Realising Realistic Medicine: Chief Medical Officer for Scotland annual report 2015-2016
Report on the adoption of the personalised, patient-centred Realistic Medicine approach in Scotland's health services.
Chapter 1: Realistic Medicine in an International Context
Across Europe in the 19th century, medical practitioners sought a collective professional identity, driven not only by a desire to be associated with progressive and affirming codes of behaviour and ethics, but by broader influences; societal, cultural, economic and political.
From its beginning in separate countries, the advance of professionalism coalesced throughout Europe, regardless of cultural or political background, strengthened within these states by a growing interest in sharing approaches and thinking through the formation of medical colleges, societies, and periodic journals. This international movement reinforced not only this sense of shared understanding and identity, but eventually precipitated the development of licensing standards expected for doctors too. In Scotland, as medical training became more formalised and also was undertaken in groups, medical students and doctors formed 'cliniques' where learning was shared and supportive networks with strong allegiances were created. Here, we see some of the origins of modern approaches to lifelong learning and professional development.
International learning through communities of shared interest has long been a part of the advancement of science and practice of medicine. As clinicians in Scotland contemplate how the consequences of the referendum on UK membership of the European Union will affect their European networks, there has never been a more important time to restate the importance of continuing to be outward looking in our pursuit of learning and critical appraisal. Though it is perhaps not in our nature to admit it, we should also appreciate that there are occasions when others will learn from us, and that as part of our professional compact with colleagues across the world we must ensure that we create the opportunities, by whatever means, to share learned knowledge and experience.
When 'Realistic Medicine' was published in January 2016, it soon became clear that there was interest in its content from outside Scotland. The social media footprint alone demonstrated that in this digital age, sharing a message was incredibly quick and effective, with responses from almost every continent, and from places as remote as within the Arctic Circle. By January 2017, Realistic Medicine had reached almost ten million Twitter feeds and new networks for learning and collaboration were forming.
The report was written acknowledging and reflecting conversations and questions that were taking place in surgeries and hospitals up and down the country, so it should really be no surprise in this ever shrinking global environment that similar conversations were occurring elsewhere. Indeed, the original report acknowledged this, picking out the Welsh 'Prudent Healthcare' approach as one from which we could learn.
Dr Albert Mulley is Director for Global Healthcare Delivery Science at the Dartmouth Institute for Health Policy and Clinical Practice, and Professor of Medicine at Geisel School of Medicine. His policy paper for The King's Fund, 'Patient Preferences Matter' 1 , was influential in shaping some of the content within 'Realistic Medicine'. He describes 'Realistic Medicine' as a 'bold and important statement from a Chief Medical Officer' and feels that this has enabled an honest and challenging dialogue in Scotland that puts the country at the forefront of an international response to concern about over-reliance and over-provision of high expense, highly technical care as a substitute for getting the basics of health and social care right.
Dr Mulley provides two key challenges: 'How do we choose to measure?' and 'How do we choose to manage?' Both are interlinked, as health systems across the world tend to manage what they measure, but sometimes measure only what is readily accessible. He said, 'We need to learn from variation and deliver what adds value; not just variation in outcomes and cost, but variation in attitudes to risk and patients' preferences - that should be the strategic intent of every health system.'
There is a strong history of sharing between Scotland and Wales, and many similarities between approaches described in 'Realistic Medicine' and 'Prudent Healthcare' 2 . Dr Sally Lewis of Aneurin Bevan University Health Board, Wales, has led on the implementation of Prudent Healthcare. Her appointment as the UK's first Assistant Medical Director for Value-Based Care is a strong statement of commitment by her health board. She agrees with the need to find measures that are relevant to the care we want to provide. She says, 'We must be able to justify our decision-making and also to provide people we care for and support and clinicians with the tools for co-production. One of the essential aspects therefore is to define, measure and analyse true outcome data, including Patient Reported Outcome Measures ( PROMs).'
Dr Mulley is typically expansive and forthcoming in his observations here. Just as there are reductionist clinicians, unyielding in their commitment to science and technology and who evade more subjective or context specific considerations, so also there are reductionist managers with an assembly line approach and exhibiting Taylorism [i] thinking. He contends, the potential hazard is that this thinking is applied at its extreme to guidelines and to pathway development, and becomes a form of reductionism too.
"We fail to measure what really matters in producing value-based care because we've been trained in a reductionist environment where people don't trust measures that aren't highly objective and generalisable, when most things that contribute to value at the level of the individual are highly subjective and context specific, including their preferences. If we don't measure whether services delivered are concordant with people's preferences, we can't measure that value creation".
He suggests an alternative response to this, 'Because the services we deliver are so complex, don't over-specify. Instead, think like the parent or the guardian and create the simple rules that set direction of travel or purpose, boundaries and the basis for reward. The way you make that practical, is to measure what matters; don't over-specify or tread on someone's autonomy, think about the intrinsic motivation of people who have the normative values that got them into that role in the first place. Develop the simple rules and direction setting; what you reward is respect, manifest by listening to what matters to the person. Then you develop a measure that allows clinicians, or the team that they're responsible for, to hold themselves accountable for following those simple rules.'
The CollaboRATE measurement tool 3 was developed by a Dartmouth research group, led by former Welsh GP Glyn Elwyn, whose aim is to develop tools and interventions that improve shared decision-making in healthcare. This fast, simple scale, intended for use with people to assess the quality of the shared decision-making in the clinical encounter from their perspective, shows discriminative validity in the amount of shared decision-making present and correlates with other established measurement tools such as SDM-Q-9 and Perceived Involvement in Care Scale 4 .
Despite the increasing need to provide care to people with complex needs in integrated multi-disciplinary teams, the experience of some remains that their care is fragmented and poorly co-ordinated. The Dartmouth group are also in the process of developing, with public involvement, and testing, a fast, simple patient-reported measure of integration in care delivery, IntegRATE, that allows assessment of the perception of these teams working practices in four domains: information sharing, consistent advice, mutual respect and role clarity 5 . As Realistic Medicine becomes part of the way that we deliver care in Scotland, tools such as these will become very important in providing measures that will allow us to assess our ability to truly involve people in the decisions relating to their care, and ensuring that this is delivered in a joined up, integrated fashion between professionals, communicating and acting with clarity of role and mutual respect. Without this feedback for reflection, how can we assess whether we are truly practising in the style that we intend?
Dr Mulley acknowledges the operational obstacles to achieving this style of healthcare. He suggests that you have to redesign teams, and roles within teams, to level hierarchies and make care less expensive: 'Because it's a step change, rather than a marginal improvement, the other operational piece is you need to know how to organise for innovation, rather than just improvement.
'You can make incremental change, you can improve, by asking everyone to do two jobs, to deliver performance, using current measures, and to improve, and you can do the improvement in 5-10% of your job, and delivery in the rest. But if you're asking people to do new job descriptions, new teams, new ways of communicating it's too much to ask for people to do in 10% of their time; and no-one can do it alone.'
This recognises one of the challenges to realising Realistic Medicine, identified during engagement across Scotland over the last 12 months, that needs to be overcome; the need for time.
Dr Mulley continues, 'My colleague Professor Chris Trimble, from Tuck School of Business, Dartmouth, is an expert on making innovation happen inside established organisations from Tuck School of Business, Dartmouth. He argues that there needs to be a dedicated team, responsible for learning about whether or not the hypothesis that you're using to design a new role or team holds, not managing old performance issues, they're devolved of that responsibility, but they are held accountable for disciplined learning that create the hypothesis for future models and innovation. Without this dedicated team, supported by the CEO, and dealing with the creative tensions that will always exist between performance management and innovation teams, it doesn't happen 6 '.
Not only will this take time, but it also requires a change of mind-set. Dr Lewis has experience of this in Wales: 'As healthcare professionals we tend to do what we always have done and present solutions which are framed as such. Changing the way we think about how to do things is extremely challenging, needs good facilitation and good information.'
Lewis continues, 'There is often a profound lack of understanding about what other healthcare professionals actually do, and the scope of their practice. Getting everyone in the room we have found to be hugely beneficial in building that mutual trust and confidence necessary to redesign.
'In Wales, the term 'minimum appropriate intervention' was discarded as it was not properly understood by those outside health. This really does involve a change in mind-set for many, including the 'gentle art of doing nothing'. We need to understand better why healthcare professionals tend to default to action and often make incorrect assumptions about what people are seeking.'
Realistic Medicine attempts to deal with the dual conundrum of providing care that has greater worth to individuals through proper identification of preferences and shared decision-making, whilst also addressing the need to improve health and wellbeing at a population level. These two aims are not distinct and are closely aligned by the concept of 'value'.
Professor Sir Muir Gray is Director of the Value-based Healthcare Programme at Oxford University, and has provided advice to countries on healthcare systems and value-based care all around the world.
He describes the different ways to think about value.
"Personalised healthcare and population healthcare are two sides of the same coin. The best way to think about this is to think about value.
'The term 'value' in the plural - 'values' - means principles, for example 'this health board values openness'. In the singular, the meaning is economic, and in England NHS Rightcare developed the concept of Triple Value:
- Allocative - determined by how well the assets are distributed to different sub-groups in the population
- Technical - determined by how well resources are used for outcomes for all the people in need in the population. This is much more than efficiency, which is determined by the outcomes and costs for the people seen, but ignores overuse and underuse
- Personal - determined by how well the outcome relates to the values of each individual'.
Sally Lewis agrees: 'There is so much hidden harm from over-intervention, but we are relatively blind to this, instead focusing on harm from missed diagnoses or under-intervention which is of course important as well'.
When he speaks to audiences, Muir Gray uses a couple of slides to try to illustrate this.
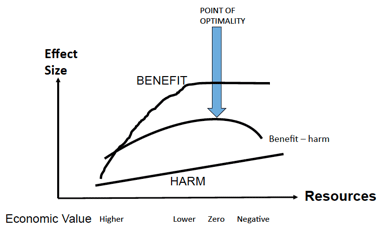
He views this diagram, first created by Avedis Donabedian, as one of the most important in healthcare. It shows how benefits to people increase rapidly with investment of resources, but then level out, even though investment increases, whereas harm rises in a straight line. 'The more work we do,' he says, 'the more harm we cause because procedures we carry out have risks'. Therefore finding the point of optimality is critical.
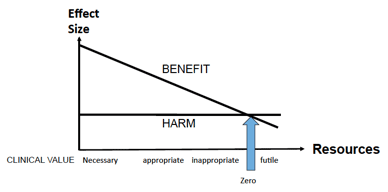
Gray then uses this second figure to show the different relationship from an individual's perspective. He says: 'When there is only enough resource to make interventions available to a few, they are offered to people who have most to gain, and who are more willing to accept risk. However, as investment increases, interventions are offered to people who are less severely affected, therefore the maximum benefit they can expect is less, but the probability and magnitude of harm remains the same.'
The Royal College of General Practitioners ( RCGP) new standing group on over diagnosis and overtreatment is interested in interventions and activity on the right side of this spectrum 7 . McCartney and Treadwell call out the need for clinicians to have readily accessible 'evidence that matters' and is useful to people we care for and support when decisions are being made, such as number needed to treat and relative risk, and this is essential if we are to shift the model of decision-making. Greenhalgh et al suggest that evidence-based medicine should not be viewed as a failed model, but that we need to go back to the movement's founding principles 'to individualize evidence and share decisions through meaningful conversations in the context of a humanistic and professional clinician-patient relationship. 8 '
Dr Lewis, a GP by clinical background, feels building a more personalized approach to care, through co-production and shared decision-making, is perhaps the most important aspects on which to concentrate: 'Evidence-Based Medicine has been great but we have, in my opinion, allowed it to push us into a very formulaic mode of delivering care where one size fits all, rather than using the evidence to inform care. Guidelines have become rules - this has made us very risk averse at a system level. Arguably, the Quality and Outcomes Framework has reduced variation, but it has also reduced patient-centred, holistic care! We need a balance.'
Dr Mulley describes how innovation and this approach to evidence has shaped the care provided by a new primary care practice, Dartmouth Health Connect. When he left Harvard, where he had been Chief of General Medicine at Massachusetts General Hospital ( MGH) for nearly three decades to join Dartmouth, he saw the opportunity to build a care model truly fit for the purpose of engaging people and supporting their role in decision-making and co-production of care. He recruited Rushika Fernandopulle, a former MGH colleague, to design 'from scratch' and implement a care model based on his experience at the Atlanticare Special Care Center 9 .
Rather than recruiting the usual number of clinicians for the target population of service users, he recruited about half that number but also recruited 'coaches', half of whom had no experience in healthcare. Coaches were recruited for their shared life experience with the local population, their empathy and engagement skills, and enthusiasm to make a difference. Rather than a GP spending an hour with a person identified as having the potential to benefit from deeper interviewing, one of these coaches would spend time with them developing a deeper understanding of their preferences and using skilled interview techniques to assess and to motivate.
'Every morning there's a huddle, it could be 10 coaches, two GPs and one nurse in the room, and leadership of the huddle is rotated on a daily basis so 10 out of 13 days it's a coach that's leading the huddle. The purpose of the huddle is to have a conversation that prioritises the urgency of the people we care for and support every day that they're concerned about. So for example, a doctor might think that it's important to focus on Mrs X with her diabetes and improving her diet and exercise; she's gained weight and her A1c is too high, and there's a suspicion that she's still smoking. And the coach says, I couldn't agree with you more, but this isn't the week. She just got bad news about the messy divorce she's going through and she needs some support.'
Professor Gray considers how the understanding of systems-based thinking in healthcare, and its implications has evolved: 'One of the concepts that has emerged, which we didn't think of as students, is one of overuse of healthcare and the potential harm and waste this creates; even if there was lots of money, Realistic Medicine would still be very important. It's only partly stimulated by consideration about the sustainability of delivering a population-based approach to healthcare.
'I think as a nation, you're probably at the forefront of the approach to value-based healthcare, but you can strengthen this further, learning from elsewhere, especially on the population health side'.
In his landmark work with Dartmouth on unwarranted variation, Professor John Wennberg identified that the use of accessible data, to stimulate understanding and change practice was critical. This led to the development of the Dartmouth Atlas of Variation, variants of which are now being used by clinicians in many countries across the world. In England, NHS Rightcare 10 has been developed in partnership with a wide variety of organisations, whilst in New Zealand, the Health Quality and Safety Commission has a visually impressive, easily navigated and public online version 11 .
Case Study

Realistic Medicine workshop with NHS Tayside and Open Change
Realistic Medicine and Service Design
Dundee has recently been named the UK's first UNESCO City of Design. The city has adopted a design values statement which includes the following: 'focusing on social design, redesigning public service and community engagement'. In light of this, NHS Tayside has started the process of realising Realistic Medicine using a service design philosophy. This means involving both healthcare and design professionals in changes to services, always while involving the public.
The 'Health and Social Care Designed in Dundee' alliance has initiated a wide range of events and activities that have aimed to raise awareness of service design within NHS Tayside and teach methods that can use service design to realise Realistic Medicine. A number of these events have been hosted alongside Open Change, a Scotland-based service design agency.
The aim has been to 'begin a conversation about how we can work collaboratively and how we build a trusting and supportive environment that supports a diverse range of clinicians, nursing staff, allied health professionals, people and carers to work together to deliver healthcare, better.'
A workshop on design in healthcare will be held at a future NES conference, led by NHS Tayside representation.
The strength of Atlases is not to provide answers but to provoke questions that lead to better understanding of the reasons for variation, and to help identify variation that is unwarranted. They do not suggest an ideal level, nor do they suggest that high is bad, or average is ideal. This is important, as in this respect they cannot be used as a tool to judge performance of one area against another. Instead, they are intended to facilitate debate and reflection and for this to be used to drive improvement.
'Improving population health, by addressing unwarranted variation, needs a public health approach, but to be owned by the chief executives and chairs of the Boards in Scotland,' says Gray. 'To start, focus on the culture and the systems of a couple of symptoms, a couple of diseases and a couple of characteristics using population based systems thinking. For example look at people with headache, or end of life care, but within each area you need to look at the systems.
"To create a new culture, you need the right glossary, a common language; language creates reality. We need to work towards a common language that is understood. A system is a set of activities with a common set of objectives; a network is a set of organisations that delivers the system; a pathway is a route that people usually follow through the network. We should also identify the words that we should stop using."
As we begin to realise the concepts within Realistic Medicine, it is encouraging and reassuring to know that around the world, just as opinion coalesced around the advent of professionalism in the 19th century, there exists a broad international movement with expert consensus and helpful experience around shared aims; and that these all assert the need to co-create health between practitioners and citizens as an inviolable standard.
Contact
Email: Catherine Calderwood