Annual Report of the Chief Medical Officer 2012 - Population Health and Improvement Science
The Annual Report of the Chief Medical Officer 2012
CHAPTER 6
Communicable Disease
Inequalities play an important role in the epidemiology of infectious diseases, and illness caused by environmental hazards. Globally the main burden of infectious diseases falls on developing countries where infection rates are exacerbated by poverty, environmental degradation, poor sanitation and extreme weather events; and where attempts at prevention and control are hampered by lack of resources and political will.
In Scotland infectious diseases and environmental hazards disproportionately affect marginalised populations and can be linked to upstream determinants such as low socio economic status and migration, which can lead to downstream risk factors such as tobacco, alcohol and drug use, poor living conditions, limited social networks and difficulty in accessing services.
For example:
- in 2012 the main groups at risk of TB were those who consume excess alcohol and migrants/new entrants from countries with a high TB prevalence (9.9% and 56.2% of cases where risk factors and country of birth were recorded)
- around 62% of the 3,490 new cases of HIV diagnosed in 2012 are presumed to have acquired infection abroad with an increase in the numbers of previously infected individuals migrating from areas of high prevalence such as Sub Saharan Africa http://www.hps.scot.nhs.uk/bbvsti/hivandaids.aspx; http://www.documents.hps.scot.nhs.uk/bbvsti/annual-data-tables/2012/hiv-cases-exposure-2012.pdf
- those at highest risk of extreme cold weather events are the elderly and those on low income. In 2011 29% of the Scottish Households lived in fuel poverty, 56% of these being single pensioner households http://www.scotland.gov.uk/Resource/0041/00410389.pdf. Of the 2,000 excess winter deaths over 2012/13, 95.5% occurred in people over 65 years. http://www.gro-scotland.gov.uk/files2/stats/winter-mortality/2012-2013/winter-mortality-2012-13.pdf
However, inequalities are only one of many challenges facing Health Protection. For example, global interconnectedness affects population, and individual, health risks through influences on health related sectors (such as agriculture, water and food safety), increased travel and migration, and, via emerging global health threats such as extreme weather, epidemic and pandemic infections and bioterrorism.
Key Scottish challenges are:
- Gastro intestinal and foodborne infections: The global food industry maintains complex transnational foods chains which are hard to regulate and can contribute to local and international incidents. Of 1,604 food and environmental contamination incidents in the UK in 2012 50% involved food originating from outside the UK http://www.food.gov.uk/multimedia/pdfs/incidents-report-2012.pdf. Out of an estimated total of around one million cases of foodborne disease each year in the UK, Campylobacter is considered to be responsible for around 460,000 cases, 22,000 hospitalisations and 110 deaths, and 80% of infections are estimated to be foodborne.
- Travel and international health: In 2012 there were an estimated 3.6 million journeys made by travellers from Scotland. Imported infections included the first confirmed case of Crimean Congo fever virus to occur in the UK.
- Environmental factors: Environmental factors are estimated to account for 14% of the UK's disease burden and 23% of worldwide deaths.
http://www.who.int/quantifying_ehimpacts/national/countryprofile/unitedkingdom.pdf http://www.who.int/quantifying_ehimpacts/publications/preventingdisease.pdf - Emerging and re-emerging infections: Zoonoses (infectious diseases that can be transmitted from animal to humans), account for 61% of all human infections including established infections such as Campylobacter, Salmonella, Cryptosporidia, VTEC /Ecoli O157; and, potentially emerging problems such as Hepatitis E, Hantavirus, Lyme disease, Avian Influenza and rabies; Antimicrobial resistance such as carbapenemase producing Enterobacteriaceae is recognised by the European Centre for Disease Control as a significant threat to public health in Europe; Epidemic infections - 2012 saw the re-emergence of pertussis infection, plus, the largest outbreak Scotland has ever seen of Legionnaires disease; Pandemic infections - in 2012 a further 32 cases and 20 deaths brought the global total of cases of avian influenza A(H5N1) to 610 with 360 deaths.
- Resilience and emergency preparedness: Scotland needs to predict and respond to established and emerging global health threats posed by infectious diseases, environmental hazards, natural disasters and bioterrorism. Delivery of effective Health Protection services requires development of the workforce, standards, protocols and governance structures to maintain quality, and, preparation for major disruptive challenges involves clear emergency planning. For example, following the very large 2011 outbreak in Germany of the novel infection E Coli 0104:H4, associated with fenugreek sprouts, the threat of an emerging zoonotic or foodborne infection may be considered for the national risk register along with pandemic influenza.
Experience shows that partnership working between statutory agencies, the private sector and voluntary sectors and communities is essential and that is why for complex issues such as the control of TB, Legionnaires' disease and VTEC/E Coli 0157 the Scottish Government supports multiagency action plans and the development of national guidance. Further, since 2008, Health Protection in Scotland has successfully taken a network approach, to develop guidance, share good practice and maintain quality in areas such as immunisation, Hepatitis C, sexual health, infection control and TB.
Communities have an important role in reducing risk from infectious disease and environmental hazards: voluntary sector organisations are key to the successful delivery of care for vulnerable groups such as those who are difficult to reach, difficult to engage with statutory services, and living with conditions such as TB, blood borne viruses and alcohol misuse. Furthermore, individuals can mitigate risk to themselves and others by measures such as seeking advice on travel health, maintaining domestic hygiene, avoiding exposure to tick bites and by vaccination.
Communication is key to partnership working and research shows that simply providing information and expecting individuals, communities and professional groups to change their behaviour is ineffective. Equally, when hazards are not immediately obvious, innovative approaches to distributing information are required. For example 'Know and Respond-Scotland' is a free service, which provides subscribers with text message alerts when air pollution is predicted to be moderate, high or severe. Texts are accompanied by health advice. The service is of particular benefit to those with medical conditions exacerbated by air pollution, such as respiratory or cardiac conditions.
http://www.scottishairquality.co.uk/know-and-respond/about.php
Innovative approaches are also needed to increase linkages between policy and service delivery areas. For example interventions to reduce alcohol consumption, smoking and overcrowding; testing and adopting new food hygiene processing and packaging technologies; the development of policies to provide high quality and accessible services for migrants/new entrants; the extension of immunisation programmes; promotion of best practice in management of petting farms and private water supplies; and closer working of health protection with primary care all have a part to play in reducing the impact of infectious diseases and environmental hazards on vulnerable populations.
What follows is a summary of significant trends, incidents and responses during 2012 that reflect these current challenges to Health Protection in Scotland.
Travel and International Health
During 2012, there were an estimated 3.6 million journeys by travellers from Scotland abroad. The majority of these journeys were to Europe (79%) followed by North America (8%), Asia (3%), Africa (3%) and Central, South America and the Caribbean (2%).2 (Figure 8).
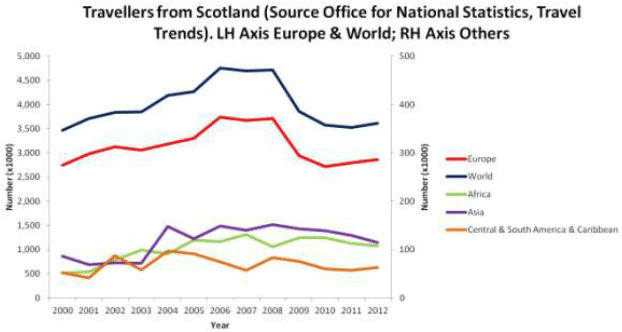
In 2012:
- The most commonly identified infection in persons returning from overseas was travellers' diarrhoea.
- The most common vector-borne virus reported was dengue fever (19 cases). Dengue is transmitted by the day-biting Aedes aegypti species of mosquito, and is present in the Americas, Asia, and Pacific regions and sporadically in Africa. Dengue is an example of a re-emerging infection, with the mosquito vector spreading to more temperate regions and higher altitudes than previously witnessed.
- The first laboratory confirmed case of Crimean Congo Haemorrhagic Fever (CCHF) to have occurred in the UK, was diagnosed in a 38 year old male who had returned to Glasgow following a three week visit to Afghanistan. Although rapidly admitted to the local infectious disease hospital, he unfortunately died despite intensive treatment. No secondary transmission occurred. Areas endemic for CCHF include Africa, the Balkans, the Middle East and Asia. Transmission is through tick bites, or close contact with contaminated animal or human blood or tissues. In this particular case it was likely transmission occurred during animal slaughter. (HPS weekly Report 10 October 2012 Volume 46 No. 2012/41 ISSN 1753-4224 (Online) http://www.documents.hps.scot.nhs.uk/ewr/pdf2012/1241.pdf)
- Schistosoma was the most commonly reported parasite, with 146 positive episodes. Individuals potentially exposed by bathing in freshwater in endemic countries are advised to be screened for this infection on return to Scotland. In response to surveillance data and concerns about pathogen exposures by those participating in school trips HPS has developed guidance specifically for schools (Anon. Travel Health Guidance for Schools. Available at: http://www.fitfortravel.nhs.uk/media/405657/travel%20health%20guidance%20for%20schools%20feb%202013.pdf).
- Malaria reports indicate that of the 1,378 UK malaria episodes recorded, 54 (4%) were imported into Scotland. These 54 episodes represent a decrease of 18% since 2011(66). Of the Scottish episodes in 2012, 67% were associated with P. falciparum and 26% were associated with P. vivax. P. ovale 6% and P. malariae 2% made up the remainder. No deaths from malaria were reported. The quality of the Scottish malaria data requires continuous improvement and there is work underway to increase the proportion of episodes with accompanying data on country of origin and reason for travel. (HPS Weekly Report 24 July 2013 Volume 47 No. 2013/30 ISSN 1753-4224 (Online) http://www.documents.hps.scot.nhs.uk/ewr/pdf2013/1330.pdf )
- TRAVAX (http://www.travax.nhs.uk) is an important resource for health care professionals in Scotland, particularly with regards information on current international disease outbreaks. Outbreaks are published on TRAVAX to highlight increased risk for travellers, and are accompanied by advice and recommendations to help reduce the risk. Scottish public can access similar information on www.fitfortravel.nhs.uk.
Gastrointestinal and foodborne infections
During 2012, case numbers declined for 4 of the 5 pathogens that are responsible for the greatest burden of foodborne gastrointestinal infections (GI) in Scotland (http://www.documents.hps.scot.nhs.uk/giz/annual-report/hps-fsa-joint-annual-report-2012.pdf). Laboratory reports of Campylobacter fell by 1%, Listeria by 21% ,E. coli O157 by 8% and Salmonella by 1%. Reports of Norovirus, however, increased markedly by 75%. Despite their contribution to foodborne GI disease, however, not all outbreaks or cases of these 5 pathogens are due to foodborne transmission (http://www.documents.hps.scot.nhs.uk/ewr/pdf2013/1320.pdf). Of 148 GI outbreaks involving confirmed cases with Campylobacter (1 outbreak), E. coli O157 (6), Salmonella (4) or Norovirus (137), in only one outbreak was foodborne spread identified as the main mode of transmission (an outbreak of Salmonella Newtown involving watermelon, mentioned above). No Listeria outbreaks were identified. Two other foodborne outbreaks involved Scombrotoxin (tuna mayonnaise sandwiches) and an unknown infectious or toxic agent (rice).
A fourth foodborne outbreak highlighted the importance of ready-to-eat food, which has been increasingly identified in gastrointestinal infection outbreaks in recent years. This involved Cryptosporidium cases who were part of a UK-wide outbreak in which bagged salad was the suspected food vehicle.
On the other hand, the importance of environmental exposures (e.g. contact with environments contaminated by farm animal faeces) or waterborne spread, was demonstrated by their being identified as the main mode of transmission in nine outbreaks in 2012 (5 involving E. coli O157, 3 Cryptosporidium, and one Campylobacter and Cryptosporidium).
The above data from Health Protection Scotland routine and enhanced surveillance systems, and from outbreak investigations, nicely illustrates some of the key priorities in future work on GI and foodborne infections. These include the continuing importance of multi-agency work to tackle - in particular - novel and ready-to-eat food vehicles and drinking water quality; and to improve public awareness and management of risks from animal and environmental exposures. These factors - which have all involved large, multi-national outbreaks, and zoonotic transmission - also highlight the overlapping nature of different areas of health protection work. This is exemplified by the multi-agency VTEC/E. coli O157 Action Plan for Scotland 2013-2017 (http://www.scotland.gov.uk/Resource/0043/00437879.pdf) and the currently underway multi-disciplinary revision of guidelines for the investigation of zoonotic disease in Scotland.
Vaccine Preventable Disease
Measles: In 2012, there were 28 cases of laboratory confirmed measles and 23 probable cases, a number well in excess of the maximum of 5 cases a year required for accreditation by the WHO as having eliminated measles. The majority of these cases were in small clusters among partially and un-immunised patients with no evidence of transmission to the wider community. Most cases were seen in the second half of the year coinciding with a widespread measles outbreak in England, Wales and France and, in members of the Traveller Community. A risk assessment by Health Protection Scotland in 2011 identified young people caught up in the controversy generated by the Wakefield paper to be at increased risk of measles transmission. NHS boards now routinely offer vaccine to under-immunised individuals at the teenage DTP vaccine booster appointment.
Pertussis (whooping cough): In 2012, the national outbreak across the UK was the largest seen for over a decade. During 2012, 1,926 laboratory confirmed cases of Bordetella pertussis were reported in Scotland, and 2,034 clinical notifications. This is 16 times more cases than were reported in 2011. The highest morbidity and mortality occurs in infants too young to be protected through routine vaccination, and in 2012, 7.3% of the laboratory confirmed cases were infants <1 year. A temporary programme to protect young infants by offering vaccine to pregnant women began in October 2012 and had an uptake rate of approximately 70% when estimated in January 2013 among women delivering in selected maternity units in Scotland.
Influenza and other Acute Respiratory illnesses: In 2011/12, 14 acute respiratory illness outbreaks (ARI) in closed settings (predominantly in nursing/care homes) were reported which was much higher than the previous year. Most of these outbreaks were confirmed to be due to influenza A, with a small number involving other pathogens such as rhinovirus and para-influenza. One unusual feature of these outbreaks was that they occurred at the end of the usual flu season and continued into early May. Individuals affected were predominantly elderly and in a highly vaccinated population. A relatively small number of deaths were associated with these outbreaks and incidents were managed by NHS Boards in partnership with private sector nursing homes and primary care.
Extension of the immunisation programmes: Following receipt of advice from the Joint Committee on Vaccination and Immunisation (JCVI), the independent expert advisory group, in September 2012, the Scottish Government along with the other UK Administrations announced significant extensions to the existing immunisation programmes to be phased in over a number of years. These include:
- Extending the seasonal flu immunisation programme to all children and young people aged 2-17 years to be implemented over a number of years starting from 2013;
- Changes to the scheduling of the Meningococcal C vaccine, including introducing vaccination for adolescents.
- Adding Rotavirus vaccination to the universal childhood vaccination programme in July 2013; and
- Introducing Herpes Zoster (shingles) vaccine for all those aged 70 years as a routine programme from 2013 with a phased catch-up for those aged 71 and 79 years.
Implementing these new programmes in Scotland will pose a huge challenge over the next few years and colleagues from the Scottish Government will be working closely with Health Protection Scotland and NHS Boards to ensure programmes are implemented with minimal impacts on other vaccination programmes.
Hepatitis C Virus Infection
Considerable achievements have been secured in the nearly 5 years since the launch of Scotland's Hepatitis C Action Plan, now embedded in the Sexual Health and Bloodborne Virus Framework; these include:
- Scaling up of antiviral therapy from approximately 450 initiates per year pre-Action Plan to just over 1,000 during 2012.
- The number of people diagnosed with Hepatitis C is now more than 50% of those estimated to be infected, the rate having been 39% in 2006.
- The spread of the virus among people who inject drugs has declined by two-thirds to around 5% per year following considerable investment to improve injection equipment, and oral substitution therapy uptake.
- Prevalence of Hepatitis C is now on a downward curve and a little bit lower than that observed in 2006 (38,000 to 37,600 chronically infected people); this observation may not appear to be that pronounced but had the plan not been introduced, the numbers of chronically infected people in Scotland would now be well above the 40,000 mark.
Scotland is now in an excellent position to capitalise on therapeutic advances which have seen Hepatitis C "cure" rates increase from 50% to 80% in just over a decade. In the context of the great majority of the country's infected population being vulnerable and marginalised (90% have never injected drugs), Scotland's response to aggressively tackle a problem which, in 2004, was described by Scotland's Health Minister as one of the country's greatest public health challenges, has been hailed as a paradigm of outstanding practice globally. In the recent Report of the Global Commission on Drug Policy "The negative impact of the war on drugs on public health: the hidden Hepatitis C epidemic", the only cited best practice example of a national Hepatitis C Action Plan is that for Scotland. The Report states that "the Hepatitis C Action Plan for Scotland is an impressive example of a national strategy that is successfully focused on people who use drugs". Furthermore, recent presentations of the Plan at the WHO, World Health Assembly, European Parliament and the White House further indicate Scotland's position at the vanguard of action to address a problem estimated to affect 170 million people worldwide.
HIV Infection
In 2012, approximately 4,400 individuals were known to be infected with HIV and living in Scotland. Services have developed over the last 25 years and, the great majority of diagnosed people are now embedded in specialist care, and those eligible receiving antiviral therapy. Over 90% of those administered therapy achieve an optimal response in terms of virus suppression. This is not only good for the individual concerned but is also important in terms of preventing onward transmission of infection through, in particular, sexual intercourse. Nevertheless, challenges still exist; about 25% of all infected persons in Scotland remain undiagnosed, HIV transmission among gay men continues and certain other sexually transmitted infections such as gonorrhoea (1,065 diagnoses in 2008 to 1,904 in 2012) are on the increase. Further effort is required in encouraging those at high risk of infection to be tested. Preventing infection occurring in the first place through safer sex practice is the priority but detection of an infection as soon as possible after acquisition is crucial to prevent spread of virus at a time when circulating levels are extremely high. The Scottish Government's Sexual Health and Bloodborne Virus Framework has thus identified this challenge as a critical one.
Tuberculosis
TB is a global public health problem. In the WHO European Region, TB rates have been decreasing since 2005 but some states in Eastern Europe have much higher rates than those in the European Union (EU)/ European Economic Area (EEA) and multidrug resistant (MDR) TB is emerging as a serious threat with rates increasing 12-13% between 2009 to 2010.
In Scotland, TB rates have been increasing since 2005 and there is a mean increasing 5 year trend from 7.8 per 100,000 in 2008, to 8.8 per 100,000 in 2012. Rates have begun to level off and in 2012 incidence decreased by 9.4% compared to 2011; but it is too early to say that this is the beginning of a downward trend. Of 408 cases reported in 2012, the majority were from Greater Glasgow and Clyde (48.5%), Lothian (20.1%) and Grampian (8.8%) NHS Boards. The main risk factors for infection are being non-UK born and problem alcohol use. However, cases are becoming increasingly complex as individuals may have dual infection with blood borne viruses; they may have underlying chronic conditions such as diabetes or coronary heart disease; they may be employed as care workers; they may share multiple occupancy accommodation; and they may be both internationally and internally mobile.
Progress with recommendations from A TB Action Plan for Scotland 2011 and the ECDC indicators is generally good. National strategies, guidance, quality control and reporting systems are available; patients have access to appropriate diagnostic services, and clinical care, provided by expert and multidisciplinary teams; there are low levels of drug resistance; and public health services contribute to the prevention of transmission. However, there are challenging areas where programmes need to improve. Treatment success rates for pulmonary smear positive cases in 2011 were 75.6% against an 85% target (10% below target); and although differences in measurement and the smaller number in Scotland prevent direct comparison, there are indications that the case fatality rate for TB in Scotland is higher than the UK as a whole (9.9% vs 4.9%).
Key recommendations to address these challenges are:
- Explicit adoption of the ECDC target 'To eliminate, by 2050, TB as a public health problem (incidence <1 per million population)'.
- Clear articulation of a strategic and monitoring framework to manage implementation and measure progress towards achievement of this goal.
- Strengthened linkages to other policy areas such as long term conditions, primary care, health improvement (smoking, alcohol, diet), blood borne viruses, mental health, occupational health, migrant health and the third sector.
- Systematic and standardised approaches to case finding and follow up of TB among new entrants and those at risk due to excess alcohol intake.
- Clear guidance on, and support for the use of, new technologies to identify and follow up cases and clusters of illness, such as Interferon Gamma Release Assay (IGRA) testing, MIRU strain typing cluster analysis and electronic surveillance systems.
- Supportive networking to share good practice, reduce variation and maintain quality in TB services.
Legionnaires' Disease
The annual incidence rate of Legionnaires' disease in Scotland was 6.0 cases per million population in 2011 and 19.6 cases per million in 2012. For 2011 and 2012 the mean case fatality rate was 8.8%; below the European mean case fatality rate which was 10% in 2011: http://www.hps.scot.nhs.uk/resp/wrdetail.aspx?id=55879&wrtype=9.
The 2012 increased incidence rate was a result of an outbreak of Legionnaires' disease, which largely affected a defined population in south-west Edinburgh. It had considerable impact on NHS services during June 2012. Over 1,000 patients were investigated and treated in primary care. Forty-five of the confirmed cases were admitted to acute hospitals in NHS Lothian. Twenty-two patients required admission to Critical Care; 19 were admitted to Intensive Care and 3 to a High Dependency Unit. In total, 92 cases were identified in the outbreak; 56 confirmed cases and 36 probable and possible cases. Four deaths have been reported among formally confirmed cases. The case fatality rate was 7.1% among confirmed cases and 4.3% among all cases.
The outbreak required a multiagency response and mutual aid from other health boards to maintain routine public health functions. Appropriate control measures were applied quickly by NHS staff and Local Authority Environmental Health Officers. Work is continuing to prevent and control any future similar outbreaks including revisions to the Health Protection Network guidance on Legionella outbreaks, development of a common approach to recording complex microbiological and environmental information across agencies and a review by each agency involved of the facilities and resources required for emergency planning and resilience in order to respond rapidly and maintain response to a major outbreak.
Healthcare Associated Infection
Healthcare associated infections (HAI) are increasingly caused by multidrug resistant organisms and represent a continuing threat to patient safety and healthcare delivery and place a significant financial burden on NHS Scotland. There are an estimated 31,502 HAI in NHS Scotland acute care hospitals each year costing £137.1 million and requiring more than 300,000 additional bed days to care for patients with HAI (Health Protection Scotland. Report for the SGHSCD HAI Task Force. The Estimated Cost of Healthcare Associated Infection in NHS Scotland. 2013)
Staphylococcus aureus bacteraemia: During 2012, a total of 1,509 cases of Staphylococcus aureus bacteraemia including methicillin resistant S. aureus (MRSA) were reported, a 5.8% decrease from 2011. This decrease was not statistically significant and represents a change in the decreasing trends observed in recent years. The majority of bacteraemias in 2012 were due to methicillin sensitive S. aureus (MSSA) (1322, 87.6%).
Surgical Site Infection: During 2012, the incidence of surgical site infection (SSI) following hip arthroplasty remained stable compared with previous years. A significant reduction was observed in the incidence of SSI following caesarean section. The majority of caesarean section SSI (84.5%) were identified after the patient had been discharged from hospital. This highlights that the role of post hosptial discharge surveillance is becoming increasingly important for HAI.
Figure 9. Incidence rates of SSI following caesarean section and hip arthroplasty procedures in Scotland, 2008 to 2012
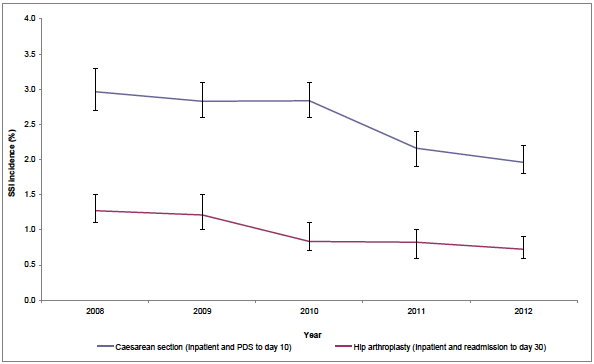
Escherichia coli bacteraemia: The proportion of HAI caused by Escherichia coli, has increased from 3.1% in 2005/6 to 12.1% in 2011 (Health Protection Scotland. Scottish National Point Prevalence Survey of Healthcare Associated Infection and Antimicrobial Prescribing 2011. HPS 2011). E. coli HAI is now a key priority area for infection prevention and control in NHS Scotland. The number of E. coli bacteraemias reported to HPS has increased year on year from 3,486 cases in 2009 to 3,924 in 2012. Preliminary work to characterise the epidemiology of E. coli in Scotland was undertaken in 2012 and will be further developed in 2013.
Clostridium difficile infection: Overall Scottish incidence rates of Clostridium difficile infection (CDI) have showed a steep downward trend in patients aged ≥65 years from 2008 however from 2011 to 2012 the trend levelled. The number of cases decreased 6% from 1,465 in 2011 to 1,382 in 2012. Epidemic ribotypes such as 001, 027 and 106 have reduced significantly while new ribotypes such as 078 have emerged, for reasons that are not currently well understood, and thus CDI should continue to be a focus for infection prevention and control.
HAI Outbreaks: The most commonly reported outbreaks and incidents were caused by Norovirus and there were also several CDI outbreaks reported in 2012. In addition, outbreaks and incidents of a variety of infection types across a range of care settings were reported. These included outbreaks of respiratory tract infection, bloodstream infection, surgical site infection and skin and soft tissue infection caused by a variety of different organisms including Acinetobacter spp., Klebsiella spp., Pseudomonas aeruginosa, Bordetella pertussis, Parainfluenza virus, Group A and Group B streptococci and Panton-Valentine Leukocidin (PVL) positive MRSA. Colonisations with multidrug resistant (MDR) organisms were also reported due to the significant public health concern associated with resistance to key, and in some cases last line, antimicrobials. These included colonisation with vancomycin resistant enterococci (VRE) including an incident/outbreak of linezolid resistant VRE and a carbapenemase producing Enterobacteriaceae.
Key priorities: Whilst there have been significant declines in the rates of Staphylococcus aureus bacteraemia including MRSA, Clostridium difficile infection and surgical site infection following hip arthroplasty surgery in recent years, these reductions were not continued in 2012 highlighting the necessity to refocus priorities to ensure continuing success in reducing HAI. There is a need to focus on HAI which are emerging as a result of changes in patient populations, interventions and technologies that bring new risks to healthcare. A new joint UK strategy for AMR 2013-2018 (agreed between the governments of the 4 UK nations and involving human and animal health agencies), aims to slow the development and spread of antimicrobial resistance, has been published (Department of Health 2013). The new AMR strategy is intended to align the approach to containing antimicrobial resistance in all 4 UK nations and to stimulate collaboration with the veterinary sector. The new Scottish AMR Action Plan will be published in early 2014. Infection prevention and control measures require to be reassessed and targeted in new ways to ensure that NHS Scotland works towards zero preventable HAI, contains AMR and maximises safe care for every patients, every time, everywhere in healthcare.
Antimicrobial Resistance
Antimicrobial resistance in Escherichia coli: The recent increase in burden of disease caused by E. coli bacteraemia does not seem to have been driven by resistant strains as decreases in resistance to key antimicrobials have been observed in this period. This includes an overall decreasing trend in resistance to the cephalosporins antimicrobial class from 10-14% in 2008 to 6-8% in 2012, and in extended spectrum beta-lactamases (ESBL) producers among E. coli (from 7.2% in 2008 to 6.6% in 2012). Resistance to gentamicin remained at 9% in E. coli in 2010-2012 despite increasing use of this agent.
Carbapenemase producing Enterobacteriaceae: Emergence of carbapenemase producing Enterobacteriaceae was recognised as a significant threat to public health in Europe by ECDC in 2010 (European Centre for Disease Prevention and Control (ECDC). Annual Epidemiological Report 2012. Reporting on 2010 surveillance data and 2011 epidemic intelligence data. Stockholm. ECDC 2013). ECDC have reported a higher 'state of spread' in 17 countries and the overall trend for the UK was reported to be increasing from 'sporadic hospital outbreaks' in 2010 to 'regional spread' in 2013. Overall, 85% of countries reported Klebsiella pneumoniae to be the most frequent species to carry carbapenemases (KPC). The UK continues to report more New Delhi Metallo-beta-lactamase-1(NDM)-producers than most other European countries. In Scotland, 25 carbapenemase producers were reported in 2012, bringing the total number of reports to 79 since 2003.
Vancomycin resistant enterococci: Since 2008, the proportion of Enterococcus faecium resistant to vancomycin (from bacteraemias) increased from 16.7% to 27.6% in 2011. In 2012 resistance reduced to 20.4% however this is still higher than the proportion reported for the whole of the UK (13.3%) and is the third highest percentage reported in Europe by ECDC. Ireland has the highest proportion in Europe (44.0%). In 2012 a strategy was developed to collect information on the epidemiology of vancomycin resistant enterococci in Scottish hospitals and molecular investigations will be conducted in order to target preventative measures.
Conclusions
Health Protection teams provide a world class service in Scotland. However, infectious diseases and environmental hazards still pose a considerable threat to the population and there is no room for complacency. Key areas for development over the coming years are:
- To become technologically smarter particularly around surveillance (e.g. TB, Anti-Microbial Resistance), communication of risk (e.g. Travel, Lyme disease, Legionella) and in linking case and outbreak management to national guidance and quality assurance. This will involve close integration of human and animal information sources and expertise, within the broader context of trade, travel and the environment.
- To develop and implement national programmes and multiagency action plans such as the extended immunisation programme, the Sexual Health and Blood Borne Virus Framework, A TB Action Plan for Scotland, the VTEC/E Coli 0157 Action Plan, and the Scottish Antimicrobial Action Plan.
- To maintain the capacity and resilience to deliver quality assured services for Scotland that are flexible enough to deal with all kinds of disruptive challenges, from infectious disease outbreaks to terrorist attacks or flooding. This requires the development of innovative approaches which promote priority setting, linkages between policy areas, effective governance, quality assurance and collaborative working between statutory agencies, the private sector, the voluntary sector and communities.
Contact
Email: Diane Dempster