Coronavirus (COVID-19): Scotland's route map - supporting evidence for moving to Phase 3
This publication provides an assessment of the evidence which informed the decision to move to Phase 3 of Scotland's route map.
WHO criterion 3: Outbreak risks are minimized in high vulnerability settings
WHO criterion 3: Outbreak risks are minimized in high vulnerability settings, such as long-term care facilities (i.e. nursing homes, rehabilitative and mental health centres) and congregate settings.
Long term care facilities can be high risk for severe Covid outbreaks due to their congregate nature and often vulnerable populations. Minimizing risks within these settings has been a core component of our response.
Hospital Associated Infections (HAI)
On 1 July 2020, National Services Scotland published the results of the intensive work to validate the data on the source of infections in hospitals. Previously, we published unvalidated cluster data that was self-reported by Health Boards. Scotland was the first country in the UK to publish both unvalidated cluster data and validated, and hopes that the data helps other countries across the world in their fight against COVID-19.
In spite of the limitations of the unvalidated cluster data, it brought benefits to Scotland's response to the virus by helping health boards to put in appropriate measures to minimise COVID-19 outbreaks, limit the impact to other care services and provide feedback to inform infection prevention and control measures.
Data published more recently is more robust than the previous data because it looks at every single positive case in hospitals and identifies a likely source. This is the most detailed picture of hospital associated infections anywhere in the UK, to date. This data will be published weekly on the Health Protection Scotland website. This data will support our ambition to detect, test, trace, isolate, and treat every case of COVID-19.
On 23 June 2020, the Scottish Government announced additional infection prevention and control (IPC) measures to safeguard patients and staff:
- Extending the use of surgical masks to be worn by all healthcare staff who work within a healthcare setting and may be unable to physically distance from either patients or staff.
- Out-patients, day case attendances and visitors will be asked to wear a facial covering.
- Asymptomatic healthcare staff testing for COVID-19 will be expanded from testing all staff working in an area where there is an outbreak of COVID-19 in a non- COVID ward to include healthcare staff working in specialist oncology wards, long term care of the elderly wards, and long term care wards in mental health facilities.
Furthermore, the Scottish Government recognises the incredible work that Health Boards have undertaken to date on remobilisation plans and on restarting paused services in a safe and clinically prioritised manner. The Scottish Government has emphasised the importance of continually reviewing infection prevention and control measures, and has asked Health Boards to ensure the effectiveness of their remobilisation plans regarding additional cleaning, the built environment (water), physical distancing, COVID/non-COVID areas for patients, and staff movement and rostering. All of these measures will reduce the risk of outbreaks of hospital associated infections to a minimum.
Prisons
The Scottish Prison Service (SPS) published its COVID-19 Route Map and related physical distancing guidance on 25 June at https://www.sps.gov.uk/Corporate/Information/covid19/covid-19-information-hub.aspx. The plan sets out a series of indicative steps through three phases. These steps will be taken to ensure the prison service can move forward while acknowledging the measures that will have to be taken due to the unique environment of prison settings. This remains essential to protect the health and wellbeing of those who live and work in prisons and to prevent the spread of the virus. It is likely that individual prisons will move between the phases at different rates due to the local guidance and different accommodation types. More guidance on key dates will be published by SPS in due course.
New powers have been put in place through the Coronavirus (Scotland) Act 2020 for the early release of a specific class of prisoners held in Scottish prisons, where considered necessary. A controlled early release scheme was undertaken in May, in order to provide the Scottish Prison Service with additional operational capacity. This supported efforts to maintain secure and effective operations within prisons, and to keep prison staff, healthcare workers and prisoners safe - including a greater use of single cell occupancy, and scope to allow prisoners to shield or self-isolate as necessary. The early release process has now been completed. 348 prisoners were released under the scheme between 4 May and 1 June, all of whom were serving sentences of 18 months or less, and were within 90 days of their scheduled release. While provision was made in the regulations, none of the individuals released under this process needed to have their release delayed due to having Covid symptoms.
Operational measures taken by prison and health staff in Scotland continue to be effective in reducing the spread of COVID-19 across the prison estate. As at week ending 26 June, there were no confirmed positive cases of COVID-19 in Scottish prisons and just five individuals self-isolating across five establishments.
Care Homes
Since the beginning of March, we have taken regular and firm action to support care homes across Scotland and protect the wellbeing of those who work and live there. Clinical and practical guidance for care homes was first published on 13 March and was most recently updated on 15 May to reflect developing circumstances. We have established a Care Homes Clinical and Professional Advisory Group led by the Chief Medical Officer (CMO) and CNO to provide up-to-date advice on the response to COVID-19 in the care home sector.
We have tasked Directors of Public Health with providing enhanced clinical leadership to care homes. To supplement this, we have asked all Health Boards and local authorities to establish multidisciplinary clinical and professional oversight teams - including Medical Directors, Nurse Directors and Chief Social Work Officers - to provide scrutiny of care home provision in their areas.
A Care Homes Rapid Action Group has been established with representatives from across the sector to receive regular updates and activate local action where it is required. As well as providing advice and oversight, we have ensured care homes have the means, resources and capacity to implement the guidance.
We have established a Care Homes oversight board and developed a safety huddle tool that enables care homes to identify residents' care needs and associated staffing requirements. The information is shared with local care home support and oversight teams to allow them to plan coordinated support for local care homes. Work is underway to automate the tool and support universal adoption.
From 25 May, we have offered testing to all care home staff regardless of whether they have symptoms or whether there is an ongoing outbreak in their care home. This is achieved through a range of methods including the UK Government Social Care Testing portal, mobile test units, self-test kits, and the employer referral process. Health Boards have been asked to oversee the implementation of this policy. From 10 June, we started to publish data on the number of tests carried out in each Health Board. We are working with Boards to finalise and review their testing plans. The intention is that these will be made publicly available in July.
Other Vulnerable Settings
The package of measures to minimise infection applies to all adult care homes as above. We will strengthen information on other residential settings including adult mental health, learning disability, and forensic services. In addition, we are putting in place comprehensive and location-specific measures across the mental health inpatient estate to minimise the risk of infection. Patient safety is an absolute priority in mental health inpatient settings.
Secure mental health services are part of the NHS and are following all Scottish Government and Public Health Scotland guidance. This includes measures relating to staff and patients as well as the wider community. In addition, the Minister for Mental Health recently wrote to NHS Chief Executives to set out the presumption that all patients being admitted to a secure hospital should have a negative test before admission, unless the patient does not consent to a test, lacks the capacity to consent, or it is in the clinical interests of the person to be moved urgently and then only after a full risk assessment. We continue to liaise with practitioners across the secure mental health estate on a regular basis and are of the view that the measures being taken by secure forensic mental health services are minimising the risks of an outbreak in these settings.
There are a wide variety of approaches to social care which pose different levels of risk for different individuals, for example, buildings-based services working with multiple people - day care and residential respite - pose greater risk than support at home, working 1:1.
We are working with stakeholders to agree a route map guiding the safe continuation, resumption, and response to changing need for people in the community in receipt of social care services. This includes carers and personal assistants employed directly by people who require support. The route map will be driven by a set of overarching and principles, based on human rights, and support the moving through different stages of recovery from the pandemic.
There may be specific concerns around the vulnerability of some user groups, for example the Scientific Advisory Committee has previously expressed caution over an Alzheimer Scotland proposal to re-open their day centres for older people with dementia with adaptations and reduced capacity. The committee is currently considering the wider issue of reopening day care and respite supports, bearing in mind the broad spectrum of ages and user groups that this covers. We expect a response this week but clearly this is a complex issue given the wide variety of supports, services and user groups involved. The committee is aware of the urgency of the issue.
We will use that scientific advice to inform a submission on national actions to support local decisions on re-opening of day care and services, highlighted in phase 1 of the route map.
The COVID-19 Children & Families Collective Leadership Group brings senior leaders together to review data on children, young people and families with vulnerabilities, and to identify issues requiring action as we move through and out of the crisis. The Leadership Group is supported by a range of organisations, to ensure that the experiences of children, young people and families inform this work. A children's residential care group, supported by SG officials including clinical advisors, considers necessary advice to that sector. Alongside continuing liaison with Social Work Scotland and the third sector, this ensures appropriate guidance for social work and social care services for children and families.
We have established a COVID-19 Advisory Sub-Group on Education and Children's Issues to support the work of the COVID-19 Scientific Advisory Group in providing expert advice to support and inform the development of policy and operational guidance for providers of learning, childcare and children's services. Its members include scientific, public health and clinical experts, and academics, as well as experts in education, early learning and children's services.
Regarding children's services at the community level, agreement has been reached with stakeholders on when incremental steps for targeted and general support might commence, inside and outdoors, and with groups and households.
The route map for social care services is particularly complex and as a result services will look different when they reopen, for example changed staff to service users ratios in day service provision which will impact on the unit cost of these services.
Personal Protective Equipment (PPE)
COVID-19 has presented many complex challenges including the provision of PPE at a time when the global supply of PPE has been, and remains, challenging. The Scottish Government, in partnership with the NHS/NSS, Scottish Enterprise, the National Manufacturing Institute Scotland and private companies, has increased both the volume of PPE being manufactured in Scotland and the amount being imported to provide PPE for both immediate and future needs. We are working with partners within Scotland, across the four UK nations and globally to ensure continued supply and distribution.
Adding to well-established arrangements in hospitals, all Health Boards now have a Single Point of Contact (SPOC) to manage local PPE supply and distribution for health and social care. For social care, in both the private and public sectors, the supply of PPE is primarily the responsibility of social care providers themselves. However given the pressure on normal supply chains due to COVID-19, we have committed to providing top-up and emergency provision to ensure staff have what they need. As of 30 June we have, since 1 March, distributed 203 million items of PPE to hospitals, 18 million to primary care, and 76 million to social care.
Other public services such as the police and fire services have their own routes of supply, but they are joined up with the Scottish Government led working group on procurement and supply for non-NHS PPE. This group ensures that different parts of the public sector are not competing with each other over PPE resources. We have also established a process with a third party supplier, making PPE available to purchase for organisations providing essential public services, where they have difficulty accessing supplies through other means.
Organisations that routinely use PPE are generally well placed in terms of demand prediction and supply. As Scotland moves into the next phase of easing lockdown, it is important that all sectors of the economy and society understand their PPE needs and that members of the public understand guidance or requirements on the use of face coverings. The Scottish Government will continue to work with all sectors to achieve this, including supporting the development of guidance and helping to address PPE demand and supply problems where they arise.
Workforce
Steps have been taken to bolster and support the social care workforce. NHS Education Scotland and Scottish Social Services Council (SSSC) have developed a national online recruitment portal to support local efforts to enable those with relevant skills and experience to re-join the workforce and support health and social care services. The national online recruitment portal went live on 29 March and as of 30 June, 154 individuals have been matched with employers with a further 804 people available to employers should they need them. This complements extensive work on the ground to deploy local health and social care staff to support care homes. A national recruitment campaign encouraging people to consider a career in adult social care ran from 27 January until 20 March. We are currently considering a second phase of the campaign.
Testing
Our approach to testing is focussed on saving lives and protecting the vulnerable, rolling out Test and Protect to interrupt chains of transmission in the community, and continuing the vital surveillance work to support our understanding of the disease in Scotland.
Test and Protect - our direct response to criterion 2 - was launched on 28 May. Anyone in Scotland with symptoms of COVID-19 should contact the NHS to arrange to be tested - either online at NHS Inform, or by calling 0800 028 2816.
Since the start of the outbreak we have significantly increased our testing capacity - original capacity was 350 tests a day. We now have active weekday NHS lab capacity of around 10,000 tests a day, and weekend capacity of around 8,000 tests a day. In addition to this we have further capacity through the Glasgow Lighthouse Lab which has capacity to process approximately 20,000 tests a day and may process tests taken from across the UK.
This increased testing capacity has enabled us to continually expand eligibility for testing, and ensure the necessary capacity exists to support Test and Protect. We are continuing to model the capacity required in the system to ensure that it meets demand and to avoid delays.
Health Boards and NHS National Services Scotland (NSS) are working hard to manage demand across different geographies and maximise daily capacity. This includes using real time data to allow variances in capacity and demand to be managed.
NSS is continuing to develop lab partnerships to further build Scotland's testing capacity. We have introduced new reporting processes for Boards which will give us more robust data on testing for key workers and staff, hospital and care home testing, which will help inform local and national planning and allow us to see where there are gaps.
We are also working with NHS Boards and health care partners on restarting health care services and will ensure there is sufficient capacity to manage additional testing. To enable the remobilisation of the NHS, we will regularly test staff working in specialist cancer units, in long-term care of the elderly, and in long-stay mental health wards.
We will also test any health care staff connected to a nosocomial outbreak regardless of symptoms. This testing will begin from 8 July. Discussions are also under way between health boards and clinical teams about testing patients before surgery, alongside all staff involved in a patient's treatment.
We are continuing to work closely with Board Chief Executives and Directors of Public Health to ensure access to resources to increase testing capacity including Mobile Testing Units MTU & UKG Social Care Testing Portal.
Scotland's approach to tracing uses established, tried and tested contact tracing techniques, delivered by health protection professionals in local teams, with support arrangements at national level. All 14 Boards across Scotland have flexible contact tracing arrangements in place. They are all ready to flexibly support any localised increases in community transmission of the virus that may occur as we take our first steps to ease lockdown restrictions.
Data valid as of 5 July:
- 1,506 total index cases, representing 785 individuals.
- 96% of those cases have completed tracing (n=1,452)
- Average contacts made per person traced is 2.72
On 5 July, Public Health Scotland (PHS) began publishing weekly Health Board level figures. The Scottish Government will continue working with PHS to understand what data breakdowns may be available in future to identify more local outbreaks, such as place of contact.
Emergency Legislation
We have brought in new legislative powers to ensure the swiftest intervention if individuals in a care home are being put at risk. The Coronavirus (Scotland) (No. 2) Act 2020 contains powers allowing directions to be made of care home providers; ministers to apply for an emergency intervention order in a care home; and powers to voluntarily purchase a care home or care at home service. These powers can be used where there is an anticipated risk to residents' health, life or wellbeing and allow the highest risk cases to be addressed urgently. These additional measures reflect our commitment to working with all stakeholders to take action, adapt and improve the system as new information comes to light.
Data
Over the week commencing 29 June:
- At least 2,678 individual care home staff, and 302 residents were tested in care homes with a confirmed case of COVID-19.
- At least 30,673 individual care home staff, and 2,002 residents were tested in care homes with no confirmed cases of COVID-19.
This is based on new data reported by NHS Boards and includes staff and residents tested across all routes. Please also note that we are no longer collecting data from Public Health Scotland regarding testing via NHS labs.
Updates are shown on the chart below - updates are published daily at 2 pm here.
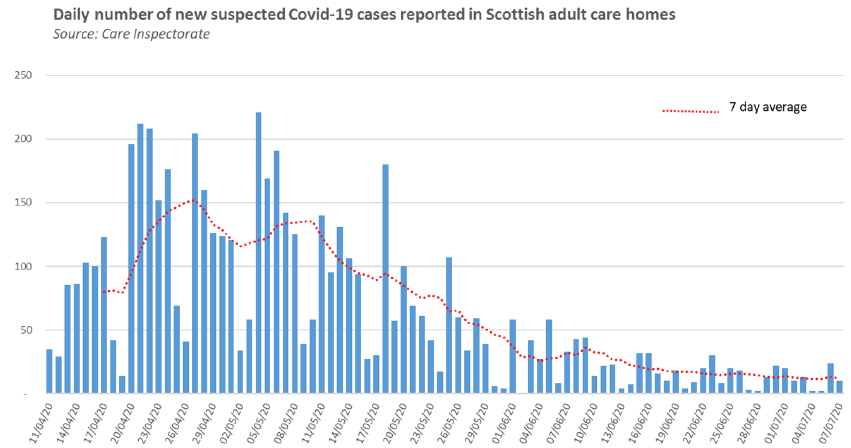
NRS figures for care home deaths
During the last few weeks, there has been a consistent decrease in both the number of care home deaths and the number of homes with an active case of COVID-19.
National Records of Scotland are the official source of COVID-19 deaths. The most recent publication on 8 July shows a steady decrease in the weekly number of deaths in care homes, falling from a peak of 341 at the end of April to 4 deaths from 29 June - 5 July.
As at 9 July, 117 (11%) adult care homes had a current case of suspected COVID-19. From 28 June the Care Inspectorate has revised the definition of care homes with current suspected case to exclude any home that has not notified of a new case of suspected COVID for at least 28 days. For more information about this change, please see the spreadsheet trends in daily data: https://www.gov.scot/publications/coronavirus-covid-19-trends-in-daily-data/.
On the 9 June, the number of adult care homes considered as active, i.e. have a current suspected cases of COVID-19 was 390 (36%). At the last review date, 18 June, this had fallen to 348 (32%). Since the 28 June, the Care Inspectorate has revised the methodology used to classify which care homes are considered active.
Previously, a care home was considered active if the home notified a suspected case and had not subsequently notified the Care Inspectorate that the care home considered itself COVID-19 free. However, subsequent analysis suggested many care homes were potentially failing to notify the Care Inspectorate when they were considered COVID-19 free, or not informing if a suspected case subsequently was found to be negative and therefore there was no COVID-19 in the home. As such, the Care Inspectorate removed any care home that had not notified a new suspected case for 28 days, in line with SAGE guidance on visiting, as well as continuing to remove any care homes notifying that they considered themselves to be COVID-19 free. The first published data using the new methodology was on the 28th June and reported 143 (13%) of adult care homes as active.
Cases of infection in hospitals, prisons and care homes have consistently declined since late April.
Robust monitoring and reporting mechanisms, together with enhanced funding, provision of PPE and bolstering of the workforce in care settings will ensure that any new cases are quickly identified and isolated and the risk of future outbreaks is minimised.
Application of robust testing measures will ensure that infections are contained, and that staff are routinely tested to ensure their health and wellbeing. We will take further action to address nosocomial infection in healthcare settings that is comprehensive and system wide and that delivers sustainably and at pace; and ensure for care homes full compliance with the testing policy in place.
Funding
The Scottish Government has allocated initial funding of over £50 million to health boards to route to integration authorities to strengthen resilience. We have also assured integration authorities that appropriate additional costs arising from COVID-19 will be met by the Scottish Government, aligned to local plans already in place.
In conclusion:
- Cases of infection in hospitals, prisons, care homes and other vulnerable settings have consistently declined since late April.
- Additional, stringent infection prevention and control measures and guidance to safeguard patients and staff in these settings have been established.
- NHS Boards remobilisation plans core aim is to restart paused services in a safe and clinically prioritised manner.
- Well-managed and established plans are in place to meet demand for PPE.
- Application of robust testing measures will ensure that infections are not being moved around the care system, and that staff are routinely tested to ensure their health and wellbeing.
- Early action to address nosocomial infection in healthcare settings that is comprehensive and system wide is being taken.
- Significant national and local funding is in place to strengthen resilience.
Contact
Email: covidexitstrategy@gov.scot