organisational responses to unintended or unexpected incidents resulting in death or harm also helps create the conditions where people feel psychologically safe to contribute to such discussions.
Truly personalised organisational responses when things go wrong require a commitment to the provision of support and training for everyone involved in meetings, reviews and actions arising from the organisational duty of candour.
The focus of the duty of candour legislation is to ensure that organisations tell those affected that an unintended or unexpected incident has occurred; apologise; involve them in meetings about the incident; review what happened with a view to identifying areas for improvement; and learn (taking account of the views of relevant persons). Organisations must ensure that support is in place for their employees and for others who may also be affected by unintended or unexpected incidents.
Organisations must set out in an annual report the way that the duty of candour procedure has been followed for all the cases that they have identified.
There are already a number of professional duties of candour such as those required by the Scottish Social Services Council, the Nursing and Midwifery Council, the General Medical Council, the General Dental Council, and the General Optical Council. This statutory organisational duty has been developed to be in close alignment with the requirements of these professional duties and will be mutually supportive.
Leadership and management
Leaders and managers within organisations should ensure that the implementation of the duty of candour procedure forms a key part of the learning systems within their organisations and that the necessary integration and alignment with organisational processes and procedures has taken place. The central emphasis on communication, support, learning focused reviews and transparency in publishing duty of candour annual reports should be reflected throughout the organisation. Each organisation must ensure that all staff who carry out the procedure on its behalf are familar with the duty of candour procedure.
Organisations should consider how monitoring of the effective implementation of the actions required by the duty of candour legislation can be integrated into existing corporate governance frameworks, processes and procedures. Assurance should be sought to confirm that all elements of the procedure are being implemented when they should be, and that there are ways of supporting continuous improvements and refinements in the way that the organisation discharges its legal responsibilities.
Who does the duty of candour procedure apply to?
Organisations that provide a health service, care service, or social work service to which the duty of candour applies is referred to in the relevant legislation as a "responsible person". This is set out at section 25 of the Act:
- a Health Board constituted under section 2(1) of the National Health Service (Scotland) Act 1978 (the 1978 Act);
- a person (other than an individual) who has entered into a contract, agreement or arrangement with a Health Board to provide a health service;
- the Common Services Agency for the Scottish Health Service constituted under section 10(1) of the 1978 Act;
- a person (other than an individual) providing an independent healthcare service mentioned in section 10F(1) of the 1978 Act;
- a local authority;
- a person (other than an individual) who provides a care service;
- an individual who provides a care service and who employs, or has otherwise made arrangements with, other persons to assist with the provision of that service (except childminders or unless the assistance in providing that service is merely incidental to the carrying out of other activities);
- a person (other than an individual) who provides a social work service.
When must the duty of candour procedure be activated?
Organisations (as responsible persons) must activate the duty of candour procedure as soon as reasonably practicable after becoming aware that:
- an unintended or unexpected incident occurred in the provision of the health, care or social work service provided by the organisation as the responsible person;
- in the reasonable opinion of a registered health professional (as defined in Annex C) not involved in the incident:
(a) that incident appears to have resulted in or could result in any of the outcomes mentioned below; and
(b) that outcome relates directly to the incident rather than to the natural course of the person's illness or underlying condition.
It is important to note that where the duty of candour procedure start date is later than one month after the date on which the incident occurred, an explanation of the reason for this has to be provided to the relevant person.
The relevant outcomes are as follows:
A. The death of the person.
B. Permanent lessening of bodily, sensory, motor, physiologic or intellectual functions (including removal of the wrong limb or organ or brain damage) ("severe harm").
C. Harm which is not severe harm but which results in one or more of the following criterion:
- an increase in the person's treatment;
- changes to the structure of the person's body;
- the shortening of the life expectancy of the person;
- an impairment of the sensory, motor or intellectual functions of the person which has lasted, or is likely to last, for a continuous period of at least 28 days;
- the person experiencing pain or psychological harm which has been, or is likely to be, experienced by the person for a continuous period of at least 28 days.
D. The person requires treatment by a registered health professional in order to prevent:
- the death of the person;
- any injury to the person which, if left untreated, would lead to one or more of the outcomes mentioned in paragraph B or C.
The view of the registered health professional
A registered health professional must give their view on the incident and its relationship to the occurrence of death or harm and pre-existing illnesses or underlying conditions.
Organisations must ensure that the registered health professional who gives the opinion mentioned above, following an unintended or unexpected incident, is not someone who was involved in the incident.
This means that the final decision by the organisation about whether to activate the duty of candour procedure for a particular incident will be informed by the views of a health professional who has not been personally involved, but could work for the organisation.
The legislation does not require this to be a detailed and comprehensive analysis of the incident to form an opinion about contributory factors. The requirement is for someone not involved in the incident to provide a view to inform a decision about activating the duty of candour procedure (which includes a review process).
Although it will be for the organisations to determine the most appropriate way of obtaining the views of the registered health professional not involved in the incident, it is likely that health professionals will require organisations to provide them with the following core information in the first instance:
- What was the incident?
- What was the outcome?
- What illnesses and underlying condition did/does the person have?
When a registered health professional has agreed to provide the responsible person with their view, this should cover the following:
- Based on the background information provided, does it appear that this incident resulted in or could result in the death or harm 1 described?
- Does the natural course of the person's illness or underlying condition directly relate to the death or harm described?
In circumstances where there is not a registered health professional working within the organisation where the incident occurred (for instance a small care at home service or some social work services), registered health professionals with an existing involvement with the relevant person should be contacted where possible. However, they must not have been involved in the incident. Health services can provide assistance in identifying a registered health professional who would be able to provide the required view in such circumstances.
Organisations who have difficulties in identifying a registered health professional can also contact Healthcare Improvement Scotland or the Care Inspectorate for advice on routes to be considered.
Although it is likely that the organisation will already have a view on whether the procedure should be activated, the views of the registered health professional not involved with the incident form an important further step in the duty of candour procedure.
What is the procedure start date?
The procedure start date is the date that the organisation receives confirmation from a registered health professional that, in their reasonable opinion, an unintended or unexpected incident appears to have resulted in, or could result in an outcome listed above and that relates directly to the incident rather than to the natural course of the relevant person's illness or underlying condition.
What does 'could result' mean and how is that decision to be made?
If the registered health professional thinks that it is unlikely that harm will occur, then the duty of candour procedure need not be activated for that incident. The diagram below sets out the decision making process in more detail.
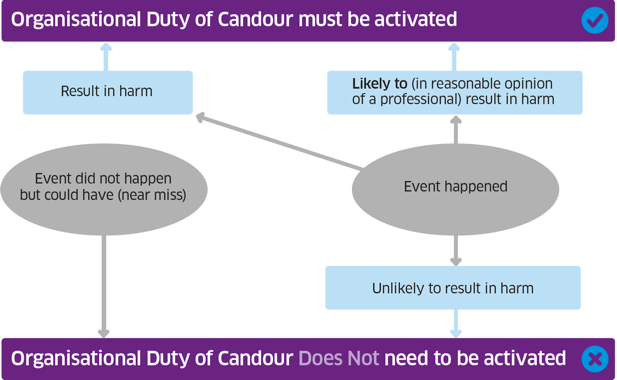
Notification
The duty of candour legislation states that the relevant person should be notified as soon as reasonably practicable but it should be considered good practice to notify the relevant person within 10 working days of the procedure start date.
This notification can be by various methods including telephone, face to face or by letter. It is important to remember that where a duty of candour procedure start date is more than a month after the incident, the organisation must provide the relevant person with an explanation of why this is.
Things to consider
Before having the conversation at the point of notification, the organisation may wish to consider:
- Who from the organisation is already in contact with the relevant person?
- What discussions or information exchange has already taken place?
- What is the relevant person's current understanding of the incident and organisational response to this?
- Where the conversation takes place?
- Who should be part of, and who should lead that conversation?
- What support should be available to the relevant person during the conversation and afterwards?
- Who will be the single point of contact following the discussion with the relevant person?
The notification must include:
- an account of the incident to the extent that the organisation is aware of the facts at the date the notification is provided; and
- an explanation of the actions that the organisation will take as part of the procedure;
- in the case where the procedure start date is later than one month after the date on which the incident occurred, an explanation of the reason for the delay in starting the procedure.
Things to consider
The information that an organisation may need to consider in deciding whether to activate the duty of candour procedure can come from a range of sources. It will be important for organisations to identify what these sources are and ensure relevant information, support and co-ordination mechanisms are in place. In some instances organisations may be contacted by other organisations providing health, care or social work services when it appears that the activation of the duty of candour procedure should be considered. Organisations should ensure that staff are aware of how to deal with such scenarios.
Organisations should consider the support needs of relevant persons at the earliest possible opportunity and while following the duty of candour procedure.
Communication with relevant person
Organisations must take reasonable steps to find out the relevant person's preferred method of communication. They must also take reasonable steps to ensure that communication with the relevant person is in a manner that they can understand.
Things to consider
Thinking about communication with the relevant person: Do you have any knowledge currently about their preferred method of communication?
It is recognised that in some instances communication channels may not exist or preferences are unknown. Establishing contact by telephone in the first instance might be necessary to find out what method of communication to use, and to begin dialogue on what steps might need to be taken in following the duty of candour procedure.
If an organisation is unable to contact the relevant person or the relevant person does not wish to speak with a representative of the organisation, the attempts made to contact them need to be included as part of the organisation's written record of following the duty of candour procedure.
Organisations need not provide information where relevant persons have indicated that they do not wish to receive it.
The Regulations do not permit or require organisations to disclose any information that would prejudice any criminal investigation or prosecution or contravene any restriction on disclosure arising by virtue of an enactment or rule of law.
Organisations need to be mindful of their general obligations to act in accordance with the European Convention of Human Rights, and any other relevant laws relating to personal information.
What are the implications if a claim for compensation is made once the decision to follow the duty of candour procedure is made?
Whilst it would not be appropriate for an organisation to try to prevent the relevant person from making a claim, organisations can suggest to relevant persons that they may wish to wait until the duty of candour procedure has concluded, when their case will have been investigated; they will have received an apology; the facts will have been established and any actions to improve the quality of care and/or learning will have been identified.
If a relevant person mentions that they are considering making a claim, the duty of candour procedure should continue. If a relevant person makes a claim ( the organisation receives formal notification of commencement of legal proceedings), then some elements of the duty of candour procedure may need to be paused until the legal process reaches a conclusion. For example, internal reviews could still proceed and organisations should still try to identify any potential improvement and learning actions.
Apology
In addition to any apology provided at the time of the incident, as part of the duty of candour procedure the organisation must offer the relevant person a written apology (this can be by electronic communication if that is the relevant person's preferred means of communication) in respect of the incident. The organisation must provide a written apology if the relevant person wishes it.
The written apology should be personal and be provided at an appropriate time during the duty of candour procedure, taking account of the facts and circumstances in relation to the particular incident.
This should take account of the circumstances relating to the relevant person and, wherever possible, the known personal meaning or impact of the unexpected or unintended incident.
There may still be misconceptions and misunderstanding that the provision of an apology equates to an admission of liability and that organisations should never offer apologies for this reason – but that is not correct.
Section 23(1) of the Act states that "an 'apology' means a statement of sorrow or regret in respect of the unintended or unexpected incident." The Act sets out that 'an apology' or other step taken in accordance with the duty of candour procedure does not of itself amount to an admission of negligence or a breach of a statutory duty."
Further guidance on making an apology as part of the duty of candour procedure and the form this might take is set out in Annex D. Further information can also be found on the Little Things Make a Big Difference website: http://www.knowledge.scot.nhs.uk/making-a-difference/resourcesaspx
Meeting
The organisation must invite the relevant person to attend a meeting and give them the opportunity to ask questions in advance. The organisation must take reasonable steps to ensure that the meeting is accessible to the relevant person, having regard to their needs.
For example, linguistic needs or reasonable adjustments that might need to be made for someone who has a disability. In some circumstances it will be necessary to have an interpreter, an advocate and/or someone the relevant person chooses to support them present.
Things to consider
A quiet room should be used, free from distraction and where the meeting will not be interrupted. It may not be appropriate to host the meeting close to where the incident happened as this could be emotionally difficult for the relevant person.
At the meeting, the organisation's representative should speak to the relevant person in the same way as they would want someone in the same situation to communicate with them or a member of their own family.
Staff should try to avoid the use of jargon or explain technical terms when speaking with relevant persons.
The meeting must include:
- a verbal account of the incident;
- an explanation of any further steps that will be taken by the organisation to investigate the circumstances which it considers led or contributed to the incident;
- an opportunity for the relevant person to ask questions about the incident;
- an opportunity for the relevant person to express their views about the incident; and
- the provision of information to the relevant person about any legal, regulatory or review procedures that are being followed in respect of the incident in addition to the procedure.
Following some unexpected or unintended incidents there may be several review processes operating in parallel. This can be confusing for people. To try to lessen this confusion, meetings with relevant persons must include details of other procedures which are being followed including their differing scope and focus.
In circumstances where an organisation is concerned, for example, that an unintended or unexpected incident was contributed to by factors influencing the capability of an employee it may be helpful for the relevant person to know that in addition to the systems review that is in operation, a separate process has been put in place to identify whether an employee may benefit from support and/or consider matters not related to organisational review and learning.
After the meeting the relevant person must be provided with:
- a note of the meeting;
- contact details of an individual member of staff acting on behalf of the organisation who the relevant person may contact in respect of the procedure.
Things to consider
Make sure the organisation agrees with the relevant person what the note of the meeting will include. This does not need to be a verbatim account of the discussion but could include when and where the meeting took place, a record of the apology and actions and timescales that were agreed.
Make sure that this note of the meeting is shared in good time with the relevant person. In some instances where the note of the meeting is brief, it may then be followed by a more comprehensive summary of the issues covered in the meeting – for example, outlining the questions that were asked or views expressed and the matters discussed. The note of the meeting may include reference to the process for producing this.
If the relevant person does not wish to, or is unable to attend the meeting, the organisation must still provide them with the information set out above (other than a note of the meeting) if the relevant person wishes it.
Where more than one organisation needs to be involved in the duty of candour procedure
The duty of candour procedure is the legal responsibility of the organisation who provided a health service, care service or social work service where the incident occurred. Other health and social care providers may have been involved in the provision of care and services, but they are not responsible persons (organisations) in respect of that incident.
It is often the case that a range of organisations are involved in the episode of treatment or care where the unexpected or unintended incident occurred. Although they are not responsible persons in terms of the legislation, they may need to become involved in providing information as part of a review or in providing support for relevant persons coping with the personal impact of death or harm arising from the unintended or unexpected incidents. In rare circumstances, several responsible persons may each decide to activate the duty of candour procedure for multiple incidents. In such circumstances, responsible persons should seek to communicate with each other, emphasising co-operation and ensuring a co-ordinated approach in their communications with the relevant person.
Where more than one organisation needs to be involved in the duty of candour review, all parties are expected to co-operate fully throughout the duty of candour procedure and share lessons learned and necessary actions identified by the procedure.
Where this is the case, the relevant person must be informed as part of the notification process, that the organisation where the incident occurred is the responsible person, as defined by the legislation, who will carry out the procedure.
The review
Organisations must carry out a review of the circumstances which they consider led or contributed to the unintended or unexpected incident. The legislation does not specify the manner in which the review is undertaken, but it is likely that this will be one of a range of review processes that are already undertaken such as an adverse event review, a significant case review of the sort undertaken by child, adult and public protection committees or a morbidity and mortality review.
Best practice requires that reviews involve clinical and care professionals with the relevant subject matter expertise, as appropriate.
Best practice in reviewing unintended or unexpected incidents that have resulted in death or harm require that a systems emphasis is adopted. This is clearly illustrated in resources such as the Systems Analysis of Clinical Incidents (known as The London Protocol) and the Social Care Institute of Excellence's Learning Together model.
It is the emphasis on contributory factors in this and similar protocols that represent best practice features of the reviews that must be conducted. Organisations may find the NHS Improvement Just Culture Guide a helpful resource for framing their approach to reviews.
Some of the resources that are available to support reviews focused on systems analysis; the identification of contributory factors and the investigation of human factors following harm events are outlined in Annex H.
In the case where the review is not completed within three months of the procedure start date, the organisation must provide the relevant person with an explanation of the reason for the delay in completing the review.
In carrying out the review, organisations must seek the views of the relevant person and take account of any views expressed. This will be best implemented through the development of a supportive relationship with the relevant person and arrangements that ensure review processes consider the views of the relevant person and are able to demonstrate the way in which these views (which are likely to reflect what matters most) have been taken account of.
Organisations must prepare a written report of the review, which must include:
- a description of the manner in which the review was carried out;
- a statement of any actions to be taken by the organisation for the purpose of improving the quality of service it provides and sharing learning with other persons or organisations in order to support continuous improvement in the quality of health, care or social work services; and
- a list of the actions taken for the purpose of the procedure in respect of the incident and the date each action took place.
This provides organisations with an opportunity to demonstrate that the views of relevant persons have been considered and that a review has been conducted that has focused on systems analysis that takes account of best practice in review and investigation of human factors.
The legal requirement to include details of the dates when each element of the duty of candour procedure took place is included to provide an overview of the process within an organisation from the point that they decide to activate the duty of candour procedure to the point the review is concluded.
Where possible, written reports on reviews should be written in a manner that minimises the need for extensive redaction.
Organisations must offer to send the relevant person:
- a copy of the written report of the review;
- details of any further information about actions taken for the purpose of improving the quality of service provided by the organisation or other health, care or social work services; and
- details of any services or support which may be able to provide assistance or support the relevant person, taking into account their needs.
Things to consider
It is important to think about how the report of the review is written if it is to be shared with the 'relevant person'. It should not contain jargon or acronyms which are difficult to understand. It should be clear and understandable.
Review reports should include information on the actions that are to be taken to make improvements in systems and processes influencing the quality of care delivery. The actions taken to share learning with other organisations (such as those who might have similar organisational processes to the ones that formed the basis of the review) should be outlined in the written review report.
The inclusion of the term 'further information' in the legislation recognises that supporting information to explain the conclusions of a review or provide details to explain why it is thought a particular action will improve quality can often be very helpful in demonstrating the approach to improvement implementation that will be adopted.
Records
Organisations must keep a written record for each incident to which the duty of candour procedure is applied, including a copy of every document or piece of correspondence relating to the application of the duty of candour procedure to the incident. The written record should be retained by the organisation in accordance with relevant local policies and procedures.
Reporting and monitoring
The Act sets out that a responsible person that provides a health, care, or social work service during a financial year must prepare an annual report, as soon as reasonably practicable after the end of that financial year.
The report must include:
- information about the number and nature of incidents to which the duty of candour procedure has applied in relation to a health service, a care service or a social work service provided by the responsible person;
- an assessment of the extent to which the responsible person carried out the duty of candour;
- information about the responsible person's policies and procedures in relation to the duty of candour, including information about procedures for identifying and reporting incidents, and support available to staff and to persons affected by incidents;
- information about any changes to the responsible person's policies and procedures as a result of incidents to which the duty of candour has applied;
- such other information as the responsible person thinks fit.
The report must not mention the name of any individual, or contain any information that could identify any individual.
The report must be published in a manner that is publicly accessible. For instance, on an organisation's website.
When an organisation has published a report, they must notify:
- Healthcare Improvement Scotland, in the case of a report published by an organisation which provides an independent healthcare service (within the meaning of section 10F(1) of the (Scotland) Act 1978). This can be submitted via the eForms system;
- The Scottish Ministers, in the case of a report published by any other organisation which provides a health service. Please send the notification to dutyofcandour@gov.scot ;
- The Care Inspectorate, in the case of a report published by an organisation which provides a care service or a social work service. The Care Inspectorate will ask for information about whether or not care services have published their duty of candour report in the first set of Annual Returns following the end of the financial year after which the report must be published.
Healthcare Improvement Scotland, Scottish Ministers and The Care Inspectorate may, for the purpose of monitoring compliance with the duty of candour provisions, serve a notice on an organisation, requiring them to provide information about any of the matters listed in the Reporting and Monitoring section as specified in the notice, and that information is to be provided within the time specified in the notice. As a result, they may publish a report on the organisation's compliance. Sample report templates have been produced as illustrative examples for responsible persons.
Training and support
Each organisation must ensure that all staff who carry out the procedure on its behalf are aware of the duty of candour procedure.
An E-Learning resource has been produced by Education for Scotland, The Scottish Social Services Council, The Care Inspectorate and Healthcare Improvement Scotland. Relevant staff should be encouraged to complete the module which takes no longer than an hour. It is available on the following web-sites:
- Turas;
- learning systems, such as learnPro;
- The Care Inspectorate;
- Scottish Social Services Council;
- Little Things make a Big Difference;
Factsheets are available on the Little Things make a Big Difference website.
Things to consider
Which staff are likely to require a more detailed knowledge of the duty of candour procedure?
Do staff who are meeting with relevant persons feel knowledgeable and confident in determining the impact of the incident on wellbeing?
Organisations must ensure that all such employees receive relevant training and guidance on the duty of candour procedure, and any services and support which may be available to relevant persons.
Organisations must provide relevant persons with details of needs-based services or support. Organisations should consider the relevance of services and support such as counselling, bereavement support and independent advocacy.
Through meetings and discussion with relevant persons, organisations should determine the impact of the unintended or unexpected event on their health and wellbeing. This will assist with identification of their needs and the way in which services or support might provide them with assistance.
Organisations must provide any of their employees who were involved in the incident with details of any services or support of which the organisation is aware which may be able to provide assistance or support to any such employee, taking into account the circumstances relating to the incident; and the employee's needs. This may take the form of debriefing or direct support.
Related documents
Letter sent by the Scottish Government setting out the duty of candour procedure obligation on NHS Boards during the coronavirus pandemic.
Contact
There is a problem
Thanks for your feedback