Realising Realistic Medicine: Chief Medical Officer for Scotland annual report 2015-2016
Report on the adoption of the personalised, patient-centred Realistic Medicine approach in Scotland's health services.
Chapter 4: Creating the Conditions to Realise Realistic Medicine
If we are to realise Realistic Medicine, it will require us all, collectively and individually, to consider how we approach care delivery.
It should stimulate reflection about our attitudes and behaviours, in how we interact with the public and colleagues of all professions, and how we learn and share with others. This honest reflection, aided by measures that matter, must motivate us to innovate, improve and change when this is appropriate.
When I published 'Realistic Medicine', I sought feedback from readers on its content. I received it in large numbers from people of different backgrounds, through letters, emails, an online survey and via social media. The volume and usefulness of this was such that my team prepared a short report 14 in which the assessment of this feedback was presented.
"Realistic Medicine - not Nihilistic Medicine."
It was very clear that colleagues across Scotland identified and supported the themes within Realistic Medicine. Time after time, I received stories from people about what practising Realistic Medicine had meant to them and resonated with changes that they had made, or were making, in their own practice. It soon became very clear to me that the report had precipitated powerful conversations and had the potential to be a catalyst for change in medical culture. People felt most energised by the potential to positively influence culture through more shared decision-making, and to reduce harm, waste and variation. Delivery of these linked aims will require a co-ordinated set of actions across all clinical and care professions in Scotland.
The 'Health and Social Care Delivery Plan' was published in December 2016 15 . In it, the Scottish Government emphasised its commitment to Realistic Medicine and to begin work that would help to create the conditions for it to flourish:
- As part of the National Clinical Strategy work-stream a Realistic Medicine team will be established within Scottish Government. This will ensure the correct policy and operational environment at a national level so the numerous examples of local Realistic Medicine practice can thrive.
- The Scottish Health Council and the ALLIANCE will explore with Scottish people what Realistic Medicine means to them during 2017, and how best it can be co-produced.
- The national health literacy plan 'Making it Easy' will support Realistic Medicine by helping everyone in Scotland to have the confidence, knowledge, understanding and skills to live well with any condition they have.
- The consent process for people we care for and support in Scotland will be reviewed by the Scottish Government, General Medical Council and the Academy of Medical Royal Colleges to update advice to clinicians following the Montgomery Supreme Court judgement.
- The Professionalism and Excellence in Medicine Action Plan will be refreshed aligning and prioritising high impact actions that will support clinicians with Realistic Medicine.
- A Scottish Atlas of Variation will be published and a collaborative training programme for clinicians initiated to create better understanding and aid identification of unwarranted variation and promote high value care.
- A single national formulary will be developed to help achieve more equitable, greater value-based care so that the potential population benefit from medicines use can be maximised.
- The principles of Realistic Medicine will be incorporated as a core component of lifelong learning in medical education; in undergraduate and specialty training programmes and through continuing professional development.
Case Study

NHS Education Scotland: A PBSGL in progress
Realistic Medicine as an Educational Tool
Practice-Based Small Group Learning ( PBSGL) groups are a familiar part of learning, particularly in general practice. There are now around 2,250 members in over 350 groups in Scotland including over a third of all Scotland's, practice nurses and pharmacists.
In December 2016 a survey was circulated asking PBSGL members what they would like to see in new modules. 856 people replied, with Realistic Medicine being a priority. Therefore a new module is now in development with NHS Education Scotland: ''Realistic Medicine: building on the challenge in the 2016 Chief Medical Officer's report'
Through my conversations with other health and social care professionals and patient groups during the course of the past year, I have been able to identify many pieces of work demonstrating how Realistic Medicine is already being realised in some parts of Scotland's health and social care services. We already know that doctors use or would wish different treatments for themselves than the people who consult them for the same conditions, that people tend to overestimate the benefits of treatment and can underestimate the risks. In January 2017 the Lown institute published the 'Right Care Series' 16 in 'The Lancet'. These powerful articles discuss overuse and underuse of medical care internationally. The examination conducted by this series of papers is timely and fits closely with the questions asked in 'Realistic Medicine': 'Achieving the right care is both an urgent task and an enormous opportunity'.
These concepts are not new. Philippe Pinel, a renowned French physician, said over 200 years ago:
'It is an art of no little importance to administer medicines properly: but, it is an art of much greater and more difficult acquisition to know when to suspend or altogether omit them.'
Pinel's observation has as much relevance today, as it had two centuries ago; it has been very difficult to achieve this in modern practice but it is encouraging that international interest and debate around this is becoming much more evident. In my view, it is only by working through these issues, openly and transparently, with the public and across the professions, that we will find sustainable, acceptable solutions.
While there is consensus that shared decision-making is an essential part of practicing Realistic Medicine, there is also potential for tension between this and the other aims of Realistic Medicine if the relationship between personal and population health is not understood or clearly articulated in the design and delivery of new models of care. The two approaches can co-exist and are complimentary if viewed through the prism of value-based care that enables a safe, effective and person-centred approach. Here, to re-iterate wise counsel offered earlier by Dr Mulley, it is important to consider 'How do we measure?' and 'How do we manage?' To this, I would also add 'What do we research?'
Worldwide evidence consistently shows that research is a cornerstone of all high performing health systems, leading to better targeted and more personalised treatment and to improved outcomes for people. In Scotland we have a rich tradition of research across all aspects of healthcare, with Scottish academic work having influence all over the globe.
Translation of research into clinical practice has transformed how healthcare is delivered and Realistic Medicine must support the further translation of research into improved care.
We have committed to invest up to £4m in a Precision Medicine Ecosystem that will co-ordinate precision medicine resources and opportunities across Scotland, bring together the findings from individual research projects and improve information sharing in the fight against diseases such as cancer and multiple sclerosis. Scotland also has a vibrant academic primary care research community, supported by the Scottish School of Primary Care and the Scottish Primary Care Research Network. It will be important to continue to provide the highest quality research and evaluation to support the new GP contract and the new models of care. Responsibility for health is devolved to the Scottish Parliament with policy and funding of the NHS research and ethics system lying with the Chief Scientist Office.
Case Study

'Alistair's Story': A story of shared decision-making in treatment at the renal conservative care clinic: https://vimeo.com/181638187
Conservative Care for Renal Disease
Renal services in NHS Lothian have made explicit, supportive discussion about the option of not receiving dialysis for end-stage kidney disease the norm, recognising that this treatment does not always increase life expectancy or quality. This work pre-dates Realistic Medicine by many years, however closely reflects the Realistic Medicine philosophy. A formal programme has been established to support those who choose not to start dialysis or choose to withdraw from dialysis. This includes alternatives such as home visits, holistic care and social work input. People continue to attend clinics and have regular opportunities to discuss future planning. Demand for this 'conservative care' treatment has been high amongst people and commended nationally through healthcare awards programmes. An essential part of this is inclusion of trainees who learn about having these realistic conversations in practice.
Scotland manages its research activity through NHS Research Scotland as a single, unified point of access for both non-commercial and commercial research studies and clinical trials, including recruitment of members of the public. Proactive public involvement in research is crucial to success and we work closely with patient representatives on all aspects of our research support. Over 140,000 people have registered with SHARE (the Scottish Health Research Register) as willing participants in research projects. This streamlined approach makes Scotland a globally attractive place to undertake research and for investment in health science. Over the last three years active study sites have increased by 19.7% (11.8% in 2014-15 alone) and Scotland currently attracts ~10% -13% of Medical Research Council funds.
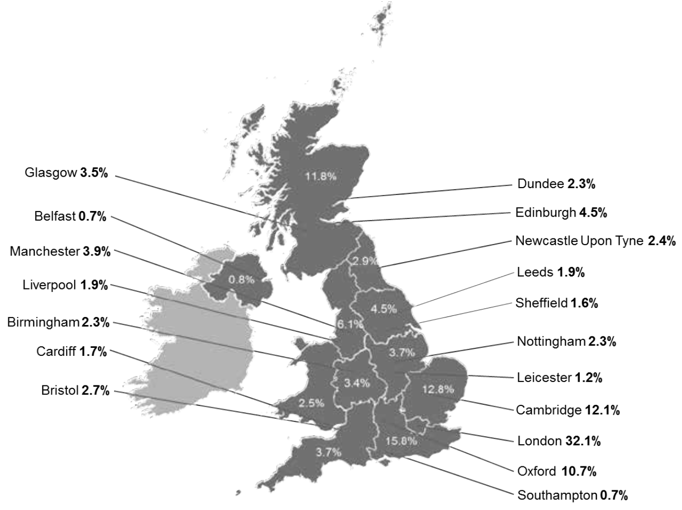
With a population encompassing 8.4% of the UK population, Scotland accounts for 11.8% of UK health research expenditure in Scotland (Figure 1, UKCRC, 2015).
The National Clinical Strategy 17 proposes supporting people to 'fully understand and manage their problems' and providing 'care that is person-centred rather than condition focused, based on long-term relationships between people we care for and support and the relevant clinical team(s)'. Evidence-based decisions retain importance and are discussed in the National Clinical Strategy, however it is acknowledged that evidenced-based medicine and protocols are often based on studies in specific populations. This means that evidence is not always directly transferrable to the context and preferences of individuals, therefore limiting the utility of protocols if applied indiscriminately. This does not however mean we should move away from using evidence-based medicine rather that we should consider 'using guidelines realistically' in future interactions with people. This will require approaches that place a greater prominence on personally meaningful outcomes as one of the primary endpoints when determining the impact of interventions.
Realistic Medicine describes the culture we need in our health service to meet the expectations and challenges of our modern society. Changes in those expectations mean that no matter the setting in which medical decisions are made, clinicians must work in partnership with people to ensure good care.
The landmark decision by the Supreme Court in 2015 in the Montgomery vs. Lanarkshire Health Board 18 case makes it clear that both a personalised approach and shared decision-making are crucial in gaining consent for treatment and thus in delivering modern healthcare. To achieve both we need to develop a better understanding of people's needs as well as the factors influencing how decisions are made and consent provided. Central to this is the principle that the relational factors underpinning conversations about care need to support a partnership based on openness, trust and communication.
Figure 1: Research expenditure in 2014
"The doctor's advisory role cannot be regarded as solely an exercise of medical skill without leaving out of account the patient's entitlement to decide on the risks to her health which she is willing to run (a decision which may be influenced by non-medical considerations). "
The Supreme Court Judgment, Montgomery (Appellant) vs Lanarkshire Health Board (Respondent) (Scotland) March 2015
When we are faced with making decisions about care and treatment we need to have information about issues that matter to us and the opportunity to make sense of this in a way that encourages collaboration as the foundation for decisions and subsequent care and support planning.
It is increasingly expected that people will receive care, support and treatment in environments where they are treated as equals and they must not be influenced by pressure from medical staff, friends or family.
The GMC describes a basic model of partnership between doctor and patient: 'The doctor explains the options to the patient, setting out the potential benefits, risks, burdens and side effects of each option, including the option to have no treatment. The doctor may recommend a particular option which they believe to be best for the patient, but they must not put pressure on the patient to accept their advice. The patient weighs up the potential benefits, risks and burdens of the various options as well as any non-clinical issues that are relevant to them. The patient decides whether to accept any of the options and, if so, which one.' 19
The move away from a traditional, paternalist 'doctor knows best' approach will require more discussion with people about the treatment options available to them (including no treatment) as well as relevant risks and benefits. The Supreme Court's judgment emphasises that discussing risk is not about potentially overwhelming people with information covering every conceivable risk. It is about having a meaningful, clear conversation and coming to a shared decision. In many instances this will take time and perhaps more than one consultation. In response our health and care services will need to adapt. This will be one of the initial areas of further work in support of a co-created vision and plan for change involving regulators, Royal Colleges and people with lived experiences within Scotland's health and social care services. Revised guidance on consent from the General Medical Council will be part of the package of change measures.
Some people who spoke to me after my first report was published expressed anxiety about how spreading some of the existing prototypes and good examples of Realistic Medicine may lead to more complaints and claims. My view is that by approaching care in a more person-centred manner, encouraging more tailored and personally meaningful conversations and shared decisions, this will lead to improved experience and outcomes, which will in turn reduce the number of complaints received (many of which relate to communication and consent) and support the communication behaviours that will also underpin a greater culture of candour and early resolution - both prominent features of the Scottish Government's support of openness and learning.
Providing people with the information they need and in a format they find helpful is crucial. Whilst some will still expect paper-based written information, others, and especially adolescents and young adults, may prefer electronic information presented in various ways and on a variety of platforms. Our health service needs to respond to this and adapt to the changing expectations of the i-generation and generations of the future. The recently launched new arrangements for NHS Inform provide a strong platform to build on.
In this context, Aye Mind ( www.ayemind.com) is an exciting and innovative development that gives us a 'window' on the future. Aye Mind focuses on young people and their mental health. It demonstrates how the internet, social media and mobile technologies can be used together to create valuable resources in a format that users want. We are exploring how the philosophy, skills and knowledge already gained in creating Aye Mind can be applied to other areas of healthcare. The potential for engaging and informing people, their families and carers is enormous.
The availability of electronic communication provides other opportunities to enhance understanding and shared decision-making. Recording consultations and producing presentations on handheld devices are good examples that are being developed by a variety of clinical groups. Both enhance the personalisation of care as well as information sharing. The Scottish Government's commitment to electronic health records will further support people to practice Realistic Medicine and care planning.
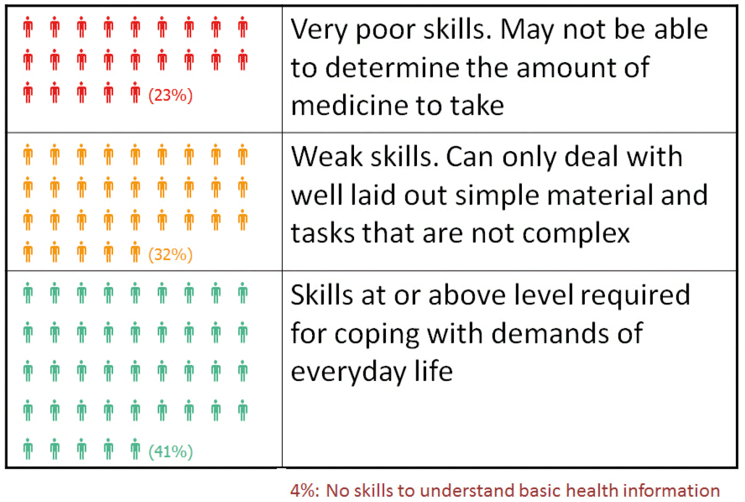
Availability of information in pictorial and graphic formats also helps in circumstances where health literacy is less developed. This is relevant not only to decision-making and consent but more broadly to other aspects of healthcare and in particular, access. Work undertaken by a National Demonstrator Programme in Dundee on health literacy suggests that a significant portion of the adult population in Scotland would benefit from support with health literacy to support understanding - through improved layout of content and understanding of information (such as the amount of medicine to take). We also need to improve our approach to enabling people to seek support where required with health literacy, recognising that understandably people may feel embarrassed about this issue.
'Teach back' allows the evaluation of a person's understanding in their own words, most usefully at the end of a consultation. The demonstration of successful understanding reflects the clinicians ability to explain in a way consistent with a person's health literacy. Examples of questions that can be helpful in starting the process include:
- 'I want to be sure I explained everything clearly. Can you please explain it back to me so I can be sure I did?'
- 'What will you tell your husband/wife/partner about your condition and treatments we discussed? What about the benefits and the risks?'
By asking a person to complete a 'request for treatment' ( RFT), a clinician seeks a record of a person's understanding of care in their own words. At present this is generally in the form of a written document but in the future there is no reason why other electronic media cannot be used or developed. The person is asked a series of relevant questions:
- 'What is wrong with me?'
- 'What treatments are available (including no treatment)?'
- 'What treatment have I decided to have and why?'
- 'What is the benefit I expect and what are the risks?'
Notwithstanding the fact that there are potential improvements that could be made in the person-centredness of the question, particularly given the Scottish Government's commitment to move from a 'What's the matter with you?' to 'What matters to you?' mindset, establishing a person's degree of comfort and engagement with this is important. Encouragement to get help from a member of staff, friend or relative to assist recording the responses may help to improve this and address any literacy concerns. The following can be helpful:
- 'Many people find it easier to speak as they answer these questions and have a friend or relative write down their answers. Would that be best for you and can we help in any way?'
Case Study
Saving Time and Improving The Quality of In-hospital Referrals in NHS Tayside 20
Reducing waste is not simply about reducing physical resources used. Time spent inefficiently can be wasteful, and an example of an improvement project focusing on this is detailed here. This was led by a foundation doctor: often the most important person to identify solutions to a problem is the person being affected by it. Foundation doctors should be supported to take on projects like this.
Making referrals to other hospital specialties is a key duty of the foundation doctor. In Ninewells Hospital, NHS Tayside, doctors noticed that the effectiveness of referrals was limited by contact details not being readily accessible and doctors not knowing what information is relevant to each specialty. The doctors reported significant delays in obtaining contact details from the operator while waiting for the phone to be answered, and found they did not know the specific information needed in each referral. Foundation doctors were phoning the operator between 1 and 7 times per day (median 4 times) and reported it took between 1-7 minutes on for the phone to be answered before being put through to or given contact details for the relevant team.
Foundation doctors reported spending 2-7 minutes finding out what information would be needed for referral, for instance by asking colleagues or nurses.
To increase the information available, a page was set up on the staff intranet called 'Referral Finder'. The page included contact details, guidelines for referral and links to relevant protocols for each specialty. By making this information readily accessible the objective was to increase the speed and quality of referrals.
When surveyed two months after the web page was established, foundation doctors reported a reduction in calls to the operator from baseline and reported achieving more effective referrals, with the majority being able to access Referral Finder in under one minute.
After a second survey 100% agreed that the website saved time and there was a 49.3% reduction in doctors who reported not knowing the specific information needed for a referral.
Calculations were undertaken investigating the cost saving of this intervention in terms of doctor and telephone operator time. An annual saving of £37,047 was made.
Having adequate information improved referrals and resulted in time saved. This simple intervention allowed more time for care and more time for the operators to answer queries from people we care for and support, relatives and other callers.
We are working with a number of services, including the Central Legal Office on RFT and believe this may be particularly suited to situations where discretionary interventions are planned, where a person chooses a form of management that is controversial or involves additional risk, or when a person chooses a non- standard form of management (for instance where a person decides not to have a treatable cancer removed surgically). In these circumstances, RFT tests and records understanding and expectation and may also guide further discussion. Those who have used it, (people we care for and support and clinicians) have found RFT both acceptable and useful.
I know that sometimes people prefer to delegate their decision-making to the clinician caring for them stating, 'you know best doctor'. This can place the clinician in an invidious position and requires some reflection on why the decision is being passed over. Work continues with patient groups to review communication and how this can be used to better ensure that all people who access our health service do so expecting and preparing to be partners in making decisions that affect their lives.
Realistic Measurement that enhances a Systems-Based Approach to Care
Delivery of care in any setting involves making decisions. Improvement results from making more good decisions and fewer bad ones. That can happen intentionally or by chance. Sustaining improvement is harder and requires us to understand which decisions were good and which were bad. To do that we need a clear view of what is happening and the capability to correctly interpret variation in that picture over time.
There is no shortage of ideas for improvement. Converting those 'ideals' into practice is an altogether more difficult challenge. As aspiration and complexity increase, it can outstrip our capability or capacity as individuals, teams or organisations to execute change. We can become overwhelmed. It can seem harder to do the right thing, or more attractive to take the path of least resistance. There is a saturation point beyond which new ideas become 'unrealistic'. Beyond that point lays risk of paradoxical reduction in quality, avoidance of difficult conversations, perverse incentive, empty assurance and low morale.
Dissecting the multiple layers of real world complexity that conspire to cloud our view or undermine the integrity of our response, can help us to understand how we might begin to recalibrate the decisions we make.
Realistic (definition)
adjective:
1. Having or showing a sensible and practical idea of what can be achieved or expected.
2. Representing things in a way that is accurate and true to life.
Measuring is the process of gathering a clear and accurate view of reality. Monitoring is the process of understanding changes in that picture over time. Together they form the basis of the decisions we make each and every day in every context - personal or professional, clinical or operational, individual, local or national. Without them we cannot learn.
The integrity of the decisions we make depends upon the accuracy and completeness of the information available, coupled with our wherewithal to process, analyse and interpret. The information we gather is in turn determined by what we choose to value and the questions we choose to ask.
As clinicians, measuring is the cornerstone of what we do. We establish a thorough account of the presenting complaint, relevant past events, medicines, family and social history. We supplement that information with careful clinical examination and selected baseline investigations, then seek to place our findings within the context of a person's understanding, wishes and expectations. The completeness of the picture we form depends directly upon the questions that we ask and determines our basis for informed, shared decision-making. Gaps in our 'measurement' or understanding compromise those decisions and can undermine the intelligence of our interventions.
Monitoring is what enables timely recognition of deterioration, or confirms response to the interventions we make. Our ability to monitor successfully, intervene effectively and follow up appropriately depends directly upon our understanding of variation over time.
A lack of understanding of that variation is harmful to individuals, teams and organisations on a number of levels. If we don't understand variation we don't know whether we are getting better or worse. If we don't know that, then we don't know what to start or stop doing, what to do more of and what to do less of. We don't know how and where to deploy finite resources. We risk making variation worse by changing the wrong things at the wrong time. We cause waste and harm by intervening when it would have been better to do nothing, or not intervening when it would have been timely to do so. We waste time trying to explain perceived trends when nothing has changed.
We can have all the data in the world but it is meaningless unless we are able to learn from it. Ensuring the information we seek is truly informative and that we are in a position to respond and improve can help us to simplify what is required. It releases space to think, allows focus on what adds value and helps us to move aside that which simply obscures the view. Realistic measurement and monitoring can enhance our decision-making across diverse settings. Alignment through a common approach, informed by our people we care for and support' wishes, fears and expectations, yet cognisant of real world complexity can draw together our collective efforts towards our ambition of realising Realistic Medicine.
Similarly, it is necessary to have realistic measurement within programmes that deliver population health improvement and disease prevention, utilising a public health approach to ensuring effective, consistent and high quality health and social care services. Here, colleagues in public health bring an essential contribution to creating a sharp, data driven focus on identifying unwarranted variation and addressing health inequalities. And all this whilst maintaining the important systems that protect people's health and wellbeing from infections and environmental harms. This must be at the heart of the new public health system we are committed to developing in Scotland.
As we learn more about our progress through better measurement and availability of data, such as the publication of our 'Atlas of Variation', it is essential that the expertise of colleagues from across the professions - public health, clinicians, social care, management and all our supporting infrastructure - pull together with our citizens to ensure high value, high quality care that is consistent with Realistic Medicine.
Having read 'Realising Realistic Medicine', I ask that you consider these questions:
- How would you explain Realistic Medicine to your family or your friends? Would you explain it to the people who you care for differently, and if so, how will you know whether they understand it?
- How will you know when you and your teams are practising Realistic Medicine?
- What opportunities can you create to share and learn from others across the health and social care professions, in Scotland and further afield?
- What will you commit to doing that will help me realise Realistic Medicine in Scotland?
Contact
Email: Catherine Calderwood