Becoming Breastfeeding Friendly Scotland: report
Scotland's results and the key recommendations for the continued protection, promotion and support for breastfeeding.
Background
Breastfeeding and the provision of human milk is the most accessible and cost-effective activity available to public health, which is known to prevent a range of infectious and non-communicable diseases (NCDs), specifically gastro-enteritis, childhood obesity, diabetes type 2 and maternal breast cancer[1],[2]. However, global efforts to further improve exclusive breastfeeding rates have had limited success, in part because effective scaling‐up frameworks and roadmaps have not been developed[3]. Breastfeeding rates in Scotland have improved in recent years, with an increase from 44% (2001/2002) to 51% (2017/2018) of babies reportedly receiving 'any breastfeeding' at first health visitor visit at 10-14 days, and the proportion of babies being breastfed at 6-8 weeks rising from 36% of babies (born in 2001/02) to 42% of babies (born in 2017/18)[4] However, the figures remain relatively low and drop off rates high when compared to other countries and recommended targets, with breastfeeding rates lower among women in areas of higher deprivation, exacerbating health inequalities.
BBF
The Becoming Breastfeeding Friendly (BBF) toolkit was developed through highly structured technical and academic collaboration, led by Yale University and has been piloted in Mexico and Ghana. In the short term, it provides an evidence-based tool to guide countries in assessing their breastfeeding status and their readiness to scale up. In the long term, it supports countries to identify the concrete measures they can take to sustainably increase breastfeeding rates, based on data-driven recommendations.
The BBF Gear Model is made up of eight simultaneous conditions which sustain breastfeeding: the gears. This conceptual model illustrates how each gear must be sufficiently mobilised to turn the next, whilst the central Coordination gear gathers and delivers timely feedback.
Figure 1: The BBF Gear
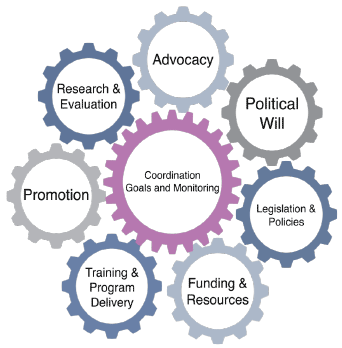
Through the BBF process, country expert committees assess the status of each 'gear' in the BBF Gear Model to deliver a complete picture of the state of action on breastfeeding. This is done by scoring a series of benchmark questions under each gear to determine the extent to which the gear is mobilised[5]. Through assessing these 54 benchmarks within the eight gears, countries are better enabled to decide subsequent actions to be taken after their own assessment.
Led by the University of Kent, breastfeeding experts from a range of statutory and non-statutory organisations across Scotland, Wales and England attended the first GB Engagement Committee in December 2017. Northern Ireland was unable to participate in the BBF process. At the meeting, participants agreed to deliver BBF separately in each country to reflect structural and cultural variation. Since then, the University of Kent has been supporting three locally developed Country Committees of experts in England, Scotland and Wales to carry out the 5 step meeting process. The BBF GB committee has continued in a 'critical friend' role across the three country committees, as appropriate.
BBF in Scotland
The BBF Scotland committee has representation from Scottish Government, diverse NHS organisations, public health, academic and third sector organisations and a royal college. Scottish Government acted as the in-country coordinator and co-chaired the Scottish BBF Committee supported by University of Kent team. They also allocated gear roles according to expertise.
Starting the BBF 5 meeting process in May 2018, the BBF Scotland gear teams used document and (social) media searches, collaborative reviews and interviews to document existing policy, practice and gaps from the previous 12 months in response to each of the 54 benchmarks. Based on this work, the gear teams produced both a final set of scores[6] for each benchmark (from '0' to '3') and 19 initial recommendations in October 2018.
Figure 2: BBF 5 meeting process
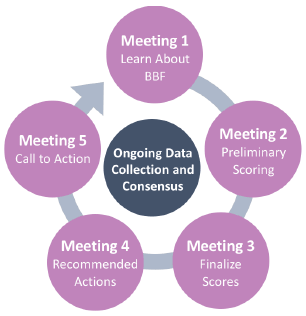
The table below shows the scores for each gear (the total benchmark score for the gear / number of benchmarks in each gear). Some scores, such as elements of the Legislation and Policy gear, reflect the wider UK context where powers are not devolved.
The final, weighted BBF Index score for Scotland, taking all gears into consideration, was 2.4. This represents a strong scaling up environment.
Figure 3: BBF Scotland Gear Scores
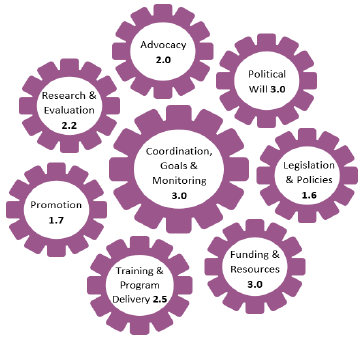
In October 2018, BBF Scotland and BBF GB members assessed these recommendations based on their effectiveness, affordability and feasibility through an online prioritisation survey delivered by the University of Kent. At Meeting 4 in late October 2018, the BBF Scotland committee went on to group the recommendations thematically using the feedback of the prioritisation survey received and facilitated discussion. They also formulated wording under these themes to best reflect the evidence and actions needed to deliver change, and with a view to current developments in the breastfeeding context.
This process produced eight recommendation themes focusing on mothers, babies and families - and what would need to be in place to sustainably improve their experience, care and support, and ensure whole system action on breastfeeding in Scotland. Embedded throughout the recommendations is an emphasis on using evidence and data - including the voices of women and families - to strengthen the whole system, public health approach to breastfeeding. These recommendations also acknowledge that attention must be paid to the Scottish context in terms of geographical and socio-economic variation. For some elements, this may necessitate more targeted or tailored approaches to realise these universal recommendations.
The wording of the themes and accompanying recommendations was further clarified and built into a 'BBF Scotland recommendations and briefing pack' between November 2018 and January 2019, with the draft version circulated to BBF Scotland members for feedback in March 2019. Their feedback has been integrated here in this final version.
This pack contains a set of briefings detailing the eight themes and their accompanying recommendations and actions. The eight themes are:
1. Strengthening and coordinating breastfeeding messages across Scotland
2. Reinforcing political will for breastfeeding among high level decision makers
3. Ensuring consistent, long term government funding commitments underpin Scotland's multi-component breastfeeding strategy
4. Promoting a supportive return to work environment for breastfeeding women through greater awareness and application of maternity, employment and child care provisions
5. Strengthening, enforcing and monitoring legislation in Scotland that supports the International Code of Marketing of Breastmilk Substitutes and subsequent relevant WHA resolutions
6. Developing coordinated, consistent and evidence-based learning outcomes across education and training programmes, based on role-appropriate competency frameworks
7. Ensuring families have equitable access to evidence-based infant feeding support when and how they need it through multi-component, structured models of care
8. Ensuring reliable, comprehensive, explanatory and comparable data on Infant Feeding for monitoring and commissioning purposes
Contact
Email: julie.muir@gov.scot