Miscarriage care in Scotland: delivery framework
The delivery framework for Miscarriage Care in Scotland outlines a plan for introducing a graded model of miscarriage care. The Framework sets out 34 actions to help NHS Boards prioritise change locally and move to a ‘One Scotland’ approach.
Aims of the Framework
In this Delivery Framework for Miscarriage Care in Scotland, a clear clinical pathway is defined for women who experience miscarriage. This includes access to early pregnancy units, miscarriage management, psychological support and a graded model of care for women who have had one or more miscarriages. The Framework also sets out expectations in relation to patient information and high-quality bereavement care.
The overarching aims are to:
- standardise miscarriage care in a ‘One Scotland’ approach.
- address inequalities in miscarriage care access, support and care including racialised health inequalities.
- ensure that early pregnancy care is equitable so that no women are disadvantaged due to their location, digital connectivity, ethnicity and/or social circumstances.
- ensure that NHS Boards have evidence that information about their early pregnancy service is effectively communicated to women and maternity care services.
- provide trauma-informed, culturally competent and responsive, quality care to women experiencing miscarriage and define a minimum expected standard of care regardless of location.
- ensure that miscarriage is an opportunity to promote access to preconception care planning to optimise next-pregnancy outcomes.
- introduce a structured, graded model of clinical care pathways including investigation and preconception care.
- promote identification of and support for the psychological needs of women/couples experiencing miscarriage.
- support evidence-based miscarriage care and the implementation of clinical audit and research into miscarriage.
- ensure that NHS Boards provide appropriate staff with the time, training, development and support they require to effectively support bereaved women, their partners and families.
The primary objectives of this framework are as follows.
Optimise pre-conception health
- Provide plain language and evidence-based information about miscarriage and ways to optimise health for future pregnancy.
- Facilitate access to advice on healthy eating, achieving normal BMI, tobacco dependency/smoking cessation, alcohol avoidance, and pre-pregnancy micronutrient supplementation (folic acid, vitamin D).
- Signpost to preconception information on NHS inform and ensure equitable access to care and information for disadvantaged or marginalised groups.
- Identify maternal medical conditions that may impact pregnancy (e.g. diabetes, hypertension, heart disease, and epilepsy) and early referral opportunities for specialist management and optimisation.
Graded model of miscarriage care
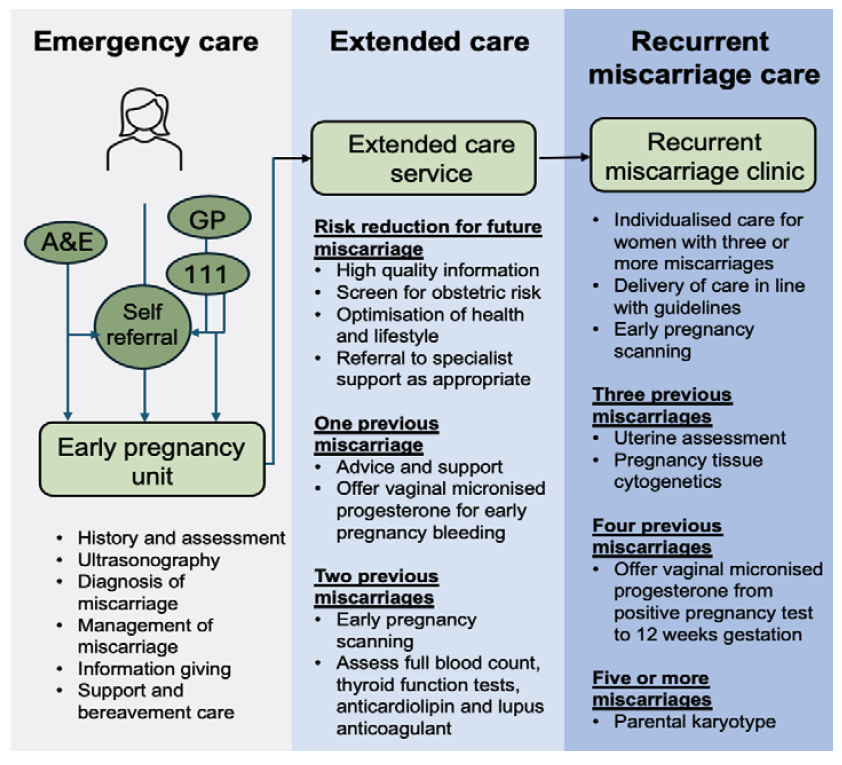
- Establish a tailored, graded model of miscarriage care to standardise increased investigation and management based on the number of previous miscarriages (Figure 1).
- Facilitate multi-disciplinary involvement and access to specialist support such as clinical genetics, fertility care, haematology, and endocrinology as indicated by miscarriage investigations.
- Standardise early pregnancy care and support for women with recurrent miscarriage in a ‘One Scotland’ approach.
- Provide access to early pregnancy reassurance scans in subsequent pregnancies after a second miscarriage.
- Enhance specialist nurse/midwife involvement in patient support and investigation.
- Share information and collaborative research for women/couples with recurrent miscarriage.
Obstetric risk prevention
- Ensure timely referral to appropriate pre-conception specialist care services for optimisation of chronic disease such as referral to hypertension or diabetes clinics.
- Ensure obstetric services have access to detailed past miscarriage history and subsequent investigations to tailor obstetric care.
- Promote increased understanding about the obstetric impact of recurrent miscarriage in community midwives who facilitate triage of care.
Bereavement and psychological support
- Provide support in line with the National Bereavement Care Pathway and ensure that all women/couples are provided with information about where to access bereavement support, including after early miscarriage, before they leave hospital.
- Signpost to patient support groups and online self-help strategies.
- Train staff in sensitive communication (e.g. the Sands midwife training session) and trauma-skilled practice and give them the tools and information to refer on for further psychological support if the woman’s situation is more complex than bereavement support can provide.
- This trauma-skilled practice should recognise not just the psychological impact of pregnancy loss but also the impact that pregnancy loss may have on people who have experienced previous trauma.
- Facilitate timely access to specialist tailored care, where appropriate, for complex psychological needs post miscarriage (e.g. post-traumatic stress, moderate or severe anxiety and moderate or severe depression).
- Remember that additional mental health support following a miscarriage may be required by not only, the woman or couple, but also, others around them who are impacted by the loss.