NHSScotland Chief Executive's Annual Report 2012/13
The NHSScotland Chief Executive's Annual Report 2012/13 presents an assessment of the performance of NHSScotland in 2012/13 and describes key achievements and outcomes.
Chapter 4 Improving Health and Reducing Inequalities
IMPROVING HEALTH AND REDUCING INEQUALITIES
Over the last few decades, the health and life expectancy of the Scottish population has improved. However we have seen a growing gap between the rate of improvement of our most affluent and most deprived communities. NHSScotland has a central role to play in helping all of the people of Scotland to lead and to live longer, healthier lives through anticipatory care and early interventions. This chapter sets out the key areas of achievement in support of improving health and reducing inequalities in health across Scotland during 2012/13.
MINISTERIAL TASKFORCE ON HEALTH INEQUALITIES
At the end of 2012 and under the Chair of the Minister for Public Health, the Ministerial Task Force on Health Inequalities, whose first report was published in 2008, reconvened. It has continued to meet during 2013 where discussions have emphasised the need to tackle the underlying social and economic factors of health inequalities and the possible effects of welfare reform. The Task Force has also taken the opportunity to explore the part 'place' and 'social connectedness' have to play, particularly in connection with Community Planning Partnerships. The Task Force will publish its recommendations in 2013/14.
WELFARE BENEFITS REFORM
Concerns over the potential negative impacts of Welfare Benefits Reform on population health led to NHS Highland conducting a literature review and presenting evidence to the Parliamentary Finance Committee in June 2012. Subsequent work by the Scottish Public Health Network (ScotPHN) resulted in the publication in December 2012 of interim guidance to support NHS Boards on mitigating measures, based on the material gathered and the various discussions undertaken at local and national level[47]. A national Health Impact Delivery Group has been convened with representatives from NHS Boards, COSLA, third sector bodies and the Scottish Government. The group aims to develop a work programme to identify practice to enable NHS Boards to support people who are negatively impacted upon by welfare reform, improve collaboration with other agencies and support organisations, and facilitate better access to relevant support such as advice services. The group met for the first time in October 2012.
KEEP WELL
Delivery of Keep Well anticipatory care health checks continued throughout 2012/13. Under the programme, 40 to 64 year olds living in deprived communities are invited to attend a health check, typically within their local GP practice but also in other local settings. The health checks focus primarily on Cardiovascular Disease (CVD) and its main risk factors, such as blood pressure, cholesterol, smoking and diabetes. In 2011, a process of mainstreaming Keep Well began across NHS Boards in Scotland with the aim of making it part of normal permanent practice. As part of the mainstreaming programme, Keep Well has been extended to specific populations, such as carers, homeless people, offenders, gypsy travellers and certain ethnic groups which, evidence suggests, are at increased risk of CVD and other health inequalities.
CHANGING SCOTLAND'S RELATIONSHIP WITH ALCOHOL
Considerable progress has been made on implementing key aspects of the Alcohol Framework, including: a record investment in tackling alcohol misuse of over £237 million since 2008 - the bulk of the funding (£211 million) being invested in local prevention, treatment and support services; and delivery of over 366,000 Alcohol Brief Interventions by NHSScotland. Work on developing an Alcohol and Drug Quality Improvement Framework includes taking forward actions to support the recommendations of Quality Alcohol Treatment and Support (QATS)*. The Alcohol (Minimum Pricing) (Scotland) Act 2012 was passed in June 2012. An NHS Health Scotland report, Monitoring and Evaluating Scotland's Alcohol Strategy: The Impact of the Alcohol Act on Off-Trade Alcohol Sales in Scotland*, published in May 2013, showed that alcohol sales have fallen by 2.6 per cent in the year following the introduction of the Alcohol etc. (Scotland) Act in October 2011, which included a ban on multi-buy promotions.
MINIMUM UNIT PRICING OF ALCOHOL
The Alcohol (Minimum Pricing) (Scotland) Act was passed in May 2012. The European Commission was notified of our intention to introduce a minimum price of 50 pence per unit of alcohol under the Technical Standards Directive notification process. The policy has been challenged by a judicial review in the domestic courts. This was successfully defended in the Outer House of the Court of Session, however has been appealed by the Scottish Whisky Association and others. A further hearing will take place. The Court judgement on 3 May 2013 found comprehensively in favour of the Scottish Government. The Court recognised the overwhelming evidence supporting the legitimate aims of Minimum Unit Pricing to reduce alcohol consumption, with a particular focus on reducing consumption by hazardous and harmful drinkers who experience so much of the alcohol-related harm we see in Scotland.
Evidence shows that addressing price is an important element in any long-term strategy to tackle alcohol misuse given the link between consumption and harm, and the evidence that affordability is one of the drivers of increased consumption. Minimum pricing will target heavy drinkers as they tend to drink the cheap, high-strength alcohol that will be most affected by the policy. The Scottish Government believes that a minimum price per unit of alcohol would be the most effective and efficient way to tackle alcohol misuse in Scotland.
ALCOHOL AND DRUG PARTNERSHIPS
The Scottish Government and NHSScotland continue to work in partnership with Alcohol and Drug Partnerships (ADPs) to provide support for those affected by alcohol and drug use. Responsibility is devolved to the 30 ADPs across Scotland to commission evidence-based, person-centred and recovery-focused prevention and treatment services to meet the needs of their resident populations. A Scottish Government team of specialist ADP Delivery Advisors is in place to support capacity building and sharing of learning and good practice amongst ADPs.
ALCOHOL BRIEF INTERVENTIONS
There has been excellent progress of the national Alcohol Brief Interventions (ABI) programme across Scotland. Over 366,000 ABIs (which include 94,916 ABIs in 2012/13) have been delivered between 1 April 2008 and 31 March 2013 by NHSScotland to help individuals cut down on their drinking to within safer guidelines[48]. These person-centred, evidence-based and cost-effective preventative interventions potentially reduce the requirement for more costly alcohol-related treatments later on, playing an important part in the Scottish Government's wider strategic approach to tackling alcohol misuse. In order to support embedding of ABI delivery, the HEAT standard is continuing for 2013/14.
DRUG AND ALCOHOL TREATMENT WAITING TIMES
The HEAT target to improve access to drug and alcohol treatment services has been exceeded at national level with 94.6 per cent of people in need receiving treatment to support them to recover within three weeks of referral[49]. This was an ambitious target involving significant efforts from NHS Boards, Alcohol and Drug Partnerships (ADPs) and service providers. To embed performance and encourage continued improvements, the HEAT target has evolved to a HEAT standard for 2013/14 on the same basis of ensuring that at least 90 per cent of people in need receive treatment within 3 weeks. This success is an important first step in a broader programme of work to ensure the delivery of effective, efficient, person-centred recovery services across Scotland.
HEAT TARGET
By March 2013, 90 per cent of clients will wait no longer than 3 weeks from referral received to appropriate drug or alcohol treatment that supports their recovery.
In the quarter ending March 2013, 94.6 per cent of clients received their first treatment within 3 weeks of their referral. The chart below shows performance since the quarter ending June 2011.
Chart 13
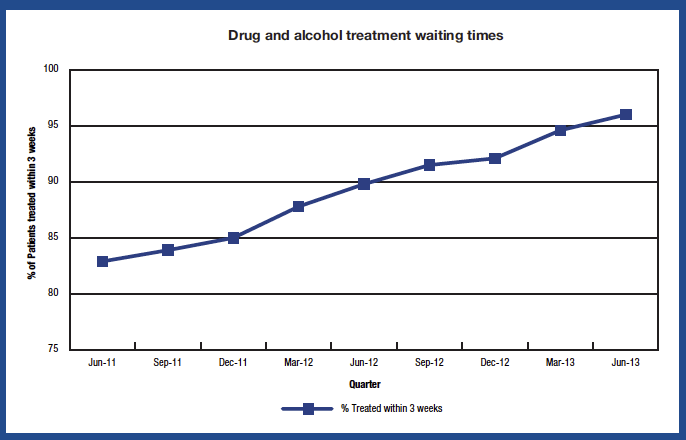
Source: ISD Drug and Alcohol Treatment Waiting Times Database
SMOKING CESSATION
The smoking cessation HEAT target, introduced from April 2011, to build on the success of the previous target will enter its final year in 2013/14. NHSScotland has a target to deliver universal smoking cessation services to achieve at least 80,000 successful quits (at one month post quit) including 48,000 in the 40 per cent most deprived within-Board Scottish Index of Multiple Deprivation (SIMD) areas over the three years ending March 2014. The target has a specific focus on inequalities with the aim of reducing the significant disparities in smoking rates between the most and least disadvantaged populations across Scotland. This in turn is a major contributor to premature mortality and health inequalities.
NHSScotland has delivered the required target levels for the current smoking cessation HEAT target one year early. Over the period April 2011-March 2013, there were 89,353 successful quits at one month, with 50,154 of these in the most deprived areas[50].
Creating a Tobacco-Free Generation: A Tobacco Control Strategy for Scotland* was published in March 2013 and set out a high level target to achieve a smoke-free Scotland status (fewer than 5 per cent of the population smoking) by 2034. The new strategy commits to the development of a successor target to the current HEAT target, which will focus specifically on addressing health inequalities and work is now underway to develop the target. There is also a specific action for NHSScotland grounds to be smoke-free by 2015.
FOOD AND DIET
In Scotland, bad eating habits are the major cause of ill health. Scotland has one of the highest levels of obesity in Organisation for Economic Co-operation and Development (OECD) countries, with a consequent increased risk of conditions such as diabetes, heart diseases and cancer[51]. In June 2012, Scottish Ministers agreed to create a new food body for Scotland. The decision followed the recommendations of the Scudamore review, which was commissioned by the Scottish Government as a result of the UK Government's decision to move responsibility for nutrition and food labelling in England from the Food Standards Agency to the Department of Health and the Department of Environment, Food and Rural Affairs in 2010.
The new food body will take over functions presently delivered in Scotland by the UK-wide FSA, but also maintain responsibility for nutrition and labelling. The new body will also offer further benefits for consumers and industry in Scotland, focusing on the need to ensure that food is safe to eat, and improving diet and nutrition for consumers
in Scotland.
MATERNAL AND INFANT NUTRITION
Continued progress has been made in the implementation of Improving Maternal and Infant Nutrition: A Framework for Action*. Significant milestones include the achievement of UNICEF UK Baby Friendly Awards in a large number of maternity units and Community Health Partnerships. Over 80 per cent of babies in Scotland are now delivered in maternity units with Baby Friendly accreditation. Working in partnership with Community Pharmacy Scotland and NHS Boards, the Scottish Government has recently launched a pilot scheme to make Healthy Start vitamins available in all community pharmacies and dispensing practices, an important opportunity to increase the uptake of this nutritional safety net.
PREVENTING OBESITY
All NHS Boards are required to deliver a programme of Child Healthy Weight Interventions. The interventions incorporate diet, physical activity and behaviour change components to children aged 2-15 years and their families. NHS Boards have developed a range of programmes, which include whole class, school-based interventions and small group and one-to-one interventions in community and/or clinical settings. NHS Boards are working towards the overall target of 14,910 interventions between April 2011 and March 2014. During 2012/13, a total of 4,951 interventions were completed with nearly half delivered to children from the two most deprived local Scottish Index of Multiple Deprivation (SIMD) quintiles[52]. By March 2013, a total of 10,183 interventions had been completed since the introduction of the target.
PHYSICAL ACTIVITY
Physical inactivity is one of our major health challenges, contributing to nearly 2,500 deaths each year[53]. The Green Exercise Partnership, which includes NHS Health Scotland, Forestry Commission Scotland and Scottish Natural Heritage, is working with NHS Boards to maximise opportunities to use NHSScotland's outdoor estate as a resource to promote better health for patients, visitors, staff and the wider community. These developments provide increased opportunities for physical activity and mental health benefits as well as contributing to delivering NHSScotland's responsibilities on sustainability, the Healthy Working Lives agenda and the Quality Strategy.
In January 2013, a pilot study began which was developed by NHS Heath Scotland to assess the feasibility of implementing a Physical Activity Pathway to deliver brief advice and brief interventions in Primary Care in Scotland. Practitioners are encouraged to complete an e-learning module to enhance their knowledge of physical activity and health behaviour change and then offered the use of an online screening tool to use
with patients.
YOUTH HEALTH IMPROVEMENT
In 2011, the Scottish Government and NHS Health Scotland established a Youth Health Improvement and Health Inequalities Strategic Leads Group to support strategic leadership and coordination of youth health improvement and health inequalities at local level. The Group brings together a senior representative from each of Scotland's Territorial NHS Boards to support effective implementation of the breadth of policy relating to youth health improvement and health inequalities, and to provide a common platform for this work. In 2012/13 the Group has undertaken work on a number of fronts to improve health outcomes for young people and has produced a series of briefing papers to inform policy and practice at national and local level.
HEALTH WORKS DEVELOPMENT FUND
In 2012/13, a Health Works Development Fund[54] was established to develop innovative practice within NHS Boards to support the delivery of the Health Works* strategy. Five projects received funding. The projects included: the trial of a new individual placement and support service in mental health in partnership with Job Centre Plus; vocational rehabilitation in a forensic mental health service; developing a single point of access to vocational rehabilitation; early identification and access to a functional work assessment for people with a minor head injury; and a workshop with a legal expert exploring the rules of disclosure for people with a mental health diagnosis when applying for jobs. Each delivered a range of successful outcomes including service improvement, development of educational resources and service redesign.
SEASONAL FLU VACCINATION PROGRAMME
NHSScotland successfully delivered seasonal flu vaccine to older people and those with specific risk conditions in winter 2012/13. Uptake rates were 77.4 per cent for over 65s and 59.2 per cent for 'at risk' people under the age of 65. Under 65s uptake rates were the highest achieved to date, however we recognise that further progress in this area is required.
HPV VACCINATION
Uptake figures for the schools-based element of the fourth year of the programme indicate that, by 30 September 2012, uptake of the first dose in S2 reached 93.1 per cent, with 91.7 per cent achieved for the second dose and 82.8 per cent for the third dose[55]. These figures compare favourably to those collected for other parts of the UK.
Contact
Email: Andrew Wilkie