NHSScotland Chief Executive's Annual Report 2012/13
The NHSScotland Chief Executive's Annual Report 2012/13 presents an assessment of the performance of NHSScotland in 2012/13 and describes key achievements and outcomes.
Chapter 1 Delivering High Quality Healthcare for Scotland
DELIVERING HIGH QUALITY HEALTHCARE FOR SCOTLAND
Through our Healthcare Quality Strategy for Scotland*, we have set ourselves three clearly articulated and widely accepted ambitions based on what people have told us they want from their NHS: care which is safe, effective and person-centred.
* All publications referred to within this document can be found in the publications section of the appendices.
THE QUALITY AMBITIONS
Safe - There will be no avoidable injury or harm to people from healthcare they receive, and an appropriate clean and safe environment will be provided for the delivery of healthcare services at all times.
Effective - The most appropriate treatments, interventions, support and services will be provided at the right time to everyone who will benefit and wasteful or harmful variation will be eradicated.
Person-centred - Mutually beneficial partnerships between patients, their families and those delivering healthcare services which respect individual needs and values and which demonstrate compassion, continuity, clear communication and shared decision-making.
During 2012/13, the pursuit of these ambitions resulted in progress in a range of areas, which has real and positive impacts for people in Scotland.
For example:
- Strong performance in waiting times with 90.6 per cent of patients seen and treated within 18 weeks of referral at March 2013.
- National results from the Scottish Inpatient Patient Experience Survey 2012 and the Patient Experience Survey of GP and Local NHS Services 2011/12 * show 85 per cent of inpatients in our hospitals rate their care and treatment as excellent or good and 89 per cent of patients reported that the care provided by their GP practice was excellent or good.
- Hospital Standardised Mortality Ratios in Scotland's acute hospitals reduced by 11.6 per cent between October-December 2007 and January-March 2013 and surgical mortality in 2012/13 was 23 per cent less than in 2008/09 [1].
- The Maternity Care Quality Improvement Collaborative was launched on 7 March 2013. The Collaborative aims to reduce the number of stillbirths and neonatal deaths by 15 per cent and to reduce the number of severe post-partum haemorrhages by 30 per cent by 2015.
- Improving our approach to the diagnosis of dementia so we have the highest national diagnosis levels in the UK[2].
- In the quarter ending 30 June 2013, 97 per cent of children and adolescents requiring mental health services were seen within 26 weeks - the average wait is currently 7 weeks.
- A HEAT target for Detect Cancer Early was introduced from April 2012, to increase the proportion of people diagnosed and treated in the first stage of breast, colorectal and lung cancer by 25 per cent, by 2014/15. Major campaigns were launched in 2012/13 to raise awareness of the signs of breast and bowel cancer. There are already positive early signs of increased awareness and activity.
- The introduction of new national Transcatheter Aortic Valve Implantation (TAVI) service, established in September 2012, is providing a treatment option for some patients with severe aortic stenosis who are not suitable for standard surgical valve replacement. In its first six months of operation, the service saw and treated more than 20 patients and is expected to treat around 60 people in its first full year[3].
- When compared to January-March 2007, the latest statistics (covering April-June 2013) show an 82.3 per cent reduction in Clostridium difficile in patients aged 65 and over and an 85.9 per cent reduction in MRSA bacteraemias in all patients. Annual rates of Clostridium difficile are now at their lowest level since mandatory surveillance began.
LOOKING AHEAD - THE CHALLENGES
Over the years ahead, the demands for health and social care and the circumstances in which they will be delivered will be radically different. We must therefore collectively recognise and respond to the most immediate and significant challenges we face. These include Scotland's public health record and level of inequalities, our ageing population, the increasing expectations arising from new drugs, treatments and technologies, and the specific impact of inflation on the health service.
During 2012/13, A Route Map to the 2020 Vision for Health and Social Care* was developed to retain our focus on improving quality and to make measurable progress to the 2020 Vision.
OUR '2020 VISION'
Our vision is that by 2020 everyone is able to live longer, healthier lives at home, or in a homely setting.
We will have a healthcare system where we have integrated health and social care, a focus on prevention, anticipation and supported self management. When hospital treatment is required, and cannot be provided in a community setting, day case treatment will be the norm. Whatever the setting, care will be provided to the highest standards of quality and safety, with the person at the centre of all decisions. There will be a focus on ensuring that people get back into their home or community environment as soon as appropriate, with minimal risk of re-admission.
A ROUTE MAP TO OUR 2020 VISION FOR HEALTH AND SOCIAL CARE
The accelerated pursuit of the 2020 Vision through the Route Map, building and developing on our model for integrated health and social care delivery, will demonstrate that Scotland is a world-leader in high quality health and care services.
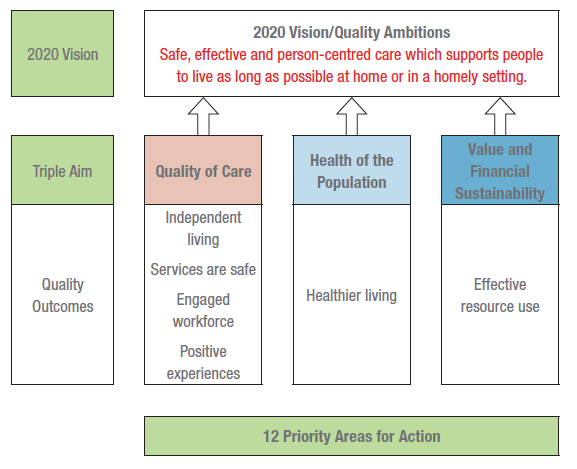
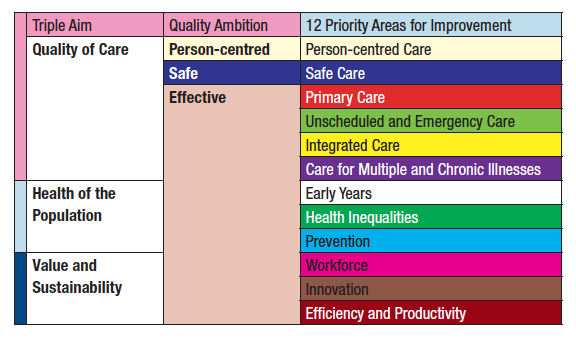
The Route Map describes 12 priority areas for action for pursuing our 2020 Vision for high quality sustainable health and social care services in Scotland in three domains: the quality of care; the health of the population; and value and financial sustainability. These domains are often referred to as the 'Triple Aim'. For each of these domains there will be a small number of priority areas for action, often building on existing work and all requiring focused attention and acceleration. In addition to these 12 priority areas for improvement action, it is vitally important to emphasise the need for a continued focus on ensuring that the underpinning foundation of high quality health and care services are maintained as 'business as usual'. These include performance (e.g. HEAT), governance, planning (services, workforce, finances and estate), IT and measurement.
The 12 Priority Areas for Action
Further improving the quality of the care we provide with a particular focus on:
1. Increasing the role of Primary Care;
2. Integrating health and social care;
3. Accelerating our programme to improve safety in all healthcare environments;
4. Improving the way we deliver unscheduled and emergency care;
5. Person-centred health and care services; and
6. Improving our approach to supporting and treating people who have multiple and chronic illnesses.
Improving the health of the population with a particular focus on:
7. Early years;
8. Reducing health inequalities; and
9. Preventative measures on alcohol, tobacco, dental health, physical activity and early detection of cancer.
Securing the value and financial sustainability of the health and care services we provide by:
10. Establishing a vision for the health and social care workforce for 2020, and setting out a clear plan of actions which have immediate effect;
11. Increasing our investment in new innovations which both increase quality of care and reduce costs, and simultaneously provide growth in the Scottish economy; and
12. Increasing efficiency and productivity through more effective use of unified approaches coupled with local solutions and decision-making where appropriate.
We continue to support the focus on performance across NHSScotland through the annual process of agreeing NHS Board Local Delivery Plans, with improved monitoring and assessment of outcomes. Ensuring that HEAT targets evolve to reflect the key priorities set out in the Route Map will make an important contribution to achieving our 2020 Vision. There is also a focus on supporting NHS Boards to strengthen their governance roles, and the commitment to work through Community Planning Partnerships (CPPs) and Integrated Health and Social Care Partnerships to ensure that Single Outcome Agreements (SOAs) properly reflect health and social care priorities, and that NHS Boards will be held to account for their effectiveness in the delivery of these priorities.
EVERYONE MATTERS: 2020 WORKFORCE VISION
Achieving our 2020 Vision will mean changing how we deliver services in the future - with staff doing different things, in different ways, and developing new skills. It will mean the relentless pursuit of our Quality Ambitions for safe, effective and person-centred care, with quality improvement and people at the heart of everything we do. The 2020 Workforce Vision concerns all NHSScotland staff and has implications for how staff across health and social care work together.
Everyone Matters: 2020 Workforce Vision* was launched in June 2013 by the Cabinet Secretary for Health and Wellbeing following development work in 2012/13. There were three specific workstreams identified in our approach to the 2020 Workforce Vision: Governance and Engagement; Leadership and Capability; and Capacity and Modernisation. Two wider workstreams support these: Values, Culture and Behaviours; and Integration.

The Vision was informed by 10,000 voices and is one of the largest qualitative exercises undertaken in NHSScotland, listening to the views of our staff and our colleagues working in healthcare. An engagement exercise with staff was carried out through participation in local facilitated discussions in NHS Boards, a website online discussion forum and four small focus groups. A consultation exercise followed, with a good spread of responses across individuals, NHS Boards, trade unions, professional organisations, local authorities, education bodies and the Scottish Government.
Subsequently we published our 2020 Workforce Vision:
'We will respond to the needs of the people we care for, adapt to new, improved ways of working, and work seamlessly with colleagues and partner organisations. We will continue to modernise the way we work and embrace technology. We will do this in a way that lives up to our core values. Together, we will create a great place to work and deliver a high quality healthcare service which is among the best in the world.'
We also published a set of common values, which will guide the work we do, the decisions we take and the way we treat each other. They are:
- Care and compassion;
- Dignity and respect;
- Openness, honesty and responsibility;
- Quality; and
- Teamwork.
Commitment was given to continuing engagement with staff and key stakeholders as the 2020 Workforce Vision implementation framework and implementation plan are developed. This is due to be published in late 2013.
Contact
Email: Andrew Wilkie