Equally Well: Report of the Ministerial Task Force on Health Inequalities
This is the report of the Ministerial Task Force on Health Inequalities
ANNEX 1 - KEY HEALTH INEQUALITIES IN SCOTLAND
Life expectancy
In Scotland in 2004-06, male life expectancy in the 10% most deprived areas in Scotland was more than 13.0 years lower than that in the 10% least deprived areas. For females the gap in life expectancy between the most and least deprived was 8.6 years. This inequality gap appears to be widening over time.
Scotland's life expectancy compares unfavourably with the rest of the United Kingdom, and other countries in Europe.
Life expectancy at birth in selected European countries (year = 2004)
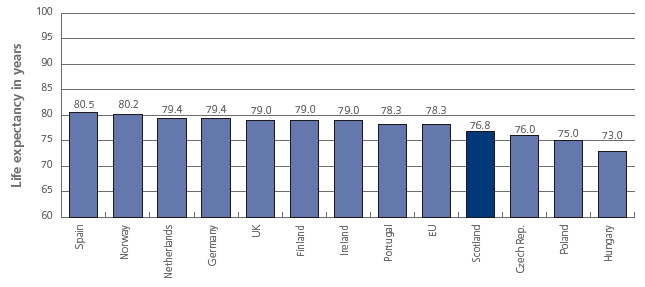
Source: Scotland & European Health for All Database - WHO / Scot PHO
[Based on countries with data for the most recent year available]
Healthy life expectancy
Healthy life expectancy is defined as the number of years a person can expect to live in good health. It is a key measure in the Government's economic strategy, which targets an increase over the period 2007-17.
In Scotland in 2006, healthy life expectancy at birth was 67.9 years for men and 69.0 years for women. In the most deprived 15% of areas in Scotland in 2005-06, healthy life expectancy at birth was considerably lower at 57.3 years for males and 59.0 years for females.
Healthy life expectancy in Scotland overall appears to be steadily increasing for men and fluctuating for women. In the 15% most deprived areas in Scotland, healthy life expectancy is increasing for men (at what appears to be a faster rate than for Scotland overall) and fluctuating for women.
It is notable that the long-term life expectancy trend-line for Scotland shows no real decline in the rate of improvement, over the last 25 years in either gender. On the other hand, the rate of improvement of healthy life expectancy has decreased since the late 1980s. This suggests that for both genders the extra years lived since that time have not been spent in good health.
Because of the way data are gathered and the methodology used to calculate estimates, there is a greater degree of uncertainty around the estimates than there is for life expectancy and trends in HLE should be interpreted with caution.
Life/Healthy life expectancy at birth (Scotland 1980-2005)
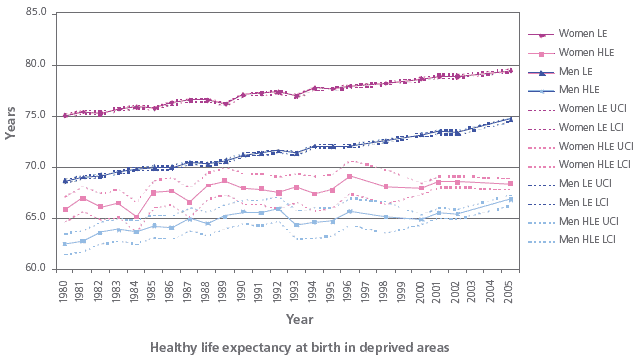
Source: Scot PHO/ ISD
[ LE = Life Expectancy; HLE = Healthy Life Expectancy]
[ UCI / LCI = Upper / Lower Confidence Interval - an indication of the uncertainty around the estimates.]
Mortality
In Scotland in 2006, mortality rates for those aged under 75 years in the 15% most deprived areas in Scotland were 1.8 times higher than those in Scotland overall. The difference between the most deprived 15% and Scotland overall seems to be increasing over time (In 1995 and 2000, under 75 mortality rates in the 15% most deprived areas were 1.5 and 1.6 times higher than in Scotland overall).
Scotland's mortality rates overall are heavily influenced by the rates in the most deprived areas, in particular because of the poor health of people in the West of Scotland.
Mortality in Scottish Local Authority Areas compared with other European Countries
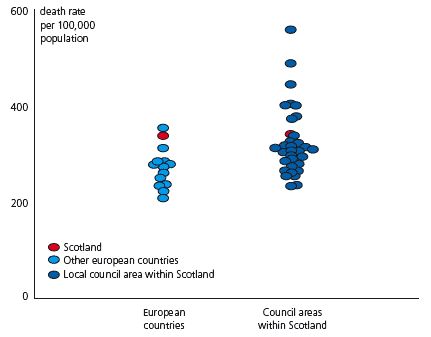
Life expectancy actually appears to be decreasing in some neighbourhoods, for example within East Glasgow and Inverclyde, although these are relatively small populations and trends should be interpreted with caution.
Life expectancy in local areas within Inverclyde (1994-98 and 2001-05)
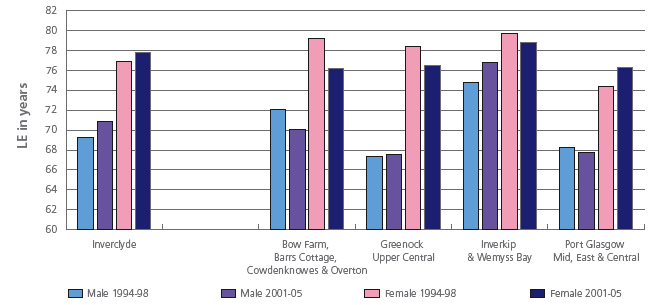
Source: Glasgow Centre For Population Health - Community Profiles
There is also a "Glasgow effect": inequalities between Glasgow and the rest of Scotland are present, regardless of deprivation or social class.
In Scotland, deaths among men aged 15-44 have increased between 1981 and 2001. They have increased among women aged 15-29 between 1991 and 2001. These increases are due to deaths from suicide, violence, chronic liver disease and mental and behavioural disorders due to the misuse of drugs and alcohol. The increases were restricted to deprived areas and this has led to rising inequalities.
Relative inequalities in mortality by cause, men, Scotland 2001
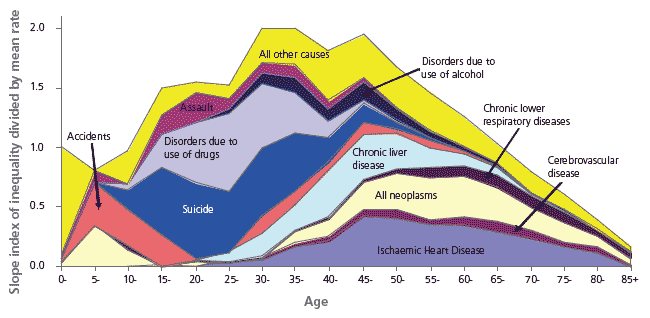
Source: Inequalities in mortality in Scotland 1981-2001. Leyland et al (2007)
Early years
There are inequalities between rich and poor that have a profound influence on the future health of children now being born in Scotland.
There is marked variation by socioeconomic group and by maternal age at birth in the proportion of pregnant women attending antenatal classes: two thirds of those aged under 20 years (the majority of whom live in deprived areas) did not attend any classes while three quarters of those aged 30-39 years went to most or all.
In addition to this, younger mothers and those from less affluent areas are more likely to find it difficult to know who to ask for help regarding concerns over their children's health or behavior and are also less likely to ask for help. Younger mothers appear more suspicious of professional help.
A higher proportion of babies born to mothers living in the most deprived fifth of the population have a low birth weight than those born to mothers living in the most affluent areas (9% compared to 5% in 2004-05). In addition to this, older and younger mothers are more likely to have a low birth weight baby. However, a higher number of babies are born to younger mothers living in more deprived areas than to older mothers living in more affluent areas.
Rates of breastfeeding at 6-8 weeks decrease with increasing deprivation and are more than three times lower in the most deprived fifth of areas than in the least deprived areas (18% compared to 57% in 2006). In addition to this, breastfeeding is related to maternal age: only 12% of younger mothers (under 20 age group) in the most deprived fifth of areas are breastfeeding at the health visitor's first visit. This compares with 73% mothers aged 40+ years in the least deprived fifth of areas at first visit.
Mental health and wellbeing
Poor mental health and wellbeing are associated with an increased likelihood of poor physical health.
In Scotland in 2006, people who had a low household income or reported finding it difficult to manage on their household income had on average lower scores on a scale of mental wellbeing than those with a high household income or who reported finding it easy to manage on their income.
Those living in the most deprived areas of Scotland have a suicide risk double that of the Scottish average. During the period 2002-06, there were 4.6 times as many suicides in the most deprived 10% areas as in the least deprived. These inequalities appear to be increasing over time.
The big killer diseases and associated risk factors
Deprived populations have considerably higher levels of mortality from coronary heart disease ( CHD). This relationship is evident for all ages, but is strongest in those aged under 75 years for whom mortality rates from CHD in the 10% most deprived areas are 3.5 times higher than in the 10% least deprived areas.
Mortality rates from cancer in the most deprived 10% areas are around 1.5 times those in the least deprived 10% areas.
Between 1995 and 2006 the mortality rate amongst those aged under 75 years in the most deprived fifth of the population fell by 16%. The corresponding decrease for those in the most affluent fifth of the population was 20%.
Alcohol-related death rates are increasing in Scotland, whilst they are decreasing in the UK as a whole and in the rest of the European Union. In Scotland in 2006, more than two thirds of the total alcohol-related deaths were in the two most deprived fifths of areas.
People living in the most deprived fifth of areas are around six times more likely to be discharged from a general hospital with an alcohol-related diagnosis than those in the least deprived fifth of areas. This compares with 1.5 times more likely for overall admissions.
Smoking accounts for about 24% of all deaths in Scotland, rising to as much as 34% in some areas. It has been estimated that lifelong smokers die on average about 10 years younger than non-smokers. Smoking also causes a great deal of long-term ill-health due to diseases of the heart, lung and arteries and a long list of cancers and other conditions.
Adult smoking rates increase with increasing deprivation. In Scotland in 2005-06, smoking rates ranged from 11% in the least deprived 10% of areas to 44% in the most deprived 10% of areas.
Prevalence of smoking by area deprivation, Scotland 2005-06
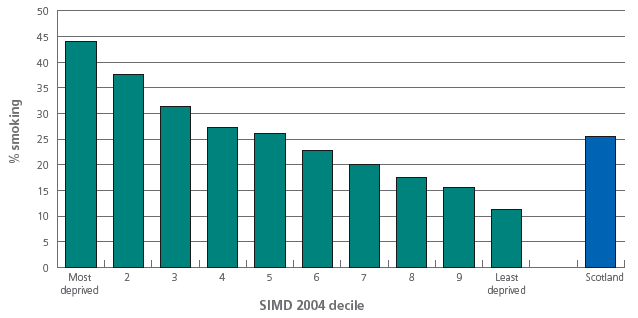
Source: Scottish Household Survey 2005-06
Scottish Index of Multiple Deprivation
http://www.scotland.gov.uk/Topics/Statistics/SIMD/Overview
Other health inequalities
There are important variations in health by ethnic group. For example, Chinese people have better self-reported health and people born in Hong Kong/China but living in Scotland have relatively low mortality rates. Differences in health between different ethnic groups are at least as large as those between rich and poor. Compared with the non-South Asian population, the incidence of heart attacks in Scottish South Asians is 45% higher in men and 80% higher in women. Overall mortality among people living in Scotland but born in India, Pakistan and Bangladesh is lower than among those born in Scotland. On the other hand, mortality from cardiovascular disease is higher among South Asian-born than Scottish-born and the prevalence of diabetes is much higher.
The mental health and wellbeing of some groups is particularly poor:
- Mental health problems affect more women than men. More women experience depressive disorders. However, men are more likely to commit suicide and experience earlier onset of schizophrenia with poorer clinical outcomes than women.
- Teenage mothers suffer from poorer mental health in the first three years after their child's birth than older mothers.
- Lesbian/gay/bisexual and transgender people experience lower self-esteem and higher rates of mental health problems and these have an impact on health behaviours, including higher reported rates of smoking, alcohol and drug use.