Annual Report of the Chief Medical Officer 2012 - Population Health and Improvement Science
The Annual Report of the Chief Medical Officer 2012
CHAPTER 3
The Early Years Collaborative and Transforming Childhood
One year ago, the Early Years Collaborative (EYC) first met. Teams from across all Community Planning Partnerships began the process of agreeing aims, timescales in which they might be delivered and ideas for changes that might deliver those agreed aims. Three main aims have been agreed:
- To ensure that women experience positive pregnancies which result in the birth of more healthy babies as evidenced by a reduction of 15% in the rates of stillbirths (from 4.9 per 1,000 births in 2010 to 4.3 per 1,000 births in 2015) and infant mortality (from 3.7 per 1,000 live births in 2010 to 3.1 per 1,000 live births in 2015). This is the aim of workstream 1.
- To ensure that 85% of all children within each Community Planning Partnership have reached all of the expected developmental milestones at the time of the child's 27-30 month child health review, by end-2016. This aim is dealt with in workstream 2.
- To ensure that 90% of all children within each Community Planning Partnership have reached all of the expected developmental milestones at the time the child starts primary school, by end-2017. This is workstream 3.
Infant mortality in Scotland
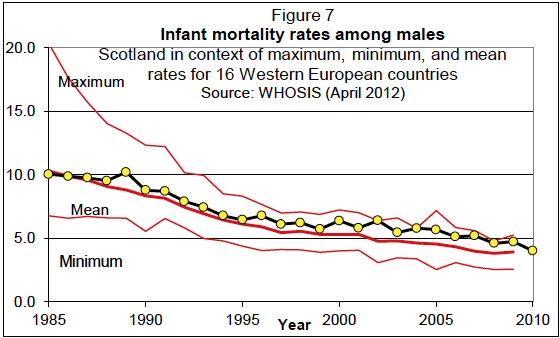
The aim of the EYC to reduce infant mortality rate by 15% is a real and significant challenge. The past decades have seen significant reductions in infant mortality across European countries. The Glasgow Centre for Population Health has shown that, in the 1950s, there were large differences between countries in terms of infant mortality rate [5] There were very high rates in Southern Europe, and Portugal in particular. However, over the last 60 years infant mortality rates have decreased consistently in all countries and the differences between countries are now small: in 2008, minimum and maximum rates ranged between 2.5 and 4.8 per 1000/year for boys and 2.1 and 4.8 per 1000/year for girls. Infant mortality rates in Scandinavian countries, with the exception of female infant mortality in Denmark in recent years, have been consistently among the lowest in Western Europe. In 2012, infant mortality in Scotland was 3.7.
Figure 7 shows how male infant mortality in 16 western European countries has converged. However, since the 1990s, male infant mortality has gradually increased above the mean and Scotland's ranking relative to other countries in Europe has deteriorated for both sexes. Achieving a 15% reduction will require a major effort across all of Scotland. The methods introduced by the Early Years Collaborative offer the best hope of attaining this goal.
Progress so far
Over the course of the year, teams from each Community Planning Partnership have developed ideas for change and are now undertaking small scale tests of change in each of the work stream areas. As expected, common themes are now emerging from this testing through discussions with local teams and the shared learning sessions in which CPPs tell each other of the results of their testing.
The pattern of testing carried out has looked for small, incremental improvements in drivers of wellbeing. However, as the Collaborative enters its second year, there is an opportunity to review the information gathered so far and consider how to focus improvement efforts on the key changes across the work streams that have the greatest potential for impact on the lives of children and their families.
Accelerating progress
Instead of making small incremental changes and testing them in PDSA cycles, Breakthrough Improvement [6] often entails introducing a few big high impact interventions, with potentially a high cost and limited staff engagement, but rapid improvement can be achieved. Incremental Improvement casts its net much wider, seeks small gains, engages the broad range of the improvement community and can also result in improvement. It has been suggested that combining these approaches increases the improvement that can be achieved exponentially.
The approach taken to date across the EYC has been to make small improvements incrementally. There is early evidence of improvement across a range of child and family services. These experiences have been shared through the network in various ways and also by use of an Extranet which allows teams to share experience electronically.
The themes emerging from the work match well with the evidence base that supports the underpinning theory for better child development but there is scope to learn more from colleagues testing approaches in different localities and the time now seems right to consider concentrating improvement efforts on higher impact interventions and to share that learning across the country using data for improvement.
It is likely that the EYC will accelerate the pace of its improvement work by identifying and focusing some improvement effort to develop high impact interventions which we are calling 'Key Changes'.
So what are the 'Key Changes'?
Essentially these are those highly significant changes that really make a difference. This WHO/IHI description of the Breakthrough approach sums it up from a healthcare perspective but the principles are the same for population change:
"All too often in health care, evidence-based interventions that have been shown to produce superior results in certain locations do not spread to other sites. Therefore, practitioners of health care improvement have broadened their focus to not only develop superior models of care but also to take such models to larger scale by focusing on intentional spread, to more rapidly meet the needs of large numbers of patients. Such spread requires making changes in the organisation of care delivery, policies, resources, and other factors that will influence the uptake of the superior model."
However, if we are to set out to disseminate a superior practice model or to scale up a practice that has proven itself on a small scale, it needs leadership and commitment from the top in spreading a superior model. We would need to ensure that these interventions were ready for optimal adoption across the EYC and in other important partners in the sector. They need especially to be aligned with agreed Single Outcome Agreements.
The relative advantage of the new intervention over current practice needs to be clear and understood by front line practitioners and understand how the new interventions may fit with the practitioner's current beliefs and work context. Put simply, we need to ensure that there are opportunities to test the intervention; and also that its results are visible to the practitioner.
Without this approach there will only be small pockets of activity (islands of excellence) and it is possible that the aims of EYC would never be realised. The first stage of testing the potential of a scaled up "Breakthrough" approach started in November 2013. National improvement partners and EYC programme managers met with Scottish Government colleagues to explore the evidence base and emerging intelligence across the EYC.
The Key Change areas that have emerged following that work are described below, but clearly there is more work to do so that the actual intervention (the 'what') is more clearly articulated and the associated measurement plan clearly sets out the measures, operational definitions and data collection guidance.
The EYC representatives at the Key Changes event have been asked to feedback the work to date to their colleagues and to identify sites in each CPP that are working on any aspects the Key Changes. They have also been asked to seek expressions of interest from areas that would consider being a 'Key Change Pioneer' site, where we can offer more improvement support and ability to share that learning.
The next Learning Session will present the work to date on Key Changes; present the evidence base and local intelligence that supports the work; and begin to explore the very early learning on work already underway with Key Change interventions and also highlight the Pioneer sites identified.
This diagram shows the main areas for improvement that have been suggested in the first year of the collaborative as being most likely to drive Scotland towards the achievement of the aims. Within each area, it is expected that front line workers will test and refine actions which they believe will effect improvements.
| Cross cutting themes | Workstream 1 | Workstream 2 | Workstream 3 |
|---|---|---|---|
| Key change area | Key change area | Key change area | Key change area |
| Workforce development - reliably delivering ways of working - such as the Solihull Approach - that enable the whole team to ensure that children have a good emotional start in life. | 1. Improving access to maternity services. | 1. Developing parenting skills to meet parents needs where and when they need it age stage 1 year to 30 months. | 1. Develop parenting skills to meet parents needs where and when they need it - age stage 30 months to P1 entry. |
Nutrition interventions across the age ranges, for children and families:
|
2. Attachment and child development-by age stage conception to one year. To include (not exhaustive)
|
2. Attachment and child- development bundle - by age stage 12-30 months (not exhaustive)
|
2. Attachment and child- development bundle by age stage 30 months to P1 entry. |
| Income maximisation achieved for families that require it - across the age ranges. | 3. Point of contact checklist. Transfer of care to next service (or from the last one). Continuity of care and carer Workforce development. Solihull. |
3. 27-30/12 review undertaken and appropriate pathway of intervention delivered. | 3. Children eligible for pre- school hours are identified and receive 95% of their allocation. |
| Stillbirth review process. | 4. Smoking cessation - delivering interventions in pregnancy reliably. |
Contact
Email: Diane Dempster