NHSScotland Chief Executive's Annual Report 2012/13
The NHSScotland Chief Executive's Annual Report 2012/13 presents an assessment of the performance of NHSScotland in 2012/13 and describes key achievements and outcomes.
Chapter 3 Key Achievements in Healthcare Quality
KEY ACHIEVEMENTS IN HEALTHCARE QUALITY
In the Quality Strategy we have established three Quality Ambitions that provide the focus for prioritising and integrating activity across NHSScotland, in partnership with the rest of the public sector, the third sector, and with the people of Scotland. In this chapter, we consider healthcare quality achievements and progress during 2012/13 in terms of their relevance to each of the three Quality Ambitions.
QUALITY AMBITION
SAFE
There will be no avoidable injury or harm to people from healthcare they receive, and an appropriate, clean and safe environment will be provided for the delivery of healthcare services at all times.
NHSScotland continues to receive international acclaim for its approach to implementing improvements in patient safety. Through pursuit of our shared Quality Ambition for no avoidable injury or harm across all aspects of healthcare services, we have made significant progress in a range of areas.
During 2012/13, the Scottish Patient Safety Programme continued to show evidence of improving the safety of care provided with a reduction in Hospital Standardised Mortality Ratios (HSMR) in Scotland's acute hospitals and a reduction in surgical mortality. The Programme has been extended into Primary Care and mental health, and in March 2013, the Maternity Care Quality Improvement Collaborative was launched. This Collaborative aims to reduce the number of stillbirths and neonatal deaths by 15 per cent and to reduce the number of severe post-partum haemorrhages by 30 per cent by 2015. There were further improvements in tackling Healthcare Associated Infection (HAI) with reductions in the prevalence of infections including Methicillin-resistant Staphylococcus aureus (MRSA), and cases of Clostridium difficile are now at their lowest level since mandatory surveillance began.
PATIENTS AND THE PUBLIC
THE SCOTTISH PATIENT SAFETY PROGRAMME
Acute Hospitals
The Scottish Patient Safety Programme was launched in January 2008. Within the acute sector its key objectives were: to reduce Healthcare Associated Infection (HAI), to reduce adverse surgical incidents and adverse drug events; and to improve critical care outcomes along with a strengthened organisational and leadership safety culture. Its primary aim was to reduce avoidable mortality and adverse events in Scotland's acute hospitals by 15 per cent by the end of 2012. This aim was increased to a reduction of 20 per cent in avoidable hospital mortality by the end of 2015.
The Scottish Patient Safety Programme is organised into five workstreams: Peri-operative; Critical Care; General Ward; Medicines Management; and Leadership.
Mortality rates for patients admitted to Intensive Care Units (ICU) continue to improve year-on-year in Scotland. Mortality rates for patients admitted to an ICU fell dramatically from a level of 34 per cent in 2003 to 20 per cent in 2012.
Chart 8
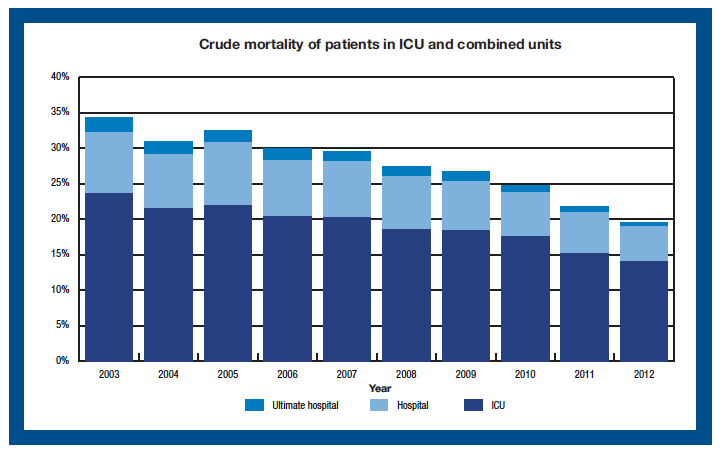
Source: Audit of Critical Care in Scotland 2013 - Reporting on 2012, Scottish Intensive Care Society Audit Group (SICSAG)
Improvements in safety continue to be championed by local teams responding to local needs and pressures. For example, at Stirling Royal Infirmary, a set of safety initiatives that commenced in 2011 are continuing to show improved outcomes for patients.
Chart 9
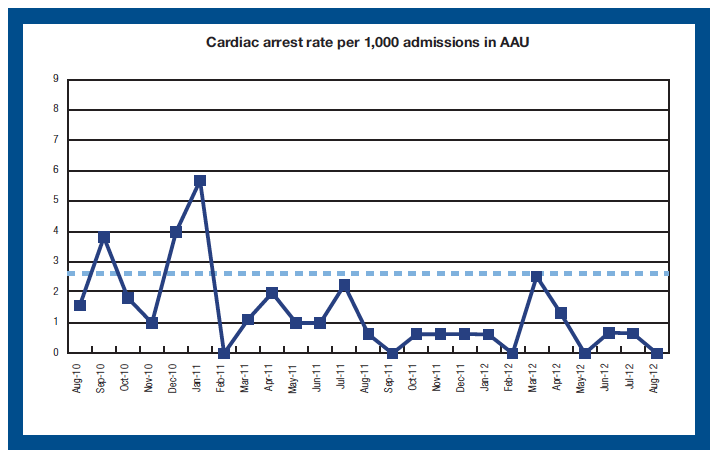
Source: Reducing cardiac arrests in the acute admissions unit: a quality improvement journey - Beckett DJ, Inglis M, Oswald S et al. BMJ, July 2013
Primary Care
The Scottish Patient Safety Programme in Primary Care (SPSP-PC) seeks to improve the delivery of care throughout the patient's journey by providing a targeted, world-leading, evidence-based range of tools, techniques and learning that will improve patient safety. In 2012/13, the early focus was on developing the leadership and organisational culture on safety. An aim was set that, by April 2014, 95 per cent of General Practices will be undertaking Safety Climate Surveys and Structured Case Note Reviews. This ambitious aim will be achieved by the introduction into the GP contract for 2013/14 of some of the key features of the Scottish Patient Safety Programme for Primary Care including the use of the Safety Climate Survey and the trigger tool for case note reviews. It will embed and spread throughout General Practice some of the important elements and lessons learnt from the safety improvement pilot work.
Mental Health
The Scottish Patient Safety Mental Health Programme is a four-year programme of work that aims to reduce episodes of harm caused through people's involvement with mental health services. Initial scoping revealed a lack of clear evidence about the interventions that will reduce harm in mental health. The programme has, therefore, commenced in 2012/13 with an initial one-year prototyping phase - Phase One - which is concentrating on testing interventions to reduce harm experienced by individuals in receipt of care from mental health services. Phase One focused on adult psychiatric inpatient units and forensic units, and has involved all NHS Boards with an inpatient unit (with NHS Orkney and NHS Shetland involved in Phase One but not testing). The work programme for Phase Two will be informed by the outcomes of Phase One prototyping.
Maternity Care
The Scottish Patient Safety Programme Maternity Care Quality Improvement Collaborative was launched on 7 March 2013. The Maternity Care Quality Improvement Collaborative will support the systematic introduction of improvement methodology within the maternity context and will help frontline staff working in maternity services to make changes at a local level which will contribute to the provision of person-centred, safe and effective care for all mothers and babies in Scotland.
SCOTTISH AMBULANCE SERVICE PATIENT SAFETY PROGRAMME
The Scottish Ambulance Service can play a critical role in supporting the Scottish Patient Safety Programme for Sepsis and Deteriorating Patients by identifying potential sepsis at an early stage. A sepsis scoring tool was built into the electronic patient record within the Scottish Ambulance Service PRF system in 2012/13. Associated work is underway with the Acute Medical Unit at Forth Valley Royal Hospital where the screening tool has been implemented for use by ambulance staff pre-hospital. Ambulance crew staff alert the receiving hospital and request a 'sepsis standby' for patients who are identified through the screening tool as having sepsis or at risk of deteriorating. The aim of this initiative is to reduce the number of deaths resulting from sepsis by 10 per cent by December 2014. So far the initiative has seen 69 per cent of those patients identified as being at risk being transported to hospital in time to deliver the sepsis 6 bundle within 60 minutes[9].
HEALTHCARE ASSOCIATED INFECTION
The current Healthcare Associated Infection (HAI) HEAT target is to further reduce Healthcare Associated Infections so that by 2014/15 NHS Boards' Staphylococcus aureus bacteraemia (including MRSA) cases are 0.24 or less per 1,000 acute occupied bed days. The latest figures from Health Protection Scotland (for the year ending June 2013), published on 2 October 2013, confirm that that the rate of Staphylococcus aureus bacteraemia was 0.30. MRSA is currently at the second lowest level recorded since mandatory surveillance began.
CLOSTRIDIUM DIFFICILE
The current Healthcare Associated Infection HEAT target is to further reduce Healthcare Associated Infections so that by 2014/15 NHS Boards' rate of Clostridium difficile infections in patients aged 15 and over is 0.32 cases or less per 1,000 total occupied bed days. The latest figures from Health Protection Scotland (for the year ending June 2013) published on 2 October 2013, confirm that the rate of Clostridium difficile infections in over 15s was 0.35. This is the second lowest level since mandatory surveillance began.
HEAT TARGET (due in 2012/13)
Further reduce Healthcare Associated Infections so that by March 2013 NHS Boards' Staphylococcus aureus bacteraemia (including MRSA) cases are 0.26 or less per 1,000 acute occupied bed days; and the rate of Clostridium difficile infections in patients aged 65 and over is 0.51 cases or less per 1,000 total occupied bed days.
In terms of Staphylococcus aureus bacteraemia (including MRSA), the target is to achieve a reduction in the infection rate to 0.26 cases or less per 1,000 acute occupied bed days by March 2013. For the year ending March 2013, the rate of MRSA/MSSA cases across NHSScotland was 0.30 per 1,000 acute occupied bed days. This represents a fall of 2.5 per cent since 2011/12.
Chart 10
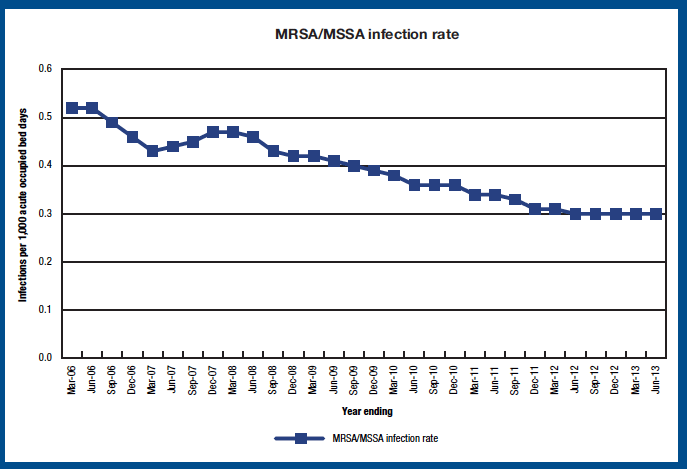
Source: Health Protection Scotland Quarterly Report on SAB (including MRSA)
In terms of Clostridium difficile infections (CDI) amongst those aged 65 years and over, the target is to achieve a reduction in the infection rate to 0.51 cases or less per 1,000 acute occupied bed days by March 2013. For the year ending March 2013, the rate of CDI cases across NHSScotland was 0.37 per 1,000 acute occupied bed days. This represents a fall of 3 per cent since 2011/12.
Chart 11
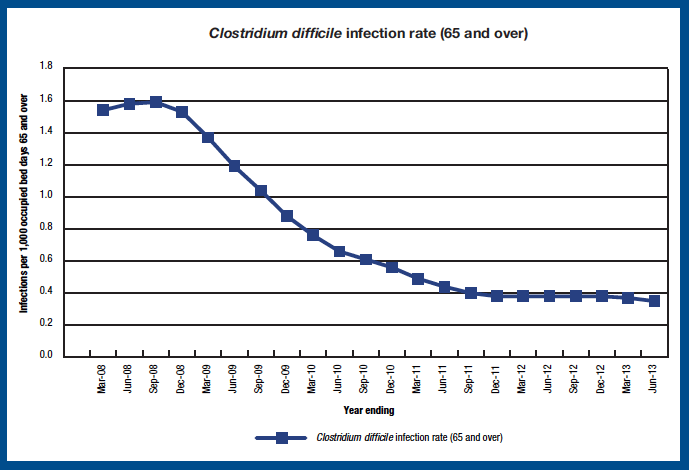
Source: Health Protection Scotland Quarterly Report on Clostridium difficile
HEALTHCARE ENVIRONMENT INSPECTORATE
The Healthcare Environment Inspectorate (HEI) was established in 2009 to provide independent and rigorous scrutiny and assurance of hospitals in Scotland. The aim was to achieve improved performance in tackling Healthcare Associated Infections (HAI) and to ensure that patients and the public can have complete confidence in the cleanliness of hospitals and the quality and safety of services. The latest Chief Inspector's Annual Report (2011/12), published on 5 February 2013, highlighted a significant reduction in the number of requirements issued to NHS Boards (110 requirements compared to 210 requirements in the previous year)[10]. From October 2012, the HEI is delivering at least 30 inspections each year, focusing on acute hospitals and ensuring the majority of inspections are unannounced. The HEI will also focus attention on hospitals that present a higher risk to patients and has started inspecting community hospitals. At the end of this inspection year (September 2013), the HEI will have carried out 32 HAI inspections - two of which were announced.
REDUCING FALLS
The National Falls Programme has been progressing the development of a Framework for Integrated Falls Prevention and Management Pathways across Scotland. During 2012/13, this work programme was driven by the Falls Leads across NHS Boards in partnership with local authorities, the Scottish Ambulance Service and various stakeholders. New resources to support prevention awareness and self-management have been developed and the Care Bundle has been tested in Fife. Work is also underway to reduce falls in hospital as part of the new Scottish Patient Safety Indicator programme. Partners across Scotland and Europe are exploring the use of technology to enhance integrated falls pathways as part of the European Innovation Partnership for Active and Healthy Ageing.
CHILD PROTECTION GUIDANCE FOR HEALTH PROFESSIONALS - THE PINK BOOK
Following the manifesto commitment to review the existing guidance for health professionals on child protection, the updated Child Protection Guidance for Professionals (A Revision Of The Pink Book)* was published in December 2012. The guidance supplements the National Guidance for Child Protection in Scotland*. The overall aim of the guidance is to act as a practical reference point for all healthcare staff working within an adult and child service context.
SUICIDE PREVENTION
Between 2000/02 and 2010/12, the European age-sex standardised rate of suicide decreased by 18 per cent, from 17.4 per 100,000 population to 14.3 per 100,000 population[11]. In February 2013, the Scottish Government published an engagement paper seeking the views of the public on future strategy for prevention of suicide and self-harm. This process was supported by several public engagement events. Plans are now in hand to publish a new suicide prevention strategy in late 2013.
INSPECTION FOR PRACTICES PROVIDING GENERAL DENTAL SERVICES
A new combined practice inspection process for NHS dental practices was introduced on 1 January 2013. This provides an effective and efficient single inspection system. The combined practice inspection process monitors quality of facilities and helps ensure the safety of patients by applying uniform standards, including decontamination requirements. This is used as part of the three-year rolling programme of inspections carried out by NHS Boards.
STAFF
NATIONAL CONFIDENTIAL ALERT LINE
A national confidential alert line was developed to further support and encourage staff to raise concerns about patient safety and malpractice in NHSScotland. Public Concern at Work, an independent whistleblowing charity, was awarded the contract to run the service. This will enhance existing whistleblowing policies by providing confidential advice and support to staff who have doubts about whether/how to raise concerns about patient safety or malpractice. This service, which was launched on 2 April 2013, also provides a safe space where staff can raise concerns and where appropriate, have these passed to the appropriate regulatory body.
CLEANLINESS CHAMPIONS
The Cleanliness Champions Programme (CCP)[12] continues to play a major role in driving down infection rates. The programme is widely recognised in NHSScotland and it is now seen as a basic requirement for infection prevention and control practice. In many NHS Boards, it is a key part of the local Healthcare Associated Infections Learning Strategy. Version 3 of the programme is now being delivered for NHSScotland and other health and social care staff. The Cleanliness Champions Programme is a work-based educational training programme designed to equip healthcare workers with the skills and knowledge necessary to ensure good local practice in preventing Healthcare Associated Infections and to take on the role of Cleanliness Champion. At April 2013, over 15,000 NHSScotland staff had completed the Programme, representing approximately 10 per cent of the total NHSScotland workforce. In addition, it is estimated that over 10,000 students and non-NHS health and social care staff have completed the programme.
NHS Lothian Story Tips for Trips and Hips[13]
Falls are a major problem for older people, and can lead to a significant number of fractured bones and hospital admissions. It can also impact on patient morbidity and mortality, carer experience and length of hospital stay.
NHS Lothian serves 700,000 people and has 3,000 adult inpatient beds in 21 hospitals. Inpatient falls account for 25 per cent of all reported incidents for NHS Lothian. In order to reduce the number of falls in their hospital by 20 per cent, a team looked at the trend in the falls and used a 'Pareto chart of falls resulting in major harm' to identify where most incidents occurred.
From these results, two pilot wards were identified to test a specific 'falls prevention bundle'. The results of the pilot showed that early compliance and improvement was encouraging but not sustained.
The next step in the process was to test a model for improvement - PDSA (Plan, Do, Study, Act) - with a group of dedicated nursing staff. As a result, a revised intervention was designed with staff engagement. This was a Care-Rounding tool which is based on individual patient assessment. It ensures that patients are checked and all care needs met at planned intervals based on risk assessment. The tool includes all elements of care including falls prevention, pressure ulcer prevention care, food, fluid and nutrition, continence and pain assessment. Its collective approach responded to the need of clinical staff to have alignment of improvement interventions.
This new intervention was piloted and enthusiastic clinical leadership was harnessed to ensure a culture of safety and improvement and readiness for the two-year change.
Currently, the clinical staff review five patient records per week to measure compliance with Care-Rounding and enter their data into Quality Improvement Data System (QiDS) which provides an up-to-date visual display of their data which is used to drive improvement.
Falls and harm data is collected using Datix web based incident reporting. This data and process measures from QiDS populate a ward scorecard enabling staff to link process reliability with outcomes, thereby providing safer care.
This was a real journey for the team who had to look at themselves as improvers and take corporate responsibility for aligning the different workstreams.
QUALITY AMBITION
EFFECTIVE
The most appropriate treatments, interventions, support and services will be provided at the right time to everyone who will benefit, and wasteful or harmful variation will be eradicated.
Many of the areas for improvement that have been prioritised over 2012/13 make a direct contribution to our Quality Ambition for more effective healthcare services. A focus of this activity has been to identify those improvements where there is clear and agreed evidence of clinical and cost-effectiveness, and to support the spread of these practices where appropriate to ensure that unexplained and potentially wasteful or harmful variation is reduced.
Key areas of progress are set out in this section for both patients and the public, and for staff. Publication of the Scottish Government consultation document on the integration of adult health and social care signalled the Government's intention to improve outcomes for people by providing consistency in the quality of services, ensuring people are not unnecessarily delayed in hospital and helping them to maintain their independence by creating services that allow them to stay safely at home for longer. Progress also includes further improvements in waiting times with 90.6 per cent of patients seen and treated within 18 weeks of referral at March 2013. Children and young people requiring mental health services are also benefiting from quicker access to services.
Major campaigns were launched in 2012/13 to raise awareness of the signs of breast and bowel cancer. There are already positive early signs of increased awareness and activity. As a result of work in dementia diagnosis, Scotland now has the highest rate of dementia diagnosis in the UK (65 per cent in Scotland compared to 42 per cent in England). In the quarter ending 31 March 2013, 96 per cent of children and adolescents requiring mental health services were seen within 26 weeks, with the average wait currently seven weeks. During 2012/13, a new Transcatheter Aortic Valve Implantation (TAVI) service for Scotland was introduced providing treatment for patients with severe aortic stenosis who are not suitable for standard surgical valve replacement.
PATIENTS AND THE PUBLIC
INTEGRATION OF HEALTH AND SOCIAL CARE
In May 2012, the Scottish Government published a consultation document, which invited views on proposals for the integration of adult health and social care in Scotland. In addition, a series of consultation events were held with a wide range of stakeholders to discuss the proposals for reforms. During the year, work was undertaken ahead of the introduction to Parliament on 28 May 2013 of the Public Bodies (Joint Working) (Scotland) Bill 2013. The Bill sets out the legislative framework for integrating health and social care including provisions such as: the removal from statute of Community Health Partnerships; the establishment via secondary legislation of national outcomes for health and wellbeing; and the requirement that NHS Boards and local authorities will establish integrated partnership arrangements - Health and Social Care Partnerships.
Two models of integration are available for NHS Boards and Local Authorities to choose from: delegation between partners (i.e. lead agency arrangements) and delegation to a body corporate. The NHS Board and local authority will delegate functions and budgets to the integrated partnership. Under the legislation, each integrated partnership will be required to establish locality planning arrangements, which will provide a forum for local professional leadership of service planning. The Bill places a heavy emphasis on the importance of effective joint planning of service provision in light of a shared understanding of population need, informed by professional understanding of local need. Partnerships will be required to engage widely in developing a joint strategic commissioning plan, building on the learning and relationships established in Reshaping Care for Older People.
EARLY YEARS COLLABORATIVE
The launch of the Early Years collaborative in October 2012 marked the world's first multi-agency quality improvement collaborative. The Early Years Taskforce recognised that a great deal of evidence about the impact of investment in the early years exists, in terms of social, emotional, educational, health and economic outcomes. This Collaborative will help organisations close the gap between knowledge and practice by creating a structure in which partners can easily learn from each other and from recognised experts in areas where they want to make improvements. Community Planning Partners work together to make improvements for children, families and communities.
WAITING TIMES
Delivery of short waiting times for patients continues to be a priority and continues to be delivered by NHSScotland. In particular, the 18-week Referral to Treatment (RTT) target was met each month in 2012/13 for NHSScotland.
October 2012 saw the introduction of the Treatment Time Guarantee (TTG) for inpatients and day cases as part of the Patient Rights Act - the first waiting times target to be enshrined in law. The majority of NHS Boards have delivered this very successfully despite a difficult winter. This is the most challenging inpatient/day case waiting times target to date and NHS Boards need to deliver for each individual patient every day of the year. The 12-week waiting times standard for outpatients and 6-weeks maximum wait for diagnostics remains critically important to patients and to the successful delivery of 18-week RTT and TTG.
The most extensive Waiting Times Audits anywhere in the UK were carried out in all NHS Boards by Board Internal Auditors and Audit Scotland after the Scottish Government instructed NHS Lothian to have their waiting times independently audited. The individual NHS Board audits undertaken by Internal Audit and the National Audit carried out by Audit Scotland were discussed in Parliament and went to the Public Audit Committee. It is reassuring that, outwith NHS Lothian, the Auditor General for Scotland identified no deliberate manipulation. We are not complacent, however, and improvements identified by the auditors were welcomed and fully accepted. There will be further audits undertaken by Audit Scotland and NHS Board Internal Auditors, which will report by the end of 2013.
We have re-emphasised our sophisticated performance management approach to waiting times, including our principles which make it clear that patient need is always more important than the delivery of targets and standards.
CANCER WAITING TIMES
NHSScotland achieved and sustained good performance against the 62- and 31-day cancer access standards throughout 2012. During the final quarter October to December 2012, 95.8 per cent of patients started treatment within 62 days of urgent referral with a suspicion of cancer. Within the same period, 98.1 per cent of patients started treatment within 31 days of decision to treat, irrespective of the route of referral[14].
DETECT CANCER EARLY PROGRAMME
Further progress has been made with the Detect Cancer Early Programme. A HEAT target for Detect Cancer Early was introduced from April 2012, to increase the proportion of people diagnosed and treated in the first stage of breast, colorectal and lung cancer by 25 per cent by 2014/15. A bold and highly acclaimed breast cancer awareness campaign was aired, followed by a campaign to support informed participation in the national bowel screening campaign. A Primary Care contract initiative was developed to complement this and work to refresh the cancer referral guidelines has also been taken forward. The first set of data for stage of cancer at presentation was published as a baseline for monitoring progress towards the HEAT target achievement. A total of £6.7 million has been allocated in this first year of the programme, which aims to improve Scotland's five-year cancer survival rates[15].
COLORECTAL CANCER
Research funded by the Chief Scientist Office (CSO) has shown that colorectal cancer screening by the NHS reduces deaths by 10 per cent overall, and by more than 25 per cent among those who take up the offer of screening. The work, which was supported by a CSO programme grant to set up a bowel screening research centre, is the first to show that a national screening programme can produce benefits similar to those found in smaller, experimental trials.
ACCESS TO SPECIALIST CHILD AND ADOLESCENT MENTAL HEALTH SERVICES
NHS Boards have continued to pursue the aim that, from March 2013, no one will wait longer than 26 weeks from referral to treatment for specialist Child and Adolescent Mental Health Services (CAMHS). In January-March 2013, 96 per cent of patients started treatment within 26 weeks, and the median wait was 7 weeks[16]. Improving access to CAMHS has been supported by significant investment in the specialist workforce, with a 45 per cent increase in the size of the workforce since September 2008[17]. NHS Boards are now working towards the target of 18 weeks from December 2014.
HEAT TARGET
Deliver faster access to mental health services by delivering 26 weeks referral to treatment for specialist Child and Adolescent Mental Health Services (CAMHS) from March 2013; reducing to 18 weeks from December 2014; and 18-week Referral to Treatment for Psychological Therapies from December 2014.
Waiting times information for CAMHS is still at an early stage of development. NHS Boards are working with ISD and the Scottish Government to improve the consistency and completeness of the information. To report on CAMHS waiting times, NHS Boards have had to develop, for the first time, systems to measure CAMHS waiting times from referral to treatment. During the quarter ending March 2013, 3,971 children and young people started treatment at CAMHS in Scotland. The initial estimates from data at an early stage of development indicate that around 96 per cent of people were seen within 26 weeks.
UNSCHEDULED CARE
Attendances at emergency departments across Scotland have been rising over the past five years. Combined with an ageing population requiring more acute care, this has acted to increase pressure on unscheduled care. An Unscheduled Care Expert Group has identified the need to improve access to assessment, diagnostics and treatment, and to improve the outcomes of care using a whole system approach. A National Improvement Programme has been established to support improvements in unscheduled care which will see an investment of £50 million over three years, and reaffirms the commitment to sustainably achieving the 98 per cent emergency access standard for all patients attending emergency departments to be admitted, discharged or transferred within 4 hours.
Evidence from Day of Care audits has shown that as many as 25 per cent of patients receiving acute hospital care could have received that care in a more appropriate setting. Prompt access to a senior decision-maker can ensure appropriate and effective treatment is commenced as promptly as possible. To support this, an investment of £1.8 million has been made to recruit additional Emergency Care Consultants. Early assessment by the multi-disciplinary team including, where appropriate, social care, can ensure patients are supported to recover and are discharged to the right place without delay.
GMS CONTRACT AGREEMENT IN SCOTLAND
The GMS contract agreement in Scotland for 2013/14, achieved in 2012/13, reflected a negotiated deal for GPs. This brings significant benefits for patients, with GPs working more closely with those patients most at risk of hospital admission, whilst addressing some of their workload pressures. The agreement brings significant clinical improvements: improved care for patients with rheumatoid arthritis, raised blood pressure and cholesterol; and an extended immunisation programme for adults and children. It embeds key elements of the Scottish Patient Safety Programme in General Practice. This agreement has paved the way for closer, more productive working with General Practice.
TRANSCATHETER AORTIC VALVE IMPLANTATION (TAVI)
A new national Transcatheter Aortic Valve Implantation (TAVI) service, based in Edinburgh, was established in September 2012. TAVI is a treatment option for some patients with severe aortic stenosis who are not suitable for standard surgical valve replacement. In its first six months of operation, the service has seen and treated more than 20 patients and is expected to treat around 60 people in its first full year[18].
INSPECTIONS OF CARE FOR OLDER PEOPLE IN ACUTE HOSPITALS
The programme of inspections by Healthcare Improvement Scotland[19] into the care of older people in acute hospitals continued throughout 2012/13. At 31 March 2013, 12 announced inspections, one unannounced inspection and four follow-ups had taken place across eight NHS Boards, with 13 reports and a six-month overview summary report published. The reports highlight many strengths in the quality of care provided to older people and positive care experiences for the vast majority of patients. A number of areas of continuing improvement were also noted.
CORONARY HEART DISEASE AND STROKE
National Records of Scotland statistics show that deaths from coronary heart disease and stroke have fallen by 48 per cent between 2001 and 2012 for those aged under 75[20]. This remarkable achievement reflects substantial investment in effective treatments, roll out of health improvement measures such as smoking cessation, and the ongoing dedication of NHSScotand staff. The Scottish Government remains committed to ensuring that this trend continues. Improving the care of people with stroke and heart disease will continue to be a clinical priority for NHSScotland.
Stroke remains one of the biggest killers in Scotland and a leading cause of disability. A HEAT target was introduced to increase stroke patient access to stroke units. This aimed to ensure that 90 per cent of all patients admitted with a diagnosis of stroke are admitted to a stroke unit on the day of admission, or the day following presentation by March 2013. Access to stroke units improved by over 10 per cent over the course of the target with 80 per cent of people with stroke admitted to a stroke unit within one day of admission during January-March 2013, compared to 68 per cent in 2010[21]. We will learn and build on our experience with the target and put in place measures to drive the necessary service improvements in order to deliver the best possible care for stroke patients.
In support of effective stroke treatment, people living within 11 out of 14 Territorial NHS Board areas in Scotland now have access to 24/7 stroke thrombolysis treatment through telestroke networks that provide access to immediate stroke specialist decision support. With thrombolysis treatment needing to be given within 4.5 hours from the onset of symptoms to be effective, NHS Board areas which had implemented telestroke had a 147 per cent increase in treatment rates compared to a 23 per cent increase in treatment rates for Boards not using (or not requiring) telestroke[22].
HEAT TARGET
To improve stroke care, 90 per cent of all patients admitted with a diagnosis of stroke will be admitted to a stroke unit on the day of admission, or the day following presentation by March 2013.
80 per cent of patients admitted with a diagnosis of stroke in the quarter ending March 2013 were admitted to a stroke unit within one day of admission.
DEMENTIA
A three-year HEAT target was established from April 2013 that by 2015/16, all people newly diagnosed with dementia will have a minimum of a year's worth of post-diagnostic support coordinated by an appropriately trained and skilled link worker. The second Alzheimer Society UK Dementia Map[23], published in 2012 using the Dementia UK prevalence model, shows that up to March 2012 in Scotland around 64 per cent of those with dementia were being diagnosed, in contrast to 44 per cent in England and 38 per cent in Wales.
Continued support was provided for Alzheimer Scotland to appoint a specialist Dementia Nurse in each NHS Board area, to work strategically with NHS Boards to improve the overall care experience of people with dementia admitted to hospital, and to act as a resource for improving practice at the frontline. In collaboration with NHS Education for Scotland (NES) and the University of the West of Scotland, a further 200 staff were trained as Dementia Champions, to act as agents of change within health and social care settings.
NHSSCOTLAND RESILIENCE PREPARATIONS FOR MAJOR INCIDENTS
NHS Boards have continued to improve their resilience planning to cope with major disruptions to their services from such incidents as severe weather and pandemic flu. To support Boards with these activities and to enhance emergency preparedness going into the Commonwealth Games, NHSScotland Resilience within the Scottish Government Health and Social Care Directorates published a number of guidance documents during 2012/13, and has worked with stakeholders and clinicians to prepare revised Preparing for Emergencies[24] guidance which was published in August 2013. This guidance will support NHS Boards to provide a safe and effective response to all disruptive incidents.
ORAL HEALTH AND THE CHILDSMILE PROGRAMME
During 2012/13, the Childsmile Programme continued to improve the oral health of people in Scotland. The most recent survey of Primary 1 schoolchildren in 2012 found that 67 per cent of children in Scotland had no obvious signs of dental decay. This is significantly higher than the 2010 Scottish target of 60 per cent, which all NHS Boards have achieved[25]. The targeted approach of the Childsmile programme will help to further improve the oral health of children in the most deprived communities, who continue to carry an additional burden of dental disease.
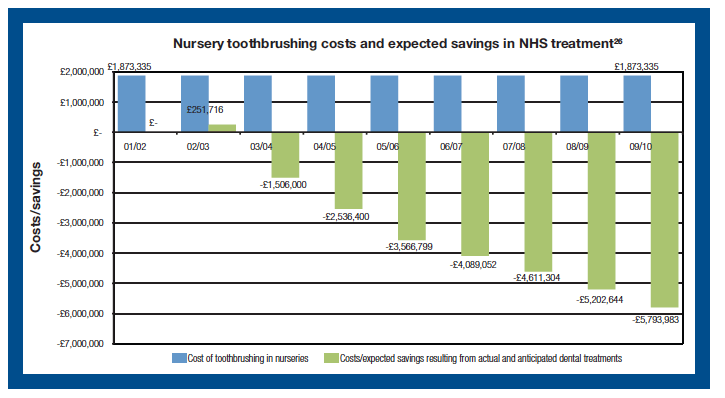
The University of Glasgow was tasked with evaluating the overall benefits of the Oral Health Improvement Programme, starting with the nursery toothbrushing element of Childsmile. This evaluation looked at the amount of treatment that children would otherwise have needed if the decay had not been prevented. It showed that, in addition to the avoidance of fillings, extractions and the need for general anaesthetic, the saving in treatment covered the cost of the preventative action. It is also important to acknowledge the impact of Childsmile on parents and children in avoiding time taken off from school and work to accommodate general anaesthetic appointments.
Chart 11[26]
HEALTH INFORMATICS RESEARCH ADVISORY GROUP
With the aim of building new capacity and setting the international standard in eHealth informatics research, Scottish researchers in October 2012 won over £4 million to establish one of the four UK eHealth informatics research centres. In 2013, the Medical Research Council (MRC) awarded a further £5 million to Scotland to build on the four centres to create a distributed research institute called The Farr Institute of Health Informatics Research. Scotland is leading this UK-wide network. The Scottish Government has committed over £2 million to the initiative and has convened a Health Informatics Research Advisory Group (HIRAG) to consider how the value of these new investments can be maximised.
COLLABORATIONS WITH RESEARCH CHARITIES
In 2013, the Chief Scientist Office (CSO) secured co-funded research opportunities with two major UK-wide research charities: Prostrate Cancer UK; and Alzheimer's Research UK. These were announced by the Cabinet Secretary for Health and Wellbeing and the Minister for Public Health respectively. The funding allocated by the charities to these research opportunities represents an inward investment of around £500,000 for the Scottish research community.
NATIONAL SPECIALIST SERVICES COMMITTEE (NSSC)
Scottish Ministers approved the role, remit, membership and ways of working of the new National Specialist Services Committee (NSSC) in September 2012. The NSSC has rapidly established its role in governance of specialist services and national managed clinical networks, acting on behalf of NHS Board Chief Executives, and providing recommendations to them and to the Scottish Government on the designation and governance of national specialist services commissioned by National Services Division of NHS National Services Scotland (NSS).
NATIONAL DATA BENCHMARKING SERVICE FOR ACUTE HOSPITALS
CHKS Insight is a national data benchmarking service that will directly support improvements in patient safety, the quality of care and clinical outcomes and has been secured for three years from 2013. The service will be implemented across Territorial NHS Boards and the Golden Jubilee National Hospital and provides clinical and managerial staff with a valuable resource that will support them to make focused and timely improvements in the quality of care and services provided by NHS Boards in Scotland. The Insight service will support NHS Boards to identify unwarranted variation in the quality of care and outcomes, and to make improvements where needed by allowing them to understand what is happening at a local level as well as allowing them to make comparisons with other NHS Boards and systems across the UK.
TELECARE AND TELEHEALTH
Already 80 per cent of people assessed as requiring some form of support at home now benefit from telecare purchased from or provided by their local authority, and the use of home monitoring and other forms of telehealth are becoming more common[27]. It is recognised, however, that further work is required to enable more people to use technology to support them to remain at home. In December 2012, the Scottish Government, COSLA and NHSScotland published A National Telehealth and Telecare Delivery Plan for Scotland to 2015: Driving Improvement, Integration and Innovation*. It aims to enable greater choice and control for an additional 300,000 people by 2015 through better use of technology in health and social care. With over £12 million investment already secured and 18 partnerships now engaged in Living it Up, SmartCare and United4Health projects, work over the next few years will see a significant upscaling of the adoption of telehealthcare in Scotland.
RESHAPING CARE FOR OLDER PEOPLE
In 2011, Scottish Ministers introduced a £300 million Change Fund to support the implementation of the Reshaping Care for Older People Programme (RCOP). The Fund is allocated across all 32 Health and Social Care Partnerships in Scotland over the four financial years from 2011/12 to act as a catalyst for improvement and innovative redesign of support and services for older people and their carers. This £300 million continues to drive the development of services that optimise the independence and wellbeing of older people at home or in a homely setting, and to rebalance care and support towards anticipatory and preventative services that enable older people to remain at home.
In 2012/13, Partnerships projected to spend over 52 per cent of their RCOP Change Fund on preventative, anticipatory and proactive community-based services to support people to live at home or closer to home. This was coupled with a reduction in Change Fund expenditure on hospitals and long-stay care homes, down from 23 per cent in 2011/12 to 16 per cent in 2012/13, while spend on preventative and anticipatory care was up by three per cent. The Joint Improvement Team (JIT) is working with policy and workforce leads to promote integrated team-based practice and to test and spread new models for delivering integrated health and social care in localities that ensure a focus on prevention, anticipatory care and enabling independence.
REDUCING EMERGENCY BED DAYS
The rate of emergency bed days for people aged 75 and over has decreased over the past three years. Across Scotland, the rate of emergency bed days per 1,000 patients aged 75 and over reduced by 10.7 per cent from 5,393 in 2009/10 to a provisional 4,814 in 2012/13[28]. The Joint Improvement Team (JIT) supported Community Planning Partnerships to use their data to improve a range of national outcomes. This showed, for example, that in 2012, 33 per cent of older people with complex care needs (defined as receiving more than 10 hours of home care per week) received their care at home compared with 26 per cent in 2003[29]. Delayed discharges over four weeks reduced by 59 per cent and delays over two weeks reduced by 34 per cent between April 2012 and April 2013[30].
HEAT TARGET
No people will wait more than 28 days to be discharged from hospital into a more appropriate care setting, once treatment is complete from April 2013; followed by a 14 day maximum wait from April 2015.
The target is for no people to wait more than 28 days to be discharged from hospital into a more appropriate care setting from April 2013. There were 44 people waiting over 28 days to be discharged from hospital in April 2013, compared with 174 waiting in January 2013.
INNOVATION FOR HEALTH AND WEALTH
Health and New Wealth in Scotland: A Statement of Intent on Innovation for Health* was launched by the Cabinet Secretary for Health and Wellbeing at the NHSScotland Event in June 2012. The Statement promotes the development and adoption of innovative solutions that improve the quality of services, and which allow Scottish industry to increase growth of the Scottish economy. A vital part of this is the partnership working between leading-edge Scottish life science companies and NHSScotland. A joint Government, NHSScotland and industry Innovation Partnership Board was set up to give direction to promoting innovation and building partnerships.
PUBLICATION OF NEONATAL CARE IN SCOTLAND: A QUALITY FRAMEWORK
Neonatal Care in Scotland: A Quality Framework* was published in March 2013, setting out recommendations for the future of neonatal care and supporting NHSScotland in its commitment to deliver evidence-based, safe, effective and person-centred neonatal care in the right place, at the right time by the right people with the right skills. The report was the work of the Neonatal Expert Advisory Group (NEAG) which was established by the Scottish Government and asked to report back on the future of services which deliver specialist hospital care to around 8,000 babies a year.
NEW REHABILITATION SERVICE FOR PEOPLE WITH ME-CFS PILOTED
The Scottish Government has invested £148,000 in NHS Lothian's Myalgic Encephalomyelitis - Chronic Fatigue Syndrome (ME-CFS) pilot rehabilitation service. The project, which began in 2012/13, is now in its second year, and is showing real promise in delivering person-centred care for over 100 adults with ME-CFS. It is expected that the lessons from this pilot will play an important part in informing local service planning, with the project already attracting significant interest from other NHS Boards and health services in Northern Ireland.
ORGAN DONATION AND TRANSPLANT
Scotland has undertaken a number of activities over the period 2008-13, in line with the UK Organ Donation Taskforce. In particular Scotland, unlike other parts of the UK, has continued to run high profile awareness-raising campaigns, which have resulted in Scotland having the highest proportion of the population on the NHS Organ Donor Register. Scotland has also invested in infrastructure, employing additional specialist nurses in organ donation, appointing clinical leads in organ donation, supported the establishment of NHS Board Donation Committees, and work undertaken to improve the consent rates of families to donation. Data released in 2012/13 showed that Scotland had achieved a 74 per cent increase in deceased donation rates from 2008-13, significantly higher than the UK average of 50 per cent increase over the same period. Scotland has also achieved a 36 per cent increase in transplants over the same five-year period, saving and improving many more lives[31].
IMPROVING DIAGNOSIS, TREATMENT AND OUTCOMES FOR PATIENTS
Building on the successful Temperature Post Cardiac Arrest (TOPCAT) studies for the treatment of community cardiac arrests in NHS Lothian, the Scottish Ambulance Service extended testing of the Q-CPR meters within Lothian and Dundee. This technology gives crews 'real time' feedback on the effectiveness of their clinical treatment in terms of cardiopulmonary resuscitation (CPR). Lothian Return of Spontaneous Circulation (ROSC) rates were 23.9 per cent for all cardiac arrests and 39.4 per cent for Ventricular Fibrillation /Ventricular Tachycardia (VF/VT) cardiac arrests and Dundee demonstrated an 8.6 per cent improvement in ROSC during the year[32]. The rollout of this service across Scotland will continue in 2013/14.
STAFF
STAFF GOVERNANCE STANDARD
Following the launch of the fourth edition of the Staff Governance Standard[33] at the NHSScotland Event in June 2012, work began in partnership on a new monitoring framework to replace previous assessment tools, including the Self Assessment Audit Tool (SAAT). Consultation was undertaken nationally and selected NHS Boards will be asked to pilot the National Reporting Framework and the Local Monitoring Framework. The results will allow NHS Boards to evidence good practice and demonstrate the links between Staff Governance and the 2020 Workforce Vision. The new Framework should be launched in late 2013.
ALLIED HEALTH PROFESSIONS NATIONAL DELIVERY PLAN
AHPs as Agents of Change in Health and Social Care - The National Delivery Plan for the Allied Health Professions In Scotland, 2012-2015* was published in June 2012 setting out actions that call for AHPs to be more visible, accountable and impact-orientated in NHS Boards and local authorities. The National Delivery Plan applies to all AHPs from across health and social care and it provides a strategic platform for future AHP activity, demonstrating the contribution and impact that AHPs can and do have on the delivery of national policy. The National Delivery Plan is a first for Scotland and for the UK.
NURSING & MIDWIFERY WORKLOAD MEASUREMENT AND WORKFORCE PLANNING TOOLS
During 2012/13, Scotland continued to lead the UK in further developing ground-breaking Nursing & Midwifery Workload Measurement and Workforce Planning Tools. These tools were developed in partnership with practitioners and staff bodies. They are used as part of a broader approach that incorporates professional judgment and quality measures to determine the number of nurses or midwives needed for particular clinical areas through measurement of actual workload. In December 2012, the application of the tools became mandatory as part of Local Delivery Planning to help ensure that nursing and midwifery workforce planning is consistent, systematic and evidence-based throughout the country and that nursing and midwifery staffing levels are appropriate and responsive to local needs.
MEDICAL REVALIDATION IN SCOTLAND
The revalidation of doctors became a legal requirement across the UK from December 2012, and Scotland has agreed a rollout plan with the General Medical Council (GMC) to ensure all doctors working and delivering services in NHSScotland will have their licence to practice revalidated over a three-year period. The Scottish Government, NHS Education for Scotland (NES) and Healthcare Improvement Scotland (HIS) have worked in close partnership to ensure that NHS Boards have the necessary guidance, tools and resources to deliver this important milestone, which will serve to reassure patients and the public that doctors are up-to-date and fit to practise.
RESHAPING SCOTLAND'S MEDICAL WORKFORCE
2012 was the fourth year of the Reshaping the Medical Workforce Project - the Scottish Government's policy to move away from a service delivered by doctors in training towards a service delivered predominantly by trained doctors as part of a mixed economy of medical and non-medical members of the clinical team. As a result of a review undertaken in February 2012, a specialty-by-specialty risk analysis approach was adopted, giving NHSScotland the ability to vary the rate of movement towards a trained medical workforce across different specialties. Reshaping was paused in 13 specialties, including Emergency Medicine and a number of other 'front-door' medical specialties. Significant progress towards a service delivered predominantly by trained doctors had been made in a further 25 specialties and this is expected to continue in 2013/14. In addition, it was agreed in 2012 that 'Reshaping' had been achieved in a total of 16 specialties.
RESEARCH CAPACITY - CAREER RESEARCHER FELLOWSHIP SCHEME
The 34 NHS clinicians who were successful in the competition for NHS Research Scotland (NRS) Career Researcher Fellowships took up post from April 2012 onwards. In most cases, the Fellowships buy out one or two days a week of the Fellow's time to carry out clinical research focused on improving patient care. In Lanarkshire, two Fellows in respiratory medicine initiated the first commercial asthma trial in the region in late 2012. The success of the scheme and quality of Fellows appointed resulted in a second competition being run in late 2012, bringing the total investment in this scheme to £6 million.
FIRST NEW GRADUATES OF ABERDEEN DENTAL SCHOOL
This year saw the first tranche of students graduating from the new Dental School in Aberdeen. The establishment of the new school was a manifesto commitment in 2007 with the first students starting in 2008. It is a graduate entry course with students coming from a background in biomedical sciences. The dental school will help in the development and retention of a high quality dental workforce in the North of Scotland.
KNOWLEDGE NETWORK SUPPORT FOR EFFECTIVE CARE
The NHS Education for Scotland (NES) Knowledge Network provides staff with equal access to learning and development resources, supporting them in work-based learning and effective use of technology to support new models of care. During 2012/13, the Knowledge Network provided knowledge in a variety of formats for use in frontline care including: a mobile app for sepsis diagnosis and management; a mobile clinical enquiry service; and a clinical decision support demonstrator. The Network supported the creation of 48 communities of practice, using online community and social networking tools in quality improvement, patient safety, dementia, palliative care and other priority areas. Training was provided for 3,356 health and social care staff in finding, sharing and using knowledge through Knowledge Network services[34].
ESTATES AND FACILITIES
REDUCING CARBON EMISSIONS AND ENERGY CONSUMPTION
During 2012/13, NHSScotland delivered a 5.84 per cent reduction in energy consumption compared to the baseline year of 2009/10, thus exceeding the target by 2.93 per cent. CO2 emissions from fossil fuel use were reduced by 7.86 per cent over the same period which missed the target by 0.69 per cent[35]. It is expected that the EcoHospitals funding programme for NHSScotland recently announced as part of the Scottish Government's Green Stimulus Package will have a significant and tangible impact on NHSScotland's direct carbon emissions and energy efficiency over the next few years. This programme will see over £24 million invested in energy and carbon reduction projects over the next three years, leading to annual reductions of over 41,000 tonnes of CO2 - equivalent to over 7.5 per cent of current NHSScotland CO2 emissions.
NHS Forth Valley Story This Bundle Saves Lives[36]
Heart failure is associated with high mortality, morbidity, readmission rates and length of stay. Well-established drugs and interventions are recognised but need to be reliably implemented.
In order to improve care for inpatients with heart failure secondary to Left Ventricular Systolic Dysfunction (LVSD), the cardiology unit at NHS Forth Valley Royal Hospital developed a 'bundle' consisting of a carefully packaged small set of standards each with a strong evidence-base. For compliance, the following three elements had to be completed: expert review (heart failure nurse or consultant cardiologist); prescription of evidence-based drugs; and referral to the heart failure nurse service.
All patients admitted with heart failure secondary to LVSD within the cardiology unit were managed with this heart failure bundle. A programme of heart failure training was also delivered to heart failure ANPs who were promoted as local 'experts'. The team also actively sought patients from the acute admissions unit to bring to their wards for bundle-driven care. Data were collected weekly with results showing 100 per cent compliance with all elements of the bundle, in all patients was achieved. Re-admissions, length of stay, in-hospital mortality and long-term mortality in patients was measured before bundle introduction and after reliable compliance. The bundle reduced re-admission rates and mortality.
This bundle of care delivered significant benefits to heart failure patients with LVSD. Small changes were tested and the process refined using Plan, Do, Study, Act (PDSA) cycles. The team noted the need to ensure good physician engagement and the need for more pre-implementation data and emphasis on outcome measures to address this. It also noted the importance of up-skilling heart nurses to become 'experts'.
The cardiology team at NHS Forth Valley General learned never to refer to improvement work as 'our project'. Instead it should be core business and therefore everybody's business.
QUALITY AMBITION
PERSON-CENTRED
Mutually beneficial partnerships between patients, their families and those delivering healthcare services which respect individual needs and values and which demonstrate compassion, continuity, clear communication and shared decision-making.
During 2012/13, we made some important progress towards our Quality Ambition for person-centred healthcare. In this section we set out details of progress on the range of initiatives that are being pursued across NHSScotland for the benefit of patients, carers, the public and for staff.
Key areas of progress include improvement in people's experiences of their care with national results from the Inpatient Experience Survey and the Survey of GP and Local NHS Services showing 85 per cent of inpatients in our hospitals rate their care and treatment as excellent or good and 89 per cent of patients reported that the care provided by their GP practice was excellent or good. In addition, the 2013 maternity patient experience survey was rolled out - the first national survey looking at women's experience of maternity care in 15 years.
The Person-Centred Health and Care Collaborative was launched to provide a framework for reliably testing and spreading best practice in person-centred care and Patient Opinion, a new national feedback website, was launched. The ePharmacy Programme has been revolutionising the way GP prescriptions are issued.
PATIENTS AND THE PUBLIC
LAUNCH OF THE PERSON-CENTRED CARE COLLABORATIVE
The Person-Centred Health and Care Collaborative is a flagship piece of work which provides a framework for reliably testing and spreading best practice in person-centred care. The Collaborative was launched as part of a programme of activity at a national learning event in November 2012 for health and social care staff from across Scotland. Following a second learning session in May 2013, local teams are beginning to drive change in health and care settings across Scotland. The Collaborative is a partnership led by Healthcare Improvement Scotland (HIS), involving NHS Education for Scotland (NES), and the Health and Social Care Alliance Scotland (the Alliance), working together with NHS Boards and their local partners.
PATIENT EXPERIENCE
Patient experience evidence has been established as a key component of how the performance of the health and social care system is judged. Building on the 2011/12 survey of people using GP and Local NHS services, a further analysis of the variation in patient experience was produced. This clearly showed that the individual GP practice can make a substantial difference to the patient experience and therefore GPs have a clear role in delivering improvement. In addition, the 2012 survey of inpatient experiences was published and the 2013 maternity patient experience survey was rolled out - the first national survey looking at women's experience of maternity care in 15 years.
KEY FINDINGS
2011/12 PATIENT EXPERIENCE SURVEY OF GP AND LOCAL NHS SERVICES
The experiences of Scottish GP patients in 2011/12 were similar to those reported for 2009/10:
- Patients were mainly positive about their experience of consultation with doctors or nurses. At least 90 per cent of patients responded positively to all of the questions about doctors and nurses.
- Patients remained very positive about their involvement in their care and treatment. Overall 89 per cent of patients felt that the care provided by the GP surgery was excellent or good.
Patients were slightly more positive about their experiences of doctors and nurses than they were in the 2009/10 survey.
Patients were less positive about their experiences of accessing GP practice services - there was a decrease in the percentage of patients rating the overall arrangements for seeing doctors and nurses as good or excellent. This decrease was seen across almost all NHS Boards. As in 2009/10 there was considerable variation in the results for individual GP practices on patients' experiences of the overall arrangements for seeing doctors.
Patients were generally positive about their experiences of out-of-hours healthcare with 72 per cent rating their overall care they received as good or excellent. However 11 per cent of patients rated the overall care as poor or very poor.
KEY FINDINGS
2011/12 PATIENT EXPERIENCE SURVEY OF GP AND LOCAL NHS SERVICES
In 2012/13, additional analysis of the findings showed that the factors that had the strongest effects on people's experiences were:
- The GP practice that they were registered with - there was considerable variation between practices, especially when it came to accessing services. There was also considerable variation between practices in people's experiences of doctors and nurses, and in the overall care provided. 41 per cent of the variation in people's experience of the overall arrangements for getting to see a doctor is explained by the practice they are registered with.
- The size of their GP practice - people reported better experiences at smaller practices. The effect of practice size was greatest when it came to accessing services.
- Age - we found that older patients reported better experiences. The effects of age were greatest for people's experiences of doctors and nurses, and the overall care provided.
- Health status - people with better health status reported better experience. Health status had a similar effect across all areas covered by the survey.
KEY FINDINGS
2012 INPATIENT PATIENT EXPERIENCE SURVEY
There was a slight improvement in the experiences of patients nationally compared to the previous survey in 2011. Scottish inpatients were again generally positive about their hospital stay.
The area with the most improvement was people's experiences of the hospital and ward environment. This year slightly more patients indicated that the ward, bathrooms and toilets were clean; they were happy with the food and drink they received; and noise at night was less of a problem.
Despite the improvements elsewhere, the percentage of patients who were confident that they could look after themselves when they left hospital saw a further reduction by one percentage point to 85 per cent; it had dropped by two percentage points in 2011.
This year, questions about care and support services that needed to be arranged before patients could leave hospital were introduced. Of patients that required care or support services, 82 per cent rated that, overall, the services they got after leaving hospital were excellent or good.
CO-PRODUCTION
Co-production is one of three strands of the Scottish Government's Person-Centred Health and Care Programme, alongside work to improve Care Experience and Staff Experience. Co-production means delivering public services in an equal and reciprocal relationship between professionals, people using services, their families and their neighbours. Six features of co-production as defined by the New Economics Foundation (NEF) and the National Endowment for Science and the Arts (NESTA) are: recognising people as assets; building on people's existing capabilities; mutuality and reciprocity; peer support networks; blurring distinctions between professionals and recipients, and between producers and consumers of services by reconfiguring the way services are developed and delivered; and facilitating rather than delivering.
The Joint Improvement Team (JIT) leads co-production and community capacity building in health and social care on behalf of Scottish Government. Allied to this the Health and Social Care Alliance Scotland (the Alliance) is leading the People-Powered Health and Wellbeing Programme which is the co-production element of the Scottish Government's Person-Centred Health and Care Programme. The Alliance brings expertise in working collaboratively with individuals who use health and care services, their families and communities, to design services that are person-centred and empower people to become active partners in their care. The Alliance is coordinating support to the Person-Centred Health and Care Programme by third sector partners, particularly small associations and those representing marginalised groups. Funding has subsequently been agreed for £1.4 million over three years, up to December 2015.
PATIENT OPINION
Patient Opinion, a new national feedback website, was launched by the Cabinet Secretary for Health and Wellbeing in March 2013, to provide an open and independent, realtime feedback and complaints platform, through which patients, carers and their families can share their experiences of NHS care and services, no matter where they live in Scotland. Comments made on the site are passed to the relevant staff who can respond or use the feedback to help to improve services.
GETTING IT RIGHT FOR EVERY CHILD
Progress has been achieved by all NHS Boards in implementing the Getting It Right For Every Child (GIRFEC) approach to improving outcomes for all children and young people. Almost all Community Planning Partnerships (CPPs) are reporting that GIRFEC processes are implemented in critical areas of the business. This includes identifying a 'Named Person' for every child and young person in universal services and redesigning business processes to secure a single planning process for all children and young people supporting a single child's plan.
27-30 MONTH REVIEW
The guidance on the reintroduction of the 27-30 month review as a universal contact for all children was published on 19 December 2012. The purpose of the review is to pick up a range of development issues including communication and language skills, family relationships as well as being a key point of delivery for health promotion messages such as healthy eating, stimulation and play, behaviour management and physical activity. Following the publication of the guidance, NHS Boards were requested to roll out the review from April 2013.
NHS FREE EYE EXAMINATION
For the year ending 31 March 2013, high street optometrists and ophthalmic medical practitioners performed 1,926,616 free NHS eye examinations in Scotland (36.3 per cent of the population), an increase of 13,051 (0.7 per cent) on the previous year[37]. This represents a continued improvement in the number of examinations carried out since the introduction in 2006 of the free NHS eye examination in Scotland. The free NHS eye examination allows patients to receive an appropriate health assessment of their whole visual system, and provides a general health check, which can detect sight-threatening and treatable conditions that might otherwise be undetected.
REVIEW OF NHS PHARMACEUTICAL CARE IN THE COMMUNITY
Led by Dr Hamish Wilson and Professor Nick Barber, this year-long Review of NHS Pharmaceutical Care of Patients in Community in Scotland* reported its findings and recommendations to the Scottish Government. The evidence from this extensive and valuable work, together with other national health and social care policy initiatives, helped to inform the Vision and 10-year action plan published in August 2013.
The action plan provides the foundation stone for the future of NHS pharmaceutical care in Scotland. It focuses on changing the experience of pharmaceutical care for the patient and community - with greater emphasis on partnership working between the patient, their GP, their pharmacist and other practitioners to improve continuity, safety and effectiveness of care. It brings the clinical role of pharmacists to the fore and highlights their vital contribution to patients' health and wellbeing and to maximising health outcomes from medicines.
TACKLING POLYPHARMACY
In November 2012, Chief Executive Letter (CEL) 36 (2012)* was issued to NHS Boards, providing guidelines on appropriate prescribing and polypharmacy (patients on multiple medicines). Guidance was produced by a national group to help clinicians review patients, and the risk stratification tool Scottish Patients at Risk of Readmission and Admission (SPARRA) was adapted to help NHS Boards identify the most appropriate patients to review. From April 2013, this person-centred approach to safe and effective prescribing has been adopted into the GP contract arrangements, with GPs and pharmacists encouraged to deal with polypharmacy using a multi-disciplinary approach.
MODERNISING LEARNING DISABILITIES NURSING
In April 2012, Strengthening the Commitment: The Report of the UK Modernising Learning Disabilities Nursing Review* was published. This review was commissioned by the Chief Nursing Officer for Scotland on behalf of UK Chief Nursing Officers, recognising the changing needs of people and the crucial role of these specialist nurses. It aimed to ensure the best possible services for people with learning disabilities, and their families and carers, and a valued and thriving learning disabilities nursing profession which maximises its role throughout the entire health and social care system. The report was the result of significant consultation with stakeholders, including people with learning disabilities. It sets out recommendations across a wide range of areas, which the four UK countries are progressing within their own contexts. The Scottish Action Plan was published in March 2013.
DELIVERING HEALTHCARE IN REMOTE AND RURAL AREAS
In January 2013, the Cabinet Secretary for Health and Wellbeing announced that the Scottish Government would support a proposal from NHS Highland to develop and test new models of healthcare service in remote and rural areas. Instead of one single model of service, principles and key elements for success will be set. Successful solutions will be grown from local need and local resilience. The models developed by NHS Highland will be evaluated to test their effectiveness and their application to healthcare settings in urban as well as rural areas across Scotland. It is expected that work will begin early in 2013/14, with specific targeted areas of work up and running by the autumn.
NEW NATIONAL STATE OF THE ART PROSTHETICS SERVICE
The Scottish Government established a Short Life Working Group in 2012 to consider the implementation of the recommendations set out in the Murrison Report, A Better Deal for Military Amputees*, which were accepted by the First Minister. The Group recommended a nationally designated and commissioned service via the National Specialist Services Committee (NSSC), National Services Division in NHS National Services Scotland (NSS). Its recommendations were accepted by the Cabinet Secretary for Health and Wellbeing. The provision of prosthetics will be based on agreed clinical need and multi-disciplinary assessment on an individual case-by-case basis. The national service will be provided through the limb-fitting and rehabilitation centres in Edinburgh and Glasgow, with links to Aberdeen, Inverness and Dundee centres. Work is underway to establish this service by April 2014.
NHS INFORM
During 2012/13, NHS 24's national health and care information service, NHS inform[38], has hosted a series of new developments of health zones, and key campaigns such as the Scottish Government's Detect Cancer Early campaigns have been hosted on the site. NHS inform is available on the web and through digital TV, and is promoted through social media platforms and the innovative STV Health Centre partnership. New services have included: a Screening Zone which brings together all elements of screening into one place; a Veterans' Zone to support the veterans' community across Scotland; Smokeline the national smoking cessation service; an Easy Info Zone providing access to health information for people with learning disabilities; and a Bereavement Zone to help and support people experiencing bereavement difficulties. A mobile version of NHS inform was also launched to allow people to access the site's wide ranging features while on the move.
STAFF
NEW E-LEARNING AND DEVELOPMENT PROGRAMME
A new e-learning and development programme for NHSScotland staff dealing with patient feedback and complaints was launched in May 2013. Developed with NHS Education for Scotland (NES) and the Scottish Public Services Ombudsman (SPSO), the comprehensive programme of education and training is being delivered service-wide over the next two years, supporting the Can I Help You? Guidance for Handling and Learning from Feedback, Comments, Concerns or Complaints about NHS Health Care Services* best practice guidance introduced last year when the Patient Rights Act was implemented.
STAFF EXPERIENCE
Pursuit of our Quality Ambitions require us to have staff who are motivated, empowered and engaged with their job, team and organisation. Evidence tells us that there are clear links between patient experience and staff experience. That is why staff experience is a priority for NHSScotland and is a key component of the Person-Centred Health and Care Programme alongside care experience and co-production. A project was funded recently to develop and pilot a new approach to measuring and addressing staff experience at a local level. This pilot Staff Experience Project - which was led by NHS Dumfries and Galloway, NHS Tayside, NHS Forth Valley and NHS National Waiting Times Centre - produced its final report in May 2013, and consideration is already being given to how the model developed by the project might be implemented across NHSScotland.
INCLUSIVE CARE FOR ALL
In 2012/13, the NHS National Waiting Times Centre was the first NHS organisation in the UK to achieve stage two (Full Investor status) from Investors in Diversity. The Investors in Diversity (IiD) accreditation scheme is designed to help organisations achieve an inclusive organisational culture which enables every employee to succeed and feel valued, regardless of their background. In addition, the Board retained Investing in Volunteers (IiV) status - the national quality standard for organisations showing a commitment to involving volunteers in their work. The NHS National Waiting Times Centre is one of the first NHS organisations in Scotland to be accredited for a second time after assessors continued to be impressed with the way volunteering is embedded into the culture of the organisation.
The NHS National Waiting Times Centre was also the top Scottish NHS Board in Stonewall's Workplace Equality Index (WEI) for the third year in a row. The WEI is a measure of how an organisation meets the needs of Lesbian, Gay and Bisexual (LGB) staff and service users and is a good indicator for equality generally.
CARERS
CARERS STRATEGY
Progress has continued in implementing Caring Together: The Carers Strategy for Scotland 2010-2015*. The Scottish Government has invested £5 million in 2012/13 in NHS Boards, including the Scottish Ambulance Service, to take forward a wide range of initiatives to support carers and young carers to help them sustain their caring role. This includes the provision of information and advice, carer training, and short breaks. In addition, investment of over £3 million in 2012/13 has been channelled through the voluntary sector to provide flexible short breaks for carers and young carers. NHS Education for Scotland (NES) and the Scottish Social Services Council (SSSC) have also taken forward workforce training on carers and young carers. This includes a set of Core Principles designed to help the workforce to support and improve outcomes for carers effectively.
EXPANSION OF THE FAMILY NURSE PARTNERSHIP PROGRAMME
The Family Nurse Partnership Programme works closely with teenage mothers from early pregnancy until the child reaches the age of two. Five new NHS Board areas are now implementing the Programme as at July 2013, increasing capacity to support up to 1,700 clients at any one time. A significant proportion of these young women come from deprived or very deprived backgrounds, whose children are more susceptible to poor health, social and emotional outcomes. The third interim evaluation report, Evaluation of the Family Nurse Partnership Programme in NHS Lothian, Scotland: 3rd Report - Infancy*, was published in December 2012. This continues to show that there was high uptake and low attrition, with high levels of engagement throughout.
NHS Tayside Story 'optimum' Weight Management in Pregnancy[39]
Obesity in pregnancy is associated with serious risks for both mothers and babies. These risks include miscarriage, stillbirth, gestational diabetes and infection.
In Tayside there are around 4,500 births each year. When booking their first appointment with a midwife, almost one third of women are obese.
There was no care pathway in place in Tayside for obese pregnant women and midwives did not routinely discuss obesity and its risks in pregnancy. In order to address this, a specialised weight management in pregnancy clinic called 'optiMUM' was introduced in Ninewells Hospital, Dundee.
The overall aim of this service is to provide a safe, effective, woman-centred quality service for obese pregnant women in Tayside. In creating this service, a multi-professional group designed an antenatal weight management intervention and women's views were sought to determine what a weight management service should look like. In addition, key messages were developed based on known risk factors and the importance of good nutrition and physical activity.
Training was developed and delivered to increase midwives' confidence to discuss obesity in pregnancy and data is collected on information obtained at each consultation. Women are also offered a consultation with a nutritionist.
The service has received positive feedback from pregnant women and the staff who work at the clinic. NHS Tayside now has guidelines for the care of obese pregnant women and will continue to provide women with information to help them manage the risks of obesity in pregnancy.
The consultant obstetrician working with the team has now developed the 'NHS Tayside Guideline for the Management of Pregnancy in Obese Women' which ensures that women receive consistent and appropriate care.
INFRASTRUCTURE
SUPPORTING AND FACILITATING ACHIEVEMENT
The Quality Strategy recognised that there were a number of key national areas of development, which need to be coordinated, accelerated and aligned to support and facilitate NHSScotland and its partners to have the maximum impact on the three Quality Ambitions. These include:
- Measurement;
- Information Technology;
- Workforce, Education and Training;
- Improvement;
- Communication; and
- Governance.
There has been a national focus on these issues and work has continued to challenge progress, accelerate pace, and to create linkages and a shared ownership of these vital developments.
MEASUREMENT
NATIONAL INFORMATION AND INTELLIGENCE FRAMEWORK
The National Information and Intelligence Framework (NIIF) for Health and Social Care now provides the strategic context for all organisations working across health and care in Scotland to make decisions about the prioritisation of developments in information and intelligence to support the 2020 Vision and Route Map.
The Framework was signed off in January 2013 and was published on the Scottish Government and ISD Scotland websites[40].
The Framework establishes four national Action Groups, each with a different focus. These are:
- Prioritisation of national data and information collections;
- Presentation of evidence for maximum impact;
- Efficient development and maintenance of the information evidence base; and
- Maximise access to and use of intelligence and evidence.
A launch event took place in June 2013, at which the four Action Groups met to discuss the issues central to the NIIF and its implementation. The next step will be to move from the Framework to a clear delivery plan that shows the alignment and integration with the 2020 Vision and Route Map, and explicitly supports the integration of health and social care agenda. This will enable the rationalisation, focusing and integration of the available analytical capacity to ensure that the right information is provided to the right people at the right time and in the right format.
QUALITY OUTCOME INDICATORS
Work has continued on the development and improvement of the Quality Outcome Indicators (level 1 of the Quality Measurement Framework), under the oversight of the Quality Measurement Action Group (QMAG). A web portal, which provides information on progress with all the indicators, is now available[41]. This page also provides information on progress on the indicators that are still under development. The indicators and outcomes have been reviewed during the year, including the consideration of the implications of the integration of health and social care. Work has also been carried out to look at the specific integration outcome indicators for partnerships.
KEY HIGHLIGHTS OF MEASUREMENT ACTIVITY
Data Linkage Work Bringing Together Health, Social Care and Housing Data
This work will help us to better understand the complexities of care pathways and will be critical to providing the evidence base needed in the world of integrated health and social care, to enable better decision-making and best use of resources.
Patient Experience Surveys
This has been a key component of the measurement of quality outcomes across the health system and with the prospect of integration, developments are now underway to survey social care users as well as Primary Care users using a single survey.
Implementation of the CHKS Insight data benchmarking service across NHSScotland
This service has been procured on behalf of NHSScotland Chief Executives to address current gaps in their ability to effectively benchmark with peers in Scotland and across the rest of the UK. This links to the work programme for Information Services Division (ISD) which will create enhanced benchmarking products and tools over the next two-three years.
Quality Improvement National Reporting Tool (QINRT)
This new system to collect local improvement data has recently been launched by ISD to support NHS Boards' local improvement activities. This is currently set up to support the Scottish Patient Safety Programme and Leading Better Care, but has the facility to incorporate other programmes.
Hospital Scorecard
A hospital scorecard was developed and is now used by the Health and Social Care Management Board. Recent improvements in data visualisation mean that it can now be viewed as a dashboard with the facility do drill down to examine trends in the indicators.
Review of Equality Health Data Needs in Scotland
This report was published by NHS Health Scotland in September 2012, and the QMAG is overseeing implementation of its recommendations by NHS Health Scotland's Person-Centred Enquiry Programme, as well as ensuring appropriate prioritisation of the remaining recommendations by embedding this within the work of the NIIF.
KEY HIGHLIGHTS OF MEASUREMENT ACTIVITY
Development of Whole System Indicators (Wisdom 2, to be renamed Discovery)
This is a major project being taken forward by ISD, the aim of which is to bring together indicators from various sources on a dynamic system that will be organised around the dimensions of quality and the 2020 Vision priorities.
INFORMATION TECHNOLOGY
Developing and supporting the appropriate IT infrastructure to deliver safe, effective and person-centred care is a key priority for NHSScotland. The areas of progress are described here and provide an overview of activity during 2012/13.
eHEALTH STRATEGY
The Second eHealth Strategy 2011-2017* focuses on benefits and customers. It aligns IT activity with our Quality Ambitions and includes six key aims in the areas of: clinical communication; person-centred care; patient safety; support for patients in the community; improvements in efficiency; and access to key information. The six key aims are outlined here accompanied by an example of activity during 2012/13 to achieve these aims.
Improved Safety for People Taking Medicines
The Emergency Care Summary (ECS) was introduced to record information about the most recent medication and allergies of patients in Scotland. Initially used in Accident and Emergency, out-of-hours service and NHS 24, it has over 5.5 million records which are updated daily providing up-to-date information. This information is valuable in the scheduled care setting and work was undertaken to widen access to scheduled care clinicians. There are 250,000 ECS accesses monthly and this is likely to increase as use in the scheduled care setting increases[42].
Maximising Efficient Working Practices, Minimise Wasteful Variation, Bring About Savings and Value for Money
The McClelland review of Scottish Public Sector ICT infrastructure recommended greater collaborative procurement. NHSScotland has a key role in the Scottish Wide Area Network (SWAN) Programme, designed to deliver a single public services network available for the use of any, and potentially all, public service organisations within Scotland; with aggregated demand delivering both cost and performance advantages. The SWAN initiative aims to enable infrastructure and service sharing that will produce cost efficiencies and facilitate the creation of public services that are high quality, continually improving, efficient and responsive to local needs.
Person-Centred eHealth Strategy
A Person-centred eHealth Strategy and delivery plan was published in December 2012, and focuses activity in five areas: improving information and providing opportunities for patients to give feedback (through websites, social media, apps etc.); improving one-way communication from NHSScotland to the person (more/better use of email, SMS etc.); improving two-way communication to and from NHSScotland and the person (patient portals, telehealth, telecare, e-consultation); carrying out transactions (managing appointments, repeat prescriptions using patient portals); and peer support (greater use of web forums, social media and improved access to information).
Care Integration and Support for People with Long Term Conditions
In support of health and social care integration, an Information Sharing Board (ISB) has been established with membership drawn from NHS Boards and local authorities. This Board will oversee the overall direction of technology and information sharing support for health and social care integration and will support local initiatives while agreeing common standards. The Board will play a key role in developing a health and social care information technology strategy and will contribute to improved collaborative working in support of better outcomes for clients.
Clinical Portal (or Electronic Windows to Information)
The Clinical Portal has continued to be rolled out across NHSScotland. The Portal provides access to clinical systems and information in one place, and supports the provision of excellent and safe patient care. In secondary care, they are the clinicians interface with the Electronic Patient Record. By the end of 2013, Portals were in place in the majority of NHS Boards, with remaining Boards scheduled to implement solutions by March 2014. Clinicians find the information extremely helpful. As an example, NHS Tayside have 4,000 registered users and there are around 60,000 accesses each month.
ePHARMACY PROGRAMME
The ePharmacy Programme has been revolutionising the way GP prescriptions are issued, dispensed at community pharmacies and processed for payment by NHSScotland, using Electronic Transmission of Prescriptions. The Programme has made significant progress in developing and delivering the platform to support serial prescribing and dispensing. A number of community pharmacies and GP practices were in involved in the Early Adopters phase to test serial prescriptions in advance of full rollout during the course of 2013. To date, some 1,000 community pharmacies and 600 GP practices have been enabled.
In time, patients with long term conditions will be able to get serial prescriptions from their doctor covering a 24- or 48-week period. With the serial prescription the patient gets their medicine directly from the pharmacy where they are registered for the Chronic Medication Service (CMS) without having to see their doctor. Working closely with the patient's GP, the pharmacist will review with the patient, use of their medicines and whether the patient should have a CMS care plan. The care plan helps the pharmacist to give the patient more regular care and advice about their medicines. Over 200,000 items have already been dispensed through the service[43].
WORKFORCE, EDUCATION AND TRAINING
An appropriately trained and motivated workforce is essential to our aims for a modern, quality-driven and patient-centred service. Partnership working involving NHS Education for Scotland (NES), NHS Boards and education providers has, across the spectrum of NHS care, achieved significant gains for practitioners, for those in training, and tangible benefits for patients. This approach to agreeing and developing appropriate training, development and appraisal will provide the fundamental basis for NHSScotland to achieve our Quality Ambitions for safe, effective and person-centred healthcare - particularly focusing on the requirement to ensure that all staff feel supported and engaged in pursuing and achieving world-leading quality healthcare. The workforce contributions to our Quality Ambitions can be found throughout this report but a number of cross-cutting areas of progress and key achievements during 2012/13 are set out here.
EVERYONE MATTERS: 2020 WORKFORCE VISION
Achieving our 2020 Vision will mean changing how we deliver services in the future - with staff doing different things, in different ways, and developing new skills. It will mean the relentless pursuit of our Quality Ambitions for safe, effective and person-centred care, with quality improvement and people at the heart of everything we do. The 2020 Workforce Vision concerns all NHSScotland staff and has implications for how staff across health and social care work together.
Everyone Matters: 2020 Workforce Vision* was launched in June 2013 by the Cabinet Secretary following development work in 2012/13. The Vision was informed by 10,000 voices and is one of the largest qualitative exercises ever undertaken in NHSScotland involving listening to the views of our staff and our colleagues working in healthcare. An engagement exercise with staff was carried out through participation in local facilitated discussions in NHS Boards, an online discussion forum and four small focus groups. A consultation exercise followed, with a good spread of responses across individuals, NHS Boards, trade unions, professional organisations, local authorities, education bodies and the Scottish Government. Commitment was given to continuing engagement with staff and key stakeholders as the 2020 Workforce Vision implementation framework and annual plan are developed. Both are due to be published in late 2013. Further information on Everyone Matters: 2020 Workforce Vision was in chapter 1.
STRENGTHENING WORKFORCE PLANNING
In 2012/13, a pan-Scotland approach to workforce planning was adopted and developed to improve the quality and usefulness of NHSScotland workforce data. An intelligence-based approach to the identification, assessment and mitigation of risks to service delivery or sustainability was also developed. In addition, joint work between the Scottish Government Health and Social Care Directorates, NHSScotland and the College of Emergency Medicine in 2012 formed the basis of current work on unscheduled care which has seen an unprecedented focus on, and investment in, dealing with the issues faced at hospital front doors across Scotland.
IMPROVEMENT
PROCUREMENT OF A STRATEGIC QUALITY IMPROVEMENT PARTNER
A procurement exercise commenced in March 2013 for a strategic quality improvement partner for NHSScotland and the wider public sector. Following this procurement process, in July 2013, the Institute for Healthcare Improvement (IHI) was announced as the successful bidder and will be Strategic Quality Improvement Partner for 2013-16. NHSScotland has had a highly successful relationship already with IHI as its national technical partner for Patient Safety. IHI will work with the Scottish Government and NHSScotland to develop and implement our approach to quality improvement in pursuit of the 2020 Vision. It is intended that this appointment will further support the spread of quality improvement methodologies and approaches into new areas of government, and the public and third sectors.
QUALITY IMPROVEMENT HUB
NHSScotland Quality Improvement Hub (QI Hub) is a national collaboration between: Healthcare Improvement Scotland (HIS); NHS Education for Scotland (NES); Health Scotland; ISD Scotland in NHS National Services Scotland (NSS); and the Scottish Government's Quality and Efficiency Support Team (Quest). Its purpose is to support the implementation of the Quality Strategy through the provision of support, education, training and technical expertise in improvement science.
Following a period of review, the QI Hub has established a work programme that is designed to support NHS Boards to create the conditions to increase the pace and scale of improvement. Priority areas for development include: support NHS Boards to undertake an analysis of quality improvement capacity and capability; implement a strategy to increase capacity and capability in quality improvement within the workforce; develop the approach to spread and sustainability of quality improvement in NHSScotland; and develop the QI Hub website[44] to enable open, dynamic access to resources, support and expertise to embed improvement as an integral part of delivering quality and transforming care across Scotland.
Spread and sustainability of quality improvement is recognised as a challenge in health care systems across the world. Recognising that this is a wide-ranging, complex issue, the specific focus for the QI Hub over the next two years is to: help NHSScotland understand the key factors required to reliably spread sustainable change across a system; provide mechanisms to enable them to build capacity and capability in the service to improve patient outcomes; and inform the design of national programmes to enable sustainable change to be 'hardwired' into the system.
COMMUNICATION
The need for clear and consistent communication of our Vision for high quality sustainable healthcare, and the respective roles of everyone with a part to play has been identified as being key to the pursuit of our Quality Ambitions.
Revised messaging was created to take account of developments during the year, including the publication of A Route Map to the 2020 Vision for Health and Social Care. In addition, work was undertaken in conjunction with the development of the 2020 Workforce Vision to ensure integration of messaging and to test existing staff messaging through focus groups. This resulted in a revised set of staff messages and key learning for future communications activity.
Opportunities were identified throughout the year to share messages and engage with key audiences through media releases, speeches, publications, conferences and meetings. The annual NHSScotland Event in 2012 was themed 'Driving Quality Through Innovation' and continued to provide a major platform to engage with staff across NHSScotland on our Quality Ambitions and the improvements required to deliver safe, effective and person-centred care. The Event demonstrated the impact of work being undertaken across NHSScotland and served to share best practice. Opportunities to engage with a wider UK and international audience included attendance in April 2012 at the International Forum on Quality and Safety in Healthcare held in Paris.
The next stage is to consider what is now needed to support a conversation with the public about its role in ensuring quality sustainable services for the future and to support the public engagement work already happening across NHS Boards.
GOVERNANCE
NATIONAL GOVERNANCE AGREEMENT
During 2012/13, the Quality Infrastructure Delivery Group developed a national resource to support NHS Boards to emphasise the key principles that underpin effective governance. Governance for Quality Healthcare in Scotland[45] is a simple resource that clearly describes the respective roles of NHS Board executives, non-executives, staff and the Scottish Government in ensuring governance to support a health and care system that focuses on the needs of communities and on delivery of high quality care and services. It covers the four interdependent areas of clinical, financial and staff governance, and information assurance - as represented in the following diagram. The governance of caring behaviours, research and education are embedded and integrated across all four areas of governance. Good governance arrangements will ensure all staff are supported to share issues in a safe and confidential environment.
The governance agreement was subsequently launched in June 2013 by the Cabinet Secretary for Health and Wellbeing.
NHS Tayside Story Engaging Junior Doctors in Incident Reporting and Quality Improvement[46]
NHS Tayside identified the need to ensure junior doctors routinely report incidents - including systems errors - on their Incident Management System. As part of Foundation Year 2 training participation in audit is a compulsory requirement.
In order to improve this reporting, a quality improvement project was initiated which aimed at engaging junior doctors in incident reporting. One of the key recommendations from the project was to include incident reporting and identifying quality improvements in Foundation Year 1 (FY1) doctor's induction.
As part of the teaching programme these junior doctors are also encouraged to identify safety and quality improvement priorities they deal with on a regular basis. The process also requires them to present these results to senior managers of the executive team within NHS Tayside at which point the priorities for incident reporting and improvement are agreed. Training for the incident reporting system is provided to the FY1 doctors and they are expected to report an incident on the system and reflect on this incident using the Mayo Evaluation of Reflection on Improvement Tool (MERIT).
Participation in the quality improvement project in the FY1 year is optional and these junior doctors have the opportunity to attend evening meetings each month to gain training in quality improvement methods and improvement coaching with their projects.
To date, 21 of the 83 FY1 doctors are currently participating in quality improvement projects and around half of the 83 have reported an incident and completed a reflective report. The FY1 doctors work in teams of three-eight and their projects include: improving handover between wards; improving ease of access to patients' case notes; and improving the completeness of the Electronic Discharge Document (EDD).
Junior doctors have a clear role to play in the reporting of incidents and taking forward quality improvement projects. They are the leaders of the future with great potential to improve the service for patients.
Contact
Email: Andrew Wilkie