Coronavirus (COVID-19) Family Nurse Partnership insights: evaluation report
Report commissioned to explore the experiences of the family nurses and clients in Scotland during the COVID-19 pandemic. This includes initial findings on service delivery, mode of delivery, dosage, materials and resources.
4. Results
4.1 Participants
In total, 31 family nurses from the 11 Health Boards areas participated in one-to-one interviews (n=23) and focus groups (n=8). Fifteen clients from 6 Health Boards participated in one-to-one interviews. Six clients were enrolled onto the programme prior to the pandemic, nine clients were enrolled following the introduction of COVID-19 restrictions. The staff survey was completed by 90 respondents providing an eligible response rate of 41%.
4.2 Response to COVID-19 Outbreak and Restrictions
Many family nurses commented that in the initial six weeks following the UK-based outbreak of COVID-19 and the onset of national lockdown restrictions brought the most uncertainty in terms of delivering the FNP service. Family nurses noted that the closure of offices and workplaces in March 2020 resulted in a sudden shift to home working for FNP nurses and that changes were implemented quickly across the service. Rapid adaptation was required to deliver FNP in line with newly introduced public health measures and restrictions while using locally available technologies and resources.
"So I very quickly had to get my laptop, collect a pile of paperwork and head home, as we were advised to do, and it took me quite a bit of time to work out how to do remote working and get all that set up, and I just found it incredibly stressful, it was like learning a whole new job." – [Family Nurse, East]
"It felt like overnight it was, like, that's it. You know, no home visit. We need to be really careful. It's lockdown." – [Family Nurse, North]
Throughout the pandemic, NHS Board's implemented restrictions affecting FNP service delivery based on clinical guidelines issued by the Scottish Government. Initially, under national-level lockdown restrictions, home visits were advised to be conducted only for essential visits and for extremely vulnerable clients and families, such as those with child protection or social work involvement and mental health challenges. Before undertaking home visits, family nurses recalled increased levels of decision making, largely based on their own clinical judgements as well as COVID-19 risk assessments in accordance with newly introduced clinical guidelines. As the first national lockdown lifted[1], a tiered system was introduced which allowed some Health Board areas to ease restrictions on activities such as home visiting. During periods of relaxed and regional level restrictions a number of family nurses were able to offer home visits to larger proportions of their caseload.
"I suppose for us, the biggest change in terms of COVID was thinking about the, sort of, variance of the tiers and following the Scottish government guidance in terms of the amount of face-to-face visits. We were certainly much more mindful of the risk for clients, for their babies, for staff." – [Family Nurse, West]
Family nurses described that the frequent fluctuation of guidelines impacted their ability to deliver the FNP service as intended and required significant amounts of adaptation and innovation to deliver the service to a high standard.
Family nurses described having realistic expectations about the quality and delivery of the programme during COVID-19. Family nurses felt that the service was still able to be delivered, however many family nurses emphasised the efforts they and colleagues had made in order to continue service delivery, including often going the 'extra mile'. Across all Health Boards, family nurses recounted the efforts of their teams and colleagues in adapting quickly and efficiently from the outset of the pandemic so that clients across Scotland continued to receive a high-level of uninterrupted support from the FNP programme.
"I'm incredibly proud of the family nurses and the work that they do. They've been so adaptable, so flexible, so resilient and so strong, which has been really quite incredible to watch, because they're working in the middle of a pandemic when it's frightening. And it's frightening for all of us. But they wanted the clients to still have a really good service." – [Family Nurse, West].
4.3 Modes of Service Delivery
During COVID-19, modes of FNP service delivery varied from home visiting to phone calls, SMS 'text' messaging, emails, video calls and other encounters such as face-to-face outdoor walks with clients. While various communication formats were suited to different forms of contact or programme delivery more than others, a key finding was that having a range of communication options was highly beneficial for family nurses.
Staff reported mixed frequencies of usage for various service delivery modes. This highlights that various tool combinations were adopted by family nurses and used in conjunction with one another to deliver the programme. Text messaging, telephone calls and video calls were among the most frequently used telehealth modes. See Table 2.
| Mode of Service Delivery | Always | Most of the time | About half the time | Sometimes | Never |
|---|---|---|---|---|---|
| Telephone calls | 5% | 23% | 33% | 38% | 1% |
| 3% | 8% | 3% | 31% | 56% | |
| Mobile apps | 0% | 0% | 3% | 18% | 79% |
| Attend Anywhere | 1% | 12% | 22% | 24% | 40% |
| Near Me | 1% | 18% | 24% | 36% | 21% |
| Video Call (other) | 0% | 9% | 8% | 18% | 65% |
| Text messaging | 21% | 23% | 11% | 27% | 17% |
| Home visits | 1% | 19% | 34% | 45% | 1% |
Additional findings in relation to key modes of service delivery are presented in the sections below.
4.3.1 Home Visiting
Family nurses felt that the ability to continue to offer home visits during the pandemic was crucially important and allowed them to provide timely and essential support to many vulnerable and at-risk clients during this time. In addition to routine clinical judgements, family nurses had to balance multiple risk factors to determine whether visiting a family in the home was a priority.
Clients and family nurses widely perceived home visiting as their preferred format of programme delivery and the 'gold standard' for FNP. Home visiting was deemed to be crucial for developing strong therapeutic relationships, successfully conducting assessments, observations and core programme activities (e.g. PIPE and DANCE).
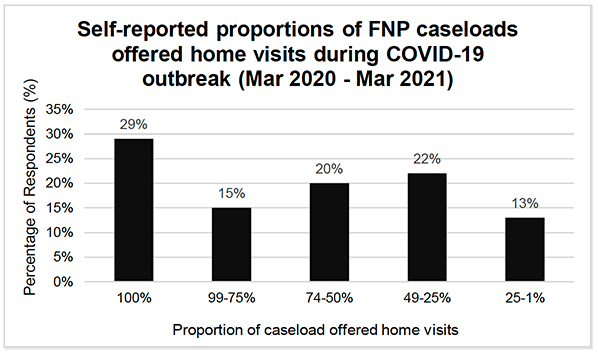
All surveyed staff (100%) reported delivering home visits during the COVID-19 outbreak. When a home visit was offered to clients, 41% of family nurses reported offers of home visits were always taken up while 51% said these were taken up most of the time. The proportion of caseloads who were offered home visits from March 2020 to March 2021 varied between family nurses, see Figure 4. Twenty-nine percent of family nurses offered home visits to 100% of their caseloads; 15% of family nurses offered home visits to 75-99% of their caseload; 20% of family nurses offered visits to 50-74% of their caseload; and 22% of family nurses offered home visits to 25-49% of their caseload.
Family nurses reported that home visits were conducted in accordance with Scottish Government Clinical Guidelines under the direction of their local teams and Health Board's. Essential visits were permissible at all times and typically depended on the level of local restrictions and stage of programme for a client (i.e., pregnancy, infancy, toddlerhood), as well as the outcome of the individual risk assessment.
Restrictions placed on home visiting meant that family nurses had to undertake new responsibilities involving an increased focus on safety and risks relating to COVID-19 transmission, as well as an increased use of clinical judgement to offer essential visits to clients in accordance with guidelines. Family nurses expressed this was a challenging aspect of their role but felt that their local teams were supportive, and that supervisors often helped them to consider or reflect on decision making concerning home visits.
Essential visits were typically conducted for assessments, newborn visits, pregnancy phases 'P1' visits and child protection reasons. Family nurses also reported visiting clients suffering from mental health issues and domestic violence. Some family nurses also mentioned visiting the homes of non-English speaking clients, due to challenges around digital engagement and connecting with interpreters remotely.
"So in COVID we've obviously had to be directed by Scottish government to which visits we can do face to face, in their communication with us which visits we could do face to face and which visits have to be done on a digital pathway. However, in all of this we have had...we're qualified nurses so we have had freedom to be able to assess ourselves whether a face-to-face visit is required. And predominantly I would say that would be for domestic abuse or for child protection. […] We've had to work very carefully with Scottish government from a FNP point of view [and] with our health board as well, but we've had to keep our clients and our nurses safe." – [Family Nurse, North]
Clients were understanding of the pandemic restrictions and ultimately valued having a line of communication with their family nurses, regardless of delivery format. However, most clients reported a preference to see their family nurse in person, agreeing that they were more comfortable talking to their family nurses face-to-face, compared with phone or video calls, and felt that in-person interactions were more efficient and re-assuring.
"I actually prefer the face-to-face, it's nice to see somebody especially during all of this, I feel like face-to-face is a lot more reassuring than over the phone and it is nice to speak to somebody who is not family either." – [Client, West, enrolled during COVID-19]
Family nurses also noted their preference for home visiting and mentioned that clients frequently requested home visits in place of or in addition to telehealth contacts. Several family nurses reported visiting homes more regularly during the summer months when restrictions were relaxed.
Overall, several family nurses stated that they conducted more home visits during the second national lockdown[2] compared with the first. Family nurses described feeling more knowledgeable and comfortable with transmission risks over time, due to factors such as lower case numbers being reported and becoming vaccinated against COVID-19. Some family nurses also felt under increased pressure from clients to conduct home visits during subsequent lockdown periods in place of virtual contacts. Family nurses attributed this to higher levels of vulnerabilities across their caseloads, often associated with the impacts of the pandemic. Most frequently these were regarded as increased mental health challenges, risks of domestic violence and changes to a family's circumstance or home environment that raised cause for concern.
Clients were understanding of COVID-19 risks when being offered a home visit. Most clients felt safe during home visits, noting that they trusted their family nurses as health professionals to appropriately use PPE and mitigate transmission risks.
"With the PPE and stuff, we were all well protected, she had her mask and her gloves and her apron on at all times, she never came in the house without it. And I knew at any point if she felt she wasn't well or anyone in this house wasn't well, that we wouldn't allow her to come in, so we felt safe with her in the house." – [Client, West, enrolled during COVID-19]
In contrast, some clients were less comfortable about receiving home visits and didn't want to put themselves, their child or their family at risk of COVID-19 transmission.
"This was when lockdown was over, but obviously still COVID was going about, so I didn't feel comfortable with her coming in to my home with, obviously, my child, due to her being… I know that she goes home and sanitises her hands and everything, but just with her being in other people's houses, I just wasn't comfortable." – [Client, East, enrolled pre-COVID-19]
Where home visits were offered, most clients were reported to take these up. However, in some instances, clients declined home visits due to reasons such as being clinically vulnerable or having 'shielding' family members; being afraid of COVID-19 risks; or having to isolate as a result of COVID-19 exposure. In rarer instances, family nurses perceived that some clients with lower engagement used reasons relating to COVID-19 to avoid face-to-face engagement with the programme. Similarly, some believed that technical issues and connectivity problems were also used by a small proportion of clients to avoid digital contact and engagement. In these instances, family nurses reflected that most clients avoiding contact were already exhibiting lower levels of engagement with FNP pre-COVID-19.
Similarly, some family nurses also reported feeling afraid or anxious about catching COVID-19 during in-person visits. Some family nurses perceived that it was not always safe to enter the clients' home due to large numbers of people sharing a household, despite taking precautions such as wearing PPE.
"They're also going to home visits that sometimes, despite every best effort, they're doing their risk assessment, they're trying to keep themselves safe, they're going in and having their PPE on, but they go in and the house is really full with other family members. And they're thinking to themselves, 'are they all following the rules … I'm in the house and putting myself out there, even though I'm trying to follow the rules myself.' And that for them at times has been scary." – [Family Nurse, West]
When addressing coronavirus transmission risks, family nurses in a number of Health Board's shared that they offered alternative face-to-face forms of programme delivery to clients. These included taking socially distanced walks or sitting outside in a café. While these types of contacts are not atypical to traditional FNP delivery, family nurses, and clients experiencing these for the first time reported enjoying opportunities for outdoor face-to-face contacts and perceived that they worked well. A number of family nurses also perceived that some clients were able to open-up and discuss more challenging or sensitive matters in a different environment (i.e., on a walk). Family nurses noted that factors such as walking side-by-side and having less eye-contact made clients feel more comfortable to disclose information or talk freely.
"We used to take them in the car sometimes for appointments or housing or whatever and you would get your best conversations there because you're not looking at them. So I think because of the teenage brain, and they find eye contact difficult, they really struggle with the video calls." – [Family Nurse, North]
4.3.2 SMS (Text Messaging)
Text messaging was commonly used between clients and family nurses for scheduling appointments, providing updates or reminders, and communicating about concerns relating to the client or their child. Text messaging was described as a longstanding method of communication in the programme (pre-COVID-19) and was perceived as being very accessible format for both clients and family nurses to communicate in between scheduled contacts.
"[My family nurse has] given me her number so if I ever felt the need to I could just text her if I had any concerns but like that sort of calling, that's usually like once every four weeks or so." – [Client, West, enrolled during COVID-19]
Some family nurses noted that clients would often send texts late in the evening or early mornings and described the importance of setting boundaries to protect their personal time by turning off work phones at the end of the workday.
"I'm thinking about one [client] in particular whose mental health has not been great. She will be quiet and 'yeah, it's okay, and it's…yeah, we're doing okay', and then I'll put my work phone on in the morning and there's a fairly extensive text about what's actually going on. If they're up feeding the baby during the night or whatever, they'll text, so I learned very quickly to put my phone off at half past four and put it back on again at half past eight, because quite a lot of my texts come in late at night or early in the morning." – [Family Nurse, West]
Overall, many described text messaging as an effective way to supplement and organise remote programme delivery. It also helped to support engagement and maintain relationships with the younger client age group, in particular.
"Text messaging is probably the main way that I do speak to people apart from videocalls, so I tend to remind them about the videocall the day before and remind them what time to connect. And then they do text now and again to say, can you call me, I've got a question about teething, and stuff like that." – [Family Nurse, East]
4.3.3 Telephone Calls
Most family nurses described using telephone calls to some extent to deliver FNP remotely. A number of family nurses reported that the majority of their remote contacts with clients were conducted over the phone. Phone calls were widely used across all Health Boards at the outset of the COVID-19 outbreak until other telehealth options became available.
Telephone calls were identified as a preferred option for many clients despite the option of videocalls being available. It was noted that conducting certain activities (e.g., assessments and PIPE) were considerably limited via the telephone as opposed to by video call or face-to-face interaction.
"My clients, at the moment, most of them want phone calls rather than NearMe." – [Family Nurse, East]
4.3.4 Video calls: NHS Attend Anywhere & NHS Near Me
NHS Attend Anywhere and NHS Near Me were frequently cited as two main modes of approved video communication with clients. Most clients and family nurses perceived the platforms as being intuitive and easy to use.
"It's really easy to use NearMe, it's really easy to use and the way it's set out and when your client reads it, it's really welcoming for the clients. [It names] the four nurses in our team… and I think that's really nice, so the client knows they're in the right place. Actually, when you text them your appointment and you put the link in it automatically comes up with a link on their phone, so they just click onto it on their phone if they've got an iPhone or a smartphone. That is so easy for them and I really like that. So I think the system is really good. I think the system is really smart… It's a really efficient system." – [Family Nurse, West]
"So, technology comes quite easy for me, I know it doesn't to a lot of people. So, I can attend anywhere and stuff that's used to Zoom and things like that, all comes second nature to me because just now a lot of my life is online." - [Client, West, enrolled during COVID-19]
Family nurses felt that they had a better sense of a child's development and the home environment via videocalls when compared with telephone calls. However, most nurses and clients expressed that these platforms did not offer the same benefits, in terms of social interaction, experience and relationship building when compared with face-to-face programme delivery.
Family nurses reported successfully using the platforms for supervised contacts and to involve clients in activities such as the interview processes for new family nurses and service improvement.
Challenges relating to technical difficulties and connection issues were raised by clients and nurses when discussing the NHS Attend Anywhere and Near Me platforms. Data usage constraints for clients were also noted, however where possible family nurses sought to mitigate these barriers by accessing mobile credit, data and WiFi for clients either through their local teams or organisations such as Connecting Scotland[3].
Many family nurses also reported that clients felt uncomfortable and anxious about engaging in video calls compared to other forms of contact.
"And I think it's, they're starting to get used to it, but it's a new way of working, even for clients, and I think some struggle, and also, obviously issues with IT, and wifi, data, you know, all the other things that go along with that." – [Family Nurse, East]
"That's right, NearMe or telephone call because a lot of our clients…a lot of my clients are struggling with video calls. Some are absolutely fine with it and actually really love it but I would say, the majority of them do struggle with it, with signal, rural living and signal or just not liking to be seen on a video call, women with low self-esteem or just feeling uncomfortable or just not liking having to balance looking after their baby and being on a screen at the same time; those kind of things." – [Family Nurse, West]
Some family nurses mentioned that their teams had been asked to nominate local champions for the use of NHS Near Me/NHS Attend Anywhere. This was described as a useful and positive link to support teams troubleshoot and resolve issues with the platforms.
4.3.5 Social Media and Other Communication Platforms
WhatsApp:
In at least one Health Board, family nurses and clients reported using WhatsApp to communicate with each other. Due to its widespread availability, some Health Board's quickly received clearance to use WhatsApp at the onset of the pandemic. Latterly, due to the introduction of NHS approved platforms and information governance requirements, approval was withdrawn for the use of WhatsApp as family nurses were encouraged to use the NHS Attend Anywhere or NHS Near Me platforms instead.
WhatsApp was considered to be a widely available, trusted and accessible to clients which enabled them to conduct phone calls, video calls and send messages to their family nurses using a familiar platform. Family nurses felt this mode of communication was particularly beneficial when engaging minority groups and for being able to send documents and resources to clients.
"And for me, there felt like a lot of pressure to move to Attend Anywhere from top down. When actually I've always felt, and I still maintain that using a WhatsApp video call was more accessible to lots of the clients. Because as a service we went to them. Before COVID we went to them. We made it easy, we went to their house, we met them where they wanted to meet us." – [Family Nurse, West]
Family nurses were encouraged to move towards a standardised approach for service delivery that adhered to NHS Scotland information governance protocols. Many family nurses reported that supporting clients to switch to another, less familiar, platform such as Near Me was a challenging aspect of the new service delivery. Family nurses continued to believe that solely moving to NHS approved platforms did not provide the opportunity to align with the interest, needs and personal preferences of clients for communication purposes.
YouTube & Social Media:
Family nurses also reporting using websites resources and NHS YouTube clips for distributing information and conducting demonstrations with clients as they felt could sometimes be more effective than providing clients with text heavy resources.
"I've used a lot of NHS YouTube clips [for] a few clients in the pregnancy days, so things like, coping in labour, induction of labour, and even virtual tours around the hospital, they have that in [my local Health Board] now, they have a link to a site for [a local] maternity unit, so using this kind of thing, like video clips. My clients are quite visual, so sometimes just directing them to a website that has a lot of written information, I don't really feel [its] appropriate for some clients. Sometimes, I'll do that and hope they read it, but I'll maybe do a bit of both, try and find more visual things that they can watch." – [Family Nurse, West]
A small proportion of family nurses also mentioned that their teams created Facebook, Twitter or Instagram accounts for the FNP service in their local Health Board's as a way of encouraging clients to connect with one another other and reduce isolation. Another suggestion included forming a WhatsApp group for connecting clients with one another to form supportive groups.
"[My team has] an FNP Facebook, Twitter and Instagram account, because again socially-wise, we want clients to connect with each other. We aren't totally at that stage yet, but at least we've now got the social media platforms as well. There's been a lot of good that actually has come out of last year, you know, with things that've been sitting in the pipeline for ages and it's actually moved on quickly because we're so desperate to have, a virtual system with these things. There has been some good that has come out of such a terrible year." – [Family Nurse, West]
Family nurses and clients also reported using emails to send and receive programme resources such as facilitators.
Microsoft Teams:
Microsoft Teams was primarily used by family nurses for team meetings, supervision, communicating with colleagues as well as other professionals and agencies. Microsoft Teams was also used for updates and quick chats between colleagues, trainings, and Child Protection meetings. Family nurses mentioned that Microsoft Teams was set up quickly for them at the outset of COVID-19 outbreak and that they find the platform accessible and convenient. Overall, family nurses had positive experiences with Microsoft Teams.
4.4 Client Engagement and Retention
4.4.1 Remote Recruitment
Recruitment rates were largely reported to have remained the same during COVID-19 restrictions. Family nurses reported conducting recruitment predominantly by telephone. Despite recruitment rates remaining roughly the same, many family nurses reported that recruiting clients using telehealth was considerably more challenging when compared with face-to-face recruitment. While the implications of this may not be centred around recruitment or attrition rates, many perceived that recruiting clients using telehealth impacted the quality of relationships and communication established during early phases of the programme.
"I have managed to recruit the majority of [my clients] but it's definitely much more difficult and then keeping that engagement through pregnancy has been difficult. I've not lost any [clients] but it's been hard." – [Family Nurse, West]
"I think… it was twofold really I would say with the pregnancy [clients] initially with the telephone sessions. When you are trying to meet [clients] face-to-face it's a lot easier to try and engage [clients] and explain about what FNP is all about initially and try and engage them on the programme. – [Family Nurse, East, 4]
4.4.2 Client Engagement and Remote Delivery
Surveyed family nurses reported the following changes to client engagement with the FNP programme following the COVID-19 outbreak: slight decrease (46%), stayed the same (32%), increased slightly (13%), significant decrease (9%), significant increase (0%). More than half of the family nurses surveyed perceived a decrease in client engagement to some extent.
In the qualitative research, some family nurses recalled initially worrying that client engagement would be severely impacted by COVID-19 and the associated changes to service delivery. However, many felt engagement levels remained stable, highlighting that the majority of clients worked well with family nurses when adapting to new forms of contact and engagement in the programme.
"I think the clients, because I worried when COVID first came, that we would lose them, and you know, because you think, what are they going to do if you stop going to visit them, are they not going to let you back in. But if anything, I think for the majority of them, it's been the opposite. Because we're their link, and you're the person that they can trust to ask things." – [Family Nurse, North]
In terms of wider engagement, most family nurses identified that existing clients who had already demonstrated good levels of engagement with the programme pre-COVID-19, largely continued to engage well with telehealth. Clients who already exhibited lower levels of engagement, were less likely to engage in the programme via telehealth.
One family nurse reported that virtual calls allowed them to engage clients' partners more successfully in the programme due to being able to offer calls later in the day suit partners' working hours. However, other family nurses felt it was challenging to engage multiple participants on a virtual call and that partners of clients would often lose interest as time went on. Family nurses drew on the importance of engaging partners and wider families early in the programme and were alert to the prospect that remote delivery could affect this negatively as partner's may have felt less comfortable engaging virtually or that there was less need for them to join in on a call.
4.4.3 Variations in Remote Recruitment and Engagement
Client engagement and interaction over telehealth was variable depending on the stage of programme (e.g., pregnancy, infancy, or toddlerhood phase). During the pregnancy phase, once clients had been successfully recruited, family nurses felt it was easier for clients to engage in the programme remotely due to there being fewer distractions at this stage.
"So, during pregnancy, delivery of the programme and maintaining the structure of the visit is easier because they're not so distracted. But that's the crucial time where you're trying to build up the therapeutic relationship." – [Family Nurse, North]
It is important to note that engagement in pregnancy is key since it is a period where family nurses can start developing strong therapeutic relationship with clients and influence positive behaviour change.
During the infancy phase, a mixture of face-to-face and telehealth contacts were valued by clients as many sought reassurances at this stage regarding their baby's development. Some clients found remote engagement more challenging during infancy and some would try to plan calls around the baby's routine or feeding times to accommodate this.
Toddlerhood was reported to be the most challenging phase for both clients and family nurses when conducting contacts using telehealth. Clients found looking after a small child was difficult while also trying to maintain focus on a video call with their family nurses. Likewise, family nurses found it challenging to engage clients remotely due to increased distractions at this stage. Family nurses and clients reported that telephone calls using speaker phone or face-to-face visits were preferable in these instances. One family nurse recalled:
"Some [clients] have really embraced it, have found it really helpful, and quite like to see your face on screen. Whereas… the ones that have found it more challenging, maybe have small children. So, if you've got a baby who needs attention and you're trying to hold a phone up, because the majority of mine are using it through phone, rather than a tablet, or a laptop. So, holding a phone, and holding a baby, it can be quite difficult in that respect." – [Family Nurse, East]
4.4.4 Retention and Attrition
In the survey, most family nurses self-reported that client retention had either stayed the same (74%) or increased slightly (6%) following the COVID-19 outbreak. A slight decrease was reported by 18% of family nurses and only 1% reported a significant decrease.
Overall FNP attrition rates were perceived to be low throughout the COVID-19 pandemic period. Family nurses felt that any clients who dropped out of the programme were previously at risk of doing so pre-COVID-19.
The qualitative research revealed that there was an overall sense that attrition rates had remained low due to the importance of the FNP programme and support provided to clients and their children during a time of widespread difficulties and isolation.
"I really do think we're seeing very little attrition. We're seeing very [few] people leaving the programme as well. I think what the clients are telling us is having that contact with their family nurse is more important than ever because they might be the only person they're getting to see out with their home." – [Family Nurse, West]
4.4.5 Sustaining Engagement via Telehealth
A few family nurses mentioned that clients were beginning to struggle with fortnightly telehealth engagement over time and began requesting more home visits and face-to-face contact. This was often described in reference to lockdown restrictions re-introduced towards the end of 2020 and early 2021. Family nurses perceived that clients were becoming fatigued with ongoing virtual contacts and were expressing preferences for face-to-face contact.
"Right now, keeping clients engaged is quite difficult. They've done really well but they're getting to the point where I think we're all starting to notice that they're struggling. Yeah, they're starting to say, no, I don't want a phone call, I want you to come and visit. So they're not saying that they won't engage with the programme but they won't engage with the programme remotely anymore, so that's quite a challenge." – [Family Nurse, North]
All clients interviewed were ultimately understanding of the restrictions and the need to conduct contacts remotely but those who had received face-to-face contact expressed how valuable it was to be able to speak in person with a trusted source of support and receive reassurance about their child's development and wellbeing. Clients who had been engaging remotely for longer periods of time felt that being offered reassurances and positive feedback about their children via remote platforms was less beneficial compared with face-to-face contact. Clients felt it was important for their baby's development to be reviewed in-person and looked forward to the resumption of home visits for this purpose.
"Well, I prefer face to face talking, especially when it's about the wee one, because it is kind of hard to like think what he has been doing, and like do it over the video call. It was just easier when she was there and she could actually see for herself what he's doing." – [Client, West, enrolled pre-COVID-19]
4.4.6 Barriers and At-Risk Groups
While many family nurses felt able to engage a proportion of their caseload in the programme remotely, particular challenges were reported for certain groups of clients such as those with complex vulnerabilities, migrants and clients who spoke English as a second language. Family nurses generally perceived that it was not feasible to engage their most vulnerable clients remotely and felt strongly that home visiting was the most appropriate form of engagement in these instances.
Clients living with mental health conditions such as ADHD, anxiety, and depression were perceived to have difficulties engaging with the programme remotely. Family nurses reported clients with poor health were less comfortable to speak over the phone or by video call. They also noted an increase in poor mental health across their caseloads during the pandemic partially attributed to by the re-introduction of national lockdown restrictions. Some family nurses felt that clients struggling with their mental health were more able to withdraw and hide their circumstances or avoid remote engagement attempts.
"We can still deliver the programme and we can still check in with them, but they can shelter us a bit and hide from us if they don't want us to know, if they don't want to know that they're feeling particularly low or whatever, they just don't tell us. They're on the phone, and so it's easy for them to not have to admit if there's something going on, or something they're not coping with, or they're just feeling a bit rubbish that day, do you know." – [Family Nurse, West]
A common finding reported by family nurses was that clients often felt very self-conscious or anxious discussing themselves or their situations over a video call.
Family nurses also felt that they were less able to detect cues from client's body language remotely and that this presented challenges when trying to communicate effectively. Some of these challenges have been highlighted within modes of service delivery, under the video calls sub-theme.
4.5 Programme Dosage and Fidelity
Most clients were reported to be within fidelity ranges[4], often due to the increased provision of additional contacts. Family nurses perceived that some of these clients were at most risk of being unable to meet programme fidelity. In these instances, family nurses had difficulties maintaining engagement and had limited opportunities to offer in-person engagement to clients whose situations did not warrant essential home visits.
Interviewer: "Have you seen a difference in clients meeting fidelity ranges over the past few months?"
"Yeah. I think I've got clients who are probably well within fidelity range, rather than just meeting it. Well within because they've needed a bit extra. And I've got the other clients, as I say, that group who don't do phone calls, don't do Near Me, don't respond to letters, will see me but if they can't see me, they're not doing it. If they can't see me in person, they're not doing it. That's really affecting things, yeah." – [Family Nurse, North]
Family nurses reported that opportunities provided by different telehealth modes helped them achieve dosage[5] with some clients who were busy with work or education commitments. Clients also mentioned that they appreciated this flexibility and the convenience afforded by remote contacts when trying to manage responsibilities and commitments.
Most clients did not experience any major differences in the number of contacts with family nurses during COVID-19 compared with prior programme delivery. Many clients reported keeping in contact with their family nurses via text messaging between scheduled programme contacts and most felt able to contact family nurses with queries and concerns during this time if necessary. The quote below from a client reflects this:
"Every two weeks I think where we have a proper catchup every two weeks, but I can text her or phone her any time if I've got any questions or anything. So, sometimes it's maybe like once a week, but it will just be over text type thing, but we have a proper catchup every two or three weeks." – [Client, West, enrolled pre-COVID-19]
Clients who were pregnant commented that they were given the choice on how frequent visits would be.
"Yes, she came over to my house for the first 12 weeks, and then she had to stop for the last trimester just because it was a bit unsafe, but she still…I had voice calls with her every week when she couldn't come which was also really supportive… It was a choice that she could still come and see me in my last trimester or do phone calls, and I picked phone calls for her safety as well." – [Client, West, enrolled during COVID-19]
Virtual meetings over videocall were reported to be as frequent as home visits.
"[My family nurse] has not really been able to see [my baby]. Just having to, like, video call and stuff. You know, not being able to see [my baby]. Not being able to see her grow up more and… it's harder not knowing what she's weighing and stuff like that, I think. But we have…I managed to see her a few times. But, yeah, it has affected it…kind of." – [Client, North, enrolled pre-COVID-19]
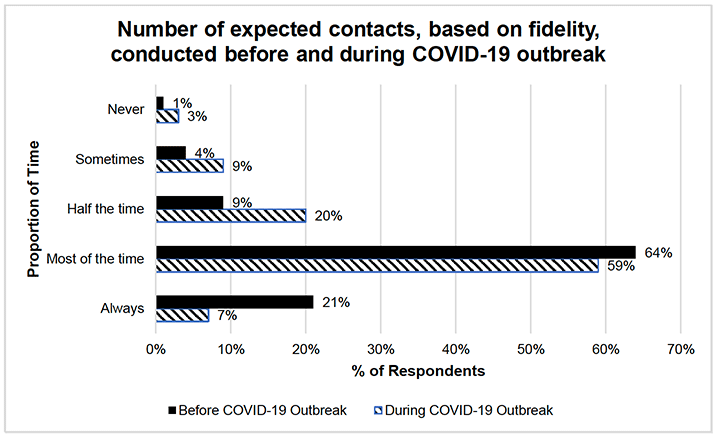
In terms of programme dosage, survey findings show there are small differences in the overall self-reported provision of visits to clients, before and during the COVID-19 pandemic. Figure 5 shows that during COVID-19 there was a slight decrease in the number of contacts being conducted. For example, family nurses reported a decrease of 14% in always meeting programme fidelity following the outbreak, and a 5% decrease in meeting this most of the time (see Figure 5).
4.6 Additional Contacts and Support
Many clients discussed having ongoing personal issues that they spoke to family nurses about informally between visits. Although scheduled contacts were weeks apart, clients were able to contact their family nurses by phone call or text message regularly between visits. Many clients felt that contacting family nurses this way built a more personal relationship. They commented that their family nurses were key supportive figures in their lives whom they trusted and felt able to contact regularly with any concerns.
"I've personally got [my nurse's] number so I can text her if I've got any questions and she'll give me the information. Even if it's not a scheduled call time, she's always there and can always help us. And it's like, I don't know, it doesn't feel like a teacher type of thing as such, it's more like a friend." – [Client, East, enrolled during COVID-19]
Increased vulnerabilities such as mental health challenges, increased risk of domestic violence and changes to family circumstances during the pandemic have meant that some clients required higher levels of additional support. FNP nurses felt they were amongst some of the few professionals working with vulnerable clients during the pandemic and as such provided more support to clients who needed additional contacts during this time. Some family nurses commented that providing such increased levels of support was unsustainable in the long-term.
"I would say we have managed. And I suppose that would be to the credit of the nurses that are delivering the programme that we would still maintain the same level of service. But we've had to – the [clients] say in the green level – they're still getting their fortnightly contacts but those in the red zone are getting much more contact than that. Which, I suppose I would say it impacts on the nurses. We're doing it but I think longer term it's going to burnout, people are feeling extremely stressed and, you know, that's what I think it is. It's impacting on the nurse as well, being longer term it cannot be sustainable." – [Family Nurse, North]
Self-reported survey findings indicated that family nurses perceived that their volume of additional visits was somewhat above average (20%) or far above average (2%) during the COVID-19 outbreak. These findings were slightly lower for self-reported visiting patterns prior to COVID-19, which were 25% and 3% respectively (see Appendix 2).
4.7 Therapeutic Relationship
Relationship building, communication and social interaction were found to be negatively impacted by the use of telehealth. Early relationship building was reported by family nurses to be the most significantly affected aspect, perceiving that it took longer and required more effort to establish a strong therapeutic relationship with clients remotely. Over time, family nurses felt able to build the relationship with clients as normal, but many reported that face-to-face contacts were key to establishing this more successfully.
"So, I do feel like probably my relationship with the [clients] that I've recruited during lockdown is not quite as good as the ones I had recruited before. Because they've all been on videocall as opposed to face-to-face. So, I feel there is a bit of a barrier there." – [Family Nurse, East]
Family nurses also felt that clients were less able to disclose and communicate feelings about issues over the phone or by videocall and felt that it was harder to pick up on subtle cues that would usually alert them to an issue during a face-to-face interaction.
No clients reported feeling unsupported by their family nurse. Clients perceived their relationships with family nurses as valued and highly personal, often describing them as trusting and reliable professional friendships.
Being listened to and supported often gave clients much needed assistance during a challenging and vulnerable period of their lives. For clients, the pandemic only made this relationship more necessary to their support system when access to other services, family members and friends was often restricted.
"I mean I think more than anything having someone to talk to. I think everybody has been really isolated during COVID and well, I haven't really been able to see people and with being pregnant, I've tried to keep myself away from as many people as possible, so getting to actually add to that and bond with somebody I think made that even more special" – [Client, West, enrolled during COVID-19]
While clients felt supported overall by the programme, a number felt slightly less supported by virtual and distanced communication. Clients' reflections on the impact of COVID-19 on their relationship with their family nurse demonstrated a preference for face-to-face communication, which they agreed had lessened during the pandemic. Many clients commented that it was easier to build up a relationship face-to-face. However, clients recruited during the pandemic felt they were still able to establish a good relationship with their family nurses and while happy to receive the programme regardless of delivery mode, they looked forward to receiving more in-person visits in the future.
Although clients felt that being able to text message their family nurse when needed, many mentioned that talking to someone face-to-face was more important therapeutically to discuss complex or personal issues and to relieve anxiety or provide reassurance.
"Yeah, it's really good. It really just helps to kind of keep myself and my partner in check. 'Cause if there's just anything we have doubts about or, as well 'cause it's a lot about becoming a parent but it's also about how we're feeling. And it's almost like a therapy session but it's not in such a drastic way. It's just kind of making sure we're all feeling okay with it. And if we're not then getting help and advice on what to do about that". [CLIENT, EAST, enrolled during COVID-19]
Many clients described their family nurse as being their 'first port of call' or 'go-to' and highlighted a number of instances when family nurses went 'above and beyond' to help them address issues during the COVID-19 pandemic.
"[My nurse], she asks this all the time, she says, 'is there anything I could do better?' Literally nothing, I don't know if it is the programme or if it is her or if it is everything put together, but everything is just better than we could ask for. She has opened up a lot of opportunities, like we are struggling to get moved, our house isn't really appropriate for the baby to come in to and she is working outside of her duty to help us with that…she is helping us in real life as well not just, 'oh, this is how you be pregnant, and this is how you bring up the baby'. She got stuck in to just helping us all round. I would say her as a whole in the programme it works really well for us." – [Client, North, enrolled during COVID-19]
4.8 Programme Activities, Assessments, and Observations
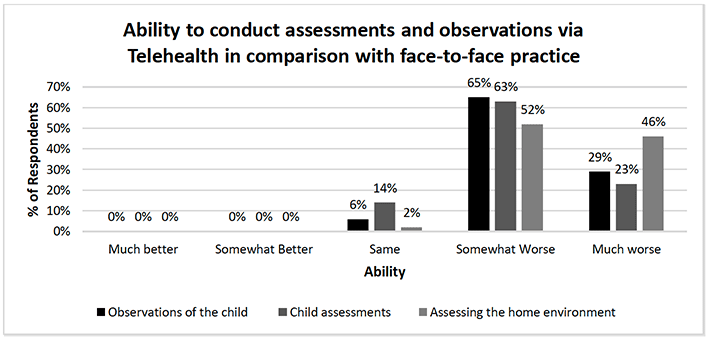
Overall, survey, focus group and interview findings all showed a significant impact on the ability of family nurses to effectively conduct assessments and observations using telehealth. Figure 6. illustrates the survey findings. These show that the ability to conduct assessments of the home environment was most affected, with 98% of family nurses reporting this had been negatively impacted, overall. Observations of the child were perceived to be negatively impacted by 94% of family nurses and child health assessments were reported as being worse by 86% of family nurses. No family nurses reported improvement in any of the key assessments and observation domains.
In relation to clinical observations, family nurses reported that their ability to do this via telehealth was somewhat worse (76%), much worse (17%), about the same (6%), somewhat better (1%) and much better (0%), see Appendix 2.
4.8.1 Partners in Parenting Education (PIPE)
Most family nurses felt that telehealth limited their ability to conduct PIPE activities with clients due to their interactive and illustrative nature. They relayed that some activities were very challenging to deliver virtually and perceived that clients were finding it difficult to engage with these activities remotely. Family nurses specifically cited not being able to do certain activities that involved props such as a doll and expressed that they tried to be more creative and innovative to adapt the programme.
"So, [for] PIPE, you really need to bring stuff out to the house, so often you would bring a doll to do a demonstration, or you would bring some kind of toy, which it's very difficult to do that over a videocall. There are a few that we can do on videocall but not many. So I think probably all together we might have 25 PIPEs and there might be three that we can do at the minute. So they're missing out on that." – [Family Nurse, East]
Clients reported that remote delivery impacted the use of facilitators in the programme. Clients described finding programme materials and teaching from family nurses useful and informative. When family nurses were able to show clients practical information in person, clients reported finding this to be a more positive and useful experience compared with remote formats. Some clients described that during periods of lockdown, family nurses had stricter guidelines, so were unable to use facilitators in clients' homes.
"Yes, actually before Christmas she brought a baby… it was like a weighted baby… and we did this exercise during the appointment seeing what we did with a baby when we were left with it, to see if we are the kind of people that would just kind of sit with the baby slumped on the couch, even though it is a pretend baby. Like were we going to be responsible with this baby. I would say it was quite fun to be honest, like I'm finding quite a lot of it quite fun. It's not, it doesn't feel like a programme, it just feels like we've just got somebody coming to see us to have a chat some days." – [Client, North, enrolled during COVID-19]
4.8.2 Assessments of the Home Environment
Family nurses felt that remotely assessing home environments was extremely difficult, or 'impossible' in some cases. Key challenges related to being unable to identify who else might be present in a room with a client and being unable to detect the overall condition of a home as well as more subtle signals including, family dynamics, body language, smells, and potential hazards.
Several family nurses reported conducting home visits with clients following extensive period of remote delivery, to ascertain more about the home environment. Sometimes these visits allowed the family nurse to see that the client's home environments had become a cause of concern which they were unable to detect from remote consultations.
For clients enrolled pre-COVID-19, family nurses felt that they had a better sense of potential risks based on previous home visits and were mindful of issues to monitor in subsequent remote contacts. However, for newer clients enrolled during the pandemic restrictions, it was thought to be more difficult to adequately assess the home environment. Although family nurses felt that NHS Attend Anywhere and Near Me helped to some extent, it did not facilitate a complete assessment of the home environment.
"… the fact that you can say that you actually saw the child has been incredibly helpful by Attend Anywhere. But in terms of a robust assessment of the home environment…and again all of that stuff about picking up cues if you're thinking about domestic violence and what's going on for a family, that has been very, very challenging, doing that by virtual means." – [Family Nurse, West]
4.8.3 Ages and Stages Questionnaire (ASQ) and Child Development Assessments
The ability of family nurses to fully assess child development remotely was generally thought to be limited to some extent, however many family nurses felt they were more able to conduct ASQ assessments using telehealth, compared with other assessments, and continued to conduct these throughout the pandemic restrictions.
Family nurses indicated that many of their clients were already familiar with ASQ assessments and were able to complete the questionnaires independently due to its parent-led nature. However, family nurses reported that they encountered challenges when conducting ASQ assessments with clients who did not speak English as a first language and those who had low-literacy levels.
In terms of assessing the child's health and physical conditions, family nurses cited having some difficulties. However, the transition from phone calls to Near Me was thought to have positive impact on assessments of any visible health problems.
4.8.4 Dyadic Assessment of Naturalist Caregiver Experience (DANCE)
A large number of family nurses reported that the FNP Dyadic Assessment of Naturalist Caregiver Experience (DANCE)[6] was one of the most challenging aspects of the programme to conduct remotely. Family nurses had difficulties fully observing the interactions between mothers and children over videocalls.
"We were under quite a lot of pressure to do even DANCE assessments over a virtual call… because we were still learning, for lots of different reasons none of us really feel particularly confident with DANCE. So, to try and then do it over a video call was just…it was too much. And I was keen to do it, happy to do it, enthusiastic to do it. But it just felt like too much. And just one extra thing to think about." – [Family Nurse, West]
4.8.5 Identification of Concerns
Intimate Partner Violence (IPV) assessments were reported to be predominantly conducted during home or face-to-face visits. Family nurses felt that it was inappropriate to conduct these assessments remotely, as they could not tell if other people were also present in the client's home environment and were unable to fully gauge the client's level of comfort discussing these matters through their body language and social cues.
"One of the biggest barriers was two families in April/May time, I was thinking, there's something going on here. I don't know what it is. I couldn't ask the IPV questions, 'cause I didn't know who was in the house [or] where. I could tell from the mum's voice something was not right. And one mum gave me snippets but when I tried to pick it up, you know, she said something like, 'oh he's just gone out the door', and she'd said to me something like, 'you've no idea what it's like here really'. And I'd said something like, 'can I ask a wee bit more about that, I'm worried about you, and I have been worried for the last few phone calls'. And she just shut it down. She just said…'and he'…I didn't think he had come back into the house but I didn't know." – [Family Nurse, North]
Family nurses felt under significant pressure to identify concerns or unseen harms remotely, often mentioning that they were worried about their clients when they were unable to see them face-to-face. Many assessments had to be made based on 'snapshots' of clients lives which was perceived to be unfair. Family nurses also referred to the importance of having 'eyes on the child' and felt that video calls were vital to achieving this remotely.
4.9 Experiences of Telehealth
4.9.1 Prior Experience
The majority of family nurses reported never having used many telehealth modes to deliver the FNP service prior to the COVID-19 outbreak. Most family nurses surveyed reported that they had no or limited prior experience of most video-enabled telehealth platforms in their roles. Prior usage of Attend Anywhere and Near Me was reported by only 9% and 7% of family nurses, respectively, while 11% reported using other video call platforms with clients, see Table 3. Some family nurses reported using telehealth in previous roles, predominantly via telephone calls, but did not report any extensive service delivery conducted in this manner.
"My work was really supportive, so FNP was really, really supportive, and there was equipment available and there was advice available and there was support available. It was my lack of knowledge and skill that was the big barrier for me, because it was just not something I was used to doing." – [Family Nurse, East]
| Telehealth Mode | Yes – previous experience | No – previous experience | Don't know |
|---|---|---|---|
| Telephone calls | 92% | 8% | 0% |
| 31% | 69% | 0% | |
| Attend Anywhere | 9% | 91% | 0% |
| Near Me | 7% | 92% | 1% |
| Video Call (other) | 11% | 89% | 0% |
4.9.2 Digital Divide
Family nurses perceived that most clients felt comfortable and familiar with technologies such as Near Me and Attend Anywhere. There was an impression among family nurses that some clients were good at using technology whilst others were not confident using technology and there could often be disparities among their caseloads regarding clients' levels of digital literacy.
There were concerns among family nurses about the impact of digital exclusion and potential inequalities emerging in the access to the service for many of their clients. Many family nurses recalled accessing resources including, top-up cards, phone credit, mobile phones, laptops and tablets for clients via their local teams, Connecting Scotland and other third sector organisations. A strong need to support clients with technology and digital access was perceived and family nurses felt that these changes were placing already vulnerable clients at a greater disadvantage of accessing essential services and support.
"I had quite a vulnerable family that had, yeah, children that needed, a clinic review, which was, so they were emailed Word documents to fill in, and you know, to come on a video call, and things. And just in terms of, you know, experience using that, they didn't have a laptop, there's no way they could have filled in the Word document and didn't have the resources to do that. It makes you realise that this sort of telehealth, and using technology, can really, really, for vulnerable people, put them at a greater disadvantage." – [Family Nurse, North]
Having insufficient internet data and phone credit was reported by both family nurses and some clients as a barrier for keeping in contact with family nurses and other services. Family nurses reported having to provide devices and data for clients so they could maintain engagement with the programme and access other services.
"…obviously actually having access to devices, that has been a huge challenge. At the beginning of the pandemic, we had a number of clients that didn't even have a mobile phone. And we've worked with the third sector, which have been incredibly supportive. They gave us some mobile phones with data and top up cards at the beginning of the pandemic so that [clients] could still stay connected. And that was a huge thing. We've also worked with many charities to try and access applications for laptops and Chromebooks…iPads as well, which again, the digital exclusion stuff has become something that we're really, really mindful of and we can't have inequality and clients not being able to receive the programme if they don't have a device." – [Family Nurse, West]
Of surveyed family nurses, 34% strongly agreed and 36% agreed to some extent that the use of telehealth in FNP could lead to exclusion of clients due to a lack of technological access, see Appendix 2.
4.9.3 Connectivity
Connectivity issues were widely experienced by clients and staff using video call platforms such as Near Me. Audio and video issues were also common and many family nurses expressed that this made calls feel disjointed and frustrating.
Most clients were reported to have Wi-Fi access during the first lockdown. Many family nurses and clients reported that local FNP teams, Connecting Scotland and other organisations were able to source connectivity support for clients including, Wi-Fi boxes, Wi-Fi cards and mobile data at the early stages of the pandemic. These provisions were thought to be instrumental in allowing clients to maintain remote engagement with the programme and other services.
Family nurses agreed that being able to provide devices, data and credit to clients so quickly was an important factor in reducing barriers for some clients. Other clients were reported to have more difficulties with technology and lower levels of literacy which was a more challenging barrier for family nurses to overcome with clients. One family nurse reported that the provision of devices provided opportunities to engage with clients. This is illustrated below:
"I think that will be good for the [clients] because we can share that journey with them. 'Oh, brilliant, you've got a new iPad, let's talk through it together, let's build it up together and, oh, let's see if we can talk together on it.' I think that's a really positive thing and might help all the things that have been a bit of a struggle." – [Family Nurse, West]
4.10 Access To Resources, Equipment and Training
4.10.1 Access to Resources and Equipment
Overall, family nurses felt well equipped and supported to conduct their work remotely. Most family nurses reported that they had laptops, smartphones, PPE, headsets, access to patient records, printers, mobile credit and internet data, as well as chairs and PC monitors from the office to help make home working easier. Family nurses also reported having access to VSee (the service used by social care and council services) and IT support from their Health Boards.
Of surveyed family nurses, 79% agreed (40% somewhat agree and 39% strongly agree) that they had access to the necessary tools and equipment for remote service delivery.
Despite most family nurses reporting feeling well equipped to deliver the FNP remotely, a small proportion of family nurses felt that they had inadequate technology, devices or resources that impacted their abilities to deliver the programme.
In two Health Boards, nurses experienced delays receiving laptops and work mobile phones. Wait times varied, but a few family nurses reported waiting approximately 11 months to receive devices since the transition to home working. Family nurses who had not received laptops were reliant on delivering FNP remotely using smartphones, personal devices, sharing laptops with other team members and going into their offices at designated times to use computers. The issue was linked to long delivery delays for equipment and was typically resolved quickly when the equipment arrived. Some family nurses also reported issues accessing computerised health records remotely.
Family nurses from several Boards reported that their mobile phones and laptops were outdated and incompatible with certain software and telehealth platforms. Some devices did not have cameras, which made delivering video call contacts with clients and meetings challenging. Some also reported difficulties when downloading applications such as Microsoft Teams onto their phones due to operating system incompatibilities.
"Although we have [devices], it doesn't always work the way it should. And because there's been more of a reliance on a virtual way of working, that has been quite challenging. And I think, certainly in [my Health Board], we've realised that a lot of our IT equipment is coming to near the end of its life, but I think we're in a very long queue to have it replaced. So it's an ongoing issue and challenge, and I think, probably quite a lot of the nurses and myself have had our computers rebuilt, but it's a wee bit like the million dollar man, you know, it's not quite getting there, it's just adding bits on and it'll work for a bit, but it's, the unreliability of it can be a bit stressful as well." – [Family Nurse, West]
4.10.2 Clients Access to Resources and Equipment
When clients discussed access to resources and equipment two areas of access emerged: provision of technology; and access to programme materials. Clients described new schemes and grants that provided them with a laptop, phone or iPad and free data. This was understood to facilitate communication with family nurses and improve clients' ability to engage with family nurses and other learning opportunities.
"Well I've applied for college. I did that when I first got the laptop. So hopefully I'll find out if I'll get in and stuff. And I think that'll all be through, like…online anyway because of COVID. So it's helpful that we've got a laptop." – [Client, North, enrolled pre-COVID-19]
Clients frequently discussed using facilitators and workbooks in their engagement with the programme. Many clients commented that these were hard copies that they received during home visits from family nurses or through the post. Clients commented that for virtual meetings, family nurses would post material to clients before the meeting or would drop it through clients' letterboxes. Some clients described delays with postal services, meaning they did not have the requisite material for scheduled videocalls. A few clients expressed that they also received information through email, which they commented was easier because of fewer sheets of paper.
"Yes, especially my family nurse gives me a lot of notes and stuff, so it was waiting for them to be posted out and it is just, it's a wee bit of a nightmare when we had to do it over the phone, just like delays with the post office and stuff. So, I feel like it is a lot better when she is able to come face-to-face, we can get everything done on that day" – [Client, West, enrolled during COVID-19]
"Yes, so when it was face-to-face visits that's when I first received my blue folder, and week after week we kind of built up the folder with the materials and went through them and stuff. But since this most recent lockdown and the Zoom visits, it's been posted out to me well in advance, so by the time my next appointment came, that I had it all on time" – [Client, West, enrolled during COVID-19]
4.10.3 Training
Of surveyed family nurses, 90%, reported being provided with some form of guidance to support their working following COVID-19. In addition, 68% of family nurses reported being offered formal training opportunities to support their working during this time, 23% reported being offered no training and 10% were unsure, see Appendix 2. Family nurses reported receiving or accessing training and support from a variety of sources namely: their supervisors, the FNP National Team who distributed good practice guidelines, NHS Education for Scotland (NES), local health boards, FNP, TURAS, and UNICEF guidelines. Local FNP teams were also cited as being extremely supportive and involved in peer-learning activities.
Family nurses recalled receiving tips and instructions about delivering the programme remotely, as well as webinars about using NHS Near Me/Attend Anywhere. Many reported FNP-specific training around conducting PIPE activities and DANCE assessments virtually. In addition, many family nurses also received training on IT systems, skills practices with their teams focusing on activities such as motivational interviewing, conducting a breastfeeding assessment remotely, and psychology supervision. Family nurses noted that the availability of a wide range of support was helpful and helped them feel confident to carry out their roles remotely.
Some family nurses found training and support to be more limited. Concerns centred around high levels of preparation for some training opportunities which could feel overwhelming, as well as confusion caused by unclear instructions and frequently changing COVID-19 guidelines. Other issues were noted around a disconnection between training on how to deliver PIPE and DANCE via telehealth, and real-world situations where the feasibility of successfully doing so was significantly limited.
"We had guidance for delivery of FNP on telehealth. We had a training session about the delivery of PIPE, activities via NearMe, and we've had… I don't know if there was actual training or if it was just guidance, but there is a guidance thing about doing a DANCE observation over a video."
Interviewer: "And would you say that you feel equipped to carry out these assessments using telehealth?"
"I'm probably as equipped as you could be, but I don't think it's practical to expect people to do that and it just doesn't work." – [Family Nurse, North]
Several family nurses also reported not receiving any formal training relating to telehealth. A couple of family nurses said that they had received some tips on telehealth, however, after practicing they found using platforms such as Near Me intuitive and straightforward. Microsoft Teams meetings by supervisors and team-level support were mainly used in place of formal training. Overall, most family nurses reported that they had access to support at some level and did not describe any negative impacts from a lack of formal training in the use of telehealth.
"I would say, no, I didn't receive any formal training for anything. However, we have the weekly team meeting, and I think a lot of that, my poor supervisor was sort of taken up by people having teething issues with various things, and trying to find ways round things, and maybe reviewing it at the team meeting the week after. So that's, you know, that was kind of our main sort of access of support for any issues we were having with any of the new ways of working." [Family nurse, East, 11]
4.11 Privacy and Confidentiality
Clients and staff both identified concerns with privacy and confidentiality. Family nurses were frequently concerned about their client's privacy on phone or video calls, without knowing who else might be present in the room or home. One family nurse reported that meetings in parks and socially distanced walks gave clients a safe space to open up about sensitive issues.
Working from home presented a number of challenges for family nurses in terms of having private spaces to conduct confidential calls, avoiding interruptions and being able to store data safely and securely. Some clients also reported feeling uncomfortable with family nurses working from home. Some family nurses felt uncomfortable about clients seeing their homes in the background of video calls and preferred being able to blur the background or positioning themselves in front of a blank wall for their own privacy.
Family nurses mentioned that they had received guidelines for working with and storing confidential data at home. However, in Health Board's that used paper records, family nurses felt it was more difficult to store and maintain the confidentiality of these at home compared to electronic records.
"…my children have to do their schooling and I have to use the laptop too. We don't have resources coming out of our ears in this house. So I would say there's been a lot of careful negotiation with my video calls. Really, really careful management of the diary, ensuring that you've got privacy for confidentiality reasons. And sometimes asking sensitive questions on a video call can be challenging because you don't know if that person is genuinely alone in that room on their own, you know?" – [Family Nurse, North]
4.12 External Partnership Working
External partnership working appeared to be significantly impacted by the COVID-19 pandemic. Many agencies were reported to have limited operation which caused interruptions to referral chains. Limited access to services such as benefits advice, housing support and mental health services were described by family nurses as being most problematic. Other difficulties were noted regarding the limited or halted operation of services such as learning disability support, sexual health services and contraception access, education and employment support, Childsmile, and childcare.
"[services] are not seeing people in poverty. I'm finding the clients have difficulty accessing benefits, no gas, run out of gas, electric, food. And we're usually the first person they call. I mean, we were referring clients to the food bank and things like that, for benefit help and things. But just on a weekly basis I'm getting people, you know, running out of gas, electric, food, just not coping at all." – [Family Nurse, North]
Long waiting lists were reported by family nurses for access to speech and language therapy and paediatricians, and family nurses mentioned that many clients were not always offered face-to-face GP visits for their baby's six-to-eight-week check which would take place via phone consultation or be suspended in some areas for a period of time.
Family nurses noted that some local authority agencies and support charities were no longer accepting referrals or did not respond to requests for support. These agencies included housing support, homelessness teams and voluntary organisations. Family nurses found it challenging to work with some third sector organisations and other agencies who were frequently unable to deliver the required level of support to clients. Family nurses described that a lot of external support was provided online or virtually which they deemed inadequate when clients needed important face-to-face, in person, support during times of crisis. Family nurses also thought that clients were less likely to engage in virtual services as many had limited access to internet-enabled devices or phone credit so were unable to access services.
"They would normally have gone to the community centre to get help or to use a computer. You know, to fill out benefit forms, to get help. They can't do that now, they've shut the community centres. The benefits are all online but they can't fill in the forms online because they don't have mobile…they don't have devices, they don't have Wi-Fi. So I 'phone them and then I get – I've hardly any food, I've run out of gas, I've run out of electric. And we're the only people seem to be checking in with these clients as well. So it's these people with low resources that are really the most vulnerable." – [Family Nurse, North]
Family nurses felt as though they were trying to 'fill service gaps' that had emerged during the pandemic and they were often the only professionals involved in clients lives. Although nurses had received significant training in mental health they felt that were dealing with an increase in complex mental health cases which was beyond what they were trained to handle.
"We are now having to pick up a lot more and be left kind of holding a lot more cases that are particularly difficult than we were before, without the additional support of other services. Which then dilutes the programme that we're offering. And the level of training we have in relation to mental health I think – well, we don't have loads of training in relation to mental health when, like I say, we're dealing with someone suicidal once a week at the moment. That's a new thing, that we would be dealing with it to such an intensity." – [Family Nurse, North]
4.13 Managerial Support, Clinical Supervision and Communication with Colleagues
Family nurses saw the Scottish Government, Nursing Midwifery Council, local health boards, and FNP Scotland as key levels of management that influenced the direction of changes to service delivery. Nurses described receiving valuable levels of support from managers and colleagues during this time.
"I think it's been really positive, particularly in the beginning when the first wave was hit, we were having almost daily meetings, daily briefings about the changes and keeping us as up to date as possible. Things then were changing all the time, so it was really good to have that quick discussion and know it there and then, instead of feeling a bit overwhelmed and not really sure what we were supposed to be doing. Although things were changing we were all in it together, so I do feel that side of things has actually been really good" – [Family Nurse, West]
4.13.1 Clinical Supervision
Family nurses reported receiving supervision remotely and face-to-face via socially distanced walks, depending on local restrictions. It was widely agreed that regular clinical supervision was crucial to their roles and emphasised the importance of these meetings in terms of decision-making, supporting emotional wellbeing, problem solving, adapting to changes and being able to reflect on work practices during a challenging time.
"I mean, supervision from my point of view and the feedback I'm getting from staff has felt very, very important because of the nurses' emotional wellbeing as well and supervision, you know, quite rightly has not always just…it's not always just focussed on the visiting pattern. It's also about how they are, how the staff are coping." – [Family Nurse, West]
Family nurses felt that supervision generally worked well over video calls, using Microsoft Teams, but many felt that the added value of face-to-face meetings could not be replicated remotely, (see Appendix 2).
4.13.2 Communication with Colleagues
Family nurses in health boards with split teams had mixed opinions about the remote delivery of weekly meetings. Many in rural areas commented that it improved engagement as family nurses did not have to drive long distances for team meetings. However, family nurses commented that they missed face-to-face interaction with their teams and felt that their sense of connection with colleagues was lessened during periods of ongoing online communication. Some family nurses felt isolated working from home. Some nurses described having team WhatsApp groups, regular coffee breaks or catch-ups before team meetings as opportunities to stay connected in a more informal manner.
4.14 Impact of Covid-19 Pandemic on Clients
Many clients felt that COVID-19 had impacted negatively on their lives, particularly in regard to poorer mental health, employment challenges and social isolation due to COVID-19 restrictions. Clients all agreed that the programme was a significant source of support in their lives during a challenging time.
"I think like I've found the worst part is just…like having a baby's always hard but then it would be so much easier if…because if COVID wasn't a thing, I would be going out, like to baby groups and seeing my friends and it would just take the pressure off. But it's literally like just inside the house looking after a baby all the time with no break, you know, and then not having people to support me as much. It is really difficult. Like even, like I was going to baby groups a little while before the lockdown again just as something" – [Client, West, enrolled during COVID-19]
Family nurses also discussed the significant impact the pandemic has had on their clients with notable increases in mental health challenges. A few family nurses also commented that they had observed increased rate of suicide attempts on their caseloads following the onset of the pandemic. Family nurses mentioned that some of their clients 'were going weeks without speaking to anyone' other their family nurse and were becoming very isolated during the pandemic.
"They're used to their babies being seen all the time, for clients who have been on the programme longer, and it was really difficult, especially to start with. Especially for ones who had babies under six months, they really struggled. And I've had a lot of clients who have developed quite severe mental health problems throughout the last year. And trying to manage that has been pretty impossible because there are no other services running really." – [Family Nurse, North]
Clients' personal challenges made them realise that the programme was a significant source of positive change and support in their lives. Clients felt family nurses motivated and supported them, not only to learn more about motherhood, but also to try and make positive lifestyle changes.
"I mean, oh she's been amazing, like. She's helped a lot because, I mean, I…like, it's just some little things, not even just the pregnancy. I mean, I lost my job at the start of the pandemic last year and that was a major stress. And, I mean, she didn't…she doesn't just help with anything to do with babies, she just helps with everything in general…she'll sit and speak about me, my mental health and how I'm feeling and what I'm wanting to do in the future and things like that. I mean, like, it's a really trusting relationship that I've got with her" – [Client, East, enrolled during COVID-19]
Some clients discussed feeling empowered by their access to informative materials and described having more free time during the pandemic to read and digest this information.
"[the resources] was a really helpful thing. I mean, a lot of the stuff I knew because I was that bored that I would sit and research absolutely everything. A lot of the stuff was actually really handy to know and I got a lot of, good websites to look up and…I mean, even still now I still get shown things that I didn't know and there's a lot of helpful stuff". – [Client, East, enrolled during COVID-19]
When discussing reasons why they had enrolled on to the programme, clients perceived FNP as a source of 'extra support'.
"Yeah, I think so. Like, I wanted to build a good relationship. I think that was one of the main reasons. And getting more help, 'cause I know some people with health visitors, they don't see them, they don't really build a connection as much as you do with a family nurse. I think I have been able to build a good connection but not as much as I would of if it wasn't 'cause of lockdown and stuff". – [Client, North, enrolled pre-COVID-19]
When recruited onto the programme, clients felt well supported by the family nurses. Clients discussed three key reasons for this: accessibility of family nurses; personal commitment of family nurses to their job and clients; and non-judgemental support.
4.14.1 Impact on Children
Mothers with older children were concerned about the impact of the pandemic on their child's development and some expressed concerns about the changes in service delivery.
Mothers were worried about restrictions on socialising and baby groups and were concerned that their babies were not developing important social skills. Clients felt that their children were missing experiences that they would have had before the pandemic. Due to increased isolation, mothers felt that regular communication and contacts from family nurses was beneficial as their children could interact with another person.
Many clients expressed that they missed family nurses visiting in person, and some expressed concerns that their child was not receiving the same support because of the restrictions. A couple of clients felt that PPE was a barrier to the family nurse developing a full relationship with their client. In addition, clients felt like changes to the home visiting schedule impacted the frequency of their child's assessments.
"I think it was, like, easier before 'cause she could come in without, you know, wearing a mask and stuff like that. Like, now…if she was to come over, she's got to wear a mask and the whole uniform and stuff so, you know, [my child] isn't, you know, getting to know her face or anything. And they're not really making, like, a bond. Like, before she'd come over and she'd hold her and she'd come and see her properly. But now it's basically all just online and stuff." – [Client, North, enrolled pre-COVID-19]
Clients reported that their child enjoyed a relationship with the family nurse over virtual platforms because family nurses did not have to wear masks when working remotely and so children were able to see their family nurse's face and smile.
"No, when I'm on the video call with [my family nurse], he still gets really excited like he does on face to face. So, like he remembers her face, and he remembers her voice, thus he knows who she is." – [Client, West, enrolled pre-COVID-19]
4.14.2 Ability to Make Changes or Set Goals
All clients regarded their family nurses as supportive, and many described their relationship and support as a process. Clients reported that their conversations with family nurses helped them to understand what they should be doing, and to better understand their feelings. In particular, clients reflected that the time spent talking to family nurses was therapeutic and helped them relieve anxieties and prepare for changes. Clients felt that the time talking to family nurses was an opportunity for them to share their experiences, seek reassurances, and have their feelings verified.
Clients felt that being pregnant and raising a child during a pandemic was a challenging and uncertain experience. Clients reported struggling with restrictions and learning how to adapt to their pregnancy or child's developments in this situation. Clients commented that they felt very well supported by the programme which helped them navigate periods of uncertainty and increased isolation. Clients also expressed that they were able to receive relevant and informative advice at timely stages to understand their child's development and to support their own relationships, goals and circumstances.
In contrast, surveyed family nurses reported that clients' abilities to achieve personal goals and outcomes was negatively impacted by remote programme delivery. Forty-four percent of family nurses felt this had decreased slightly, 39% felt this had decreased significantly and 10% felt it stayed the same, see Figure 7.
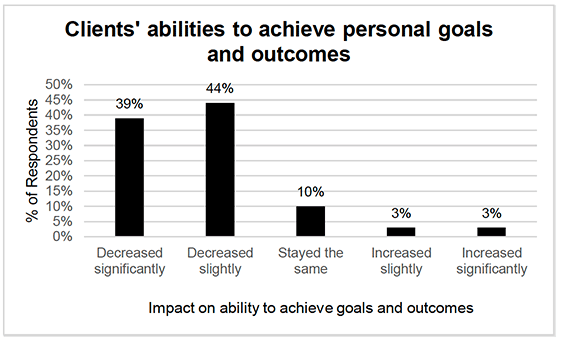
4.15 Future Delivery of FNP
Clients and family nurses were asked about their opinions for the future delivery of FNP based on their experiences of receiving or delivering the programme. Fifty-seven percent of surveyed family nurses agreed (46% somewhat agree and 11% strongly agree) that they would like to continue using telehealth to some extent to deliver FNP in the future; 29% disagreed (15% somewhat disagree and 14% strongly disagree) and 13% neither agreed nor disagreed (see Appendix 2).
When asked to rank most preferable delivery formats, 'in person visiting only', was most preferred by surveyed family nurses (55%). This was followed by 'mixed-mode (face-to-face and telehealth) delivery' (42%) with 'telehealth delivery only' being the least preferred option (77%), see figure 8.
When asked if FNP could be delivered effectively to clients using a multi-faceted (hybrid model) approach without compromising the essence or outcomes of the programme, 68% of family nurses agreed this was possible while 32% disagreed. Of the proportion of nurses who agreed with this statement, most commented that offering a hybrid model of delivery provided convenient options to maintain high levels of engagement for clients with commitments such as work or education. Some nurses also perceived that offering telehealth contacts could actually increase uptake of the programme in some instances where there were challenges in arranging face-to-face contacts with clients.
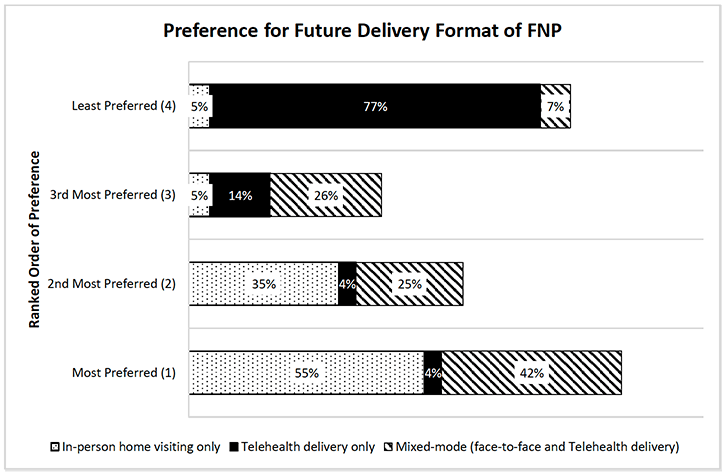
Reflecting on their experiences, some family nurses felt that a large proportion of clients had adapted and engaged well to remote delivery over the course of the pandemic. They commented that most clients were comfortable with technology and familiar with using a range of platforms for communication. Mixed-mode delivery was regarded as an effective option, but family nurses emphasised that the provision of this should first and foremost be dependent on clients' needs and their level of vulnerability.
In addition, some nurses felt a hybrid delivery model was beneficial for improved time management. Family nurses referred to benefits such as reduced work-related travel in between visits or meetings and limiting the time lost due to missed appointments. Improved access to clients living in more rural or remote areas was also perceived as a potential benefit of hybrid-delivery.
"So I'd normally do 50 to 100 miles a day and it was a lot of driving, so that would mean that when I got back from my last visit, maybe it would be nearly five o'clock, but then I'd still have to write up all the visits that I did that day and I didn't really have any time. So I ended up doing at least an hour but probably more like two hours unpaid overtime a day, to be honest, because you just never had time to write everything up that you had to do" – [Family Nurse, East]
Of family nurses who disagreed that FNP could be delivered effectively using a multi-faceted or hybrid approach most frequently commented that they had clients who were uncomfortable or had difficulties engaging via telehealth formats. They also felt strongly that therapeutic relationships were more challenging to establish, requiring more time and effort during remote engagement compared with in-person contact.
In-person communication and interaction were perceived to be more valuable as family nurses felt it was easier to explore client's feeling and interpret body language or other subtle signs indicative of issues of difficulties. In terms of programme delivery, assessments and clinical observations were regarded as more challenging via telehealth. Family nurses also felt that key aspects of the programme, such as PIPE, were considerably more difficult to conduct remotely.
Overall, family nurses were mindful of the challenges and barriers some clients might face during remote engagement. In the survey, 69% of family nurses agreed to some extent (somewhat agree 36% and strongly agree 34%) that the use of telehealth in FNP could lead to the exclusion of clients due to a lack of technological access (Appendix 2); 17% disagree and 13% neither agreed nor disagreed. However, some family nurses also viewed the increased use of telehealth in FNP as an opportunity to teach clients about accessing and engaging with other essential services online.
All clients interviewed wanted the service to return to some degree of face-to-face delivery. Many clients were missing some of the reassurances offered from home visits such as having their baby weighed or having a family nurse see their child's development in-person. Some clients felt that virtual delivery may be beneficial at times, including when managing other responsibilities, for convenience or for impromptu contacts. One client also expressed a desire to occasionally meet their family nurse in-person outside of the home (e.g., outdoor walk or other venue).
"Do you know if COVID wasn't a thing, I would probably always opt to have her come here. I like having her around, she is a very positive person she is, everything is the bright side of life… When she is here, it kind of puts a good mood back into the house because some days it's hard to be bothered during all this, and every time we speak to her we just kind of walk out with a fresh outlook on how things are just now." – [Client, North, enrolled during COVID-19]
"Hopefully, I think more home visits. I'd like to do maybe half and half. Like once it's all over with and died down. Yeah, I wouldn't mind doing half and half. I quite enjoy the video calls on days like when you can't really be bothered having someone in or you just want a quick call, if you've got something on, on those days but yeah, it would be so much nicer just to have her in and just be able to speak to her face-to-face." – [Client, West, enrolled during COVID-19]
A few clients also suggested that the age range of the FNP programme should be expanded to older groups. One client felt raising the age limit of the programme to 22 years would be helpful.
"I think that the age [range of the programme] should be risen a wee bit, because I think it is to do with people from under 16 to 20. I think that maybe up to 22 would probably be good, I feel like to me 22 is still a young mum, I feel like they should have that extra support." – [Client, West, enrolled during COVID-19]
Many of them still thought that telehealth could be used in exceptional circumstances as a way of still keeping clients engaged in the programme, for example: during bad weather conditions, if clients were away, for convenience and for ad hoc calls. Some family nurses thought that telehealth would be good for different stages of the programme, for example during the pregnancy and antenatal phases, or when the client is preoccupied with full-time education or work. Many family nurses felt that it would be good at reducing the time and costs associated with travelling.
While clients and family nurses acknowledged a number of benefits and potential for the use of telehealth in FNP, both groups agreed that the programmes value largely resided in its intensive home visiting format and the ability to build strong face-to-face therapeutic relationships. As such, many felt it would be acceptable for the programme to be delivered as a hybrid model as long as a significant core portion of home visiting and face-to-face contact remained in order to deliver key aspects FNP and to retain the quality and value of the programme for all clients.