Mental health strategy 2017-2027: first progress report
Our first progress report on the Mental Health Strategy 2017 to 2027.
1. Children and Young People’s Mental Health and Wellbeing
This theme looks at children and young people’s mental health across the whole system, including health, education and children and families. It covers the whole developmental period from preconception, through perinatal and infant mental health services, into childhood, adolescence and early adulthood. It also considers the importance of adverse childhood experiences ( ACEs) throughout that developmental journey. In short, we will support the public health priority of a Scotland where we flourish in our early years.
The Scottish Government has also committed to ensuring that the principles of the United Nations Convention on the Rights of the Child are embedded into legislation in an effective and practical way. This means that our approach to delivering the Strategy’s vision recognises that children and young people have the same basic general human rights as adults and also specific rights that recognise their special needs. Children have the right to the best healthcare possible, as well as a right to a standard of living that is good enough to meet their physical and mental needs. We must also tackle the poor mental health that is a barrier to children reaching the highest level of education of which they are capable. Our whole approach must recognise the importance of listening to the opinions of children, and involving them in decision-making.
17 of the actions in the strategy sit under this theme. This recognises the fundamental importance of prevention and early intervention in children and young people.
Perinatal mental health and infants (Actions 3, 4 and 16)
In April 2017 we established the perinatal mental health Managed Clinical Network ( MCN) to support women who experience mental health problems during and after their pregnancy (Action 16). The Scottish Government provides £173,000 per year to the MCN to support their work. The MCN has now completed a mapping and gapping exercise across Scotland, and will publish its recommendations by the end of 2018. Those recommendations are likely to focus on action at a general population level, for at-risk populations, and mothers with perinatal mental illness. Furthermore, the Managed Clinical Network’s expertise and diligent work has directly informed a commitment and investment in our 2018 Programme for Government to develop a stronger network of care and support for the 1 in 5 new mothers who experience mental health problems. That equates to 11,000 women per year. This is a major achievement which will deliver tangible improvements for women and their babies across Scotland, reducing variation and improving quality of service awareness and response.
NHS Education Scotland are leading work on developing a framework of evidence-based early intervention programmes, with a delivery date of September 2020 (Action 3).
Targeted parenting programmes for parents of 3-4 year olds with conduct disorder have been expanded, with 70 new groups being delivered by December 2018 (Action 4). The Family Nurse Partnership Programme has also been extended so that it will be offered to every eligible teenage mother by the end of 2018. The 2018 Programme for Government has identified investment to build on this work and create a multidisciplinary approach to improving infant mental health across Scotland.
All of this work together will improve the mental health of new mothers and their infants. Significant early intervention at the start of a person’s life will improve their future health and wellbeing.
School age children (Actions 1, 2, 8, 17, 18, 19 and 20)
A range of actions within the Mental Health Strategy relate to supporting school age children. As well as driving forward progress on these actions, we have gone even further to ensure children and young people’s mental health and wellbeing is supported. Action 18 was to commission an audit of rejected referrals to Child and Adolescent Mental Health Services ( CAMHS). We commissioned the Audit in October 2017 and it was published in June 2018. The Audit contained a number of recommendations for Scottish Government, which we have accepted in full. We also announced the establishment of a Children and Young People’s Mental Health Taskforce, supported by £5 million of additional funding. One of the first actions of the Taskforce will be to support implementation of the recommendations from the Audit of Rejected Referrals.
The Children and Young People’s Mental Health Taskforce is chaired by Dr Dame Denise Coia. Dame Denise has dedicated her summer to talking with children and young people, their families, services, agencies and practitioners. She published her initial recommendations on 11 September, setting out a whole systems approach to mental health services, which supports and builds on the actions in the Strategy. Dame Denise has already started work on a blueprint for how services and community support can better meet the rapidly changing need that we see across Scotland. It will look, in particular, at new provision for direct access to less intensive, education and community-based sources of help for our young people. This, in turn, will deliver Actions 8 and 17.
The Programme for Government also announced a significant investment in school based mental health support, which supports Actions 1 and 2 in the Strategy. This includes investment of over £60 million in additional school counselling services, supporting 350 counsellors as well as £20 million for 250 additional school nurses. This will ensure that every high school has a counselling service. An additional 80 counsellors will also be provided in further & higher education.
We have also invested in mental health first aid, enhancing support and professional learning materials so that every council has access to mental health first aid training for teachers. Furthermore, £65 million has been committed to develop a community mental wellbeing service for 5-24 year olds, offering immediate access to counselling, self-care advice and family and peer support.
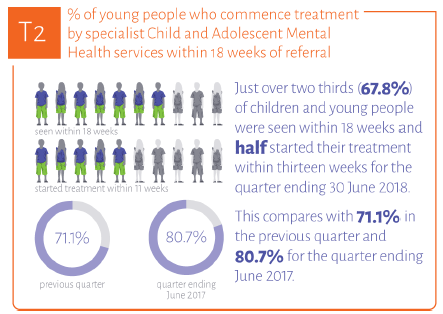
We recognise continuing public concern about access to Child and Adolescent Mental Health services. The most recent quarterly figures (Q2 Apr-Jun 2018) showed that only 67.8% of all people referred were able to access treatment within 18 weeks. This is despite increased investment, increased staffing, and the ongoing improvement support programme funded by the Scottish Government. This is, in part, because of an increased demand for services. More people are coming forward for treatment, helped by decreased stigma and rising awareness of mental health in the population. Improvement work and investment already underway as part of delivering Actions 8 and 17, combined with the new investment we have made in Programme for Government and the work of the Taskforce, will pave the way for the whole system change that is needed so that those who need specialist child and adolescent mental health services can access them in a timely manner.
Child and Adolescent Mental Health services waiting times are included in the Quality Indicator Profile as a measure of whether mental health services are timely.
The Mental Welfare Commission for Scotland reported a significant reduction in admission of under-18s to non-specialist wards, however work is ongoing through a group of lead CAMHS Clinicians to produce protocols to further improve this. The work will have concluded by the end of 2018 (Action 19).
NHS Ayrshire and Arran is the chosen site for building a National Secure CAMHS Inpatient Facility (Action 20). An options appraisal for the specialist admission needs of young people with moderate to severe learning disability or autism and mental health problems is also underway through NHS National Services Scotland. The options appraisal working group will report to Directors of Planning in December 2018.
The Scottish Government also completed a research project examining the reported worsening of mental health and wellbeing in adolescent girls. A report that was delivered to the Scottish Government in August 2018 makes recommendations for future work on internet use, associated sleep disturbance, body image, and the gathering of better data to better inform future work. We view this is a major public policy challenge.
Higher education (Action 9)
A ‘Think Positive’ launch event to improve support for student mental health is planned for this autumn (Action 9). The 2018 Programme for Government announced new investment of around £20 million to provide more than 80 additional counsellors in further and higher education over the next 4 years.
As an example of cross Government working, the Scottish Government responded to the independently chaired Student Support Review ( SSR) in June this year. In response to the SSR’s recommendations, Scottish Ministers announced that over £21 million will be invested in improving student support by the end of this Parliamentary term. The Board noted that financial worries contributed to student’s mental health issues and this was something they wanted to assist with in their work on the SSR.
As an example of other innovative work happening across the country, the Scottish Association for Mental Health ( SAMH) has been working in partnership with Glasgow Clyde College to ‘create a mentally healthy, open and vibrant college community.’ This is a two-year pilot project (which began in early 2017) and is funded by the Glasgow Clyde Education Foundation.
The project aims to train all staff on mental health and to enable them to support the college’s 27,000 students. This has involved SAMH working alongside existing Glasgow Clyde counselling services, advisory teams and engaging with the student association to build on and increase existing capacity and ensure staff have the ability to support students appropriately.
The project also aims to ‘normalise’ mental health and to encourage a culture of openness, with students and staff encouraged to be open about their mental health and confident in seeking out support if required.
Young adults (Actions 21 and 22 and 26)
Under Action 21, Transition Care Plans ( TCPs) were co-designed with young people and were launched on 29 August 2018. The TCPs have been designed by young people and clinicians, with the aim of allowing young people transitioning between CAMHS and adult mental health services to do so in a smooth and straightforward manner. Young people will be able to use them to outline their personal preferences for their own care. Crucially, they will be created, owned and updated by young people themselves. There is also a set of service documents for use by clinicians in both CAMHS and adult services. This includes a draft central transitions protocol for use by referring and receiving teams.
The Minister for Mental Health has written out to all Health Boards and Integration Joint Boards to ask them to implement use of the tool within their organisations.
Similarly, creation of a digital peer support resource to help young people with eating disorders is now being evaluated (Action 22). These are just some of the developments that show the positive benefits of closely involving young people directly in service design.
Action 26 is to deliver better service response to first presentation psychosis. We are working with NHS Healthcare Improvement Scotland to consider how this can be achieved across Scotland.
Adverse childhood experiences (Actions 5, 6 and 7)
Research shows that adverse childhood experiences ( ACEs) have a huge impact on children and young people and can have lasting effects throughout adulthood. ACEs are different types of abuse, neglect and family difficulties including parental mental ill-health. Investing in perinatal and infant mental health to support parents and infants, is therefore crucial in reducing and mitigating the impact of ACEs, Furthermore, better training of the children and families workforce around awareness and risk underpins Action 6 to support children and young people with complex needs that present a risk to themselves or others.
Evaluations of trauma, bereavement and loss services in schools and Polmont Young Offenders Institution will be published by end November 2018 in response to Action 7 to support the mental health needs of young offenders. Building on this work, the Children and Young People’s Taskforce is considering “at-risk” populations as a specific strand of service need in its framework of delivery and change. This will ensure that care pathways include mental and emotional health and wellbeing, for young people on the edges of, and in, secure care Action 5.
Contact
Email: Lisa.Cunningham2@gov.scot