Mental health strategy 2017-2027: first progress report
Our first progress report on the Mental Health Strategy 2017 to 2027.
2. Adult Mental Health and Whole System Change
A human rights-based approach to health involves making sure that services are planned and delivered in proportion to need. Services also need to be available, accessible, appropriate, and of equal quality. This theme is therefore about the need to prioritise mental health through local and national leadership. This work is critical to ensure that resources (both in terms of finances and workforce – including improving access to mental health workers in key settings) are matched to mental health priorities. This requires partnership working across sectors, as well as service redesign, and an evidence base and monitoring system that supports, challenges and informs the commissioning and delivery environment.
Integration
Improving mental health in Scotland fundamentally depends on services working together effectively in partnership. The creation of Integration Authorities provides the opportunity for delivering the necessary transformation. The Scottish Government has been discussing how to optimise these arrangements with Local Authorities, Health Boards and with the Chief Officers of their Integration Authorities. The Chief Officers National group has created specific subgroups including one on mental health.
To deliver the Strategy’s vision and ambition there needs to be better accountability with evidence of delivery of agreed outcomes. Financial investment in mental health services needs to be protected and spent appropriately. To do this commissioning guidance will be strengthened with enhanced collaborative learning between Integration Authorities and Health Boards around mental health redesign and delivery.
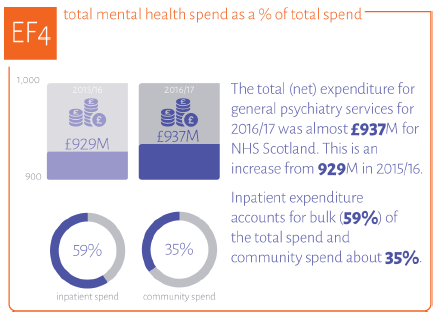
Proportion of mental health is included in the Quality Indicator Profile as a measure of whether mental health services are efficient.
Primary care transformation (Action 23)
As part of the whole transformation of primary care, £15 million of innovation funding has been offered to Health Boards to test improved models of service provision. Different local arrangements have mirrored local needs. Through this work, four important areas emerged:
- Awareness and information availability to the general public to improve self-management and improve access to the right level of service at the right time appropriate to need;
- Enhancing training in mental health for all members of primary care teams appropriate to their roles;
- Mental health professionals embedded in primary care teams to provide direct assessment and treatment, and;
- Non-clinical staff link workers delivering support whether the problems were mental or physical or both.
Some excellent examples of local innovation have been developed. For example, North and South Lanarkshire Health and Social Care Partnerships have developed a mental health liaison nurse service within 5 GP practices. Their role was facilitate an improved understanding of mental health services for primary care practitioners. The liaison nurse role is to establish a robust communication and pre-referral pathway with primary care colleagues. It offers advice, triage, signposting and supported self-help for individuals who are experiencing mild mental health difficulties of a short term nature. This model supports patients to develop the skills and capacity for self-management of their mental health and wellbeing and increased access and uptake of social prescribing opportunities. Evaluation results show improvements for patient access and experience.
In Argyll and Clyde, the introduction of a community-based Cognitive Behavioural Therapy ( CBT) programme for individuals with mild to moderate depression and anxiety has yielded a number of benefits. This uses the ‘Beating the Blues’ programme, made up of eight online sessions of approximately 50 minutes. It is confidential and available online 24 hours a day. Patients can be referred directly from NHS 24 to a GP or Community Mental Health Practitioner who can then refer the patient to the programme. In an evaluation carried out by the Department of Nursing, University of the Highlands and Islands for the Scottish School of Primary Care, online CBT was seen to be advantageous for patients in rural areas who wished to keep their mental health problems private. In addition, local evaluation data showed that people who had used the online CBT course rated their anxiety, depression and stress lower at the end of the course.
The Scottish School of Primary care are evaluating models and will publish their report in September 2018. A review of primary care improvement plans will be completed by December 2018 and these will inform future developments. As well as Action 23 in the Strategy, this was a Programme for Government commitment in 2017-18.
Psychological therapy access (Actions 24 and 25)
Despite investment, increased staffing and ongoing improvement support programme funded by the Scottish Government, 76.3% of patients started treatment within 18 weeks of referral in the last quarter against a standard of 90%.
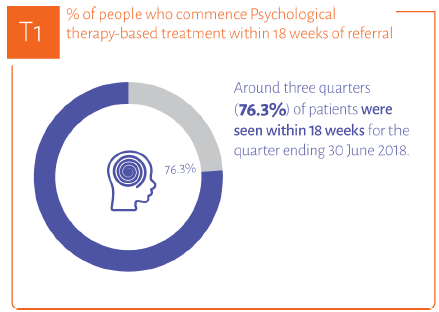
Waiting times for Psychological therapy-based treatment are included in the Quality Indicator profile as a measure of whether mental health services are timely.
The increasing demand for mental health services means that despite the increase in staffing, more people are waiting to be seen. In this context, specialist services alone can’t meet the increasing demand and community provision needs to grow. We are working with partners to help improve this community-based provision for consistent care across the country.
In addition to the work required of NHS Boards through the Government’s commitment to shifting the balance of care, there have been significant resources provided to Boards and partnerships to deliver improvements in services, with a clear expectation that this includes mental health services. An important strand being £54.1 million of funding over 4 years (from 2016-17) to allow and enable Boards to apply improvement within the context of local priorities.
Through work on capacity building there has been an increase in psychology services posts of 191 WTE posts. A programme of training has seen an additional 185 training places for CAMHS and PT workforce and wider service staff, increases in psychology and psychotherapy training posts, an increase in early intervention capacity, an increase in PT workforce capacity for primary care. There has been direct working with Boards by the Mental Health Access Improvement Support Team. This work has adopted improvement methodology to enable sharing and learning within and between teams.
During February and March 2018, the former Minister for Mental Health met with the Chairs and Chief Executives of the poorest performing boards with discussion focused on CAMHS and PT performance, prioritising mental health spending and whole system issues that need to be addressed to sustainably meet the waiting times standard. This was followed up in June by teleconferences between the Director of Population Health and Chief Executives/ senior teams.
The 2018 Programme for Government set out plans to better utilise technology, and even before that, there has been a steady increase in the use of computerised cognitive behavioural therapy ( cCBT). Since April 2018, cCBT has been operating across all health board areas in Scotland. This is an innovative way to improving psychological therapy access especially in rural communities.
Unscheduled care (Actions 13, 14 and 15)
NHS 24 has been leading on developing different supports for people with emergency mental health needs. These include:
- Extending the confidential Breathing Space service;
- Improving access to cCBT and therapy in rural areas, and;
- Strengthening the handling of mental health calls with increased direct mental health professional availability.
They have been funded by £500,000 announced in 2017, and further investment via the 2017 Programme for Government.
Examples of local innovation include the community triage model in NHS Greater Glasgow and Clyde. The National Suicide Prevention Leadership Group will review good practice in this area, including the community triage model of support, with a view to ensuring that support pathways are in place across Scotland by the end of 2019.
The 2017 Programme for Government committed to a £35 million investment over 5 years to provide access to 800 additional mental health professionals in all Accident and Emergency departments, all GP practices, and every police custody suite and to our prisons (Action 15). Over the summer, Integrated Joint Boards submitted their plans to the Scottish Government which reflect their current provision and demands for mental health services. These plans also outlined their proposals for using the additional resources under this commitment to supplement and deliver new and innovative approaches within their local areas. Following this work, Integrated Joint Boards are now in the process of recruiting additional mental health workers for the key settings outlined within this commitment.
Better mental health in the justice system (Action 10)
A governance group has been established to develop an enhanced mental health pathway as part of the Justice strategy. Recruitment and training of mental health staff is to take place in October 2018.
Access to services by people with protected characteristics and other groups, such as those living in rural areas (Action 12)
The Scottish Government has supported the further development of the National Rural Mental Health Forum with an £100,000 investment. Membership has grown to over 50 organisations. NHS 24 are exploring how technology can be used most effectively to allow isolated people to access support and treatment. The National Suicide Prevention Leadership Group will be considering how interventions can explicitly relate to people in ‘at risk’ populations.
Better use of data (Action 38)
A Quality Indicator profile that mental health services can use as part of their improvement work has been finalised following extensive consultation and feasibility testing. Launched in September 2018, initial reports will be published by NHS National Services Information Services Division from January 2019. This profile will, for the first time, balance measures of activity with outcome –in terms of both clinical and personal outcomes for patients.
To illustrate progress in delivering the ambition of the Mental Health Strategy, a data Framework has been created, consulted on, and feasibility tested. This framework pulls together data from existing sources and together will illustrate four themes:
1. Childhood determinants of a mentally healthy life
2. The impact of mental ill health
3. Population Mental Health and Wellbeing
4. Parity of mental and physical health
Data from both sources is used to illustrate this and future Annual Reports to Parliament.
Inpatient beds
Annual information on psychiatric inpatient beds and their use comes from a national census and from the Information Services Division of NHS National Services Scotland. It is good to see the continued decline in admissions and discharges for inpatient mental health patients. Treating more people at home, or in a home-like setting, is a key part of the Scottish Government’s vision for health because it helps with treatment, recovery and general wellbeing of patients.
The recent reduction in the numbers people discharged is as a result of investment in mental health and the development of these models in local community services which enable people to receive treatment at home.
The impacts of inequality are stark in these statistics: that’s one of the reasons why the Scottish Government is working with partners to deliver the Fairer Scotland Action Plan to help tackle poverty, reduce inequality and build a fairer and more inclusive Scotland.
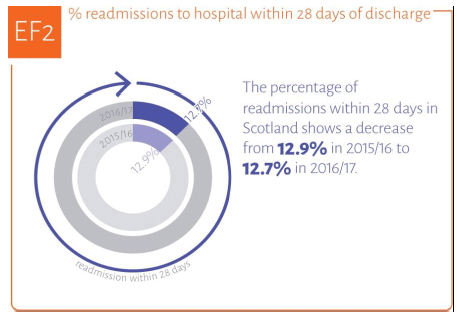
Information on psychiatric beds are included in the Quality Indicator Profile as a measure of whether mental health services are efficient.
Contact
Email: Lisa.Cunningham2@gov.scot