Infant mental health: evidence review
This report covers the key findings of a rapid literature review of UK research on infant mental health, in addition to interviews with members of infant mental health clinical teams in NHS Fife and NHS Lanarkshire.
Measures in use in Scotland
Within the papers retrieved for this report, only two reported the current use of measures in Scotland and across the UK:
The Ages and Stages Questionnaires (ASQ) is a measure of children's emotional and behavioural development. This measure has been developed for children from 1 month to 6 years, with nine age-appropriate versions (2, 6, 12, 18, 24, 30, 36, 48, and 60 months). The ASQ is designed to be filled out by parents and measures difficulties and strengths across ages and developmental domains (Squires et al., 2015). Szaniecki & Barnes (2016) report that the ASQ is routinely used by health visitors and family nurses in the Family Nurse Partnership programme across Scotland and the UK[1].
The New Orleans Intervention Model (NIM) is a method of assessment and concurrent intervention that has been developed for child aged 6 months to 6 years in foster care. The model is a relational assessment, and uses structured interviews, observations, and questionnaires to explore the relationships between a child and their caregivers. The results of these assessments are used to inform placement decisions and intervention needs (Minnis et al., 2010). Baginsky et al. (2017) report that NIM has been offered as part of the NSPCC's service delivery in Glasgow since 2011, under the name Glasgow Infant and Family Team (GIFT), and the services are being assessed as part of the BeST? Trial[2]. NIM is also being trialled in areas of London through the London Infant and Family Team (LIFT).
NHS Board engagement to understand current development of IMH measures
To find out more about the development of infant mental health services in Scotland, brief interviews were conducted with clinical practitioners from NHS Fife and NHS Lanarkshire (for interview topic guide see Annex C). There are 14 NHS boards currently in operation across Scotland, however due to the approach of the PNIMH board to provide funding in waves, many of the boards are still considered to be in the planning phase of service development. Both NHS Fife and NHS Lanarkshire boards were recipients of the "Wave 1" funding, and as such are considered to be developing and delivering services at this time. It is for this reason that these two boards were chosen for engagement and brief interviews.
Thematic analysis of the interviews was used to understand what was deemed most important to practitioners when deciding which measures to use for infant mental health needs. The thematic analysis identified three broad themes:
a) "Keeping the baby in mind" - the overarching aim of all measures
b) Challenges to service delivery, and
c) Ensuring successful delivery through increased awareness and understanding of IMH.
"Keeping the Baby in Mind": the overarching aim of all measures
"Keeping the baby in mind" was a concept that surfaced multiple times throughout both interviews. This phrase was alluded to in conversations regarding the importance of ensuring that the infant is always being considered when working with at-risk families, when the immediate needs of older members of the family may be more apparent.
"It's about counteracting the invisibility of infants when connecting with at risk families. Older children may be referred to CAMHS but infants are often left behind … It's about being an ally for infants to promote their needs early on"
– NHS Lanarkshire
When considering what measures to use to ensure an infant centred response, there were clear issues concerning a lack of appropriate or validated method of measurement. Team members from both boards discussed the need for the development of infant mental health measures that could be used effectively.
"Historically there is a problem that there are very few measures available"
– NHS Fife
"Many measures are useful in some domains but there is nothing available to encompass all areas"
– NHS Lanarkshire
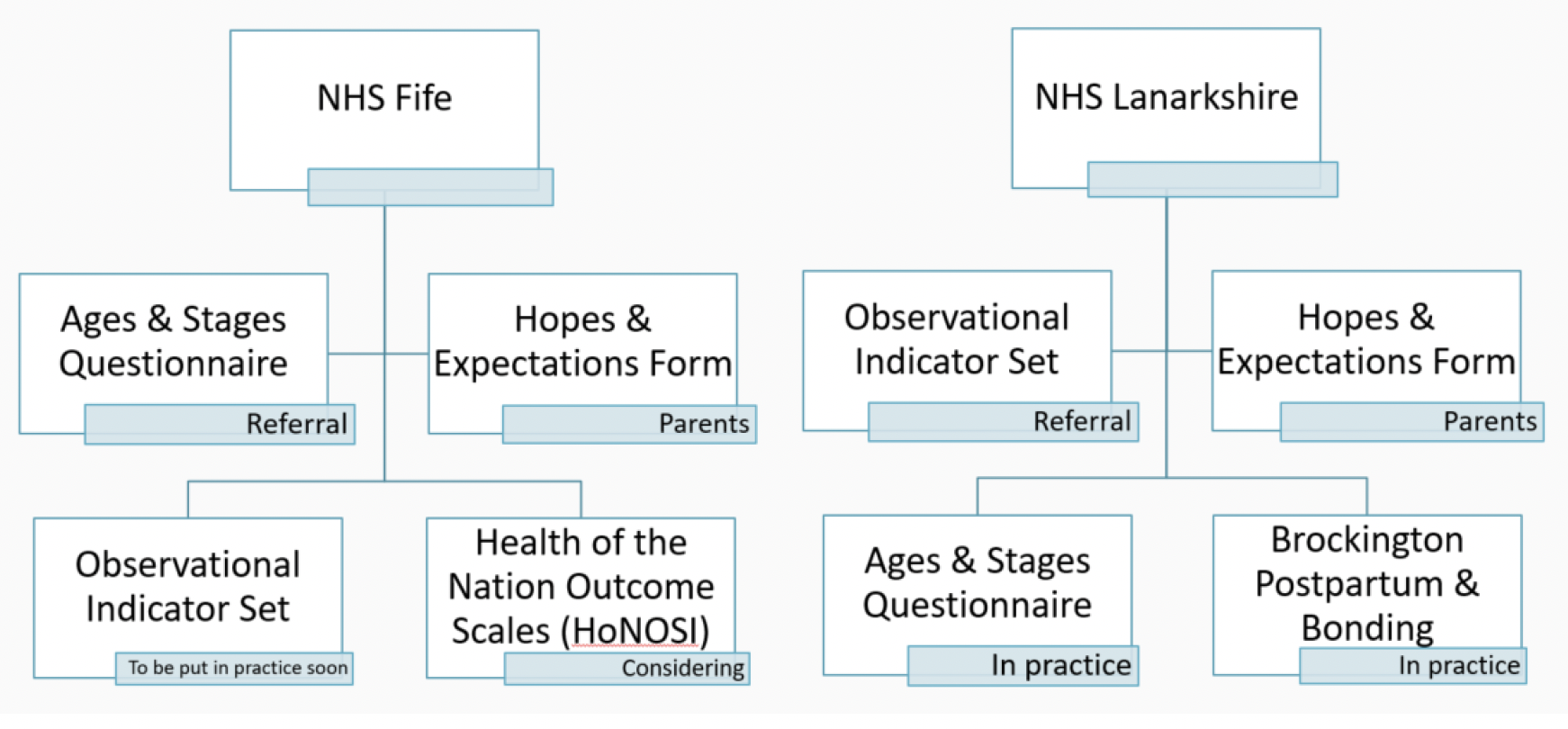
As the boards develop the rollout of their infant mental health services they have chosen to use different measures as their primary tool for referral criteria.
Due to a lack of measures deemed appropriate across all domains, the team at NHS Lanarkshire have developed the Observational Indicator Set (NHS, 2021). They believe that these tools are infant centred, and purposefully designed to promote observation across all areas of functioning in order to indicate the degree of concern. In practice alongside the Observational Indicator Set are the Observational Scales designed for use with infants aged 0-12 months, 13-24 months, and 25-36 months. When using these scales, NHS Lanarkshire clinicians will work in pairs to ensure that there is a level of inter-rater agreement on the outcome scores. The scales are designed to collect similar observations to the Observational Indicator Set. Secondary measures have also been identified for use to ensure high levels of sensitivity, for example, Health Visitors have been encouraged to use the Observational Indicator Set alongside the ASQ, which are already in use, and clinicians will also use the Brockington Postpartum and Bonding Instrument as part of their baseline assessments.
NHS Fife are currently using the ASQ as the primary measure for referral criteria. One of the reasons they have chosen this measure is that Health Visitors are already well versed in its use. The team at NHS Fife believe that the ASQ is useful as both a measureable indicator of who needs to be seen, as well as a tool that enables practitioners to notice improvements moving forward. The intention is to develop a cycle of intervention that delivers assessment, therapy, and review with punctuation points to ensure progress. The team at NHS Fife are currently considering secondary measures that they will employ to ensure levels of sensitivity, for example they are likely to put the NHS Lanarkshire Observational Indicator Set into practice. They are also interested in learning more about the Health of the Nation Outcome Scales for children and adolescents (HoNOSCA) which are currently being developed for use with infants (HoNOSI) in Australia (Brann et al., 2021).
Both NHS boards are also using the Hopes and Expectations Form in an attempt to understand the needs of parents and families. The Hope and Expectations Form is a qualitative measure which encourages parents to record three areas that they would like to see addressed for their child. This enables families and clinicians to create shared goals. Both teams were eager to employ a qualitative measure which they saw as a more holistic approach to working with families, giving parents and carers the opportunity to take part in the intervention process. This opinion is similar to that seen in the literature regarding the concept of using accessible language to ensure that parents and carers have 'bought in' to the services on offer.
"Do [parents] have the capacity to reflect on their own relationship with their infant, especially at the start of the intervention … filling out questionnaires might not be appropriate for parents"
– NHS Lanarkshire
"This is delicate work and [we] need to be sensitive when working with parents … attending to what parents think they need, rather than being told what they need for their baby"
– NHS Fife
Challenges to Service Delivery
In developing a new service, there are likely to be a number of challenges. One such challenge concerns engagement with families who would benefit from the service, which was described as "getting parents through the door". While NHS Lanarkshire did emphasise that their IMH services are provided within family households and so they were still able to visit households who had been referred, the team at NHS Fife voice concerns about parents accessing resources that would allow them to make initial contact with the services that they needed.
"Parents' isolation has meant engagement has been more difficult, particularly with the pandemic. … The usual structures and ways of getting help are not always being provided"
– NHS Fife
There is also a need to be aware of the age groups to whom the service provision will be delivering. As within the literature, there are clear challenges to defining the age range that should be included within infant mental health. For example, NHS Fife are currently working with children aged 0-4 years but are aiming to move to 0-3 years at a later date. Additionally, with the overlaps between infant mental health, early childhood mental health, and CAMHS, it is important to ensure that children do not get overlooked as they move between different services.
Possibly one of the most significant challenges to the development of infant mental health services across both boards is attributed to the impact of Covid-19 on service delivery. Both teams were conscious of the way that pandemic restrictions had affected the way they communicated and worked together. Setting up teams during the pandemic meant that staff members were working out of virtual workspaces which had challenged staff collaboration and staff training opportunities.
"We are a virtual team due to the pandemic – there is no physical base set up yet … The team members are isolated and haven't really been able to meet up in person"
– NHS Fife
"Online training and briefing sessions make it harder to connect with Health Visitors"
- NHS Lanarkshire
The pandemic has caused challenges for all frontline workers and teams from both boards talked about the concern for staff who might be feeling overwhelm or burn-out.
"We are aware of how overwhelmed health visitors currently are. The training is adding to the workload now but [we] expect that this will settle as health visitors get used to using the new tools"
– NHS Lanarkshire
Ensuring successful delivery through increased awareness and understanding of IMH
Training
When asked about short term goals for successful delivery, both teams discussed the need for an increased awareness of IMH. It was suggested that greater education of what IMH is, how to recognise IMH issues, and what can be done to promote IMH would be the most effective way of ensuring successful service development and maintenance. One way to do this is to provide meaningful training opportunities to staff teams. For example, NHS Lanarkshire were enthusiastic about the training that they are offering to upskill health visitors, family nurses, social workers, early years practitioners, as well as members of third sector organisations. Further, NHS Fife particularly reinforced the need to ensure accessibility of these training opportunities was examined.
"The larger perinatal events tend to be very psychologically driven - dialogue is usually based in psychology. [We need] more events giving voice to multidisciplinary team members … Being able to talk about the different ways that services are developing"
– NHS Fife
Championing multidisciplinary teams
Following on from the training of staff, there were discussions about the ways in which championing multidisciplinary teams would ensure the success of service delivery. It was clear from discussions with both teams that the workload is seen as a shared responsibility, not just for clinicians and psychologists, but for all adults who come into contact with the family and the infant. This could include health visitors, General Practitioners, early years practitioners, family nurses and more.
"[There is a] need for multidisciplinary work to ensure systemic success. It is a core part of work for therapeutic services … multidisciplinary teams need to be securely funded to ensure they are big enough and stable enough to work"
- NHS Fife
Communication across NHS Health Boards
In connection to a number of the challenges above and the considerations for successful set up of services throughout Scotland, discussion arose concerning the nature of communication across NHS boards and national third sector organisations. Both teams talked about the usefulness of joined up thinking across the country, and were enthused by recent events held by large third sector organisations such as AIMH (Scotland Hub) and the Parent-Infant Foundation which had allowed for the sharing of ideas and resources. There was also an indication that other NHS boards who are still in the planning phase of development are looking to the Wave 1 funded boards for a guide on how to move forward.
"We are all still in the early stage of figuring out how the mental health services will be rolled out. There has been some interest from other boards in the Indicator Set"
- NHS Lanarkshire
Contact
Email: PIMH@gov.scot