Coronavirus (COVID-19) Family Nurse Partnership insights: evaluation report
Report commissioned to explore the experiences of the family nurses and clients in Scotland during the COVID-19 pandemic. This includes initial findings on service delivery, mode of delivery, dosage, materials and resources.
1. Introduction
Family Nurse Partnership (FNP) is a licensed-based home visiting programme that is designed to support young first-time mothers and their children. The FNP programme is delivered by specially trained nurses, in an intensive, one-to-one, home visiting format (Olds, 2006).
The FNP programme was originally developed in the United States through a comprehensive body of research that incorporated three randomised trials (Olds et al., 1986a; Olds et al., 1986b; Kitzman et al., 1997; Olds et al., 2002). Following its inception and implementation in the US, FNP has been further trialled, implemented, and adapted internationally. In the UK, FNP programme has been adopted by three of the four UK nations (excluding Wales) and operates at a national level within each of these systems. FNP was first implemented in Scotland in 2010 and is currently delivered in the 11 mainland Scottish Health Boards. At present, there are also considerations to expand delivery to the three Scottish island Health Boards. Evidence suggests that FNP has integrated well into the Scottish context following its first introduction in 2010 (Scottish Government, 2019).
Evidence shows that young mothers and their babies are at greater risk of experiencing negative health and social outcomes compared with older mothers (Buchanan, 2020). Poorer mental health is also more prevalent amongst young mothers, including increased rates of stress, anxiety, and depression (Raskin et al., 2016). Young mothers and their children are more likely to experience social adversity, stigmatisation and disengagement with education or employment (Wiggins et al., 2005)
FNP is delivered as an intensive home visiting programme, underpinned by a core model, that aims to improve a range of outcomes for first-time teenage mothers and their children. In Scotland, FNP is usually offered to young mothers aged 19 years and under, however this age-range is expanded to some 20 - 24-year-olds with additional vulnerabilities in some Health Board areas. Based on the original model, participants receive regular structured home visits from early pregnancy up until the child's second birthday.
1.1 Theory of Change
Establishing a successful therapeutic relationship between a mother and a family nurse is regarded as a key mechanism to trigger positive changes that can lead to a variety of improved outcomes. The therapeutic relationships formed between mothers' and their family nurses draw on core theoretical principles relating to human ecology, self-efficacy, and attachment. In conjunction with professional training, the support and supervision of family nurses and the availability of tools and resources (Wimbush et al., 2015), therapeutic relationships are harnessed to improve pregnancy and birth-related outcomes, child health and development, parenting practices, health behaviours and the promotion of economic self-sufficiency amongst mothers (Olds, 2003).
Figure 1 shows a previously developed, simplified theory of change model, for FNP delivery in Scotland. A comprehensive programme overview and logic model can be found in Appendix 1.
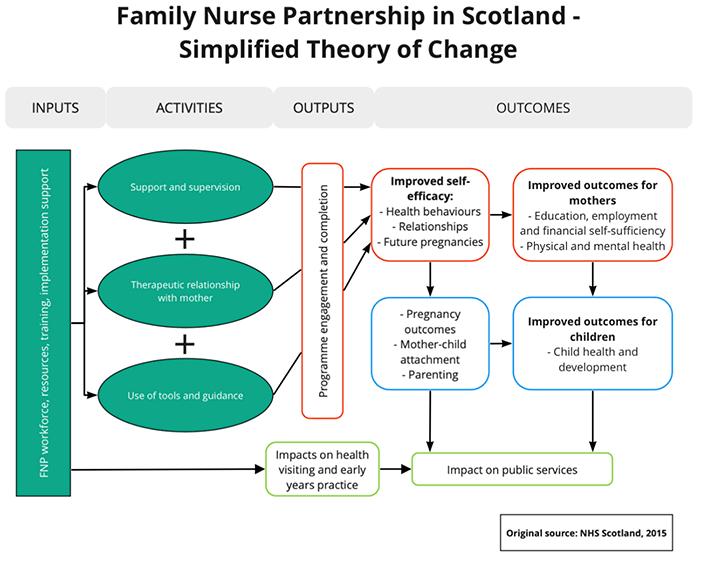
During the early phase of the COVID-19 outbreak, guidance published by the Scottish Government in April 2020 stated that the FNP programme "provides an essential service to the clients and children enrolled on the programme. Families will continue to need the support of FNP and, in fact, will likely need their connection to their FNP nurse more than ever" (Scottish Government, 2021). Subsequently, during the COVID-19 pandemic, disproportionate impacts and adversity have been witnessed throughout the Scottish society. In many cases, this has caused an exacerbation of challenges and inequalities already faced by vulnerable and minority populations (Blundell et al., 2020).
Additionally, a recent UK wide report highlighting the impact of the COVID-19 pandemic and the first UK lockdown on children aged 0-2 years old, identified that while young children were unlikely to be directly affected by COVID-19, they were more susceptible to a spectrum of hidden harms (Reed and Parish, 2020). Some of these hidden harms included:
- Maternal deprivation – deriving from poverty, financial insecurity and income loss and food insecurity which were also associated with factors such as overcrowded living conditions, digital exclusion and an increasing reliance on food banks.
- Social isolation – restrictions preventing children from having opportunities to interact with others and experience different environments that can enhance child development.
- Indirect health risks – potentially occurring as a result of limited healthcare and support services, parental reluctance to access these, delayed identification of concerns and treatment and increased sedentary behaviour.
- Poor parental mental health – potentially impacting pre-birth and child development as well as posing a risk to responsive parenting.
- Traumatic experiences – as a result of overcrowded or altered home environments and a reduction in support services.
- Invisibility to Professionals – a notable concern whereby children are not being seen or are being missed by various professionals.
Hidden harms such as these were thought to be broad, significant and far reaching for families in the UK with the severity of impacts being influenced by a child's socioeconomic background. A recent study identified that young mothers in the UK were less likely to engage with digital health and online support sources, relying instead on trusted interpersonal sources and community-based 'bridges' to provide information and support that more adequately addressed the complexity of their needs (Buchanan, 2020).
1.2 FNP delivery during COVID-19 pandemic
The coronavirus outbreak placed a rapid and enhanced focus on telehealth as healthcare services moved rapidly to implement remote delivery systems in light of infection control measures. A national clinical guidance was produced by the Scottish Government to guide nursing and allied health professionals and community health staff during the COVID-19 pandemic (Scottish Government, 2020). Fundamental changes took place to ensure the provision of continuous care and essential services where possible. In terms of FNP, this involved a predominant shift to home working and remote service delivery using technology such as telephone calls, SMS messaging and video calls via platforms known as Attend Anywhere or NHS Near Me. This enabled clients to maintain contact with family nurses while home visiting was provided for essential circumstances only in order to reduce COVID-19 transmission risks for clients and family nurses. Clinical judgement was exercised by family nurses in relation to home visiting, and when visits were required, there was still a move towards a proportion of visits being conducted remotely. The guidance document provided information in relation to interventions that can be stopped, undertaken in a different way and those that should be continued, whenever possible. Family Nurses exercising the function of the named person on behalf of their Health Board were required to be available and responsive to parents to promote, support and safeguard the wellbeing of children. They were also expected to be mindful to changes of service provision by partner agencies and the potential impact of this on children and their families (Scottish Government, 2020).
Due to the essential role FNP played in response to the COVID-19 pandemic, it is vital to gain a thorough understanding from the perspectives of practitioners and service users, around the delivery of the programme and the use of telehealth in remote delivery in order to better characterise the implications of these changes as well as key consideration for the future delivery of FNP.
1.3 Research Purpose
This evaluation aims to explore how FNP is being delivered during COVID-19 pandemic (following the outbreak in March 2020 and series of lockdowns up until the end of data collection in March 2021 - see further information on this in study setting and context below) in terms of mode of delivery, dosage, materials and resources. It intends to highlight how this largely remote delivery has impacted family nurses, clients and partnership working; the types of challenges hindering the service at the moment, and what lessons can be learned for the future delivery of the programme.
Prior to the evaluation, the research team also conducted a rapid systematic review of telehealth utilisation in the context of home visiting interventions that share similarities with FNP. The findings of the rapid review were used to inform the design of the evaluation. The review is currently being prepared for publication (draft available upon request).