Equally Well: Report of the Ministerial Task Force on Health Inequalities
This is the report of the Ministerial Task Force on Health Inequalities
INTRODUCTION
THE CHALLENGE FACING THE TASK FORCE
"Scotland's health is improving rapidly [but] it is not improving fast enough for the poorest sections of our society. Health inequalities … remain our major challenge."
Annual Report of the Chief Medical Officer: Health in Scotland 2006.
"There's no room for health inequalities in modern day Scotland."
Young Scot consultation for the Task Force
"We have made tackling health inequalities our top priority."
Nicola Sturgeon, Cabinet Secretary for Health and Wellbeing
Setting up the Ministerial Task Force on health inequalities was one of the earliest acts of the current Scottish Government. The aim is to tackle the inequalities in health which prevent Scotland reaching its potential. It is part of achieving the Government's overall purpose: "a more successful country, with opportunities for all of Scotland to flourish, through increasing sustainable economic growth". Increased healthy life expectancy is an important part of this. It must also be achieved in a way that reduces disparities between richer and poorer and narrows the gap between Scotland's best and worst performing regions.
The Task Force's key contribution to achieving these ambitions is to ensure that improvements in the health of the whole population are shared more equally between rich and poor, between other groups in the community at particular risk of poor health and across both urban and rural areas. Reducing such inequalities in health will play a significant part in creating a skilled, resilient population with the sense of wellbeing and control over their own lives, keen to look after their own health and able to participate in the economy and employment opportunities of the future.
The Task Force identified from the outset that few, if any, other countries have succeeded in reducing socioeconomic inequalities in health. We heard about some of the barriers to progress in other countries at the International Summit on Health Improvement and Health Inequalities in Edinburgh in April 2008. It is clear that governments need a shared purpose if they are to address the underlying causes of inequalities in health. They will need courage to face up to some very difficult challenges, such as the linked problems of violence, substance misuse and poor health. Radical action is needed to achieve success.
There is general, internationally-shared consensus that tackling health inequalities requires a cross-government approach and cannot be achieved through health policies and health care systems alone. International approaches so far, however, have not been driven by a clear understanding of why the whole range of public policies matters in determining the health of individuals and communities, nor of how those public policies need to change and develop, in order to alleviate the consequences of unfair and unjust health inequalities.
The Task Force's job has been to take our emerging understanding of the deep-seated causes of health inequalities and turn it into practical action. This involves working across all of national and local government's key responsibilities - for enterprise and skills, children, justice and the physical environment, as well as health and wellbeing.
This document meets the Task Force's commitment to report on what now needs to be done to tackle health inequalities more effectively. We base our recommendations for action on what is already known about what works and we build on previous experience, both positive and negative. But more dynamic approaches are now needed, based on a better understanding of what the Government and others must do. Action is required nationally and locally, to tackle both the causes and consequences of inequalities in health. That is the ambition the Task Force has set itself. That is what its radical recommendations for change can achieve.
KEY HEALTH INEQUALITIES
There are inequalities in the health of people in Scotland which are unfair and unjust, because they are based on social structures and factors such as how much money people have. These inequalities mean that some people are more likely to be ill or have low levels of wellbeing and to die younger than others.
Annex 1 describes some of the key health inequalities facing Scotland today. It identifies some of the most significant challenges facing the Task Force, which have guided its work and determined its priorities. For example:
- In Scotland in 2006, healthy life expectancy at birth was 67.9 years for men and 69 years for women. In the most deprived 15% of areas in Scotland in 2005-06, healthy life expectancy at birth was considerably lower at 57.3 years for men and 59 years for women.
- A higher proportion of babies born to mothers living in the most deprived fifth of the population have a low birth weight than those born to mothers living in the most affluent areas (9% compared to 5% in 2004-05).
- In Scotland in 2006, people who had a low household income, or reported finding it difficult to manage on their household income, had poorer mental wellbeing than those with a high household income or who reported finding it easy to manage on their income.
- There are large and increasing relative inequalities in deaths amongst young adults due to drugs, alcohol, assault and suicide.
- In Scotland in 2006, more than two thirds of the total alcohol-related deaths were in the most deprived two fifths of areas.
- Those living in the most deprived 10% of areas of Scotland have a suicide risk double that of the Scottish average.
- Adult smoking rates increase with increasing deprivation. In Scotland in 2005-06, smoking rates ranged from 11% in the least deprived 10% of areas to 44% in the most deprived 10%.
- Compared with the non-South Asian population, the incidence of heart attacks in Scottish South Asians is 45% higher in men and 80% higher in women.
- Lesbian/gay/bisexual and transgender people experience lower self-esteem and higher rates of mental health problems and these have an impact on health behaviours, including higher reported rates of smoking, alcohol and drug use.
- Just under a quarter (24%) of all individuals in households with at least one disabled adult or disabled child are living in relative low income, compared to 16% of those in households with no disabled adults or disabled children.
Health inequalities are most often described in terms of socioeconomic status and linked to poverty and deprivation. The data available are generally based on the average circumstances of populations living in particular areas rather than the circumstances of individuals. However, not everyone living in areas defined as deprived is disadvantaged. Also, many disadvantaged people do not live in areas of multiple deprivation. It is therefore important to look at health inequalities across the whole population in different ways wherever this is possible.
Health outcomes and health risks may also vary according to people's age, disability, gender, race, religion or belief, sexual orientation and other individual factors. There is information on health inequalities by gender and age, but much less is available in Scotland for health inequalities by ethnicity, disability, sexual orientation, transgender and religion or belief.
Health outcomes such as life expectancy generally improve with socioeconomic status. This is critical to the Task Force's approach, but we are seeking to address all dimensions of health inequalities, not just to improve the health of people in the most deprived areas. Previous Government targets have focused solely on the latter, however.
WHAT CAUSES HEALTH INEQUALITIES?
The Task Force has adopted the widely accepted definition of health as: "a state of complete physical, mental and social wellbeing and not merely the absence of disease or infirmity". (World Health Organization). Health may also include people's ability to lead a socially and economically productive life.
The Task Force has started its work from a social model of health, describing the factors that influence people's health and wellbeing and that determine inequalities.
Dahlgren G, Whitehead M. Policies and strategies to promote social equity in health. Copenhagen: World Health Organization, 1992.
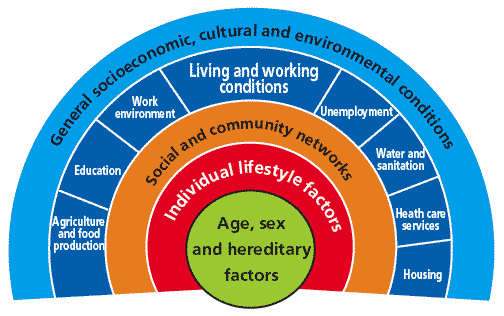
Individual characteristics, such as gender and hereditary factors are largely fixed. As seen above, diversity (age, disability, gender, race, religion or belief, sexual orientation) can lead to unequal health outcomes for people with particular characteristics, compared to the rest of the population. Working outwards from the centre of the diagram, the layers show determinants (causes) of both health and inequalities in health. These include people's personal strengths and vulnerabilities, their lifestyles and health-related behaviours eg smoking, diet, physical activity. Social and community networks can have an important impact. So may economic, social and environmental factors, which play a large part in causing inequalities in people's health.
Sometimes diversity and life circumstances interact and pose increased risks to health. People do not just live in poverty, they may also be a lone parent, may have a long-term disability that affects the work they can do, or live with discrimination which has an impact on their mental health. Gender, and masculinity in particular, contributes to problems of violence, to the reluctance of men to seek help for problems and may make men more likely to resort to alcohol and drugs than to seek help for a mental health problem.
We have based our approach on emerging scientific evidence of how deprivation and other forms of chronic stress lead to poor health, starting at the very early stages of children's lives. Hopelessness and a sense of lack of control increase people's risk of dying from the big killer diseases and of dying early. There is a biological basis for this in the body's inflammatory system. People's responses to stress of all kinds can become "toxic" rather than positive or tolerable. They fail to adapt to their physical and social environments. They may not interact effectively with the world of work, nor with public and other services that should provide support. They age earlier and are more vulnerable to harm from their health-related behaviours such as smoking, as well as from external stress caused by poverty and deprivation or lack of good employment.
Future health inequalities are, to a large extent, determined from a child's earliest years. This is down to biological factors as well as life circumstances generally. Early responses to what is happening shape future physical and psychological functioning. To help the brain develop children need secure and consistent relationships with others, or else they will not thrive, learn, adapt and form good future relationships.
"Early experiences determine whether a child's brain architecture will provide a strong or weak foundation for all future learning, behaviour, and health. The interaction of genes and experience shapes the architecture of the developing brain, and the active agent is the 'serve and return' nature of children's relationships with the important adults in their lives. Policies that support the ability of parents, providers of early care and education, and other community members to interact positively with children in stable and stimulating environments help create a sturdy foundation for later school achievement, economic productivity, and responsible citizenship."
(Center on the Developing Child, Harvard University, USA.)
Some of the Task Force's most important conclusions are therefore about providing the best possible environment for children's earliest years and ending cycles of poverty and poor health passed down from parent to child.
THE TASK FORCE'S APPROACH
In looking at the factors that bring about inequalities in health, the Task Force has examined underlying causes across the whole range of public policy. The remit with which the Task Force began its work in Autumn 2007 was:
- To agree priorities for cross-cutting government activity that will achieve both short and long-term outcomes in reducing the most significant and widening health inequalities in Scotland.
- To build on existing evidence to identify practical measures to reduce health inequalities whose impact can be assessed effectively.
- To influence emerging Government policies and strategies, including the Better Health, Better Care action plan, the early years framework and Curriculum for Excellence.
- To engage the key sectors and organisations that are involved in delivering action on health inequalities, in order to build up their commitment and support.
Members of the Ministerial Task Force on Health Inequalities |
|---|
Shona Robison, Minister for Public Health - Chair Fergus Ewing, Minister for Community Safety Maureen Watt, Minister for Schools and Skills Stewart Maxwell, Minister for Communities and Sport Adam Ingram, Minister for Children and Early Years Jim Mather, Minister for Enterprise, Energy and Tourism Mike Russell, Minister for Environment Dr Harry Burns, Chief Medical Officer for Scotland Professor Carol Tannahill, Director, Glasgow Centre for Population Health Councillor Ronnie McColl, COSLA spokesperson on Health & Wellbeing Ken Corsar, Chair, NHS Lanarkshire Andrew Muirhead, Chief Executive, Lloyds TSB Foundation for Scotland Pam Whittle, Director of Public Health and Wellbeing, Scottish Government |
The Ministerial members of the Task Force have responsibilities covering a wide spectrum across Government. We have worked together on the Task Force in a new way, embodying the Government's unified approach to its overall purpose of sustainable economic growth and the key factors that will make that a reality. Our recommendations make it clear that working together is essential to deliver change.
COSLA and NHSScotland have also taken an active part in the Task Force's thinking. This, too, represents a new way of working, in which local government is an equal partner in developing national policy and agreeing how that can be delivered in practice. Much of the change we need can only be generated locally, through the people in front-line public services. We will recommend how to foster this evolutionary process and learn from both professionals and those they serve about what really works.
The Task Force has been keen to use experience and evidence from previous strategies and inquiries into health inequalities. Annex 2 summarises the most important of these in Scotland, the UK and internationally.
The Task Force also heard helpful evidence from Professor Sally Macintyre (Director, MRC Social and Public Health Sciences Unit, University of Glasgow) about policies and interventions that are likely to help reduce health inequalities.
Box 1: Characteristics of policies more likely to be effective in reducing inequalities in health |
|---|
Structural changes in the environment: (eg installing affordable heating in damp cold houses) Legislative and regulatory controls (eg smoking bans in workplaces) Fiscal policies (eg increase price of tobacco and alcohol products) Income support (eg tax and benefit systems, professional welfare rights advice in health care settings) Reducing price barriers (eg free prescriptions) Improving accessibility of services (eg location and accessibility of primary health care and other core services) Prioritising disadvantaged groups (eg multiply deprived families and communities, the unemployed, fuel poor, rough sleepers and the homeless) Offering intensive support (eg systematic, tailored and intensive approaches involving face to face or group work, home visiting) Starting young (eg pre- and post-natal support and interventions, home visiting in infancy, good quality pre-school day care) |
The Task Force wishes to build its report and recommendations for action on policies and programmes already in place where possible. We have therefore looked to see where current action in Scotland is on the right track. Our recommendations are about what needs to be added to what's already happening.
More work will be needed to turn our recommendations into action. The Task Force therefore recommends that:
1. The Government should produce a practical implementation plan by the end of 2008, setting out how the Task Force's recommendations will be turned into action and who will be responsible, at both national and local levels.
Reducing Scotland's deep-rooted inequalities in health is a long-term task. Significant impact on health outcomes may only be achieved in a generation, or at least on a 10-15 year timescale. The Task Force does, however, want to see improvements in the short to medium-term and recommendations will set out how progress can be assessed within this time frame, as well as in the longer term.
The action that the Task Force recommends in the next three years (2008-09 to 2010-11) can be funded within resources provided by Government, both centrally and locally. Some realignment of current funding may be needed, so that efforts are focused on more effective interventions and targeted on services for people who need them the most.
In the longer term, the Task Force's ambitions for the redesign of public services may require more significant shifts in resources from dealing with consequences of inequalities to prevention and early intervention. Long-term resource implications will be explored locally through the Task Force's learning networks approach. This will inform how public resources can best be deployed in the longer term, in order to contribute to reducing health inequalities.
COMMUNICATION AND ENGAGEMENT
The Task Force itself includes members from local government, NHSScotland, the Third (voluntary) Sector and the research community. At its meetings, the Task Force discussed its work with members of the police, the business community, NHSScotland, local authorities and young people.
The Government-led discussion on Better Health, Better Care in the autumn of 2007 highlighted the importance of inequalities in health and gathered views from a wide range of individuals and groups, including the public, non- NHS organisations and NHS staff and management. These views informed the Task Force's thinking at an early stage.
The Task Force itself has organised three specific consultations:
- We listened to views of young people through Young Scot.
- We heard from a wide Third Sector audience.
- We held a delivery-proofing event, to consult frontline staff and managers from a broad range of sectors and settings about practical aspects of our emerging conclusions.
All of these discussions have been helpful in developing the Task Force's thinking and have provided a welcome reality check on its recommendations. They are reflected in this report. The Task Force is grateful to the many people who have contributed, online, in writing and in person.
THE TASK FORCE'S PRINCIPLES AND PRIORITIES
At the start of its work, the Task Force examined the wide range of inequalities in health in Scotland and the data that are available to describe these. We identified priorities among these health inequalities to guide our assessment of current and future action. The core criteria for deciding priorities were:
- The importance of the inequality in health outcomes.
- The effectiveness of current activity and potential further action.
- The feasibility of delivering such action in Scotland, eg costs, timescale for success, capacity required of delivery organisations.
- Whether we shall be able to measure and monitor success.
In the light of these criteria, the Task Force agreed that it should focus on these priority health outcomes:
- Children's very early years, where inequalities may first arise and influence the rest of people's lives.
- The high economic, social and health burden imposed by mental illness, and the corresponding requirement to improve mental wellbeing.
- The "big killer" diseases: cardiovascular disease and cancer. Some risk factors for these, such as smoking, are strongly linked to deprivation.
- Drug and alcohol problems and links to violence that affect younger men in particular and where inequalities are widening.
Given these priorities and evidence about what drives socioeconomic inequalities in health, the Task Force has agreed key principles to underpin our work. These are:
- Improving the whole range of circumstances and environments that offer opportunities to improve people's life circumstances and hence their health.
- Reducing people's exposure to factors in the physical and social environment that cause stress, are damaging to health and wellbeing, and lead to health inequalities.
- Addressing the inter-generational factors that risk perpetuating Scotland's health inequalities, particularly focusing on supporting the best possible start in life for all children in Scotland.
- Engaging individuals, families and communities most at risk of poor health in services and decisions relevant to their health, and promoting clear ownership of the issues by all involved.
- Delivering health and other services that are both universal and appropriately prioritised to meet the needs of those most at risk of poor health, and that seek to prevent problems arising, as well as addressing them if they do.
- Basing current and future action on the available evidence and adding to that evidence for the future, through introducing new policies and interventions in ways which allow for evaluating progress and success.
- Ensuring that the range of actions we take now will achieve both short and long-term impact and will address foreseeable future challenges.
Throughout its work, the Task Force has considered the importance of diversity and of people's individual characteristics in determining both health and health inequalities. This report and recommendations have undergone formal equality impact assessment. This ensures that we meet statutory requirements and get fully to the heart of the complex factors that determine Scotland's health inequalities. To ensure this continues into the action now to follow, the Task Force recommends that:
2. Those responsible for implementing the Task Force's recommendations should: carry out equality impact assessments on the action they are taking to ensure this is legally compliant; systematically consider the needs of the diversity of the population; ensure action does not adversely affect any part of the population; and consider how they can promote equality.