National Mission on Drugs: annual report 2021 to 2022
Sets out the progress made between January 2021 and 31 March 2022 by national government, local government and third sector partners towards reducing drug deaths and improving the lives of those impacted by drugs in Scotland.
5. Outcomes 3 & 4: People at most risk have access to treatment and recovery & people receive high quality treatment and recovery services
5.1 Overview
Treatment is a protective factor against drug-related deaths and harms and it is vital that treatment is high- quality, evidence based and promotes a recovery orientated system of care to get more people in to the treatment they need by making sure services are accessible and effective. This includes the wide range of treatment provision available – both community based and residential. All 10 MAT Standards are key elements in delivering these outcomes.
Near-Fatal Overdose (NFO) Pathways and community-based drug outreach programmes are crucial to connect people to the right services. This means that people at high risk are proactively identified and offered support, effective pathways between justice and community services, and near-fatal overdose pathways are established. See Section 4.3.4 for progress on the implementation of MAT standards 3 & 4.
Scottish Ambulance Services operates a referral system, post NFO, where patients are linked into local teams, services and third sector organisations for ongoing support into recovery.
Turning Point Scotland (TPS) operate Glasgow Overdose Response Team (GORT) which is a rapid response to NFO, providing short, focused periods of support to each person. GORT assertively connects individuals with mainstream alcohol and other drug services. The current service is split across West Dunbartonshire and East Dunbartonshire and across Renfrewshire, East Renfrewshire and Inverclyde.
Local, multi-agency, rapid response, assertive outreach pathways for people who have experienced a near-fatal overdose in Angus, Dundee City and Perth and Kinross have been established. The Dundee City NFO pathway was recognised with a national COSLA award.
Of all drug misuse deaths in 2021, 84% involved opiates or opioids[24] and evidence states that opioid substitution therapy (OST) is a protective factor against drug-related deaths and harms.[25] As a result, the initial focus is on increasing the number of people in OST treatment.
5.2 Progress in 2021-22
5.2.1 MAT Standards
The Medication Assisted Treatment Standards (MAT) were published in May 2021 and are ten evidence-based standards to enable the consistent delivery of safe, accessible, high-quality drug treatment across Scotland.[26] The standards apply to all services and organisations responsible for the delivery of care in a recovery orientated system.
Summary of MAT Standards
1. All people accessing services have the option to start MAT from the same day of presentation.
2. All people are supported to make an informed choice on what medication to use for MAT, and the appropriate dose.
3. All people at high risk of drug-related harm are proactively identified and offered support to commence or continue MAT.
4. All people are offered evidence based harm reduction at the point of MAT delivery.
5. All people will receive support to remain in treatment for as long as requested.
6. The system that provides MAT is psychologically informed (tier 1); routinely delivers evidence-based low intensity psychosocial interventions (tier 2); and supports individuals to grow social networks.
7. All people have the option of MAT shared with Primary Care.
8. All people have access to independent advocacy and support for housing, welfare and income needs.
9. All people with co-occurring drug use and mental health difficulties can receive mental health care at the point of MAT delivery.
10. All people receive trauma informed care.
A number of third sector partners contributed to progressing the MAT standards. The Scottish Recovery Consortium (SRC) provided training and provided support to ensure the voices of lived and living experience are involved in reporting on progress and the Scottish Drugs Forum (SDF) supported communications and engagement for the standards.
The implementation of MAT Standards – making support consistent, flexible, effective and faster – was supported by a programme of work to ensure the sustained scale-up of implementation. Dedicated funding of £6 million was provided directly to ADPs. To provide additional support £3 million was allocated towards the development of Near-Fatal Overdose pathways. £3 million was provided to expand the range of outreach services to help make sure treatment and support are available where people are. From 2022/23, funding exceeding £10 million will be provided directly to ADPs to support implementation of MAT standards.
The first year progress report for the MAT standards was published in June 2022. While the year one progress report showed progress has been made towards embedding the standards, we continue to set high ambitions to implement at pace. This includes a letter of direction to IA Chief Officers, along with the CEOs of Health Boards and Local Authorities asking for them for a public delivery plan for implementing the standards with either monthly or quarterly progress reporting depending on progress.
5.2.2 Buvidal
The vast majority of OST prescribing in Scotland is oral methadone,[27] which in many cases requires daily attendance at community pharmacies. This can impact on people's availability for work or caring responsibilities and is seen as reinforcing stigma attitudes to people who use drugs. In contrast, long-acting buprenorphine (LAB) requires only weekly/monthly injections, giving people time back for their lives and reducing risks and stigma.
Following the successful use of LAB in prisons[28] as a response to the COVID-19 pandemic, in 2021/22, £4 million was provided to Health Boards for the provision of long-lasting buprenorphine – to provide long-lasting buprenorphine in prisons and in the wider community and ensuring that this option of Opioid Substitution Treatment was more widely available across Scotland in line with MAT Standard 2.
5.2.3 Primary Care
We supported the development of models of care at a national level to deliver drug treatment within primary care. The models of care will aid the implementation of MAT Standard 7 – All people have the option of MAT shared with Primary Care. This will be supported by work to increase the number of GP practices that deliver integrated drug treatment services.
This year we provided £600,000 funding to Dundee to help establish a new shared care GP service at two practices in the city in response to calls for greater inclusion of substance use services in GP settings.
5.2.4 Substance Use Treatment Target
By 2024, we aim to increase the number of people who are prescribed community-based Opioid Substitution Therapy or "OST" treatment to 32,000 an increase of approximately 9% (2,500).
During 2021/22 Scottish Government worked with a wide range of stakeholders – including those with lived experience – to develop firm targets in relation to treatment and the target was announced in March 2022.
This target is based on analysis of prescribing data[29] conducted by Public Health Scotland which estimates that around 29,500 people in Scotland were in community based OST treatment during the 2020/21 financial year.
The Substance Use Treatment Target is designed to increase the number of people in protective treatment and to complement the existing work to improve the availability and quality of services through the implementation of the MAT Standards.
Developing the evidence base
In line with taking an evidence based approach to design and delivery of the MAT standards we have continued to support and add to this evidence base through direct work and through that of our partners. For example:
Scottish Government published an evidence review on current trends in benzodiazepine use[30] and research funded by the DDTF explored the utility and safety of benzodiazepine prescribing among people receiving OST in Scotland using linked data from a retrospective cohort of people representative of those who have received OST across Scotland. This study is currently still in the field and will report fully in Autumn 2022.[31]
In March 2022, Scottish Government published an evidence review summarising current knowledge of trends around methadone and buprenorphine-related deaths and changes to OST prescribing practices in Scotland.[32]
In addition, the Scottish Government published a follow-up report[33] to a previous rapid evaluation[34] of OST in Scotland's prisons. This report explored the experiences of patients living in prisons changing their OST prescription to Buvidal during the COVID-19 pandemic.
5.2.5 Residential Rehabilitation
We aim to increase the number of statutory funded placements in Residential Rehabilitation by 300% and increasing the number of beds available by 50% so that by 2026 there are at least 650 beds and 1,000 people are publically funded for their placement each year.
The National Mission includes a commitment of £100 million to be available for residential rehabilitation and associated aftercare over this parliamentary term. There are three key parts to our national approach to achieving improvements in treatment options and recovery pathways: improving pathways into and from rehabilitation services, in particular for those with multiple complex needs; investing in a significant increase in the capacity of residential rehabilitation services; and developing a standardised approach to commissioning residential rehabilitation services.
Our work is guided by the recommendations of Residential Rehabilitation Working Group which were published in December 2020. The group, chaired by Dr David McCartney, continues to provide advice and guidance throughout 2021/22.
In November 2021, we released a suite of publications on pathways Pathways into, through and out of Residential Rehabilitation in Scotland which map the current landscape of residential rehabilitation across the country and set out good practice guidance on pathways with the aim of establishing standardised recommendations and we have been working with Alcohol and Drug Partnerships (ADP) to aid the development of pathways in support of the Minister's commitment that all ADP areas will have a published pathway by the end of Summer 2022. ADPs will continue to be supported in this work by Healthcare Improvement Scotland.
An increase in the number of referrals to residential rehab has been supported by a £5 million fund for ADPs to support people into and through the residential rehab journey and £264,000 supported both the prison to rehab pathway and the innovative dual housing support fund which provides support to individuals to keep their tenancies whilst in rehab. Referral pathways are being further developed through work with Scotland Excel who have initiated engagement to explore a national commissioning approach to consider the different routes that are available to the Government for developing a national approach to commissioning residential drug and alcohol services.
As of March 2022, funding has been committed to four residential rehabilitation projects across Scotland over this parliamentary term – the expansion of River Garden Auchincruive (£6,056,654), the expansion of the Lothian and Edinburgh Abstinence Programme "LEAP" (£3,281,055) the construction of Harper House, a new National Family Service run by Phoenix Futures in Saltcoats (£8,738,424) and the construction of two dedicated Mother and Child Houses run by children's charity Aberlour in Dundee and Central Scotland (£5,701,125). Official openings for Harper House and Aberlour's first mother and child recovery unit in Dundee are currently on track for October and November 2022, respectively. The new capital investments via the RRRCP fund will create an additional 85 bed places and increase capacity by 20%.
Additional residential rehabilitation funding totalling £8 million is managed by the Corra Foundation, details of these funds are provided in the Finance section of this report.
In May 2022, we published a literature review of residential rehabilitation with a further publication of interviews conducted with individuals with Lived/Living Experience of residential rehabilitation in June.
5.3 Measuring Progress
This section presents statistics and potential indicators on progress for Outcomes 3 and 4 (people at most risk have access to treatment and recovery, and, people receive high quality treatment and recovery services). It summarises what the available data and evidence tells us about progress in the reporting period.
5.3.1 Measuring progress: Specialist treatment referrals & waiting times
The Drug and Alcohol Information System (DAISy) is a national database developed to collect drug and alcohol referral, waiting times, treatment and outcome information from staff delivering specialist drug and alcohol interventions. DAISy was available in all NHS Boards from April 2021.
There were 44,404 referrals to community-based specialist drug and alcohol treatment services between 1 January 2021 and 31 March 2022.[35]
Waiting times are a high-profile measure of how Scotland is responding to demand for services. Scottish Government has an established target that 90% of people referred for help with problematic drug or alcohol use will wait no longer than three weeks for specialist treatment that supports their recovery. This standard was consistently met at a national level over the period.
5.3.2 Measuring progress: Residential rehabilitation
Residential rehabilitation beds
In November 2021 Scottish Government published a suite of reports providing insight into the pathways into, through and out of residential rehabilitation in Scotland.[36] Providers reported 425 beds across 20 facilities in Scotland.[37]
Residential rehabilitation placements
Between 1 April 2021 and 31 March 2022, 540 placements for residential rehabilitation were approved in Scotland.[i] Of these, 463 were approved by local ADPs, 53 placements were approved by Ward 5 Woodland View in NHS Ayrshire & Arran, and 24 placements were approved on the Scottish Government funded Prison to Rehab pathway.[38]
5.3.3 Measuring progress: Implementation of MAT standards 1, 2 & 5
Public Health Scotland's June 2022[39] benchmarking report provides insight into progress towards implementation of MAT standards 1, 2 and 5 as of April 2022, which are core to achieving Outcomes 3 and 4 of the National Mission.
MAT Standard 1 is focussed on same day access to treatment. Overall, this standard was not implemented across Scotland. Of 29 ADP areas assessed, the standard was fully implemented in 1 ADP areas (3%), partially implemented in 11 ADP areas (38%) and not implemented in 17 ADP areas (59%).
MAT Standard 2 focusses on choice. Overall, this standard was partially implemented. Of 29 ADP areas assessed, the standard was fully implemented in 4 ADP areas (14%), partially implemented in 22 ADP areas (76%) and not implemented in 3 ADP areas (10%).
MAT Standard 5 is focussed on retention in treatment as long as is needed. Overall, this standard was partially implemented. Of 29 ADP areas assessed, the standard was fully implemented in 6 ADP areas (21%), partially implemented in 21 ADP areas (72%) and not implemented in 2 ADP areas (7%).
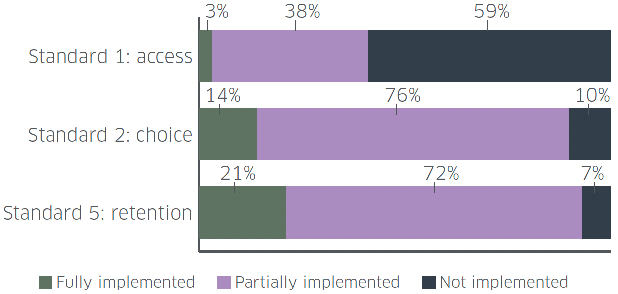
Source: Public Health Scotland, National benchmarking report on implementation of the Medication Assisted Treatment (MAT) standards 2021-22, 2022 (Management Information)
5.3.4 Measuring progress: Numbers prescribed opioid substitution therapy
In 2021/22, Opioid Substitution Therapy was prescribed to a minimum of 29,600 people in Scotland. This figure has remained fairly stable since 2016/17.[40] Numbers of people prescribed OST will be monitored regularly to measure progress towards the target outlined in Section 5.2.4 to increase this figure to 32,000 by April 2024.
29,600 People prescribed OST in Scotland in 2021/22