Mental health strategy 2017-2027: first progress report
Our first progress report on the Mental Health Strategy 2017 to 2027.
3. Public Mental Health and Suicide Prevention
This theme provides leadership and direction on public mental health by aligning mental health with the public health priorities. It will develop alliances across those priorities to deliver improved outcomes. We will use the broadest range of opportunities to improve the population’s mental health and reduce inequalities by contributing to a Scotland where:
- We live in vibrant, healthy and safe places and communities;
- We reduce the use of and harm from alcohol, tobacco and other drugs;
- We have a sustainable, inclusive economy with equality of outcomes for all, and;
- We eat well, have a healthy weight and are physically active.
This theme also contains related pieces of work, including the implementation of the Suicide Prevention Action Plan, and the piloting of Distress Brief Interventions. There is a significant and substantial role for Scotland’s Public Health organisations, with a particular focus on ensuring that service delivery is coherent and comprehensive. We want to ensure that individuals do not fall into gaps between services during transitions.
Suicide prevention
Following wide-ranging and extensive national engagement, the Suicide Prevention Action Plan Every Life Matters was launched on 9 August 2018. It sets an ambitious target of reducing suicides by 20% over 5 years. The Chair of the National Suicide Prevention Leadership Group, Ms Rose Fitzpatrick, was announced at launch and the first meeting of this group will take place on 26 September 2018, with a delivery plan for the 10 actions to be published in December 2018.
Scotland has been hugely successful in reducing suicides – from the period 2002-2007 to the period 2013-2017 the suicide rate fell by 20% (using rolling averages which smooth out annual fluctuations and give a clearer picture of the longer-term trend). This has been testament to the commitment and energy of people working in public services, as well as to the improved public awareness and reduced stigma associated with mental ill-health.
We want to fight any suggestion of complacency. The new Action Plan makes suicide prevention everyone’s business, and aims for learning from every suicide to be used in future improvement. The Actions set out include actions on creating and implementing refreshed mental health training and suicide prevention training; a coordinated approach to public awareness campaigns on suicide and its prevention; development of improved support for people experiencing crisis; and development of appropriate reviews into all deaths by suicide, to ensure that lessons from reviews are shared and acted upon. The voices of people with lived experience are central to the action plan and there is explicit consideration of its application in relation to children, young people and special ‘at risk’ populations.
The Scottish Patient Safety Programme is now in its tenth year, it has a specific work stream on mental health which is extending its improvement approach beyond general adult wards into under 18 and learning disability settings. Positive examples of change are reported in its annual reports. This approach of learning through experience puts the focus on patient’s rights and we are seeing positive examples of change which include reductions in the use of restraint and seclusion, better medicine management and safer discharge planning. The Programme has extended into piloting a new model of intensive observation practice in wards. This model emphasises the therapeutic opportunity in any necessary enhanced observation of an inpatient.
Distress Brief Intervention (Action 11)
The Distress Brief Intervention ( DBI) programme provides the offer of next day contact with a distress worker from a third sector background to anyone presenting in distress to A&E, police, ambulance services, and primary care. It has been funded by £3.4 million from Scottish Government. Since going live in 2017, four pilot sites in Aberdeen, Lanarkshire, Borders and Highlands have successfully helped more than 1000 people, by delivering packages of supportive listening and problem solving. An evaluation by Stirling University was commissioned this year, and will report in 2021. Building on the success of the DBI, the 2018 Programme for Government has committed to extending the programme to under 18s during 2019.
Substance misuse, comorbidity, alcohol minimum unit pricing (Actions 27 and 28)
The delivery of minimum unit pricing for alcohol by Scottish Government was a major international achievement which is projected to significantly save lives and reduce the burden of alcoholic liver disease.
NHS Education Scotland produced the LPASS report (Lead Psychologists in Addiction Services Scotland) which describes an evidence-based approach to therapy. Its use has being promoted through seminars to commissioners, managers, trainers and practitioners across all sectors of substance misuse services.

Waiting times for drug and alcohol treatments are included in the Quality Indicator Profile as a measure of whether mental health services are timely.
Physical health improvement in those with mental ill-health including work on activity, screening and smoking cessation (Actions 29, 30 and 31)
The premature mortality of 15-20 years in people with severe and enduring mental ill-health is a well-recognised major health inequality. The cause of premature death is cardiovascular, lung and cancer diseases. A programme to increase the physical activity of people with a physical and mental health diagnosis has been taken forward by in Fife, West Lothian and North Ayrshire, and is backed by £1m of Scottish Government funding (Action 31).
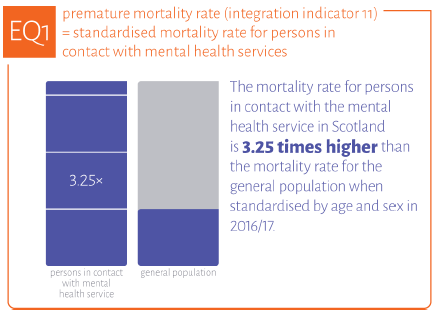
Data on premature mortality are included in the Quality Indicator Profile as a measure of whether mental health services are equitable.
In addition, there has been work on smoking cessation with IMPACT guidance rolled out to all community mental health care staff and settings in NHS Lothian (Action 29). To tackle inequality in screening services, across Scotland, for the last 2 years NHS Health Boards and third sector organisations, including those supporting people with mental health problems, were invited to bid for the Health Screening Inequalities Fund. This is a fund set up under the Cancer Strategy to help improve access to screening services. For 2018/19, three bids were received relating to supporting people with mental ill health and are currently being considered (Action 30).
Contact
Email: Lisa.Cunningham2@gov.scot