National Mission on Drugs: annual report 2021 to 2022
Sets out the progress made between January 2021 and 31 March 2022 by national government, local government and third sector partners towards reducing drug deaths and improving the lives of those impacted by drugs in Scotland.
6. Outcome 5: Quality of Life is improved for people who experience multiple disadvantages
6.1 Overview
Many people with drug problems have multiple complex needs, and therefore require support from a wide range of services to ensure these are addressed through joined up, person centred services.
The MAT Standards emphasise the importance of taking a person centred approach. This includes access to independent advocacy and support for housing, welfare and income needs. Work is ongoing across government to ensure we get it right for everyone.
Summary of MAT Standards 7 to 10
7. All people have the option of MAT shared with Primary Care.
8. All people have access to independent advocacy and support for housing, welfare and income needs.
9. All people with co-occurring drug use and mental health difficulties can receive mental health care at the point of MAT delivery.
10. All people receive trauma informed care.
The Drug Deaths Taskforce funded eight projects aimed at enhancing the evidence base around Multiple Complex Needs (MCN) and building the capacity of life-saving work in this area.
The eight projects[41] fit within the Tests of Change Framework[42] developed by the Taskforce MCN SubGroup. Funding for these projects was confirmed in March 2021 and are due to complete by March 2023.
6.2 Progress in 2021-22
6.2.1 Housing
We have continued to encourage a Housing First approach[43] for those with problem drug use and support those leaving institutions to find accommodation (such as prison and care leavers).
The Ending Homelessness Together: annual report was published in October 2021[44] and sets out the progress made against actions in the Ending Homelessness Together action plan.
The National Mission has supported this work through the Dual Housing Support Fund which provides support to individuals who want to keep their tenancies whilst in rehabilitation services. Funding has been made available to ensure that when an individual accesses rehabilitation their housing payments on their core residence do not stop for the time that they are in treatment.
Homelessness is much more than housing, and ensuring no-one ends up without a roof over their head should be a shared public responsibility. Prevention will be most effective when it is recognised as a priority across public services, which is why we are committed to introducing new homelessness prevention duties as part of a forthcoming Housing Bill.
This will include new duties on public bodies, including justice, health and social care, to 'ask and act' about housing circumstances to help prevent homelessness at an earlier stage, including for those with more complex needs which may include substance use.
6.2.2 Mental Health
The Mental Health Strategy for Scotland, 2017- 2027 includes actions to test and learn from better assessment and referral pathways, and to pilot improved arrangements for people with co-occurring substance use and mental health conditions.
In summer 2021 the government commissioned Healthcare Improvement Scotland (HIS) to take forward an ambitious programme to test new approaches to integrating substance use and mental health services in local areas. This work aimed to improve the quality of care, increase access to treatment and ultimately improve overall health outcomes for people with substance use and mental health problems.
The HIS Mental Health pathfinder programme has expanded beyond NHS Tayside and now includes NHS Grampian, NHS Greater Glasgow and Clyde, NHS Lothian and NHS Lanarkshire. The government has also commissioned a separate rapid review into substance use and mental health services which will report in late 2022.
Case Study: Mental Health and Recovery
The Lochee Hub and 5TRP project, Dundee
The 5TRP project at Lochee Hub in Dundee delivers concurrent support for people with mental health and substance use problems to help individuals advance their recovery journey.
Through this project, clients have 5 stages of support, from 1:1 therapeutic support to volunteering opportunities and training for employment. Participants choose what services they wish to support their recovery, allowing the clients to be in control of their own recovery.
Since being on the 5TRP I'm feeling a wee bitty better in myself. My goals for the future, to be off my script, a wee job and someone to give me a chance and maintain contact with the children."
This project was awarded £40,093 from Scottish Government via National Mission Improvement Fund and continuation funding of £173,351 for a further two years.
6.2.3 Justice
The Vision for Justice in Scotland[45] sets out our transformative vision of the future justice system for Scotland, spanning the full journey of criminal, civil and administrative justice, with a focus on creating safer communities and shifting societal attitudes and circumstances which perpetuate crime and harm.
Case Study: The Positive Outcomes Plus Project (POP), Glasgow
The Positive Outcomes Plus Project (POP) delivered in Glasgow by Police Scotland in partnership with SACRO.
Custody Peer Mentors (CPMs) engage with people who have substance use issues whilst in custody. All service users receive brief interventions to help reduce harms. Many also receive more ongoing support after they leave custody.
Over the life of the project (September 2020 – March 2022) 499 people in custody were engaged, 33% accepted support, compared with 3% before this project. 67% of service users felt their drug/alcohol misuse had reduced while 86% felt that their offending behaviour had declined.
This project received £128,628 from Scottish Government via Corra Foundation and will receive £290,028 continuation funding from the Service Improvement Fund, until March 2025.
The revised National Strategy for Community Justice (published June 2022) sets the national direction for community justice by building on progress made to date. It is designed to provide a clear roadmap for future improvement work, by highlighting key areas for partners to focus on. The strategy sets out four national aims for community justice, and 13 priority actions which the Scottish Government and community justice partners should seek to deliver over the duration of the strategy.
The Bail and Release from Custody (Scotland) Bill[46] was introduced to the Scottish Parliament 8 June 2022 and is currently undergoing Stage 1 scrutiny. The provisions in the Bill are intended to ensure that, as much as possible, the use of custody for remand is a last resort for the court, and greater focus is given to the rehabilitation and reintegration of individuals leaving custody.
Part I of the Bill focuses on the use of bail and remand in recognition of the negative impact that short periods of imprisonment can have. Part II of the Bill focuses on arrangements around release from prison custody, specifically, it aims to further restrict the days of the week on which individuals can be released from prison custody so that releases do not take place on Fridays or the day before a public holiday. This is intended to ensure individuals are not released from a prison sentence where access to services and support is more limited.
6.2.4 Physical Health
People who use drugs – particularly those who have used drugs for many years – often have complex physical health conditions and we need to ensure that health services take a holistic approach to care.
We are working with PHS to map the different models for providing drug treatment within primary care across Scotland and the UK. These will be published at the end of 2022 and will inform the implementation of MAT Standard 7 – All people have the option of MAT shared with Primary Care.
6.3 Measuring Progress
Limited data currently exists to measure progress towards Outcome 5 (quality of life is improved by addressing multiple disadvantages). This section presents some of the relevant context and, where possible, potential indicators for measuring progress. Here we focus mainly on aspects of this Outcome where there is currently available data – deprivation, housing and homelessness, mental health, interactions with the justice system and implementation of the MAT standards underpinning Outcome 5.
6.3.1 Measuring progress: Deprivation
In 2021, after adjusting for age, people in the 20% most deprived areas were more than 15 times as likely to have a drug misuse death as those in the 20% least deprived areas. The ratio has widened over the past two decades[47] (Figure 10).
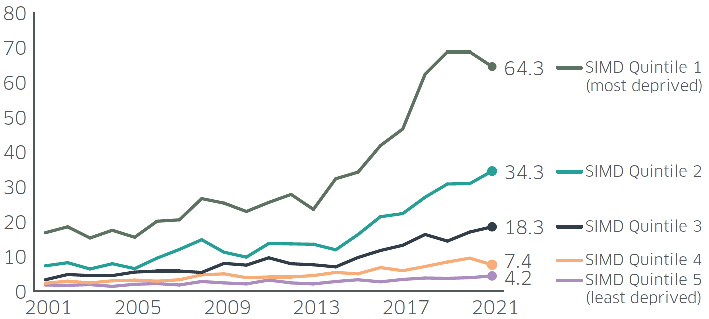
Source: National Records of Scotland, Drug-related deaths in Scotland in 2021, 2022 (National Statistics)
People from the most deprived areas of Scotland are also more likely to experience a drug-related hospital stay. In 2020/21, 50% of patients (5,175 patients, 485 patients per 100,000 population) lived in deprivation quintile 1 (most deprived). This has been consistently the case since the time series began in 1996/97, with approximately half of patients with a drug-related general acute/psychiatric stay living in the 20% most deprived areas in Scotland in each year.[48]
6.3.2 Measuring progress: housing & homelessness
The relationship between homelessness and health in Scotland was explored in research published in 2018. Of those who had experienced homelessness, there was evidence of drug and/or alcohol interactions for a fifth of people (19%). Of these, the vast majority (94%) also had evidence of mental health issues.[49]
In 2021/22, around one in ten households (11%) assessed as homeless or threatened with homelessness had support needs for drug and alcohol dependency.[50] This percentage has been broadly stable since the time series began in 2007/08. Each year since 2012/13, drug and alcohol dependency support needs were identified for between 3,109 and 3,645 households.
In 2020, over half of deaths of people experiencing homelessness were drug misuse deaths (151 deaths, 59%).[51] There has been an upward trend in the number of drug misuse deaths of people experiencing homelessness over the period for which data is available – the number of deaths in 2020 (151) was more than double that in 2017 (68). The percentage of all homeless deaths which are drug misuse deaths is also increasing (2017: 41%, 2020: 59%).
151 Deaths of people experiencing homelessness in 2020 that were drug misuse deaths
59% Percentage of deaths of people experiencing homelessness in 2020 that were drug misuse deaths
6.3.3 Measuring progress: Mental Health
Psychiatric comorbidities are common among people who use drugs – 22% of people who had a drug misuse death in 2017 had recently been in contact with mental health services. In 2017 and 2018, 63% of people who had a drug misuse death had a recent psychiatric condition recorded in the six months prior to death. The percentage of drug misuse deaths with recent psychiatric ill health has increased since 2009 (40%). Depression and anxiety were the most common psychiatric conditions recorded in the six months prior to death in both 2017 and 2018.[52]
In 2020/21, 13% of drug-related hospital stays were in psychiatric hospitals, a similar percentage to the previous year.[53] In 2020/21, the rate of drug-related stays in psychiatric hospitals was 34 stays per 100,000 population. This was a decrease from 39 stays per 100,000 population in 2019/20. After a lengthy period of stability, the rate of drug-related psychiatric stays increased from 29 to 40 stays per 100,000 population between 2014/15 and 2016/17, and remained approximately the same until 2019/20 (Figure 11). Note that measures put in place to respond to COVID-19 impacted the number of hospital stays in 2020/21.
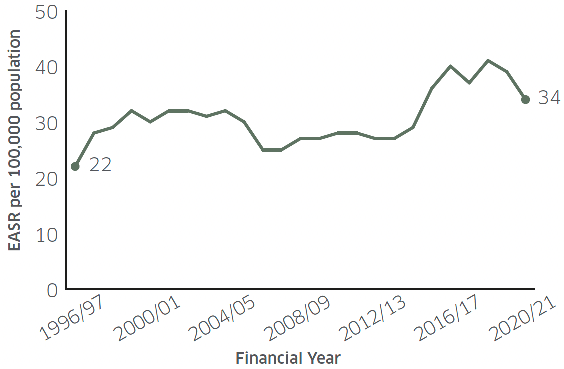
Source: Public Health Scotland. Drug-Related Hospital Statistics Scotland 2020/21, 2021 (National Statistics). EASR is European Age Standardised Rate, uses European Standard Population 2013 and National Records of Scotland 2020 mid-year population estimates.
6.3.4 Measuring progress: Interaction with the criminal justice system
Police custody
Where known, 26% (189) of people who had a drug misuse death in 2017 and 19% (187) of people who had a drug misuse death in 2018 had been in police custody in the six months prior to death. In 2017, where the length of time between police custody release and death is known, 5% of drug misuse deaths (43) occurred within four weeks of a release from police custody. The equivalent number for 2018 was 4% (47).[54]
Prison custody
Where known, slightly over half of those who had a drug misuse death in 2017 (373, 53%) had ever been in prison (2018: 471, 52%) and 14% (96) had spent time in prison in the six months prior to death (2018: 13%, 118). There was no clear trend in experience of prison custody at any time. However, there was a decrease over time in experience of a prison custody release within six months of death (2009: 20%).[55]
6.3.5 Measuring progress: Physical Health
Information on existing medical conditions of those who have a drug misuse death is recorded in the National Drug Related Death Database (NDRDD). In 2017, 70% of people who had a drug misuse death had a medical condition recorded in the six months before death, and in 2018 63% had a medical condition recorded. Reported recent medical ill health among drug misuse deaths has increased since 2009.[56]
6.3.6 Measuring progress: Implementation of MAT standards 7, 8 & 9
MAT standards 7, 8 and 9 underpin some of the work to achieve Outcome 5. Public Health Scotland's June 2022[57] benchmarking report provides examples of some of the actions and plans underway to implement these standards in the community as of April 2022.
MAT Standard 7 is focussed on primary care. Examples of work supporting the implementation of this standard included a Primary Care Facilitation Team that provides professional support to general practices signed up to the substance use national enhanced services in NHS Lothian. Moray and East Lothian have a model of care where an advanced nurse prescriber works within a primary care setting to offer opioid substitution therapy prescribing and improved pathways for holistic health care needs through general practice and the third sector – this model will be adapted for local implementation in Aberdeenshire, Midlothian, Borders and Inverclyde.
MAT Standard 8 is focussed on independent advocacy and social support. Examples of work supporting the implementation of this standard included delivery of REACH Advocacy training through workshops and courses in 16 ADP areas.
MAT Standard 9 is focussed on mental health. The Integrated Mental Health and Substance Use Pathfinder Programme is working to redesign care pathways to improve health outcomes for people with mental health and substance use support needs. Other examples of work supporting the implementation of MAT standard 9 included recruitment of an advanced nurse practitioner in Borders ADP area to offer mental health assessments through third sector services to people who not meet the criteria for the community mental health team or addictions services.